Web Stories
Latest Blogs
Cerebellum: Function, Balance Control, And Disorders
If you have ever felt unsteady on your feet, struggled with coordination, or noticed your speech sounding slightly slurred when you are tired or unwell, it is normal to feel concerned. These symptoms can have many causes, and they do not automatically mean something is wrong with your brain. Still, it helps to understand the part of the brain that fine-tunes balance and movement: the cerebellum. Your cerebellum does not start your movements. Instead, it helps make movements smooth, accurate, and well-timed. It also supports posture, balance control, and motor learning, which is how you improve with practice. (Manto M., Bower J. M., Conforto A. B., et al. 2012. PMID: 22161499) What Is The Cerebellum? The cerebellum is a compact structure at the back of your brain. The name comes from Latin and means “little brain.” Despite its small size, it contains a very large share of the brain’s neurons, which reflects how much information it processes. (Roostaei T., Nazeri A., Sahraian M. A., Minagar A. 2014. PMID: 25439284) In practical terms, you can think of the cerebellum as your brain’s quality control system for movement. It helps you walk steadily, reach accurately, speak clearly, and keep your eyes stable when you turn your head. Where Is The Cerebellum Located? Your cerebellum sits at the back of your head, below the cerebrum and behind the brainstem. Because of this location, problems affecting the cerebellum often show up as issues with balance, coordination, and eye control, rather than weakness alone. (Roostaei T., Nazeri A., Sahraian M. A., Minagar A. 2014. PMID: 25439284) Structure Of The Cerebellum The cerebellum has: Two hemispheres, one on each side A central region called the vermis Three main lobes: anterior, posterior, and flocculonodular It connects to the brainstem through bundles of nerve fibres called the cerebellar peduncles, which carry information between the cerebellum, the rest of the brain, and the spinal cord. This connectivity helps explain why symptoms can involve posture, walking pattern, eye movements, and speech clarity. (Roostaei T., Nazeri A., Sahraian M. A., Minagar A. 2014. PMID: 25439284) How The Cerebellum Works Your cerebellum constantly receives information from several sources, including: Your muscles and joints (to track body position) Your inner ear (to support balance) Your eyes (to stabilise gaze and guide movement) Other brain regions (to understand the movement you intend to make) It then integrates these inputs and helps fine-tune motor commands so your movements become fluid and precise. It also supports error correction. If you misjudge the position of a cup, for example, your cerebellum helps adjust your reach, and it helps your brain learn to do better next time. This is one reason the cerebellum is strongly linked to motor learning and adaptation. (Manto M., Bower J. M., Conforto A. B., et al. 2012. PMID: 22161499) Tests To Check The Health Of The Cerebellum There is no single “cerebellum test.” In practice, doctors assess your cerebellum through a combination of clinical examination, imaging, and laboratory tests that look for treatable causes. Common approaches include: Neurological examination Coordination checks such as finger-to-nose and heel-to-shin tests Gait assessment, including whether your steps become wide-based or unsteady Rapid alternating movement testing to check timing and control Imaging MRI is often the most informative scan for cerebellar conditions CT may be used in urgent situations, especially if bleeding is a concern Blood tests These help identify causes such as vitamin deficiencies, inflammation, metabolic problems, or toxin exposure Tests are tailored to your symptoms and medical history Additional tests when appropriate Genetic testing if an inherited ataxia is suspected Lumbar puncture if infection or inflammatory disease is a concern Clinical assessment remains central, because the pattern of symptoms often points to the most likely cause. (Javalkar V., Khan M., Davis D. E. 2014. PMID: 25439285) Functions Of The Cerebellum Cerebellum And Balance Control Balance is not controlled by one structure alone, but the cerebellum plays a key role in keeping you upright and steady. It helps coordinate signals from the inner ear and your eyes, allowing you to maintain equilibrium when you walk, turn, or stand on uneven ground. (Roostaei T., Nazeri A., Sahraian M. A., Minagar A. 2014. PMID: 25439284) Cerebellum And Muscle Coordination Your cerebellum helps you time and scale your movements. It supports: Smooth walking and controlled turning Accurate reaching and grasping Fine movements such as writing, buttoning clothing, or using cutlery When cerebellar control is disrupted, you may notice overshooting or undershooting targets, or shakiness as you approach an object. Doctors often call this an intention tremor. (Javalkar V., Khan M., Davis D. E. 2014. PMID: 25439285) Cerebellum And Eye Movements The cerebellum contributes to gaze stability. This helps keep your vision clear while you move your head. If this system is affected, you may develop abnormal eye movements such as nystagmus, or feel that your vision “bounces” when you walk. (Javalkar V., Khan M., Davis D. E. 2014. PMID: 25439285) Cerebellum And Cognitive Functions Research suggests the cerebellum may contribute to some non-motor functions, including aspects of attention and perception. This is an active area of study, and experts describe the cerebellum as influencing broader brain networks beyond movement. (Witter L., De Zeeuw C. I. 2015. PMID: 25884963) (Baumann O., Borra R. J., Bower J. M., et al. 2015. PMID: 25479821) Disorders Of The Cerebellum Many conditions can affect the cerebellum. Some are sudden and require urgent evaluation, while others develop gradually. Common categories include: Stroke affecting cerebellar blood supply Head injury, especially injury to the back of the skull Tumours in or near the posterior part of the brain Inflammatory and immune conditions, such as multiple sclerosis Infections that involve the brain Genetic or degenerative ataxias Metabolic or nutritional problems, including vitamin B12 deficiency Toxin exposure, including alcohol-related cerebellar damage Congenital conditions, such as developmental differences present from birth If your symptoms progress slowly, your doctor will often focus on identifying treatable contributors first, such as vitamin deficiency, thyroid disease, diabetes-related complications, or medication effects. (Marsden J. F. 2018. PMID: 30482319) Symptoms Of Cerebellum Damage Cerebellar symptoms often cluster around coordination, balance, and timing. Common symptoms include: Ataxia Unsteady, wide-based walking Difficulty turning or walking in a straight line Clumsiness with daily tasks Dysmetria Difficulty judging distance, such as missing an object when reaching Intention tremor Shaking that becomes more obvious as you approach a target Dysarthria Slurred or scanning speech, where words sound uneven or broken into parts Nystagmus and visual instability Jerky eye movements or blurred vision with head movement Dysdiadochokinesia Difficulty with rapid alternating movements, such as flipping your hand back and forth quickly Symptoms often appear on the same side of the body as the affected cerebellar hemisphere. (Javalkar V., Khan M., Davis D. E. 2014. PMID: 25439285) How Cerebellar Disorders Are Diagnosed Diagnosis usually includes: A careful history When symptoms began and how they progressed Recent infections, head injuries, alcohol intake, medication changes, and family history A focused neurological examination Gait, coordination, eye movement, speech, and reflexes Imaging MRI is commonly used to identify stroke, inflammation, tumour, or cerebellar shrinkage patterns Laboratory testing Blood tests help identify treatable causes or contributing factors Testing is chosen based on your clinical picture This step-by-step approach matters because treatment depends heavily on the underlying cause. (Marsden J. F. 2018. PMID: 30482319) Treatment Options For Cerebellum Disorders Treatment varies widely, but it often includes a mix of cause-specific care and supportive rehabilitation. Treating the underlying cause Vitamin replacement for nutritional deficiencies Targeted therapies for immune or inflammatory disease Appropriate management for stroke, infection, or tumours under specialist care Medication review if drugs are contributing to symptoms Managing symptoms and improving safety Fall prevention strategies at home Mobility aids when needed Vision assessment if visual instability is present Support for speech and swallowing if affected Early recognition and tailored rehabilitation can significantly improve function and independence. (Marsden J. F. 2018. PMID: 30482319) Role Of Physiotherapy And Rehabilitation Rehabilitation is often central to cerebellar recovery and long-term management. Physiotherapy helps improve gait stability, strength, and balance confidence. Occupational therapy helps you adapt daily tasks, reduce fall risk, and support independence. Speech and language therapy can help if you have dysarthria or swallowing difficulties. Rehabilitation also supports motor learning, which aligns with the cerebellum’s role in adapting movements through practice. (Marsden J. F. 2018. PMID: 30482319) Can Cerebellum Damage Be Reversed? It depends on the cause. Some causes can improve substantially, especially when treated early. Examples include vitamin deficiencies, medication-related effects, or certain inflammatory conditions. Some causes may partially improve with time and rehabilitation, such as recovery after stroke or head injury, although residual symptoms may remain. Progressive degenerative or genetic ataxias are often managed rather than reversed. In these cases, treatment focuses on function, safety, and quality of life. Even when full reversal is not possible, targeted support can make daily life easier and reduce complications such as falls. (Marsden J. F. 2018. PMID: 30482319) When To See A Doctor You should seek urgent medical evaluation if you or someone with you develops sudden onset: Severe dizziness with inability to walk steadily New slurred speech New double vision or major visual changes Sudden severe headache Sudden vomiting with severe imbalance New weakness, numbness, or collapse You should book a medical appointment if you notice: Gradually worsening unsteadiness Repeated falls or near-falls Persistent clumsiness or difficulty with fine hand movements Speech changes that persist Ongoing dizziness that affects daily life If you are supporting a loved one, it can help to note when symptoms began, how they change through the day, and whether there were triggers such as infection, alcohol intake, or medication changes. Key Takeaways Your cerebellum fine-tunes movement, balance, posture, and motor learning. Cerebellar problems often cause unsteadiness, coordination issues, abnormal eye movements, and changes in speech clarity. Many different conditions can affect the cerebellum, including stroke, inflammation, infection, injury, nutritional deficiency, and genetic causes. Diagnosis usually combines neurological examination, MRI imaging, and blood tests to identify treatable contributors. Treatment depends on the cause and often includes physiotherapy, occupational therapy, and speech therapy. Early assessment helps you access the right treatment and improve safety, especially if falls are a risk. Diagnostic Support With Metropolis Healthcare If you have balance or coordination symptoms, your doctor may recommend blood tests to check for treatable contributors such as vitamin deficiencies, thyroid dysfunction, diabetes-related issues, inflammation, or metabolic imbalance. Metropolis Healthcare supports this diagnostic work-up with NABL and CAP-accredited quality processes and a comprehensive test menu of 4,000 plus tests, including wellness testing and full body check-ups. For added convenience, you can book through the website, app, call, or WhatsApp, and opt for home sample collection backed by 10,000 touchpoints. Accurate reporting and quick turnaround can help your doctor make timely decisions about next steps. You can also explore more health and wellness articles on Metropolis Healthcare for practical guidance on prevention and early detection. FAQs What Happens If The Cerebellum Is Damaged? You may develop problems with coordination, balance, posture, eye movements, and speech clarity. Many people notice unsteady walking (ataxia), clumsiness with hand tasks, or shakiness during precise movements. (Javalkar V., Khan M., Davis D. E. 2014. PMID: 25439285) Does The Cerebellum Control Balance Only? No. The cerebellum supports balance, but it also helps coordinate voluntary movements, stabilise eye movements, and support motor learning. Research also suggests it influences some broader brain networks related to perception and cognition. (Manto M., Bower J. M., Conforto A. B., et al. 2012. PMID: 22161499) (Witter L., De Zeeuw C. I. 2015. PMID: 25884963) Can Cerebellum Problems Affect Speech? Yes. Cerebellar dysfunction can cause dysarthria, where speech becomes slurred or uneven in rhythm and emphasis. Speech therapy can help many people improve clarity and confidence. (Javalkar V., Khan M., Davis D. E. 2014. PMID: 25439285) What Is The Difference Between Cerebrum And Cerebellum? Your cerebrum is the largest part of your brain and supports thinking, sensation, and initiating voluntary movement. Your cerebellum is smaller and sits at the back of the brain. It fine-tunes and coordinates movement and supports balance and motor learning. (Roostaei T., Nazeri A., Sahraian M. A., Minagar A. 2014. PMID: 25439284) How Is Cerebellar Damage Detected? Doctors usually combine symptom history, neurological examination, and brain imaging, often MRI. Blood tests can help identify treatable causes such as vitamin deficiency or metabolic issues. (Marsden J. F. 2018. PMID: 30482319) References Baumann O., Borra R. J., Bower J. M., Cullen K. E., Habas C., Ivry R. B., et al. (2015). Consensus paper: The role of the cerebellum in perceptual processes. Cerebellum, 14(2), 197–220. PMID: 25479821 Javalkar V., Khan M., Davis D. E. (2014). Clinical manifestations of cerebellar disease. Neurologic Clinics, 32(4), 871–879. PMID: 25439285 Marsden J. F. (2018). Cerebellar ataxia. Handbook of Clinical Neurology, 159, 261–281. PMID: 30482319 Manto M., Bower J. M., Conforto A. B., Delgado-García J. M., da Guarda S. N., Gerwig M., et al. (2012). Consensus paper: Roles of the cerebellum in motor control, the diversity of ideas on cerebellar involvement in movement. Cerebellum, 11(2), 457–487. PMID: 22161499 Roostaei T., Nazeri A., Sahraian M. A., Minagar A. (2014). The human cerebellum: A review of physiologic neuroanatomy. Neurologic Clinics, 32(4), 859–869. PMID: 25439284 Witter L., De Zeeuw C. I. (2015). Regional functionality of the cerebellum. Current Opinion in Neurobiology, 33, 150–155. PMID: 25884963
Breast Cancer Medications: Types, How They Work, And What To Expect
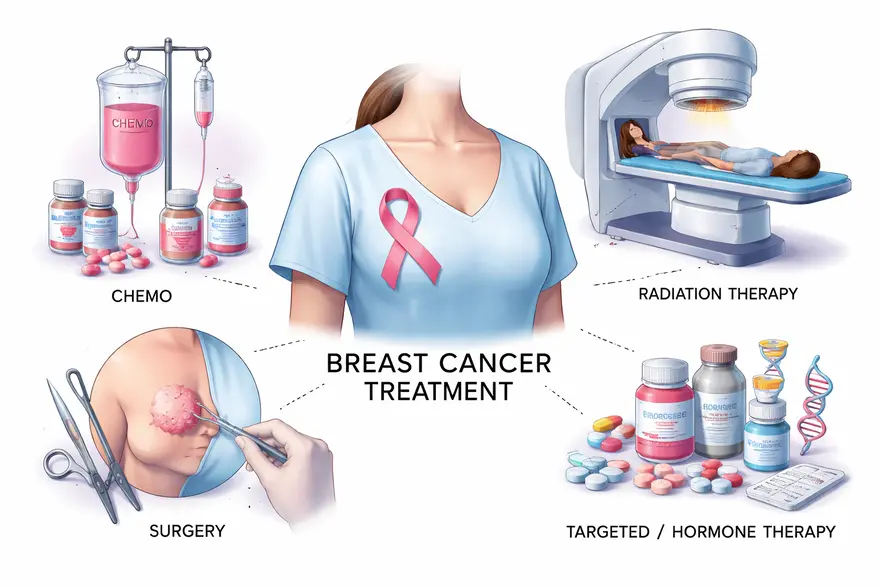
Breast cancer medications include chemotherapy, targeted therapy, hormone therapy, immunotherapy, and antibody drug conjugates. Your doctor chooses these medicines based on your tumour’s characteristics, such as whether it is HER2 positive, hormone receptor positive (ER and or PR positive), or triple negative, as well as the stage and your overall health. You may receive one medicine or a combination. In many treatment plans, medicines are combined to improve effectiveness or given in a planned sequence over time. This guide explains the main medication types, how they work, the tests that help guide treatment choices, and what side effects you may experience and manage. Key Takeaways Breast cancer medicines fall into a few main groups: hormone therapy, targeted therapy, chemotherapy, immunotherapy, and antibody drug conjugates. Your doctor selects medicines using tumour markers like ER, PR, and HER2, plus factors such as stage and menopausal status. Many treatment plans use combination therapy or step-by-step sequencing to improve results and reduce the risk of recurrence. Most side effects can be prevented or managed with supportive care, monitoring, and timely medical advice. Breast Cancer Medication Breast cancer medication refers to drugs used to treat breast cancer, lower the chance of it coming back, or in some situations reduce risk in people at high risk. Medicines may be used: Before surgery (neoadjuvant therapy) to shrink the tumour and assess response After surgery (adjuvant therapy) to reduce recurrence risk For advanced or metastatic breast cancer to control disease and support quality of life WHO reports that breast cancer caused an estimated 670,000 deaths globally in 2022 and that breast cancer occurs in every country in the world. Understanding Breast Cancer Type And Stage Why Subtype Matters Your treatment depends heavily on tumour biology. The most common labels you may hear are: Hormone Receptor Positive (ER and or PR positive) The cancer cells use hormones (oestrogen and or progesterone) as “fuel”. HER2 Positive The cancer cells have higher levels of a growth signal called HER2. Triple Negative Breast Cancer (TNBC) The tumour is ER negative, PR negative, and HER2 negative. Treatment often relies more on chemotherapy, and sometimes immunotherapy, depending on your situation. How Stage Influences Treatment Stage reflects tumour size and spread. Early-stage treatment often aims to cure and prevent recurrence. Advanced-stage treatment focuses on controlling cancer and preserving day-to-day wellbeing. Your doctor may also consider whether medicines should come before or after surgery, and whether radiotherapy is part of the plan. Types Of Breast Cancer Medications Hormone Therapy Hormone therapy (also called endocrine therapy) is used when the cancer is hormone receptor positive. Common examples include: Tamoxifen Aromatase inhibitors such as letrozole, anastrozole, and exemestane Fulvestrant (used in specific settings) Ovarian suppression medicines in selected premenopausal patients (your oncologist will advise) These treatments can be highly effective for ER-positive breast cancer. Large patient-level analyses show meaningful reductions in recurrence and mortality with endocrine therapy. Targeted Therapy Targeted treatments focus on specific features of cancer cells. Many require biomarker testing. HER2-targeted therapy (for HER2-positive breast cancer) may include: trastuzumab (Herceptin) pertuzumab (Perjeta) tucatinib (Tukysa) neratinib (Nerlynx) Trials have shown that adding trastuzumab to treatment improves outcomes in HER2-positive breast cancer. CDK4/6 inhibitors (commonly used for HR-positive, HER2-negative advanced breast cancer, often with hormone therapy): palbociclib (Ibrance) ribociclib (Kisqali) abemaciclib (Verzenio) These drugs help slow cancer cell division and are typically combined with endocrine therapy. PARP inhibitors (for eligible patients, often linked to inherited BRCA mutations): olaparib (Lynparza) talazoparib (Talzenna) For high-risk early breast cancer with BRCA1 or BRCA2 mutations, a year of adjuvant olaparib has been shown to reduce recurrence risk. Chemotherapy Chemotherapy kills fast-growing cells and is used in many breast cancer settings, especially: Triple negative breast cancer Higher-risk early breast cancer HER2-positive breast cancer (often alongside targeted therapy) Advanced breast cancer Examples include paclitaxel, docetaxel, doxorubicin, cyclophosphamide, capecitabine, and others. Your regimen depends on tumour biology, stage, and health factors. Immunotherapy Immunotherapy helps your immune system recognise and attack cancer. It is not used for every breast cancer type. One example is pembrolizumab (Keytruda), used in selected triple negative breast cancer settings. A key trial in early triple negative breast cancer showed benefit when pembrolizumab was added to neoadjuvant chemotherapy and continued after surgery. Antibody Drug Conjugates Antibody drug conjugates (ADCs) deliver a chemotherapy payload directly to cancer cells through a targeted antibody. Examples include: ado-trastuzumab emtansine (Kadcyla, also called T-DM1) trastuzumab deruxtecan (Enhertu, also called T-DXd) sacituzumab govitecan (Trodelvy) In HER2-positive metastatic breast cancer, trastuzumab deruxtecan has shown improved outcomes compared with trastuzumab emtansine in a major randomised trial. Medicines Used For Risk Reduction In High Risk Individuals If you are at increased risk of breast cancer, your clinician may discuss “chemoprevention”, meaning medication to reduce risk. This is a specialist decision based on your risk profile and medical history. Evidence from large prevention trials supports risk reduction with tamoxifen in selected high-risk women, and raloxifene as an option in postmenopausal women. How Breast Cancer Medications Work Blocking Hormones That Fuel Cancer Growth Hormone therapies reduce oestrogen’s effects or lower oestrogen levels, depriving hormone receptor-positive cancer cells of growth signals. Targeting Growth Signals And Cancer Pathways HER2-targeted treatments block HER2 signalling, while CDK4/6 inhibitors slow cell cycle progression. Killing Fast Growing Cells Chemotherapy affects fast-growing cells, including cancer cells. This is why it can also affect hair follicles and bone marrow. Helping Your Immune System Recognise Cancer Checkpoint inhibitors like pembrolizumab help immune cells stay active against cancer in selected cases. Delivering Treatment Directly Into Cancer Cells ADCs link a targeted antibody to a chemotherapy payload so treatment is delivered more directly to cancer cells. How Doctors Choose The Right Breast Cancer Medication For You Your oncologist considers multiple factors, including: ER, PR, and HER2 status Stage and whether lymph nodes are involved Menopausal status and overall health Past treatments and how the cancer responded Your preferences and practical priorities, such as daily tablets versus hospital infusions You may receive: Combination therapy (for example endocrine therapy plus a CDK4/6 inhibitor) Sequential therapy where medicines change over time depending on response, side effects, or recurrence risk This approach is normal and is designed to keep treatment both effective and sustainable. Tests That Guide Breast Cancer Medication Choices Accurate testing is central to choosing the right medicines. Tests On Your Biopsy Sample Your biopsy report typically includes: Tumour type and grade ER and PR status HER2 status Sometimes Ki-67 (a marker related to cell growth rate) ICMR’s Standard Treatment Workflow for breast cancer recommends testing ER, PR, HER2/neu, and Ki-67, and using FISH when HER2 is equivocal on IHC. Biomarker And Genetic Testing That May Influence Treatment Depending on your clinical scenario, your doctor may suggest: Inherited mutation testing such as BRCA1 and BRCA2 Tumour mutation testing (for example PIK3CA in selected cases) PD-L1 testing in some triple negative breast cancers (to guide immunotherapy decisions) Baseline And Monitoring Tests During Treatment Many treatments require monitoring to keep you safe and comfortable, such as: Full blood count (to monitor white cells, haemoglobin, platelets) Liver and kidney function tests Glucose and lipids for certain targeted therapies Heart function monitoring when using therapies that can affect the heart, such as anthracyclines and HER2-targeted therapy ASCO guidance recommends assessing and monitoring heart function in people receiving cancer therapies that may affect the heart, especially when risk factors are present. Benefits Of Early And Appropriate Medication In Breast Cancer Starting the right medication at the right time can: Reduce the risk of recurrence after surgery Shrink tumours before surgery, sometimes allowing less extensive procedures Improve control and quality of life in advanced disease For HER2-positive breast cancer, HER2-targeted therapy added to standard treatment has shown clear benefits in clinical trials. Common Side Effects Of Breast Cancer Medications Side effects vary by medication and by person. You may experience none, a few, or more than expected. The aim is always to treat cancer effectively while supporting you through side effects. Side Effects Of Chemotherapy Common effects may include: Tiredness and weakness Nausea and appetite changes Hair loss (with some regimens) Mouth sores Lowered blood counts, which can increase infection risk Side Effects Of Hormone Therapy Possible effects include: Hot flushes and night sweats Joint and muscle aches (especially with aromatase inhibitors) Vaginal dryness Changes in mood or sleep Rare risks such as blood clots with tamoxifen (your doctor will assess your risk) Side Effects Of Targeted Therapy These depend on the drug: HER2-targeted therapy can sometimes affect heart function, which is why monitoring is often recommended. CDK4/6 inhibitors can lower white blood cells and may cause fatigue or diarrhoea, so regular blood tests are common. Side Effects Of Immunotherapy Immunotherapy can cause inflammation in healthy tissues because it activates the immune system. Your doctor will explain what to watch for and when to seek advice. Side Effects Of Antibody Drug Conjugates ADCs can cause nausea, fatigue, and low blood counts. Some ADCs have specific side effects your team will monitor for, and early reporting of symptoms is important. Managing Side Effects And Staying Comfortable During Treatment Practical Tips You Can Try At Home Eat small, frequent meals if nausea or poor appetite is an issue Stay hydrated and rest when you need to Use gentle oral care to reduce mouth soreness Keep a simple symptom diary so you can describe patterns clearly to your doctor Ask about safe physical activity, as gentle movement can help fatigue and mood Supportive Medicines Your Doctor May Prescribe Supportive care can make a big difference, for example: Anti-sickness medicines Medicines for diarrhoea or constipation Treatments for hot flushes or sleep Bone health support in selected patients When You Should Contact Your Doctor Urgently Seek prompt medical advice if you have: Fever or chills during chemotherapy Severe diarrhoea or vomiting New breathlessness, chest pain, or fainting Unusual bleeding or bruising A rapidly worsening rash You are not “bothering” your team by calling. Early support is often the easiest way to prevent complications. Taking Your Medicines Safely Take medicines exactly as prescribed, and do not stop suddenly unless your clinician advises it. Tell your doctor about supplements, herbal products, and over-the-counter medicines, as interactions can matter. If you miss a dose, follow your prescription guidance or ask your care team rather than doubling up. Discuss contraception and pregnancy planning early, because some medicines can harm a developing baby. Frequently Asked Questions What Are The Side Effects Of Chemotherapy For Breast Cancer? Common side effects include tiredness, nausea, hair loss (with some regimens), mouth sores, and lowered blood counts. Not everyone experiences the same effects, and most can be managed with supportive medicines and monitoring. What Is The Difference Between Hormone Therapy And Chemotherapy For Breast Cancer? Hormone therapy works by blocking oestrogen’s effects or reducing oestrogen levels and is used when the cancer is hormone receptor positive. Chemotherapy attacks fast-growing cells and is used across several breast cancer subtypes, especially when the cancer is higher risk or hormone therapy alone is not enough. How Long Do Side Effects Of Breast Cancer Medication Last? Some side effects are short-term and improve after treatment cycles end, such as nausea or low blood counts from chemotherapy. Others can continue while you are taking long-term medicines such as hormone therapy. If a side effect is affecting your day-to-day life, tell your doctor early, because adjustments and supportive care are often available. Do All Breast Cancers Need Chemotherapy? No. Some breast cancers are treated primarily with surgery and hormone therapy, with or without targeted therapy, depending on the tumour subtype and recurrence risk. Your oncologist will explain why chemotherapy is recommended or not recommended in your case. Why Do You Need ER, PR, And HER2 Testing Before Treatment? These markers help identify which medicines are most likely to work. For example, ER-positive cancers often respond well to hormone therapy, and HER2-positive cancers may benefit from HER2-targeted medicines. Can Medicines Help Prevent Breast Cancer If You Are High Risk? In selected high-risk individuals, medicines such as tamoxifen or raloxifene can reduce the risk of developing invasive breast cancer. This decision should be made with a clinician after weighing benefits and risks. How Long Will You Need To Take Hormone Therapy? Many people take endocrine therapy for several years. Your oncologist will individualise duration based on your recurrence risk, menopausal status, and how well you tolerate treatment. Can You Continue Working During Treatment? Many people can, but you may need adjustments. Fatigue and appointment schedules can be challenging. It can help to plan for flexible hours, accept support, and speak to your team about symptom control. How Metropolis Healthcare Can Support You When your doctor recommends breast cancer testing, reliable results matter because they guide treatment decisions. Metropolis Healthcare supports you with a wide range of diagnostic services, including speciality testing aligned to oncology pathways. With NABL and CAP-accredited labs, 4,000+ tests, and full body checkups, Metropolis Healthcare helps make testing accessible and dependable. You can also choose home sample collection, supported by a strong home collection network with 10,000 touchpoints, along with quick turnaround and accurate results. Booking is designed to be convenient through the website, app, call, and WhatsApp. In addition to supporting your testing needs, you can explore more Metropolis articles to stay informed and feel more confident in discussions with your care team. Conclusion Breast cancer medications can include hormone therapy, targeted therapy, chemotherapy, immunotherapy, and antibody drug conjugates. Your treatment is chosen based on your tumour’s markers, stage, and your overall health, and it is normal for plans to involve combinations or step-by-step changes over time. If you feel anxious about side effects or decisions, bring those concerns to your doctor early. You deserve clear answers and practical support throughout treatment. References Early Breast Cancer Trialists’ Collaborative Group (EBCTCG), Davies C., Godwin J., Gray R., et al. (2011). Relevance of breast cancer hormone receptors and other factors to the efficacy of adjuvant tamoxifen: Patient-level meta-analysis of randomised trials. Lancet, 378(9793), 771–784. PMID: 21802721 Early Breast Cancer Trialists’ Collaborative Group (EBCTCG). (2015). Aromatase inhibitors versus tamoxifen in early breast cancer: Patient-level meta-analysis of the randomised trials. Lancet, 386(10001), 1341–1352. PMID: 26211827 Piccart-Gebhart M. J., Procter M., Leyland-Jones B., et al. (2005). Trastuzumab after adjuvant chemotherapy in HER2-positive breast cancer. New England Journal of Medicine, 353(16), 1659–1672. PMID: 16236737 Romond E. H., Perez E. A., Bryant J., et al. (2005). Trastuzumab plus adjuvant chemotherapy for operable HER2-positive breast cancer. New England Journal of Medicine, 353(16), 1673–1684. PMID: 16236738 Finn R. S., Martin M., Rugo H. S., et al. (2016). Palbociclib and letrozole in advanced breast cancer. New England Journal of Medicine, 375(20), 1925–1936. PMID: 27959613 Hortobagyi G. N., Stemmer S. M., Burris H. A., et al. (2016). Ribociclib as first-line therapy for HR-positive, advanced breast cancer. New England Journal of Medicine, 375(18), 1738–1748. PMID: 27717303 Schmid P., Cortes J., Pusztai L., et al. (2020). Pembrolizumab for early triple-negative breast cancer. New England Journal of Medicine, 382(9), 810–821. PMID: 32101663 Cortés J., Kim S. B., Chung W. P., et al. (2022). Trastuzumab deruxtecan versus trastuzumab emtansine for breast cancer. New England Journal of Medicine, 386(12), 1143–1154. PMID: 35320644
Cerebrum: Functions, Lobes And Key Disorders
Your brain does an extraordinary amount of work every second. The cerebrum is the largest part of your brain and is responsible for the skills you rely on most in daily life, such as thinking, learning, memory, speech, sensation, and voluntary movement. This guide explains what the cerebrum is, what each lobe does, and the most important warning signs that mean you should seek medical care without delay. What Is The Cerebrum? The cerebrum is the upper, largest portion of your brain. It helps you stay aware of your surroundings, make decisions, understand language, and control voluntary movements. It also plays a major role in your personality, emotions, and behaviour. In simple terms, if you are consciously thinking or intentionally doing something, your cerebrum is heavily involved. Where Is The Cerebrum Located In The Brain? Your cerebrum sits at the top and front of your skull. It covers deeper brain structures and connects with: The brainstem, which controls vital functions like breathing and heart rate The cerebellum, which fine-tunes balance, posture, and coordination Structure Of The Cerebrum The cerebrum includes several important layers and parts: Cerebral Cortex: The outer grey matter, responsible for higher processing and interpretation of information White Matter: The inner “wiring” that carries signals between different brain regions Gyri And Sulci: The folds and grooves that increase surface area, helping you process more complex information Corpus Callosum: A major bridge of nerve fibres that helps the left and right hemispheres communicate Thalamus: A relay centre that routes sensory signals (except smell) to the right areas Basal Ganglia: A group of structures involved in movement control and habit learning Left Vs Right Cerebral Hemisphere Your cerebrum is divided into two hemispheres: The left hemisphere mainly controls the right side of your body The right hemisphere mainly controls the left side of your body Some abilities are more “dominant” on one side for many people. For example, language is often left-dominant, while some aspects of spatial attention and visual processing are often right-dominant. Even so, both hemispheres typically work together, and there is natural variation between individuals. Functions Of The Cerebrum Role Of The Cerebrum In Thinking And Memory Your cerebrum supports attention, planning, judgement, problem-solving, and decision-making. The prefrontal cortex is especially important for organising thoughts and controlling behaviour. Memory is not stored in one single place. Different networks help you store and retrieve experiences, facts, and skills, and they work together depending on what you are trying to remember. Cerebrum And Voluntary Movements When you decide to move, signals from the motor areas of your cerebrum travel through nerve pathways to your muscles. This is how you walk, write, lift objects, and speak. Your cerebellum and basal ganglia help refine and coordinate those movements. Cerebrum And Sensory Processing Your cerebrum interprets information from your senses, including touch, pain, temperature, sound, and vision. This is how you recognise a familiar voice, feel heat, or notice when something is sharp. Cerebrum And Speech And Language Language is supported by a network rather than a single “spot.” Traditionally, the frontal region is linked with speech production and the temporal-parietal region is linked with comprehension. Modern research highlights that language comprehension involves broader connected areas than many people assume. Lobes Of The Cerebrum Each hemisphere has major lobes with special roles. Understanding them helps make sense of symptoms when something goes wrong. Frontal Lobe: Functions And Disorders What It Helps You Do Plan and organise Focus attention Control impulses and behaviour Start voluntary movements Produce speech Common Problems If Affected Personality or behaviour changes Poor judgement or reduced concentration Weakness on one side of the body Speech difficulty Frontal lobe function is strongly linked to executive control networks. Parietal Lobe: Functions And Disorders What It Helps You Do Process touch, pain, and temperature Judge distance and spatial relationships Direct attention to what matters Common Problems If Affected Numbness or reduced sensation Trouble judging space or navigating Difficulty with attention, including neglect in some cases Temporal Lobe: Functions And Disorders What It Helps You Do Understand spoken language Form and retrieve memories Recognise faces and objects Link emotions with memory Common Problems If Affected Memory issues Language comprehension problems Seizures (temporal lobe epilepsy is a common form) Memory systems rely on distributed networks involving temporal lobe structures. Occipital Lobe: Functions And Disorders What It Helps You Do Process visual information such as movement, shapes, and colour Common Problems If Affected Blurred vision or blind spots Difficulty recognising objects Visual field loss after stroke or injury Key Disorders Of The Cerebrum Stroke Affecting The Cerebrum A stroke happens when blood flow to part of the brain is interrupted. If the cerebrum is affected, symptoms depend on the region involved. Common signs include facial drooping, arm weakness, speech changes, sudden confusion, or sudden vision problems. Stroke is time-critical. Early assessment and treatment can reduce disability and improve outcomes. Traumatic Brain Injury A traumatic brain injury (TBI) can happen after a fall, road traffic accident, sports injury, or assault. Symptoms can range from headache and confusion to severe weakness, seizures, or loss of consciousness. Moderate to severe TBI requires urgent medical evaluation and careful monitoring. Cerebral Tumours Tumours in the cerebrum may cause headaches, seizures, weakness, speech changes, or personality changes. Some tumours are benign, while others are malignant. Diagnosis usually involves imaging and specialist assessment. Neurodegenerative Disorders Conditions such as Alzheimer’s disease affect brain networks over time. Early symptoms often include memory changes, difficulty finding words, and problems managing daily tasks. Diagnosis usually involves clinical assessment and may include cognitive testing and blood tests to rule out other causes. Symptoms Of Cerebrum Damage Symptoms vary depending on the affected region, speed of onset, and underlying cause. Common symptoms include: Sudden weakness or numbness on one side New speech difficulty or trouble understanding speech Sudden confusion or reduced alertness New seizures Persistent or worsening headaches, especially with vomiting Memory problems or noticeable personality changes Vision problems such as blind spots or loss of part of your visual field Difficulty with balance, coordination, or planning tasks If symptoms start suddenly, treat it as urgent. How Cerebral Disorders Are Diagnosed Diagnosis usually combines: Medical history and symptom timeline Neurological examination Imaging such as CT or MRI when needed EEG if seizures are suspected Cognitive assessment for memory and thinking concerns Blood tests to check for treatable contributors (for example thyroid issues, vitamin B12 deficiency, infection, inflammation, or metabolic causes) Common Tests To Check The Cerebrum Depending on your symptoms, your doctor may recommend: CT scan or MRI brain EEG Blood tests (glucose, lipids, thyroid function, vitamin B12, infection markers) Lumbar puncture in selected cases Neuropsychological testing Treatment Options For Cerebrum Disorders Treatment depends on the cause and may include: Medicines (for example, to control seizures, reduce inflammation, treat infection, or manage risk factors) Surgery for certain tumours or bleeding Rehabilitation to regain function after stroke or injury Lifestyle and risk-factor management such as controlling blood pressure, diabetes, cholesterol, sleep, and weight Role Of Rehabilitation And Cognitive Therapy Rehabilitation can make a meaningful difference. Your care plan may involve physiotherapy for movement, occupational therapy for daily skills, speech and language therapy, and cognitive therapy for attention and memory. Can Cerebrum Damage Be Reversed? Some causes are reversible or treatable, especially when addressed early. For example, seizures may be controlled, infections can be treated, and certain deficiencies can be corrected. In other cases, such as stroke or neurodegenerative disease, the goal is often to reduce damage, support recovery, and help you function as well as possible. Even when full reversal is not possible, many people improve with timely treatment and structured rehabilitation. When To See A Doctor Seek medical advice if you have: Persistent headaches or new neurological symptoms Memory changes that affect daily life New speech or vision problems A first-time seizure Behavioural or personality changes noticed by you or your family When To Seek Emergency Care Get urgent medical help if you have sudden symptoms such as: Face drooping, arm weakness, or difficulty speaking Sudden confusion or collapse A seizure that is new, prolonged, or followed by slow recovery Severe headache with vomiting, fainting, or neck stiffness Sudden vision loss Conclusion Your cerebrum supports the abilities that make daily life possible, from movement and speech to memory and decision-making. If you notice new or sudden symptoms, timely evaluation can make a real difference. You do not need to manage worrying symptoms alone. Medical teams can identify the cause and guide you with the right next steps. If your doctor recommends blood tests to check for contributing factors such as diabetes, thyroid imbalance, infection, inflammation, vitamin deficiencies, or cholesterol, Metropolis Healthcare can support you with accurate testing and reliable reports. With 4,000+ tests, full body checkups, and home sample collection supported by a wide network of touchpoints, you can book conveniently via the website, app, call, or WhatsApp and access quality diagnostics as part of your overall brain health plan. FAQs What Does The Cerebrum Control? It controls higher functions such as thinking, memory, language, sensory processing, emotions, personality, and voluntary movement. How Is The Cerebrum Different From The Cerebellum? Your cerebrum supports conscious thought and intentional actions, while your cerebellum mainly helps coordinate movement, posture, and balance. Can Cerebrum Damage Affect Behaviour? Yes. Changes in behaviour, judgement, impulse control, and personality can occur, especially when the frontal lobe is affected. Which Lobe Controls Speech? Speech production is strongly linked with frontal lobe networks, while understanding language involves temporal and broader connected regions. Is Cerebrum Damage Permanent? It depends on the cause and how quickly you receive treatment. Some issues are treatable and some effects can improve with rehabilitation, while others may be long-term. References Miller E. K., Cohen J. D. (2001). An Integrative Theory Of Prefrontal Cortex Function. Annual Review of Neuroscience, 24, 167–202. PMID: 11283309 Squire L. R. (2004). Memory Systems Of The Brain: A Brief History And Current Perspective. Neurobiology of Learning and Memory, 82(3), 171–177. PMID: 15464402 Binder J. R. (2015). The Wernicke Area: Modern Evidence And A Reinterpretation. Neurology, 85(24), 2170–2175. PMID: 26567270 Dronkers N. F., Plaisant O., Iba-Zizen M. T., Cabanis E. A. (2007). Paul Broca’s Historic Cases: High Resolution MR Imaging Of The Brains Of Leborgne And Lelong. Brain, 130(5), 1432–1441. PMID: 17405763 Constantinidis C., Bucci D. J. (2006). Posterior Parietal Cortex: Functional Organization And Role In Cognitive Functions. Reviews in Neuroscience, 17(4), 415–427. PMID: 17139842 Bloom J. S., Hynd G. W. (2005). The Role Of The Corpus Callosum In Interhemispheric Transfer Of Information: Excitation Or Inhibition? Neuropsychology Review, 15(2), 59–71. PMID: 16211466 Uddin L. Q., Nomi J. S., Hébert-Seropian B., Ghaziri J., Boucher O. (2017). Structure And Function Of The Human Insula. Journal of Clinical Neurophysiology, 34(4), 300–306. PMID: 28644199 Graybiel A. M. (2008). Habits, Rituals, And The Evaluative Brain. Annual Review of Neuroscience, 31, 359–387. PMID: 18558860 Powers W. J., Rabinstein A. A., Ackerson T., et al. (2019). Guidelines For The Early Management Of Patients With Acute Ischemic Stroke: 2019 Update. Stroke, 50(12), e344–e418. PMID: 31662037 Maas A. I. R., Stocchetti N., Bullock R. (2008). Moderate And Severe Traumatic Brain Injury In Adults. Lancet Neurology, 7(8), 728–741. PMID: 18635021 Wen P. Y., Kesari S. (2008). Malignant Gliomas In Adults. New England Journal of Medicine, 359(5), 492–507. PMID: 18669428 McKhann G. M., Knopman D. S., Chertkow H., et al. (2011). The Diagnosis Of Dementia Due To Alzheimer’s Disease. Alzheimer’s & Dementia, 7(3), 263–269. PMID: 21514250 Fisher R. S., Acevedo C., Arzimanoglou A., et al. (2014). ILAE Official Report: A Practical Clinical Definition Of Epilepsy. Epilepsia, 55(4), 475–482. PMID: 24730690
Renal Parenchymal Disease: Causes, Symptoms, Tests, And Treatment
Renal parenchymal disease is an umbrella term for damage to the working tissue of your kidneys (the parenchyma). This tissue includes the tiny filters and tubes that clean your blood and make urine. When the parenchyma is affected, your kidneys may not filter as efficiently, and over time this can contribute to chronic kidney disease (CKD). In many people, renal parenchymal disease is linked to long term conditions such as diabetes or high blood pressure. It can also develop after infections, immune related inflammation, certain medicines, or inherited kidney conditions. The right treatment depends on the cause and how early the problem is detected. What Is Renal Parenchymal Disease? Renal parenchymal disease refers to conditions that affect the kidney parenchyma, which is the functional tissue that filters your blood and helps balance fluids and salts. This includes the glomeruli (tiny filters), tubules (small channels that process filtered fluid), and the interstitial tissue that supports them. In everyday practice, the term is often used in imaging reports, particularly ultrasound, to describe changes like increased echogenicity (the kidney looks “brighter” than expected) or altered kidney size. These changes can be linked with many different conditions, so your doctor will usually combine imaging with blood and urine tests to understand what is happening. Renal parenchymal disease can be: Acute, meaning it develops suddenly (for example, due to a severe infection, dehydration, or a medication reaction). Chronic, meaning it develops gradually over time and may contribute to chronic kidney disease (CKD). Causes Of Renal Parenchymal Disease Renal parenchymal disease is not one single illness. It is an umbrella term for many possible causes, including: Diabetes: High blood glucose can damage kidney filters over time. High Blood Pressure: Persistent high pressure can scar kidney tissue and reduce kidney function. Autoimmune Conditions: Conditions such as lupus can inflame kidney tissue. Glomerulonephritis: Inflammation of the kidney’s filtering units. Infections: Some bacterial or viral infections can affect the kidneys. Medications And Toxins: Certain drugs can strain the kidneys. High-dose, long-term NSAID use has been associated with faster CKD progression in some studies. Inherited Or Structural Conditions: Such as polycystic kidney disease or congenital kidney abnormalities. Kidney Stones Or Obstruction: These can affect drainage and lead to tissue stress. You may be at higher risk if you live with diabetes, hypertension, cardiovascular disease, obesity, older age, or a family history of kidney disease. Symptoms Of Renal Parenchymal Disease Many people have no symptoms in early stages, especially if kidney function is only mildly affected. When symptoms appear, they can be non-specific and easy to miss. Common symptoms can include: Feeling unusually tired or weak Swelling in ankles, feet, legs, or around the eyes Changes in urination (foamy urine, blood in urine, passing less or more urine than usual) Loss of appetite, nausea, or an unpleasant taste in the mouth Shortness of breath (sometimes due to fluid retention or anaemia) High blood pressure that is new or hard to control Itchy, dry skin When You Should Seek Medical Help Quickly Contact a doctor promptly if you notice blood in urine, rapidly worsening swelling, very low urine output, severe breathlessness, confusion, chest pain, or persistent vomiting. These symptoms do not always mean severe kidney disease, but they do need timely assessment. Diagnosis Of Renal Parenchymal Disease Diagnosis usually focuses on two things: How well your kidneys are working What is causing the damage Your clinician may start with your medical history (including diabetes, blood pressure, infections, and medication use) and a physical exam. Then they typically recommend a combination of tests. Key lab checks include: Serum Creatinine And eGFR (Estimated Glomerular Filtration Rate) eGFR estimates how effectively your kidneys filter waste. Many labs use creatinine-based equations such as CKD-EPI. Urine Tests These look for protein (albumin) and blood. Albumin-to-creatinine ratio (ACR) is a common way to measure albumin loss. Electrolytes And Related Blood Tests Depending on your situation, your doctor may check potassium, bicarbonate, haemoglobin (for anaemia), and other markers to understand how kidney changes are affecting your body. Renal parenchymal disease is often linked with CKD risk assessment, which considers both eGFR and albuminuria. Large cohort analyses show that lower eGFR and higher albuminuria are associated with higher risk of adverse outcomes, which is one reason clinicians take these measures seriously. Imaging And Diagnostic Tests To Identify Renal Parenchymal Disease Imaging helps your clinician understand kidney structure and rule out blockage or stones. Ultrasound Ultrasound is commonly the first imaging test. It can assess: Kidney size Cortical thickness Echogenicity (brightness) Evidence of obstruction Increased cortical echogenicity is commonly reported and can correlate with chronic tissue changes such as fibrosis and tubular atrophy, although ultrasound alone cannot reliably identify the exact underlying disease. CT Or MRI These may be recommended in selected situations, for example if your clinician needs a detailed view of anatomy, stones, masses, or complicated obstruction. Kidney Biopsy A biopsy is not needed for everyone. It may be advised when the cause is unclear, when there is significant proteinuria or blood in urine, or when your clinician suspects a condition that needs targeted treatment (such as specific glomerular diseases). A biopsy can provide definitive tissue-level information to guide management. Treatment Options For Renal Parenchymal Disease Treatment depends on the underlying cause, how advanced the disease is, and your overall health. The goals are usually to: Treat the cause (where possible) Slow progression Reduce symptoms and complications Protect your heart and blood vessels, which are closely linked with kidney health Common treatment components include: Managing Diabetes And Blood Pressure Tightening blood glucose control can reduce ongoing kidney stress. Keeping blood pressure in a healthy range is one of the most effective ways to protect kidney function long term. Medication Adjustments Your clinician may: Review pain medicines and advise safer options if needed, especially if NSAIDs are being used frequently. Prescribe treatments to reduce protein in urine, depending on your diagnosis and blood pressure. Treating Immune Or Inflammatory Causes If autoimmune disease is involved, your specialist may use corticosteroids or other immunosuppressive medicines. This is highly individual and needs close monitoring. Diet And Fluid Planning A renal diet approach may be recommended, often focusing on: Reduced salt intake Appropriate protein intake Managing potassium and phosphate if kidney function is reduced Advanced Care If Kidney Failure Develops If kidney function becomes severely reduced, your clinician may discuss kidney replacement therapy options such as dialysis or transplant evaluation. Many people never reach this stage, especially with early detection and good long-term control of risk factors. Managing Renal Parenchymal Disease Living with renal parenchymal disease can feel like a lot to carry, especially when you are waiting for results or trying to understand a new diagnosis. A structured plan helps you regain a sense of control. Practical Steps That Often Help Take medicines exactly as prescribed and keep a list of all medicines and supplements. Monitor blood pressure at home if your clinician advises it. Stay active with gentle, regular movement that fits your energy levels. Aim for a healthy weight in a gradual, sustainable way. Avoid smoking and limit alcohol, as advised by your clinician. Salt And Lifestyle Guidance The World Health Organization recommends less than 2,000 mg sodium per day, which is under 5 g salt per day for adults. The American Heart Association recommends no more than 2,300 mg sodium per day, with an optimal goal of 1,500 mg per day for most adults. The Indian Council of Medical Research encourages practical blood pressure habits such as regular exercise and cutting down on salt and fried foods. Follow-Up And Monitoring Your doctor may recommend repeating kidney tests over time. This matters because CKD is defined by persistence over at least 3 months, not a single abnormal report. Can Renal Parenchymal Disease Be Prevented? You cannot prevent every cause, but you can meaningfully reduce risk by addressing the most common drivers of kidney damage. Prevention-focused habits include: Regular checks if you have diabetes or hypertension Consistent blood pressure control Safer use of pain medicines and avoiding unnecessary high-dose NSAIDs Maintaining healthy salt intake and balanced nutrition Staying active and smoke-free Getting early evaluation for recurrent urinary infections or kidney stone symptoms Even if you already have renal parenchymal disease, these steps can still slow progression and reduce complications. Renal Parenchymal Disease And Its Impact On Kidney Function When kidney parenchyma is damaged, filtering becomes less efficient. Clinicians often track this using eGFR categories and albuminuria levels. The KDIGO 2024 CKD guideline classifies eGFR (G1 to G5) and albuminuria (A1 to A3) to help estimate risk and guide monitoring and treatment intensity. Complications Of Renal Parenchymal Disease Not everyone develops complications, but possible issues include: Fluid retention and swelling High potassium levels Metabolic acidosis (acid build-up) Anaemia Bone and mineral imbalance Higher cardiovascular risk This is why your clinician may check more than just creatinine and urine protein, especially if your kidney function is reduced. FAQ What Are The Symptoms Of Renal Parenchymal Disease? You may have no symptoms at first. If symptoms develop, they often include tiredness, swelling in legs or around the eyes, changes in urination, nausea, itchy skin, and blood pressure changes. If you have sudden breathlessness, very low urine output, or blood in urine, seek medical advice promptly. How Is Renal Parenchymal Disease Diagnosed? Diagnosis usually involves blood tests (including creatinine and eGFR), urine tests (including ACR), and imaging such as ultrasound. In selected cases, a kidney biopsy may be recommended to confirm the cause and guide treatment. Can Renal Parenchymal Disease Be Cured? Some causes are reversible or treatable, especially if found early. In other cases, the focus is on slowing progression and preventing complications. With the right plan and regular follow-up, many people maintain stable kidney function for years. A Reassuring Next Step If you have been told you may have renal parenchymal disease, the most helpful step is a clear, test-led assessment of kidney function and the likely cause. Early answers reduce uncertainty and help you and your doctor make practical choices. At Metropolis Healthcare, you can access a wide range of kidney-related investigations, including routine and speciality testing, with NABL and CAP-accredited quality systems. You can also choose home sample collection across a large network of touchpoints, with convenient booking via website, app, call, or WhatsApp, and reliable reporting to support timely clinical decisions. References Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. (2024). KDIGO 2024 Clinical Practice Guideline For The Evaluation And Management Of Chronic Kidney Disease. Kidney International, 105(4S), S117–S314. PMID: 38490803 Levey A. S., Stevens L. A., Schmid C. H., et al. (2009). A New Equation To Estimate Glomerular Filtration Rate. Annals Of Internal Medicine, 150(9), 604–61 PMID: 19414839 Matsushita K., van der Velde M., Astor B. C., et al. (2010). Association Of Estimated Glomerular Filtration Rate And Albuminuria With All-Cause And Cardiovascular Mortality In General Population Cohorts: A Collaborative Meta-Analysis. The Lancet, 375(9731), 2073–2081. PMID: 20483451 Nderitu P., Doos L., Jones P. W., Davies S. J., Kadam U. T. (2013). Non-Steroidal Anti-Inflammatory Drugs And Chronic Kidney Disease Progression: A Systematic Review. Family Practice, 30(3), 247–255. PMID: 23302818 Page J. E., Morgan S. H., Eastwood J. B., et al. (1994). Ultrasound Findings In Renal Parenchymal Disease: Comparison With Histological Appearances. Clinical Radiology, 49(12), 867–870. PMID: 7828393 Hull K. L., Adenwalla S. F., Topham P., Graham-Brown M. P. M. (2022). Indications And Considerations For Kidney Biopsy: An Overview Of Clinical Considerations For The Non-Specialist. Clinical Medicine (London), 22(1), 34–40. PMID: 34921054
Fine Motor Skills: Meaning, Examples, And How To Improve
Fine motor skills are the small, precise movements you make using the muscles in your hands, fingers, and wrists. These skills help you manage everyday tasks like writing, buttoning clothes, using cutlery, typing, and handling small objects. They rely on coordination between your brain, eyes, nerves, muscles, and joints, so they can feel effortless on a good day and frustrating when something is off. If you are reading this because you are worried about your child, or because you have noticed changes in your own hands, try to remember this. Fine motor skills can improve at any age with the right practice and support. And when help is needed, there are clear next steps. What Are Fine Motor Skills? Fine motor skills are the small, controlled movements that allow you to handle objects with accuracy. They involve the tiny muscles in your hands and fingers, along with the stability of your wrist and forearm. Most people think of handwriting and pencil grip, but fine motor skills also show up in daily self-care, cooking, crafts, phone use, and work tasks. Fine motor skills depend on three main abilities: Control: You can start, stop, and adjust movement smoothly. Strength: You have enough grip and pinch strength to hold objects without strain. Coordination: Your eyes and hands work together so you can aim and adjust in real time. Fine Motor Control: What Has To Work Together Fine motor control is a team effort inside your body. It typically includes: Planning and attention from your brain Signals travelling through nerves to muscles Movement at joints in your fingers, wrist, and hand Visual guidance, so you can place and adjust accurately Sensation from your fingertips, so you can judge pressure, texture, and position When one part of this system is not working well, tasks like using buttons or holding a pen can become slower or tiring. Fine Motor Skills Vs Gross Motor Skills Gross motor skills use large muscles for bigger movements like sitting, walking, running, climbing, and jumping. Fine motor skills build on that foundation, because you often need a stable body and shoulder position before your hands can move with precision. Quick Comparison Feature Fine Motor Skills Gross Motor Skills Main muscles used Small hand and finger muscles Large muscles in arms, legs, and trunk Typical tasks Writing, buttoning, using utensils Walking, jumping, throwing, climbing Key focus Precision and dexterity Strength, balance, and large movement control Why Are Fine Motor Skills Important? Fine motor skills support independence in everyday life. They affect how confidently you can care for yourself, how easily your child can manage school tasks, and how smoothly you can work with tools and technology. Fine motor skills matter because they support: Self care: Dressing, eating, grooming, and basic household tasks Learning: Drawing, colouring, writing, cutting, and using classroom tools Work and productivity: Typing, tool use, lab work, repairs, and many professional tasks Confidence: When tasks feel easier, you are more likely to try new activities Research suggests that fine motor ability is linked with early academic achievement, especially in the early school years when children are learning to write and manage classroom tasks. Fine motor skills and executive function both contribute to kindergarten achievement. Why They Matter At Different Life Stages In children, fine motor skills support school readiness, handwriting, and independence in dressing and eating. In adults, they support work tasks, parenting, cooking, and daily routines. In older adults, they can affect independence and safety, such as managing medication packaging or using keys. Examples Of Fine Motor Skills In Daily Life Fine motor skills show up in more places than you might expect. Here are common examples. Self Care Examples Buttoning shirts, fastening zips, tying shoelaces Brushing teeth and hair Washing hands thoroughly and handling toiletries Using a spoon and fork without spilling Opening small lids and packaging School And Work Examples Holding a pencil and writing or drawing Cutting with scissors Turning pages and organising stationery Typing and using a mouse or trackpad Using tools that require accuracy, such as screwdrivers or craft tools Play, Hobbies, And Technology Examples Building with blocks or construction toys Threading beads and doing puzzles Playing a musical instrument Gaming with a controller Texting, swiping, and tapping on a phone Fine Motor Skills In Children In childhood, fine motor skills develop gradually from simple grasping to more refined movements like using scissors or writing neatly. Healthcare professionals often track these skills because significant delays can sometimes be linked to broader developmental challenges. At the same time, it is normal for children to develop at different speeds, especially when they are learning a new skill. If you are comparing your child to others, try to focus on progress. A child who is improving, even slowly, is usually moving in the right direction. Early Development: From Grasp Reflex To Pincer Grip In early life, fine motor control often follows a pattern like this: Newborns show a natural grasp reflex Babies begin reaching and grabbing objects as coordination improves They learn to pass objects between hands Many develop a pincer grasp, using thumb and finger, by around their first birthday These are general patterns rather than strict rules, so your child’s overall progress and daily function are what matter most. Development Of Fine Motor Skills By Age Milestones help you understand what is typical at different ages. Use these as a guide, not a test. If your child is not doing one item yet but is progressing in other ways, that can still be normal. Fine Motor Skill Milestones In Toddlers Common skills you may notice include: Stacking a few blocks Scribbling with a crayon Turning thick pages Feeding themselves with a spoon, with some mess Picking up small objects using thumb and finger Trying to pull zips up or down with help Fine Motor Skill Development In Preschoolers Preschool years are often a big leap forward. You may see: Better pencil control and copying simple shapes Cutting with child-safe scissors, starting with straight lines More independent dressing, such as pulling on clothes and managing bigger buttons More accurate building, puzzles, and crafts Early tripod grip for crayons or pencils in some children School Age Progress As school demands increase, fine motor skills often become more efficient. You may notice: Improved handwriting and spacing Better endurance for longer writing tasks More precise cutting and craft skills Ability to tie shoelaces, depending on the child Better control using sports equipment or musical instruments Fine Motor Skills And The Brain Fine motor skills feel like they happen in your hands, but the brain is doing the planning, timing, and constant correction. When you reach for a button or write a word, your brain predicts what should happen, receives feedback from your eyes and fingertips, and adjusts pressure and direction in real time. Role Of The Cerebrum In Fine Motor Skills The cerebrum supports voluntary movement, planning, attention, and problem solving. This is the part of your brain that helps you decide what you want to do and organise the movement needed to do it. Role Of The Cerebellum In Precision And Coordination The cerebellum supports timing and smooth coordination. It helps fine tune movement so actions feel steady rather than shaky or jerky. Why Touch And Body Awareness Matter Sensation is a quiet but essential part of fine motor control. When your fingertips can clearly feel texture and pressure, it is easier to grip lightly, adjust force, and move with confidence. If sensation is reduced, you may squeeze too hard, drop objects, or avoid tasks that feel awkward. Causes Of Poor Fine Motor Skills Fine motor difficulties can develop at any age. The cause is not always serious, but it is worth paying attention to patterns, associated symptoms, and whether things are getting better or worse. Common contributing factors include: Reduced hand strength or endurance Coordination challenges, including visual motor integration difficulties Pain or stiffness in the joints of the hand or wrist Nerve irritation or compression that affects sensation or grip Recovery after injury to the hand, wrist, shoulder, or neck Differences in sensory processing or motor planning in some children Neurological conditions that affect movement control Fine Motor Skill Difficulties In Children Children may struggle with fine motor skills for a range of reasons, including coordination challenges, motor planning difficulties, or differences in attention and sensory processing. In some children, handwriting can be particularly affected when fine motor precision and in-hand manipulation are not well developed. Causes In Teens And Adults In teenagers and adults, fine motor issues can be linked to overuse, nerve compression, joint inflammation, or recovery after injury. If you notice numbness, tingling, pain, or weakness, it is sensible to discuss it with a doctor, especially if it is persistent. If you have a sudden change in hand strength or coordination, or you notice other sudden symptoms such as facial drooping, speech changes, or severe dizziness, seek urgent medical help. Signs You May Need Help For Fine Motor Skills You may benefit from extra support if you notice one or more of the following: You or your child often drop objects or seem unusually clumsy with hands Buttons, zips, cutlery, or handwriting feel much harder than expected for age Your child avoids colouring, crafts, or writing due to frustration or fatigue You notice persistent hand pain, stiffness, numbness, or tingling Tasks take much longer than before, even with practice Skills are getting worse rather than gradually improving How To Improve Fine Motor Skills Fine motor improvement is usually about consistent, well chosen practice. You get better when tasks are challenging enough to build skill, but not so hard that they create daily battles. A helpful approach is: Practise little and often, rather than doing long sessions Build strength and coordination together Start with larger objects and easier movements, then progress to smaller and more precise tasks Praise effort and progress, not just the final result Fine Motor Skill Activities For Babies And Toddlers Choose safe, supervised activities that encourage grasping and release: Let your baby hold safe toys with different textures Offer larger blocks or stacking cups Use posting toys, where your child puts shapes into slots Encourage finger feeding with age appropriate foods and supervision Use chunky crayons for scribbling as they get older Fine Motor Skill Activities For Preschool And School Age Children These activities build hand strength, precision, and coordination: Playdough squeezing, rolling, and pinching Threading beads or pasta onto a string Cutting along thick lines, then moving to thinner lines Colouring within simple shapes Tweezers games, such as moving small objects between bowls Building sets, puzzles, and craft projects If handwriting is a concern, short daily practice with correct posture and an age-appropriate pencil grip can help. Handwriting support can also be more effective when it is built into play and classroom routines, rather than treated as a daily struggle. Kadar M., Wan Yunus F., Tan E., et al. (2020). A systematic review of occupational therapy intervention for handwriting skills in 4-6 year old children. Fine Motor Exercises For Adults If you want to improve control and endurance, focus on functional exercises: Practise pinch strength by picking up coins or buttons and placing them into a container Do finger isolation drills, such as tapping each finger to your thumb slowly Use therapy putty or a soft stress ball for gentle grip work, if it does not cause pain Improve dexterity through hobbies like knitting, simple DIY, or musical practice Check your workstation setup so your wrists are supported and you take regular breaks Fine Motor Skills Improvement After Injury After an injury, it is normal to feel slower and less confident. A gradual return works best: Start with gentle movements and light objects Increase difficulty slowly, guided by comfort and function Avoid pushing through sharp pain or increasing numbness Focus on quality of movement rather than speed If you are recovering from a fracture, tendon injury, or nerve injury, structured rehabilitation guidance is often important. Everyday Habits That Support Improvement Small daily habits can make practice more effective: Keep posture stable, especially when writing or doing precise tasks Take short breaks to avoid fatigue and overuse Aim for good sleep, as coordination and learning consolidate with rest Maintain a balanced diet and hydration, since muscles and nerves depend on good overall health Occupational Therapy For Fine Motor Skills Occupational therapy is one of the most practical supports for fine motor difficulties. An occupational therapist can assess how you or your child uses hands in daily tasks, then create a plan that builds strength, coordination, and confidence. Support may include: Exercises for grip, pinch, and finger control Activities to improve hand eye coordination Practical strategies for dressing, eating, and school tasks Adaptive tools, such as pencil grips or modified cutlery, when appropriate A home programme that fits your routine Occupational therapy is focused on function. The goal is to help you manage everyday life more comfortably and independently. Fine Motor Skills And Learning Fine motor skills can influence classroom confidence, especially when tasks involve handwriting, cutting, drawing, or copying from a board. When fine motor control is still developing, your child may know the answer but struggle to show it on paper. Research suggests fine motor skills are linked with academic outcomes, particularly in early schooling, which is why early support can be helpful when difficulties are persistent. Simple School And Home Adjustments These supports can reduce stress while skills improve: Use short practice bursts rather than long worksheets Offer thicker pencils or pencil grips if holding a pencil is tiring Try a slightly slanted writing surface Break tasks into smaller steps with clear targets Allow alternative ways to show learning when needed, such as verbal answers or typing When To See A Doctor Or Therapist You should consider professional advice if: Your child’s fine motor skills are not progressing over time Daily tasks cause significant frustration, fatigue, or avoidance There is regression, meaning a skill that was present has noticeably worsened You notice pain, swelling, numbness, tingling, tremor, or weakness You have a sudden change in hand function or other sudden neurological symptoms A doctor can help rule out medical causes and guide the next steps. If therapy is appropriate, earlier support often makes daily life easier. How Metropolis Healthcare Can Support You If you are concerned about fine motor difficulties, you are not expected to figure it out alone. Your doctor may sometimes recommend tests to check for conditions that can affect nerves, muscles, or energy levels, such as blood sugar issues, vitamin deficiencies, thyroid imbalance, inflammation, or other underlying factors. Testing is not always needed, but it can be useful when symptoms are persistent, worsening, or accompanied by numbness, tingling, weakness, or fatigue. Metropolis Healthcare can support your care journey with NABL and CAP accredited labs, expert pathologists, and a wide test menu of 4,000 plus tests, including full body checkups and specialised testing. You can also choose home sample collection with quick turnaround and accurate results, supported by a strong home collection network across 10,000 touchpoints. Booking is convenient through the website, app, call, or WhatsApp, so you can focus on the next step with less stress. For more guidance, you can explore more health and wellness articles from Metropolis Healthcare and use their diagnostic services as part of your doctor led care plan. Key Takeaways Fine motor skills are the precise movements you do with your hands, fingers, and wrists, and sometimes your toes. They support independence, school readiness, work tasks, and hobbies. Fine motor skills usually develop after gross motor skills like sitting, crawling, and walking. Children develop at different speeds, so patterns and progress matter more than a single milestone. Fine motor difficulties can happen for many reasons, including coordination challenges, pain, nerve problems, or recovery after injury. With simple home activities and, when needed, occupational therapy, you can strengthen fine motor control over time. Frequently Asked Questions What Are Fine Motor Skills In Simple Words? Fine motor skills are the small, precise movements you do with your hands and fingers, like writing, buttoning clothes, using cutlery, and typing. How Can I Improve Fine Motor Skills At Home? You can improve fine motor skills by practising little and often. Try activities like playdough, bead threading, tweezers games, colouring, cutting practice, and everyday tasks like buttoning and using utensils. Choose tasks that are slightly challenging but not overwhelming. What Causes Poor Fine Motor Skills? Fine motor difficulties can be caused by low hand strength, coordination challenges, pain or joint stiffness, nerve irritation, sensory changes, or recovery after injury. In children, differences in motor planning or attention can also play a role. Are Fine Motor Skills Linked To Brain Development? Yes. Fine motor skills rely on the brain’s ability to plan movement, coordinate timing, and adjust using feedback from your eyes and fingertips. This is why fine motor development and learning can be closely connected in early childhood. Cameron C. E., Brock L. L., Murrah W. M., et al. (2012). Fine motor skills and executive function both contribute to kindergarten achievement. Child Development, 83(4), 1229–1244. PMID: 22537276 Can Adults Improve Fine Motor Skills? Yes. Adults can improve fine motor skills with consistent practice, strength building, and functional activities like hobbies, dexterity exercises, and ergonomic adjustments. Improvement is often gradual, so regular practice matters more than intensity. References Cameron C. E., Brock L. L., Murrah W. M., et al. (2012). Fine motor skills and executive function both contribute to kindergarten achievement. Child Development, 83(4), 1229–1244. PMID: 22537276 Kadar M., Wan Yunus F., Tan E., et al. (2020). A systematic review of occupational therapy intervention for handwriting skills in 4-6 year old children. Australian Occupational Therapy Journal, 67(1), 3–12. PMID: 31799722 Li Y., Wu X., Ye D., et al. (2025). Research progress on the relationship between fine motor skills and academic ability in children: A systematic review and meta-analysis. Frontiers in Sports and Active Living, 6, 1386967. PMID: 39850871 Manto M., Bower J. M., Conforto A. B., et al. (2012). Consensus paper: Roles of the cerebellum in motor control. Cerebellum, 11(2), 457–487. PMID: 22161499 Seo S. M. (2018). The effect of fine motor skills on handwriting legibility in preschool age children. Journal of Physical Therapy Science, 30(2), 324–327. PMID: 29545705
Gardner Syndrome: Symptoms, Diagnosis And Cancer Risk
What Is Gardner Syndrome? Gardner syndrome is a rare inherited condition in the same family of disorders as familial adenomatous polyposis (FAP). It is best known for causing numerous adenomatous polyps in the colon and rectum. Over time, these polyps can progress to colorectal cancer if they are not monitored and managed appropriately. What makes Gardner syndrome distinctive is that it can also cause growths outside the bowel. These are called extracolonic manifestations. They may involve the bones, skin, soft tissues, teeth, and eyes. In some people, these visible or easily detected signs can appear before bowel symptoms, which is why early evaluation matters. Is Gardner Syndrome A Type Of FAP? Yes. Gardner syndrome is widely described as a phenotypic variant of FAP, meaning it shares the same underlying genetic pathway but tends to show additional features beyond bowel polyps. In classic FAP, bowel polyps are the dominant finding. In Gardner syndrome, you may see bowel polyps plus extracolonic features such as osteomas (benign bone growths), epidermoid cysts, dental abnormalities, and desmoid tumours. This overlap is important because the screening approach focuses on preventing cancer while also monitoring other body systems. Causes Of Gardner Syndrome Role Of The APC Gene Mutation Gardner syndrome is most commonly associated with a pathogenic variant in the APC gene. APC acts as a tumour suppressor, meaning it helps regulate cell growth. When APC function is disrupted, the lining of the bowel can develop multiple adenomas, and there can also be growths in other tissues. Is Gardner Syndrome Inherited? Gardner syndrome is usually inherited in an autosomal dominant pattern. This means if one parent carries a pathogenic APC variant, each child has a 50 percent chance of inheriting it. It is also possible to have Gardner syndrome without a known family history due to a new, spontaneous genetic change (often called a de novo variant). This is one reason why your doctor may still consider testing even if no one else in your family has been diagnosed. Symptoms Of Gardner Syndrome Symptoms can vary from person to person and often change over time. Some people notice extracolonic signs first, while others only become aware after bowel screening. Gastrointestinal Symptoms Many people do not feel symptoms early on, even if polyps are present. When symptoms occur, they may include: Blood in stools Persistent diarrhoea or constipation Abdominal pain or cramping Unexplained tiredness, sometimes related to anaemia Unintended weight loss in some cases Even if you feel well, screening is still essential because polyps can develop silently. Bone And Dental Symptoms Bone and dental findings can be early clues. These may include: Osteomas, commonly affecting the jaw or skull Dental abnormalities such as extra teeth, impacted teeth, or enamel and jaw changes that may complicate alignment Jaw lesions may be detected on dental X rays, sometimes before bowel symptoms appear. Skin And Soft Tissue Symptoms Skin and soft tissue features may include: Epidermoid cysts, often on the face, scalp, or trunk Fibromas or lipomas Desmoid tumours, which are non cancerous but can grow aggressively and press on nearby structures depending on their location Desmoid tumours need careful monitoring because their behaviour can be unpredictable. Eye Findings That Can Be A Clue Some people have a characteristic eye finding called congenital hypertrophy of the retinal pigment epithelium (CHRPE). These are pigmented retinal lesions seen on an eye examination. CHRPE patterns can support clinical suspicion in the right context, although interpretation should be done by an eye specialist with awareness of inherited polyposis syndromes. Gardner Syndrome And Cancer Risk Risk Of Colorectal Cancer The main cancer concern in Gardner syndrome is colorectal cancer. Without surveillance and timely treatment, the likelihood of cancer becomes very high over time. This is why specialist follow up is not optional. It is the core of staying safe and well. Risk Of Other Cancers Gardner syndrome and the broader FAP spectrum can be associated with increased risk of other cancers, which may include: Upper gastrointestinal cancers, especially duodenal and gastric areas Thyroid cancer Other tumours reported in some families, with risk influenced by genetics and clinical history Because risks vary, your doctor will tailor surveillance based on your personal and family profile. At What Age Does Cancer Risk Increase? Polyps often develop during adolescence or early adulthood. Cancer risk rises as polyps accumulate and as time passes without preventive care. In practice, this is why screening and genetic counselling typically start early in families where an APC pathogenic variant is known. Your specialist will advise exactly when you should begin and how often follow up is needed. How Gardner Syndrome Is Diagnosed Diagnosis usually combines your personal history, family history, clinical signs, endoscopic findings, and genetic testing. Genetic Testing For Gardner Syndrome Genetic testing looks for pathogenic variants in APC. Testing may be recommended if: You have a close relative diagnosed with FAP or Gardner syndrome You develop multiple adenomatous polyps You have suggestive extracolonic signs such as jaw osteomas with skin cysts or significant dental anomalies A positive test can clarify your surveillance plan and also guide testing for family members. Colonoscopy And Other Tests Your doctor may recommend: Colonoscopy or sigmoidoscopy to detect and manage bowel polyps Upper gastrointestinal endoscopy based on risk profile Imaging such as ultrasound, CT, or MRI if desmoid tumours are suspected or need monitoring Dental imaging for jaw lesions Eye examination to assess for CHRPE patterns Differential Diagnosis Several inherited conditions can cause multiple polyps or early cancers. Distinguishing between them is important because screening intervals, associated risks, and family implications differ. If you have multiple polyps or a strong family history of bowel cancer, a specialist evaluation and genetic counselling can help you get the correct diagnosis and plan. Management And Treatment Options There is no single cure that removes the genetic cause, but there are highly effective strategies to reduce cancer risk and manage symptoms. Colon Surveillance And Surgery The cornerstone of care is regular surveillance of the colon and rectum. If polyp burden becomes difficult to manage endoscopically, preventive surgery may be recommended to reduce colorectal cancer risk. The timing and type of surgery depend on polyp number, polyp behaviour, and your overall health, and should be discussed carefully with a specialist team. In some situations, your doctor may also discuss medicines used to reduce polyp burden. These decisions are individual and should always be guided by a specialist. Management Of Bone, Skin And Soft Tissue Tumours Management is often shared across specialties: Dentists and maxillofacial specialists can help with impacted or extra teeth and jaw lesions Dermatology care can support treatment of epidermoid cysts and skin lesions Desmoid tumours may be observed with imaging when stable, or treated when they threaten organs or quality of life, in line with expert guidance Role Of Genetic Counselling Genetic counselling helps you understand: What your results mean for your future screening Which relatives may benefit from testing How autosomal dominant inheritance affects family planning decisions If you feel overwhelmed by the implications, that is normal. Counselling gives you a structured way to make decisions without feeling rushed. Living With Gardner Syndrome Living with Gardner syndrome often means living with a plan. A clear plan can reduce anxiety because you know what you are monitoring and why. Helpful steps include: Keep a written record of your tests, results, and next due dates Tell your doctor about new lumps, persistent bowel changes, or unexplained symptoms Focus on sustainable health habits, including balanced nutrition, sleep, and activity Ask for emotional support when needed, especially around major procedures or screening milestones You do not need to manage this alone. Coordinated care is part of good treatment. Prognosis And Life Expectancy With early detection, structured surveillance, and timely preventive treatment, many people live full lives. The main risk comes from missed screening and delayed intervention. If you follow your specialist plan, the outlook is generally much more reassuring than it first sounds when you read the diagnosis. When To See A Doctor Speak to a doctor if you notice: Blood in stools Persistent diarrhoea or constipation lasting more than two to three weeks Ongoing abdominal pain Unexplained anaemia or fatigue New or growing lumps, especially in the abdomen or jaw area Strong family history of multiple polyps or early colorectal cancer Seek urgent care for severe abdominal pain, persistent vomiting, fainting, or heavy rectal bleeding. Key Takeaways Gardner syndrome is a hereditary condition linked to changes in the APC gene and is considered a variant of familial adenomatous polyposis (FAP). It often causes many bowel polyps and can also lead to bone, skin, dental, and eye findings that may appear earlier than bowel symptoms. With the right screening plan and timely treatment, you can significantly reduce cancer risk and protect long term health. Frequently Asked Questions Is Gardner Syndrome Cancerous? Gardner syndrome itself is not cancer. It is a genetic condition that can greatly increase your risk of colorectal cancer and some other cancers if you do not have proper surveillance and preventive care. How Is Gardner Syndrome Different From FAP? Gardner syndrome is considered a variant of FAP. Both involve APC gene related polyps, but Gardner syndrome more often includes extracolonic findings such as osteomas, skin cysts, dental abnormalities, and desmoid tumours. Dinarvand P, Davaro EP, Doan JV, et al. (2019). Familial Adenomatous Polyposis Syndrome: An Update And Review Of Extraintestinal Manifestations. Archives Of Pathology And Laboratory Medicine, 143(11), 1382–1398. PMID: 31070935 Can Gardner Syndrome Be Cured? There is no cure that removes the genetic change. However, the risks can be managed effectively through regular screening, preventive interventions when needed, and monitoring of extracolonic features. Should Family Members Be Tested? If you have a confirmed APC pathogenic variant, your close relatives may benefit from genetic counselling and testing. This helps identify who needs early screening and who does not. At What Age Should Screening Start? This depends on your family history and genetic results. In families with known APC variants, screening often begins earlier than standard population screening. Your specialist will advise an age and schedule that fits your risk profile. Waller A, Findeis S, Lee MJ. (2016). Familial Adenomatous Polyposis. Journal Of Pediatric Genetics, 5(2), 78–83. PMID: 27617147 How Metropolis Healthcare Can Support You If you are exploring genetic risk, need screening, or are monitoring a known condition, reliable diagnostics can make decision making easier. Metropolis Healthcare supports you with: NABL and CAP accredited quality systems and expert pathology oversight 4,000 plus tests, including speciality testing and preventive health check ups Convenient home sample collection with strong coverage across 10,000 touchpoints Accurate reports with quick turnaround times Simple booking through the website, app, call, or WhatsApp You can also explore more Metropolis articles on preventive screening, hereditary cancer risk, and long term wellness so you feel informed at every step. References Dinarvand P, Davaro EP, Doan JV, Ising ME, Evans NR, Phillips NJ, Lai J, Guzman MA. (2019). Familial Adenomatous Polyposis Syndrome: An Update And Review Of Extraintestinal Manifestations. Archives Of Pathology And Laboratory Medicine, 143(11), 1382–1398. PMID: 31070935 Waller A, Findeis S, Lee MJ. (2016). Familial Adenomatous Polyposis. Journal Of Pediatric Genetics, 5(2), 78–83. PMID: 27617147 Desmoid Tumor Working Group. (2020). The Management Of Desmoid Tumours: A Joint Global Consensus Based Guideline Approach For Adult And Paediatric Patients. European Journal Of Cancer, 127, 96–107. PMID: 32004793 Deibert B, Ferris L, Sanchez N, Weishaar P. (2019). The Link Between Colon Cancer And Congenital Hypertrophy Of The Retinal Pigment Epithelium (CHRPE). American Journal Of Ophthalmology Case Reports, 15, 100524. PMID: 31384696 Utsunomiya J, Nakamura T. (1975). The Occult Osteomatous Changes In The Mandible In Patients With Familial Polyposis Coli. British Journal Of Surgery, 62(1), 45–51. PMID: 1111674 Monachese M, Mankaney G, Lopez R, O’Malley M, Laguardia L, Kalady MF, Church J, Shin J, Burke CA. (2019). Outcome Of Thyroid Ultrasound Screening In FAP Patients With A Normal Baseline Exam. Familial Cancer, 18(1), 75–82. PMID: 30003385 Tulchinsky H, Keidar A, Strul H, Goldman G, Klausner JM, Rabau M. (2005). Extracolonic Manifestations Of Familial Adenomatous Polyposis After Proctocolectomy. Archives Of Surgery, 140(2), 159–163. PMID: 15723997
Bone Scan: Uses, Preparation, Results And Risks
If you have ongoing bone pain, a suspected fracture that has not shown clearly on an X-ray, or a condition that affects your bones, your doctor may suggest a bone scan. A bone scan is a nuclear medicine test that highlights areas of increased or reduced bone activity across your skeleton. It can often detect changes earlier than standard X-rays, which is why it is commonly used when the cause of symptoms is not yet clear. Bone Scan At A Glance What It Is: A scan that shows how actively your bones are changing or repairing. What It Helps Detect: Fractures, infection, inflammation, arthritis, some bone disorders, and cancer spread to bone. Key Steps: Injection of a radiotracer, a waiting period, then imaging with a special camera. Timing: Imaging is commonly done 2 to 4 hours after the injection. Results Language: Areas of higher activity can appear as “hot spots”, and areas of lower activity can appear as “cold spots”. What It Cannot Do Alone: It may not confirm the exact cause of an abnormal area, so follow-up tests are sometimes needed. What Is A Bone Scan A bone scan, also called skeletal scintigraphy, is an imaging test that uses a tiny amount of radiotracer to help identify abnormal bone metabolism. Your bones are living tissue that constantly remodels. When there is injury, infection, inflammation, or tumour-related change, bone turnover can increase or decrease. A bone scan visualises these changes. Unlike an X-ray, which mainly shows bone structure, a bone scan focuses on bone activity. This is one reason it may detect a problem earlier, even when an X-ray looks normal. How A Bone Scan Works Radiotracer And Bone Metabolism Most bone scans use a technetium-99m labelled diphosphonate tracer that binds to areas of active bone formation. Regions where bone is remodelling more quickly tend to absorb more tracer, making them stand out on the images. Understanding Hot Spots And Cold Spots Hot Spots: Areas where the tracer uptake is higher than expected. This can happen with healing fractures, arthritis, infection, Paget’s disease, and bone metastases. Cold Spots: Areas where uptake is lower than expected. This can be seen in some conditions that reduce blood supply or bone activity. A key point is that a bone scan is sensitive, but not always specific. More than one condition can produce a similar pattern. That is why your doctor interprets results alongside your symptoms, examination findings, and other tests. Types Of Bone Scans Standard Whole-Body Bone Scan This is the most common approach when your doctor needs a broad overview of bone activity across the skeleton. Three-Phase Bone Scan In a three-phase bone scan, images may be taken during injection, shortly after, and again several hours later. This approach can help when infection or inflammation is being considered. SPECT Or SPECT-CT Imaging Sometimes, additional imaging called SPECT or SPECT-CT is added to improve localisation and confidence in interpretation, especially in complex areas like the spine or joints. Studies show SPECT-CT can improve diagnostic confidence when differentiating benign from malignant bone lesions in certain settings. Why A Doctor May Recommend A Bone Scan Your doctor may recommend a bone scan when they need to: Investigate bone pain that remains unexplained after initial tests. Look for a stress fracture or other small fracture that is not clear on X-ray. Check for bone infection (osteomyelitis) or inflammation. Assess cancer spread to bone or monitor response to treatment. Evaluate certain bone disorders that affect bone remodelling patterns. Uses Of A Bone Scan Bone Scan For Cancer Detection And Spread A bone scan can help detect bone metastases and map where bone involvement may be present, which can support staging and treatment planning. Bone Scan For Fractures And Injuries Bone scans can identify stress fractures and some fractures that are difficult to see on early X-rays, because bone repair activity can show up before structural changes are obvious. Bone Scan For Bone Infections And Inflammation Bone infection and inflammatory bone processes can increase tracer uptake. When infection is suspected, your doctor may choose a three-phase scan or add other tests to strengthen the diagnosis. Bone Scan For Arthritis And Paget’s Disease Arthritis can cause focal uptake around affected joints. Paget’s disease can produce more extensive uptake patterns related to increased remodelling. Bone Scan For Unexplained Bone Pain If you have persistent pain and initial imaging does not explain it, a bone scan can guide the next step by showing where bone activity is abnormal, even if the exact cause still needs clarification. Preparation For A Bone Scan What To Do Before A Bone Scan Tell your doctor and the imaging team if: You are pregnant, may be pregnant, or are breastfeeding. You have allergies or have reacted to medical injections in the past. You have had recent illnesses or ongoing medical conditions. You recently had imaging that used contrast, or you have taken certain medicines that may interfere with results. Medicines And Recent Contrast Tests Bismuth-containing medicines (such as some indigestion remedies) and recent barium contrast studies can interfere with bone scan results. Your doctor may ask you to avoid or time these appropriately before the scan. Can You Eat Or Drink Before A Bone Scan In many cases you can eat as normal. Your team may ask you to limit fluids for a few hours beforehand, then drink extra water after the injection to help flush out tracer that your bones do not absorb. What To Wear And What To Bring Wear loose, comfortable clothing and avoid jewellery or metal accessories, as these may interfere with the imaging process. If you have prior imaging reports, it can help to bring them or ensure your doctor has access to them. Bone Scan Procedure Step By Step Injection Of Radioactive Tracer A small amount of radiotracer is injected into a vein in your hand or arm. You may feel a brief pin-prick and sometimes a cool sensation in the arm. Waiting Period It usually takes 2 to 4 hours for the tracer to circulate and bind to your bones. During this time, you are typically asked to drink water and pass urine as advised. Imaging With A Gamma Camera You lie on a table while a gamma camera captures images. The scan itself is usually painless, but staying still can be uncomfortable if you already have joint or bone pain. Additional Imaging If Needed Sometimes extra images are taken to clarify a finding. This does not automatically mean something serious is present. After The Bone Scan: What To Expect Most people return to normal activities afterwards. You may be advised to drink plenty of fluids for the next day to help clear the tracer from your body. Patient guidance notes that the radiation level is small enough that contact with others is generally not a risk after the test, but always follow the specific instructions you are given, especially if you are around pregnant women or young children. What Do Bone Scan Results Mean Normal Bone Scan Results A normal scan typically shows a relatively even distribution of tracer uptake, without suspicious focal hot spots or cold spots. Abnormal Bone Scan Results Abnormal findings often show as: Focal hot spots More widespread areas of increased uptake Cold spots in a defined region Conditions Linked To Hot Spots Hot spots are commonly associated with: Healing fractures and stress injuries Arthritis and joint degeneration Infection or inflammation Paget’s disease Bone metastases Why Further Tests May Be Needed A bone scan may not identify the exact cause of abnormal uptake by itself. Your doctor may recommend additional imaging such as X-ray, CT, MRI, or further testing such as blood tests or, less commonly, biopsy, depending on the pattern and your symptoms. Accuracy Of A Bone Scan Bone scans are valued because they can detect abnormal bone activity early. However, because different conditions can produce similar uptake patterns, your result is most useful when interpreted alongside your clinical picture and other investigations. Risks And Side Effects Of A Bone Scan Radiation Exposure In A Bone Scan A bone scan involves a low level of radiation exposure. There is always some risk with any radiation, but the dose used is generally considered low in clinical practice, and serious side effects are uncommon. Injection-Related Side Effects Allergic reactions to radiotracers are described as extremely rare and usually mild. You may have temporary soreness or redness at the injection site. Is A Bone Scan Safe During Pregnancy Or Breastfeeding A developing fetus can be exposed to radiation, and radiotracer can pass into breast milk. If you are pregnant or breastfeeding, your doctor will advise whether the scan should be delayed, modified, or whether special precautions are needed. Bone Scan In Children And Older Adults Children may find it harder to stay still for imaging, and the team may use comfort measures and age-appropriate support. For older adults, the main challenge is often comfort during the waiting period and scan positioning. Tell the team if you have pain or mobility issues so they can help you stay as comfortable as possible. How Long Does A Bone Scan Take The full appointment time varies. The scan typically includes: A short visit for the injection A waiting period (commonly 2 to 4 hours) Imaging time that can range from around 30 minutes to longer depending on the protocol and whether extra images are required When To See A Doctor After A Bone Scan Contact your doctor promptly if you develop: Rash, swelling, or breathing difficulty after the injection Worsening pain, fever, or new symptoms while waiting for results Also follow up if you have not received your report within the timeframe your doctor advised. How Metropolis Healthcare Can Support Your Next Steps A bone scan is one part of the diagnostic picture. Your doctor may also want blood tests to understand bone health, inflammation, infection risk, or treatment response. Metropolis Healthcare supports this process with 4,000+ tests, including bone and mineral profiles, inflammatory markers, and other doctor-directed investigations, with accurate results and a quick turnaround time. If you need testing, you can book conveniently through the website, app, call centre, or WhatsApp. Metropolis also offers home sample collection, supported by a strong network of 10,000 touchpoints, which can be especially helpful if you are in pain or have limited mobility. Conclusion A bone scan is a widely used test that helps detect abnormal bone activity linked to injuries, infection, inflammation, and some cancers. The process is usually straightforward: an injection, a waiting period, and imaging with a special camera. Most people tolerate it well. If your scan shows an abnormal area, do not assume the worst. Many findings are treatable, and your doctor will guide the right next step based on your symptoms and any additional tests. FAQs Is A Bone Scan Painful The scan itself is usually painless. You may feel a brief pin-prick during the injection, and you may feel uncomfortable if you have pain and need to lie still. Is A Bone Scan Better Than An MRI It depends on the clinical question. A bone scan shows bone activity across the skeleton, while MRI provides very detailed images of bone marrow and soft tissues in a specific area. Your doctor chooses the test that best fits your symptoms. Can A Bone Scan Detect Cancer Early A bone scan can sometimes detect bone involvement earlier than standard X-rays because it highlights changes in bone turnover. However, it may not identify all cancer types, and abnormal uptake is not always cancer. What Is The Difference Between A Bone Scan And MRI A bone scan is a nuclear medicine test that maps bone activity, often across the whole body. MRI uses magnetic fields to give detailed structural images, usually focused on a specific region. Are Bone Scan Results Always Accurate Bone scans are sensitive, but they are not always specific. Many conditions can look similar, so additional tests may be needed to confirm the cause of an abnormal finding. References Van den Wyngaert T., Strobel K., Kampen W. U., et al. (2016). The EANM practice guidelines for bone scintigraphy. European Journal of Nuclear Medicine and Molecular Imaging, 43(9), 1723–1738. PMID: 27262701 Utsunomiya D., Shiraishi S., Imuta M., et al. (2006). Added Value of SPECT/CT Fusion in Assessing Suspected Bone Metastases: Comparison With Scintigraphy Alone And Scintigraphy Plus CT. Radiology, 238(1), 264–271. PMID: 16304081 Koppula B. R., Morton K. A., Al-Dulaimi R., et al. (2021). SPECT/CT In The Evaluation Of Suspected Skeletal Pathology. Tomography, 7(4), 581–605. PMID: 34698290 Adams C., Banks K. (2023). Bone Scan. StatPearls Publishing.