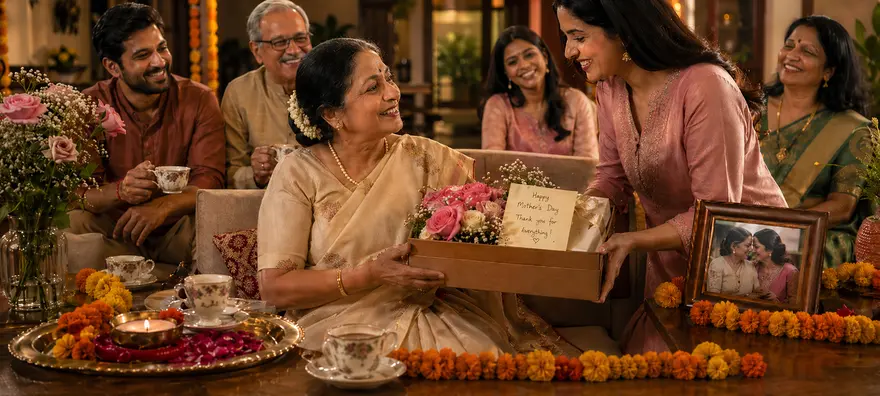Web Stories
Latest Blogs
International No Diet Day 2026: Key Health Tests To Check Metabolism, Thyroid And Nutrient Levels
International No Diet Day 2026 is a gentle reminder that your health is not defined by a number on the weighing scale. Celebrated every year on 6 May, the day encourages body respect, food freedom, and a healthier relationship with eating. This does not mean ignoring your health. It means moving away from guilt, restriction, and crash diets, and moving towards care, awareness, and informed choices. Instead of asking, “How quickly can I lose weight?”, International No Diet Day invites you to ask, “Is my body getting what it needs to function well?” That question is often better answered through your symptoms, lifestyle, medical history, and key health tests that check metabolism, thyroid function, blood sugar, cholesterol, and nutrient levels. What Is International No Diet Day? International No Diet Day is an annual health awareness day that promotes body acceptance, body diversity, and freedom from harmful diet culture. It is part of the wider body acceptance movement, which encourages you to treat your body with respect at every size. The day does not promote overeating or ignoring medical advice. It encourages a kinder, more practical approach to health. You can still eat balanced meals, move your body, manage a health condition, and monitor important health markers without following extreme food rules. When Is International No Diet Day 2026 Celebrated? International No Diet Day 2026 will be celebrated on Wednesday, 6 May 2026. The day is observed globally on 6 May every year. It is a good time to pause, reflect on your relationship with food, and choose habits that support your physical and mental wellbeing. International No Diet Day Theme 2026 There is no single official global International No Diet Day theme 2026 announced by one central body. However, the message remains clear: reject diet culture, respect your body, and focus on health without shame. A useful theme for 2026 can be: “Know Your Health, Not Just Your Weight.” This theme shifts the focus from appearance to real health markers such as thyroid function, blood sugar, cholesterol, iron levels, vitamin D, vitamin B12, and overall metabolic health. It also supports balanced diet awareness, where the aim is nourishment and consistency, not punishment or perfection. International No Diet Day History International No Diet Day was started in 1992 by Mary Evans Young, a British feminist and activist. She had personal experience with anorexia and wanted to challenge the pressure placed on people to look a certain way. The first observance was held in the United Kingdom. Over time, the day became an international movement that promoted body acceptance, awareness of eating disorders, and a shift away from unsafe dieting practices. Today, International No Diet Day history is closely linked with conversations around body image, mental health, food freedom, and sustainable wellbeing. Why International No Diet Day Is Important International No Diet Day matters because many people confuse weight loss with health. In reality, your health is shaped by many factors, including nutrition, sleep, stress, hormones, genetics, activity levels, and access to healthcare. This day encourages you to: Respect your body without waiting for it to look different. Avoid crash diets and extreme food rules. Build a healthier relationship with food. Focus on energy, strength, mood, sleep, and medical markers. Speak to a qualified professional for medical concerns. Choose prevention and regular health checks over guesswork. A balanced diet can support your health, but it does not need to be restrictive or fear based. Key Messages Promoted On This Day International No Diet Day promotes simple and meaningful health messages: Your weight is not your worth. Food should not be labelled as “good” or “bad”. Health looks different for different people. Extreme dieting can affect both body and mind. Preventive health screening can help you understand your body better. Eating well should be flexible, realistic, and enjoyable. Medical diets should be followed only when advised for a specific health condition. Body respect can support better health decisions. Risks Of Extreme Dieting Extreme dieting may look appealing because it promises quick results. But it can affect your body in several ways, especially when done without medical guidance. Possible risks include: Fatigue and weakness. Nutrient deficiencies. Dizziness or headaches. Constipation or digestive discomfort. Irregular periods in some people. Hair fall. Mood changes and irritability. Poor concentration. Increased cravings or binge eating. Loss of muscle mass. A cycle of weight loss and regain. Higher stress around food and body image. If you have diabetes, kidney disease, thyroid disease, heart disease, pregnancy, an eating disorder, or any long term medical condition, avoid major diet changes unless guided by your doctor or dietitian. Which Health Checks Support Healthy Weight And Wellness? Healthy weight management is not only about eating less. It is also about understanding how your body uses energy, processes sugar, stores nutrients, and responds to hormones. Your doctor may suggest some of the following tests based on your age, symptoms, family history, and health goals. 1. Thyroid Function Tests Your thyroid gland helps regulate metabolism, energy, body temperature, heart rate, digestion, and mood. Common thyroid tests include: TSH: Often used as the first screening test for thyroid function. Free T3 And Free T4: Help assess thyroid hormone levels in more detail. Thyroid Antibodies: May be advised if an autoimmune thyroid condition is suspected. You may benefit from discussing thyroid testing if you have unexplained fatigue, weight changes, constipation, hair fall, cold intolerance, palpitations, anxiety, or irregular periods. 2. Blood Sugar Tests Blood sugar tests help assess how your body handles glucose. Common tests include: Fasting Blood Sugar: Measures blood glucose after fasting. HbA1c: Shows average blood sugar levels over the past 2 to 3 months. Post Meal Blood Sugar: May be advised to check sugar response after food. These tests are especially useful if you have a family history of diabetes, frequent thirst, frequent urination, tiredness, slow wound healing, increased hunger, or unexplained weight changes. 3. Lipid Profile A lipid profile checks fats in your blood, including: Total cholesterol. LDL cholesterol. HDL cholesterol. Triglycerides. Cholesterol changes may not cause symptoms. That is why regular testing can help you understand your heart and metabolic health early. 4. Complete Blood Count A complete blood count, also called CBC, gives a basic picture of your blood health. It checks: Haemoglobin. Red blood cells. White blood cells. Platelets. Low haemoglobin can suggest anaemia, which may cause fatigue, weakness, dizziness, breathlessness, and poor stamina. These symptoms are sometimes mistaken for stress, ageing, or lack of fitness. 5. Iron And Ferritin Levels Iron helps your body make haemoglobin, which carries oxygen. Ferritin reflects stored iron. Low ferritin can sometimes appear before haemoglobin drops. Your doctor may suggest iron studies if you feel tired often, have heavy periods, follow a restrictive diet, or have symptoms of anaemia. 6. Vitamin D Test Vitamin D supports bones, muscles, nerves, and immune function. Low vitamin D can contribute to tiredness, muscle aches, bone discomfort, and low strength. A vitamin D test can help identify deficiency and guide safe supplementation if needed. 7. Vitamin B12 Test Vitamin B12 supports nerve function, blood cell formation, and energy metabolism. Low levels may cause fatigue, tingling, numbness, mouth ulcers, memory concerns, mood changes, or anaemia. People who follow vegetarian or vegan diets, older adults, and those with gut absorption issues may need closer monitoring. 8. Liver And Kidney Function Tests Your liver and kidneys help process nutrients, medicines, waste products, and fluids. Liver function tests and kidney function tests can support a clearer picture of your metabolic health, especially if you have diabetes, high blood pressure, long term medication use, alcohol intake, or a family history of liver or kidney disease. 9. Calcium, Magnesium And Electrolytes Calcium, magnesium, sodium, and potassium support muscle, nerve, heart, and fluid balance. Your doctor may suggest these tests if you have cramps, weakness, dehydration, kidney concerns, irregular heartbeat, or are taking certain medicines. Do These Tests Require Fasting? Not all health tests require fasting. Tests such as TSH, CBC, HbA1c, vitamin B12, and vitamin D often do not need fasting. Fasting blood sugar and some lipid profiles may need fasting, depending on your doctor’s advice and the laboratory protocol. Always follow the instructions given at the time of booking your test. How To Maintain A Healthy Weight Without Dieting You do not need extreme diets to care for your health. A realistic routine is often more effective. Try these simple steps: Eat regular meals instead of skipping food. Include vegetables, fruits, whole grains, pulses, nuts, seeds, dairy or alternatives, and good quality protein. Drink enough water through the day. Move in a way you enjoy, such as walking, dancing, cycling, yoga, swimming, or strength training. Sleep well, as poor sleep can affect hunger, cravings, mood, and metabolism. Manage stress through breathing, journalling, hobbies, prayer, meditation, or supportive conversations. Avoid comparing your body with others. Track health markers, not just weight. Seek professional advice if you feel stuck, tired, anxious, or unwell. This is where balanced diet awareness becomes useful. It helps you focus on nourishment, variety, and moderation rather than strict food rules. How To Celebrate International No Diet Day You can celebrate International No Diet Day in small but meaningful ways: Take a break from weighing yourself for the day. Avoid negative body talk. Unfollow social media accounts that make you feel ashamed of your body. Eat a meal you enjoy without guilt. Thank your body for what it helps you do every day. Choose joyful movement instead of punishment exercise. Have a kind conversation with a child or teen about food and body image. Book a preventive health check if you have been postponing it. Speak to a doctor or counsellor if food or body thoughts feel overwhelming. When Should You Seek More Support? Please speak to a healthcare professional if you notice: Constant worry about food, calories, or body size. Skipping meals often. Fear of eating certain foods without medical reason. Episodes of overeating with loss of control. Vomiting, laxative use, or over exercising to compensate for eating. Dizziness, fainting, palpitations, or menstrual changes. Sudden or unexplained weight change. Ongoing fatigue, weakness, or low mood. Eating disorders and disordered eating patterns are treatable. Early support can make recovery easier. Role Of Preventive Healthcare In Weight And Wellness Preventive healthcare helps you understand what is happening inside your body before problems become harder to manage. On International No Diet Day, this matters because many symptoms linked to “weight” may actually relate to thyroid imbalance, blood sugar changes, anaemia, vitamin deficiency, stress, poor sleep, or other health concerns. A full body checkup can give you a wider view of your health markers. It can help you and your doctor make better choices about nutrition, movement, sleep, supplementation, or treatment if needed. Stay Informed About Your Health With Metropolis Healthcare International No Diet Day 2026 is a reminder to treat your body with respect and care. Healthy living is not about punishing yourself. It is about understanding your body and supporting it well. Metropolis Healthcare makes preventive health screening simple and accessible with over 4,000 tests, full body checkups, thyroid profiles, vitamin tests, blood sugar tests, lipid profiles, liver and kidney function tests, and speciality testing. With NABL and CAP accredited laboratories, expert pathologists, accurate results, quick turnaround time, and a strong home sample collection network with 10,000 touchpoints, you can monitor your health with confidence. You can book easily through the website, app, call, or WhatsApp. Knowing your health markers can help you make kinder, smarter, and more personalised decisions for your wellbeing. Key Takeaways International No Diet Day is celebrated every year on 6 May. International No Diet Day 2026 falls on Wednesday, 6 May 2026. The day promotes body acceptance, food freedom, and respect for all body shapes and sizes. It does not reject health. It rejects shame based and extreme dieting. Metabolism, thyroid function, blood sugar, cholesterol, and nutrient levels can affect energy and wellness. Useful tests may include thyroid profile, HbA1c, fasting blood sugar, lipid profile, CBC, ferritin, vitamin D, vitamin B12, LFT, and KFT. Preventive testing can help you understand your body beyond the weighing scale. Sustainable health comes from nourishment, movement, sleep, stress care, medical guidance, and self respect. FAQs About International No Diet Day 2026 Who Started International No Diet Day? International No Diet Day was started by Mary Evans Young in 1992. She was a British activist who wanted to raise awareness about body acceptance, eating disorders, and the harm caused by diet pressure. How Can I Maintain A Healthy Weight Without Dieting? You can maintain a healthy weight by eating regular balanced meals, staying active, sleeping well, managing stress, drinking enough water, and monitoring health markers. Focus on habits you can follow consistently rather than strict short term rules. Where Was The First International No Diet Day Celebrated? The first International No Diet Day was celebrated in the United Kingdom in 1992. It later became a global awareness day observed on 6 May every year. Are All Diets Bad? No. Not all diets are bad. Some medical diets are necessary for conditions such as diabetes, kidney disease, coeliac disease, food allergies, or digestive disorders. The concern is with extreme, restrictive, or shame based diets followed without professional guidance.
World Ovarian Cancer Day 2026: Ovarian Cancer Tests, CA-125 And Early Diagnosis Signs
World Ovarian Cancer Day is observed every year to raise awareness about ovarian cancer, its symptoms, risk factors, and the importance of timely medical care. In 2026, this day continues to remind you that ovarian cancer symptoms can be easy to miss because they often feel like common digestive, urinary, or menstrual concerns. The purpose of this day is not to create fear. It is to help you listen to your body, notice persistent changes, and seek medical advice early. Awareness can support timely diagnosis, better treatment planning, and stronger emotional support for women and their families. What Is World Ovarian Cancer Day? World Ovarian Cancer Day is a global awareness day dedicated to ovarian cancer. It brings together healthcare professionals, survivors, caregivers, families, and awareness groups to speak openly about this serious women’s health condition. The day focuses on ovarian cancer symptoms awareness, early diagnosis, better access to care, and support for women affected by the disease. It also helps correct common myths, such as the belief that a Pap smear can detect ovarian cancer. A Pap smear screens for cervical cancer, not ovarian cancer. When Is World Ovarian Cancer Day 2026 Celebrated? World Ovarian Cancer Day 2026 will be observed on 8 May 2026. It is marked on 8 May every year. The day encourages women to learn about symptoms that should not be ignored, especially when they are new, persistent, or unusual for their body. World Ovarian Cancer Day 2026 Theme The World Ovarian Cancer Day 2026 theme is No Woman Left Behind. This theme highlights the need for fair access to ovarian cancer information, timely diagnosis, quality care, and emotional support for every woman. It also reminds healthcare systems and communities that symptoms should not be dismissed, delays should be reduced, and every woman deserves to be heard. World Ovarian Cancer Day History World Ovarian Cancer Day was first established in 2013 by ovarian cancer advocacy organisations from different parts of the world. The aim was to create one dedicated day for global awareness about a cancer that is often diagnosed late. Over the years, this day has become an important platform for education, survivor stories, community events, and public health campaigns. It has helped bring more attention to early warning signs, diagnostic challenges, and the need for better research. Why This Day Is Important World Ovarian Cancer Day is important because ovarian cancer can be difficult to detect early. Symptoms may be mild, vague, or similar to common health issues. Key reasons this day matters include: It encourages women to notice persistent symptoms. It improves awareness about early detection ovarian cancer. It explains why there is no routine screening test for average-risk women without symptoms. It highlights the role of medical evaluation, including CA-125 blood tests and ultrasound when advised. It supports women and families affected by ovarian cancer. It encourages open conversations about gynaecological health. It reminds women with family history to discuss their risk with a doctor. What Is Ovarian Cancer? Ovarian cancer is a cancer that starts in the ovaries, fallopian tubes, or nearby tissues. The ovaries are small organs in the pelvis that produce eggs and hormones such as oestrogen and progesterone. Ovarian cancer begins when abnormal cells grow in an uncontrolled way. If not detected and treated, these cells may spread to other parts of the body. There are different types of ovarian cancer. Epithelial ovarian cancer is the most common type. The exact treatment and outlook depend on the type, stage, overall health, and individual medical needs. Global Impact Of Ovarian Cancer Ovarian cancer has a major impact on women’s health worldwide. It is often diagnosed at a later stage because early symptoms may not be clear. Important points to know: It is one of the most serious gynaecological cancers. Many symptoms overlap with digestive or urinary problems. Delayed diagnosis can make treatment more complex. Awareness helps women seek medical advice sooner. Women with a family history of ovarian, breast, or colorectal cancer may need personalised risk assessment. Better awareness can help reduce stigma around discussing pelvic and menstrual symptoms. Common Awareness Messages Shared On This Day World Ovarian Cancer Day campaigns often focus on simple but important messages. Common awareness messages include: Do not ignore persistent bloating. Speak to a doctor if pelvic or abdominal pain continues. Notice changes in appetite, bowel habits, or urination. A Pap smear does not detect ovarian cancer. CA-125 is useful in evaluation but is not a standalone screening test for everyone. Family history matters. Early medical advice can make a difference. Support and compassion are important for every woman affected by ovarian cancer. Common Symptoms To Watch Ovarian cancer symptoms can be subtle. They may come and go at first. What matters most is persistence, frequency, and whether the symptoms are unusual for you. Common symptoms include: Persistent abdominal bloating or swelling Pelvic or abdominal pain Feeling full quickly while eating Difficulty eating your usual portion size Frequent urination Urgent need to urinate Unexplained weight loss Ongoing fatigue Constipation, diarrhoea, or other bowel changes Back pain Pain during sex Abnormal vaginal bleeding or discharge, especially after menopause You should speak to a doctor if these symptoms happen often, last for several weeks, or feel different from your usual health pattern. Who May Have A Higher Risk Of Ovarian Cancer? Anyone with ovaries can develop ovarian cancer. However, some factors may increase risk. You may have a higher risk if you have: A family history of ovarian, breast, or colorectal cancer Inherited gene changes such as BRCA1 or BRCA2 Age above 50 years Postmenopausal status Endometriosis Personal history of breast or bowel cancer Long-term hormone replacement therapy Infertility or no history of pregnancy Obesity or lifestyle-related health risks Having a risk factor does not mean you will develop ovarian cancer. It only means you may need a more personalised discussion with your doctor. Which Tests Are Done For Ovarian Cancer? There is no single test that can confirm ovarian cancer in all cases. Doctors usually use a combination of symptoms, examination, blood tests, imaging, and sometimes biopsy or surgery. Common evaluation methods include: Pelvic Examination: A doctor checks for swelling, tenderness, or unusual masses in the pelvic area. CA-125 Blood Test: CA-125 is a protein that may be higher in some women with ovarian cancer. However, CA-125 can also rise due to non-cancer conditions such as menstruation, endometriosis, pelvic inflammatory disease, fibroids, liver disease, or ovarian cysts. This is why the test is interpreted along with symptoms and imaging. Transvaginal Ultrasound: This imaging test helps doctors view the ovaries, uterus, and nearby structures. It can help identify cysts, masses, or other abnormalities. Abdominal Or Pelvic Ultrasound: This may be used to look at the pelvis and abdomen, especially if there is swelling or pain. CT Scan Or MRI: These imaging tests may help assess the size, location, and spread of a suspected tumour. PET Scan: In selected cases, this may help doctors understand whether cancer has spread. Biopsy Or Surgical Evaluation: A tissue diagnosis is usually needed to confirm cancer. In ovarian cancer, this may happen during surgery or through a carefully planned biopsy, depending on the case. A doctor may also advise a cancer test panel or other blood tests to understand your overall health before treatment planning. Can Ovarian Cancer Be Detected Early? Early detection can be difficult because ovarian cancer may not cause obvious symptoms in the beginning. Also, there is no reliable routine screening test for women without symptoms who are at average risk. This does not mean you are powerless. The most practical step is to pay attention to persistent symptoms and discuss them with a doctor early. Women with strong family history or known genetic risk may need closer monitoring, genetic counselling, or personalised testing plans. Why CA-125 Alone Is Not Enough CA-125 is a useful test, but it has limitations. A high CA-125 result does not always mean ovarian cancer. A normal CA-125 result also does not completely rule it out. This is because CA-125 levels can vary due to many reasons, including benign conditions. Doctors may use CA-125 to: Help evaluate symptoms Assess an ovarian mass Support diagnosis when combined with imaging Monitor response to treatment Watch for recurrence in women already treated for ovarian cancer It should not be used as a standalone test for self-diagnosis. Importance Of Early Detection And Screening Early detection ovarian cancer efforts mainly depend on awareness, risk-based assessment, and timely medical evaluation. Since routine screening is not recommended for every woman without symptoms, knowing your body becomes important. You should not wait for symptoms to become severe. If bloating, pelvic pain, appetite changes, or urinary urgency are frequent and persistent, seek medical advice. Routine women’s health check-ups also help you stay informed about your overall health. While they may not prevent ovarian cancer, they support better conversations about symptoms, family history, menstrual changes, and preventive care. How You Can Participate In World Ovarian Cancer Day You can support World Ovarian Cancer Day in simple ways. Learn the common symptoms and share them with women in your family. Talk openly about pelvic and menstrual health. Wear teal, the awareness colour for ovarian cancer. Share verified health information on social media. Encourage loved ones not to ignore persistent symptoms. Support women going through diagnosis or treatment. Ask about family health history. Book routine health check-ups as part of preventive care. Speak to a doctor if you have symptoms or risk factors. Small conversations can help someone seek help sooner. Role Of Preventive Healthcare In Women’s Health Preventive healthcare helps you stay aware of your body and health markers before problems become advanced. For women, this includes regular health check-ups, discussions about menstrual and pelvic symptoms, age-appropriate tests, and risk-based screening. A full body checkup can help you monitor important health markers such as blood sugar, thyroid function, liver function, kidney function, vitamin levels, and other wellness indicators. It does not replace ovarian cancer evaluation, but it supports proactive health management. Metropolis Healthcare makes preventive health monitoring simpler with 4,000 tests, full body health check-ups, speciality testing, expert pathologists, accurate reports, quick turnaround time, and convenient home sample collection. You can book through the website, app, call, or WhatsApp. With a strong home collection network and 10,000 touchpoints, Metropolis helps you stay informed about your health with ease and confidence. Key Takeaways World Ovarian Cancer Day 2026 will be observed on 8 May 2026. The World Ovarian Cancer Day 2026 theme is No Woman Left Behind. Ovarian cancer symptoms can look like common digestive or urinary issues. Persistent bloating, pelvic pain, early fullness, and urinary urgency should not be ignored. A Pap smear does not detect ovarian cancer. CA-125 is helpful but cannot diagnose ovarian cancer on its own. Ultrasound, imaging, examination, and tissue diagnosis may be needed. Women with family history should discuss risk assessment with a doctor. Awareness, timely medical advice, and preventive healthcare can support better health outcomes. FAQs About World Ovarian Cancer Day 2026 What Is The Slogan For Ovarian Cancer? A widely used awareness message for World Ovarian Cancer Day 2026 is No Woman Left Behind. It reflects the need for timely diagnosis, equal access to care, and support for every woman affected by ovarian cancer. How Can Ovarian Cancer Be Detected Early? Ovarian cancer may be detected earlier when persistent symptoms are recognised and evaluated promptly. Doctors may advise a pelvic examination, CA-125 blood test, transvaginal ultrasound, and other imaging tests based on your symptoms and risk factors. There is no reliable routine screening test for average-risk women without symptoms. When Should I Get Tested? You should speak to a doctor if you have persistent bloating, pelvic or abdominal pain, feeling full quickly, frequent urination, unexplained weight loss, fatigue, or abnormal bleeding. You should also seek medical advice if you have a strong family history of ovarian, breast, or colorectal cancer. Can A Pap Smear Detect Ovarian Cancer? No. A Pap smear screens for cervical cancer. It does not detect ovarian cancer. If you have symptoms that may suggest ovarian cancer, your doctor may advise other tests. Is CA-125 A Confirmatory Test For Ovarian Cancer? No. CA-125 is not confirmatory by itself. It may provide useful clues, but levels can rise due to many non-cancer conditions. Doctors interpret CA-125 along with symptoms, examination findings, ultrasound, and other tests. Are Ovarian Cysts Always Cancerous? No. Most ovarian cysts are benign, especially in younger women. However, persistent, complex, large, or postmenopausal cysts need medical evaluation and follow-up. Can Ovarian Cancer Happen After Menopause? Yes. Ovarian cancer is more common after menopause, especially after the age of 50. Any new bloating, pelvic pain, urinary changes, or postmenopausal bleeding should be discussed with a doctor.
Mother's Day 2026: Essential Health Checkups & Diagnostic Tests Every Woman Needs
Mother’s Day is a time to celebrate the women who care, support, guide, and strengthen families every day. In 2026, Mother’s Day will be celebrated on Sunday, May 10. While flowers, cards, meals, and thoughtful gifts are lovely ways to show love, one of the most meaningful Mother’s Day gifts ideas is the gift of health. Many women put their health last while caring for others. They may ignore tiredness, body pain, irregular periods, mood changes, poor sleep, or weight changes because daily life feels too busy. Regular health checkups can help detect hidden concerns early, even before symptoms become clear. This Mother’s Day 2026, you can make the celebration more meaningful by encouraging your mother, grandmother, wife, sister, daughter, or yourself to take a proactive step towards better health. What Is Mother’s Day? Mother’s Day is a special day dedicated to honouring mothers and mother figures. It celebrates their love, care, sacrifices, strength, and role in shaping families and communities. For many people, Mother’s Day is about gratitude. It is a day to pause, spend time together, and remind mothers that their wellbeing matters too. When Is Mother’s Day 2026 Celebrated? Mother’s Day 2026 will be celebrated on Sunday, May 10. In many countries, including India and the United States, Mother’s Day is observed on the second Sunday of May every year. The date changes each year, but the meaning remains the same: celebrating mothers with love, respect, and care. History And Origin Of Mother’s Day The modern history of Mother’s Day is often linked to Anna Jarvis in the United States. She wanted to honour her mother and recognise the contribution of mothers to families and society. In 1908, the first formal Mother’s Day service was held, and in 1914, Mother’s Day became an official national observance in the United States. Over time, Mother’s Day became popular across many countries. Today, people celebrate it through gifts, family gatherings, handwritten notes, meals, phone calls, and other thoughtful gestures. Why Mother’s Day Is Important Mother’s Day is important because it reminds you to: Appreciate the emotional, physical, and mental effort mothers put into family life Recognise that women’s health often gets ignored due to caregiving responsibilities Encourage mothers to take time for rest, joy, and self-care Start open conversations about preventive health and regular checkups Celebrate not only motherhood, but also the woman behind the role A meaningful Mother’s Day theme for 2026 can be simple: care for the one who has always cared for you. Common Ways To Celebrate Mother’s Day There are many simple ways to celebrate Mother’s Day with warmth and thoughtfulness: Spend quality time with your mother or mother figure Cook her favourite meal or take her out for a relaxed meal Write a personal letter or card Plan a family video call if you live away Gift her something useful and thoughtful Create a memory album with family photos Help her take a break from daily responsibilities Book a preventive health checkup for her comfort and peace of mind Among the many ways to celebrate Mother’s Day, supporting her health can be one of the most lasting gestures. Health And Wellness For Mothers Women’s health changes through different life stages. Hormones, pregnancy, childbirth, menopause, stress, nutrition, sleep, and lifestyle can all affect health. Common health concerns in women may include: Anaemia Thyroid disorders Vitamin D or vitamin B12 deficiency Diabetes or prediabetes High cholesterol High blood pressure PCOS Fibroids Breast health concerns Cervical health concerns Bone weakness after menopause Heart health risks Many of these conditions can be managed better when detected early. That is why preventive checkups are important, even when you feel well. Which Health Tests Are Recommended For Women? The right tests depend on age, symptoms, lifestyle, medical history, family history, and your doctor’s advice. However, the following checkups are commonly useful for women. 1. Blood Pressure Check High blood pressure can remain silent for years. Regular monitoring helps assess the risk of heart disease, kidney problems, and stroke. You may need more frequent checks if you have diabetes, obesity, stress, kidney disease, or a family history of hypertension. 2. Complete Blood Count A complete blood count, or CBC, helps check haemoglobin, white blood cells, red blood cells, and platelets. It can help detect anaemia, infections, inflammation, and some blood-related concerns. This test is especially useful if you often feel tired, weak, dizzy, breathless, or have heavy periods. 3. Blood Sugar Tests Fasting blood sugar and HbA1c help screen for diabetes and prediabetes. Women with PCOS, excess weight, a sedentary lifestyle, previous gestational diabetes, or a family history of diabetes may need regular screening. Early detection can help you make timely changes in food habits, activity, weight, and treatment. 4. Lipid Profile A lipid profile checks cholesterol and triglyceride levels. It usually includes total cholesterol, LDL cholesterol, HDL cholesterol, and triglycerides. Heart disease can affect women too, and risk may rise after menopause. A lipid profile helps assess heart health and supports early prevention. 5. Thyroid Profile Thyroid disorders are more common in women. A thyroid profile may include TSH, T3, and T4. It can help detect hypothyroidism or hyperthyroidism. You may need this test if you have weight changes, hair fall, irregular periods, tiredness, constipation, anxiety, palpitations, or fertility concerns. 6. Vitamin D And Vitamin B12 Tests Low vitamin D and vitamin B12 levels can contribute to fatigue, bone pain, muscle weakness, low mood, tingling, numbness, and poor energy. These deficiencies are common and can often be corrected with the right medical guidance. 7. Liver And Kidney Function Tests Liver and kidney function tests help assess how well these important organs are working. They are often included in routine health packages and are useful for ongoing wellness monitoring. These tests may be especially important if you take long-term medicines, have diabetes, high blood pressure, or a family history of kidney or liver disease. 8. Pap Smear And HPV Test Cervical cancer screening helps detect early changes in the cervix. A Pap smear checks for abnormal cervical cells. An HPV test checks for high-risk human papillomavirus types linked to cervical cancer. Your doctor can guide you on the right screening schedule based on your age, sexual history, previous reports, and risk factors. 9. Breast Screening Breast health checks may include breast self-awareness, clinical breast examination, ultrasound, or mammography, depending on age and risk. Women aged 40 and above may be advised to discuss mammography with their doctor. Screening may start earlier if there is a strong family history or other risk factors. 10. Pelvic Ultrasound A pelvic ultrasound can help assess the uterus, ovaries, and surrounding structures. It may help detect fibroids, ovarian cysts, PCOS-related changes, endometrial concerns, and other gynaecological conditions. It may be recommended if you have irregular periods, heavy bleeding, pelvic pain, bloating, or fertility concerns. 11. Bone Health Tests Bone density can reduce after menopause due to hormonal changes. A DEXA scan may be advised for women after menopause or earlier if there are risk factors such as repeated fractures, long-term steroid use, low body weight, or vitamin D deficiency. Calcium, vitamin D, and other related tests may also support bone health assessment. 12. Heart Health Tests Apart from blood pressure and lipid profile, your doctor may advise ECG, hs-CRP, 2D echo, or other cardiac tests based on your symptoms and risk profile. This is more relevant if you have chest discomfort, breathlessness, diabetes, high blood pressure, high cholesterol, obesity, smoking history, or a family history of heart disease. 13. Full Body Health Checkup A full body checkup can help you review key health markers in one place. It may include blood counts, sugar levels, cholesterol, liver function, kidney function, thyroid profile, urine tests, vitamin levels, and other tests based on the package. It is a practical option for mothers who have not had routine health screening for a long time. Age-Wise Health Checkups For Women In Your 20s This is the time to build a health baseline. Useful checks may include: CBC Blood pressure Blood sugar if risk factors are present Thyroid profile if symptoms are present Vitamin D and B12 STI screening when relevant Pap smear as advised by your doctor PCOS assessment if periods are irregular In Your 30s This is often a busy stage with work, family, pregnancy, parenting, and stress. Useful checks may include: CBC Thyroid profile Blood sugar and HbA1c Lipid profile Liver and kidney function tests Vitamin D and B12 Pap smear or HPV test as advised Pelvic ultrasound if symptoms are present Breast examination In Your 40s Health risks may begin to rise in this decade, especially with stress, weight changes, hormonal shifts, and family history. Useful checks may include: Blood pressure CBC HbA1c Lipid profile Thyroid profile Liver and kidney function tests Pap smear or HPV test Breast screening Pelvic ultrasound if needed ECG if risk factors are present In Your 50s Menopause and post-menopause can affect bones, heart health, metabolism, sleep, and mood. Useful checks may include: Blood pressure Blood sugar and HbA1c Lipid profile Thyroid profile Bone density test if advised Vitamin D and calcium assessment Breast screening Cervical screening as advised Heart health evaluation Kidney and liver function tests In Your 60s And Beyond The focus is on maintaining strength, independence, mobility, and quality of life. Useful checks may include: Blood pressure monitoring Diabetes screening Lipid profile Kidney and liver function tests Bone density testing Eye and hearing checks Breast screening as advised Heart health tests Vitamin levels Cancer screening based on medical advice How To Make Mother’s Day Meaningful You do not need a grand plan to make Mother’s Day special. Thoughtfulness matters more than cost. You can: Spend uninterrupted time with her Ask about her health and listen without dismissing her concerns Help her schedule a long-pending health checkup Create a calm day with rest, food, and family time Gift a wellness package, comfortable footwear, fitness tracker, or health journal Encourage her to restart a hobby Join her for a walk, yoga class, or doctor visit Make preventive health part of the family conversation Unique gift ideas can include a memory book, a handwritten letter, a home-cooked meal, a relaxing wellness day, or a preventive health screening package. Role Of Preventive Healthcare For Mothers Preventive healthcare is not only about finding illness. It is about staying informed, building healthy habits, and reducing future risks. For mothers, regular health checkups can help detect changes in blood sugar, cholesterol, thyroid function, vitamin levels, haemoglobin, bone health, and organ function. This gives you and your doctor a clearer picture of health before problems become serious. Metropolis Healthcare supports proactive health management with advanced diagnostic testing, 4,000 plus tests, full body health checkups, speciality testing, accurate results, quick turnaround time, and home sample collection. With easy booking through the website, app, call, and WhatsApp, you can help your mother prioritise her health with comfort and convenience. This Mother’s Day 2026, celebrate her love by supporting her wellbeing. Key Takeaways Mother’s Day 2026 will be celebrated on Sunday, May 10. The modern history of Mother’s Day is linked to Anna Jarvis and her wish to honour mothers. A meaningful Mother’s Day theme can focus on health, gratitude, and preventive care. Women should not wait for symptoms to begin routine health screening. Important tests may include CBC, blood sugar, HbA1c, lipid profile, thyroid profile, vitamin D, vitamin B12, Pap smear, HPV test, breast screening, pelvic ultrasound, and bone health tests. The right tests depend on age, symptoms, medical history, lifestyle, and doctor’s advice. A health checkup can be a thoughtful and practical Mother’s Day gift. FAQs About Mother’s Day 2026 Why Is Mother’s Day So Early In 2026? Mother’s Day is not unusually early in 2026. It falls on Sunday, May 10, because many countries celebrate it on the second Sunday of May. The exact date changes every year depending on the calendar. Who Started Mother’s Day? The modern Mother’s Day tradition is linked to Anna Jarvis. She organised a Mother’s Day observance in 1908 to honour her mother. The day later became an official observance in the United States in 1914. How Can I Make Mother’s Day Special? You can make Mother’s Day special by spending quality time with your mother, writing a heartfelt note, cooking for her, planning a relaxed family day, or helping her prioritise her health with a preventive checkup. What Are Some Unique Gift Ideas? Unique Mother’s Day gifts ideas include a memory album, handwritten letter, wellness hamper, comfortable walking shoes, hobby class, family experience, health journal, or preventive health checkup. Which Health Checkup Is Best For Mothers? There is no single best health checkup for every mother. A suitable package depends on age, symptoms, lifestyle, family history, and existing health conditions. Common tests include CBC, blood sugar, HbA1c, lipid profile, thyroid profile, vitamin levels, liver function, kidney function, and urine routine tests. Are Health Checkups Needed If There Are No Symptoms? Yes, routine screening can still be useful because conditions such as high blood pressure, diabetes, high cholesterol, anaemia, thyroid disorders, and vitamin deficiencies may not cause clear symptoms in the early stages. When Should Women Start Breast Screening? Women should discuss breast screening with their doctor based on age and risk. Many guidelines recommend mammography from age 40 for average-risk women, while women with a family history or higher risk may need earlier or more personalised screening. How Often Should Women Get A Thyroid Test? The frequency depends on symptoms, medical history, pregnancy plans, age, and previous thyroid results. Your doctor may advise testing if you have fatigue, weight changes, hair fall, irregular periods, palpitations, or mood changes.
World Lupus Day 2026: Lupus Diagnosis, ANA Test And Symptoms You Shouldn’t Ignore
World Lupus Day is observed every year to help more people understand lupus, a chronic autoimmune disease that is often difficult to recognise. Lupus can affect the skin, joints, kidneys, lungs, heart, blood cells, brain and other parts of the body. Its symptoms may look like many other health conditions, which is why it is sometimes called “the great imitator”. World Lupus Day 2026 is an important reminder to learn the early signs, seek timely medical advice and understand the role of diagnostic tests such as the ANA test. While lupus cannot be diagnosed with one test alone, the right combination of clinical evaluation and lab tests can help doctors reach a clearer diagnosis. What Is World Lupus Day? World Lupus Day is a global awareness day observed on 10 May every year. It brings attention to lupus, its symptoms, its impact on daily life and the need for timely diagnosis and better care. The day also helps reduce stigma around autoimmune diseases. Many people living with lupus may look well on the outside but experience fatigue, pain, flare-ups and organ-related complications. Awareness helps families, workplaces and communities become more understanding and supportive. When Is World Lupus Day 2026 Celebrated? World Lupus Day 2026 will be observed on Sunday, 10 May 2026. May is also recognised as Lupus Awareness Month in many parts of the world. During this month, organisations, healthcare experts and communities share information about lupus symptoms awareness, early detection lupus, patient support and ongoing research. World Lupus Day Theme 2026 The World Lupus Day theme 2026 is Make Lupus Visible. This theme focuses on making the unseen impact of lupus better understood. Lupus symptoms can come and go. They may not always be obvious to others. The theme encourages people to talk openly about symptoms, support those living with lupus and promote early diagnosis. The broader world lupus day theme also reminds you that better awareness can lead to earlier medical attention, better monitoring and improved quality of life. World Lupus Day History World Lupus Day was established in 2004 to unite lupus organisations across the world and raise awareness about the physical, emotional, social and economic impact of lupus. Since then, 10 May has become a global day of education and advocacy. People wear purple, share awareness messages, take part in campaigns and support those affected by lupus. Why This Day Is Important World Lupus Day matters because it helps: Improve public understanding of lupus Encourage people to recognise early symptoms Reduce delay in diagnosis Support people living with chronic autoimmune symptoms Highlight the importance of research and better treatment options Promote regular health monitoring for people at risk Reduce myths, fear and stigma around lupus What Is Lupus? Lupus is a chronic autoimmune disease. In autoimmune diseases, your immune system mistakenly attacks your own healthy tissues. This can cause inflammation, pain and damage in different parts of the body. The most common type is systemic lupus erythematosus, often called SLE. It can affect many organs and body systems. Lupus can be mild in some people and more serious in others. Symptoms may appear in phases. A period when symptoms worsen is called a flare. A period when symptoms improve is called remission. Common Lupus Symptoms You Shouldn’t Ignore Lupus symptoms can vary from person to person. They may develop slowly, appear suddenly or come and go over time. Common symptoms include: Extreme fatigue that does not improve with rest Joint pain, swelling or stiffness A butterfly-shaped rash across the cheeks and nose Skin rashes that worsen after sun exposure Unexplained fever Hair thinning or patchy hair loss Mouth or nose ulcers Chest pain while taking a deep breath Swelling in the feet, legs or around the eyes Fingers or toes turning white, blue or numb in cold or stress Headaches, confusion or memory problems Unexplained anaemia or low blood cell counts These symptoms do not always mean you have lupus. However, if they are persistent, recurrent or affecting your daily life, you should speak to a doctor. When Should You See A Doctor? You should seek medical advice if you notice: Ongoing fatigue with no clear reason Repeated joint pain or swelling Skin rashes after sunlight exposure Unexplained fever Swelling around the eyes or legs Blood or protein detected in urine Frequent mouth ulcers Chest pain while breathing deeply Symptoms that come in flares Seek urgent medical care if you have severe chest pain, severe breathlessness, seizures, sudden weakness, confusion or symptoms that feel like a medical emergency. Which Tests Are Done For Lupus? There is no single test that confirms lupus on its own. Doctors usually diagnose lupus by combining your symptoms, physical examination, medical history and lab test results. Common tests include: ANA Test: The antinuclear antibody test checks for antibodies that may attack your own cells. Most people with lupus have a positive ANA test, but a positive ANA does not always mean lupus. Anti-dsDNA Test: This test looks for antibodies that are more specific to lupus and may also help assess kidney involvement. Anti-Sm Antibody Test: This is another specific antibody test that may support a lupus diagnosis. Complete Blood Count: This checks for anaemia, low white blood cells or low platelets. ESR And CRP: These tests help assess inflammation in the body. Urine Routine And Microscopy: This helps detect protein, blood cells or other signs of kidney involvement. Kidney Function Tests: These assess how well your kidneys are working. Complement Tests: C3 and C4 levels may be checked because they can fall during active lupus. Liver Function Tests: These may be done to assess overall health and treatment safety. Kidney Biopsy: This may be advised if lupus nephritis is suspected. If your doctor advises an ANA test, you may also want to understand the ana test price and whether follow-up autoimmune tests may be needed based on your result. What Does A Positive ANA Test Mean? A positive ANA test means antinuclear antibodies are present in your blood. These antibodies may be linked with autoimmune activity. However, a positive ANA test does not confirm lupus by itself. Some healthy people may also have a positive ANA result. ANA can also be positive in other autoimmune diseases, infections or due to certain medicines. This is why doctors do not rely on ANA alone. They look at your symptoms, examination findings and other specific tests before making a diagnosis. Why Early Detection Of Lupus Matters Early detection lupus can help reduce the risk of complications. Lupus can affect important organs such as the kidneys, heart, lungs and brain. When it is recognised early, your doctor can monitor your health closely and start the right treatment plan. Timely diagnosis can help: Reduce flare frequency Protect kidney health Manage joint and skin symptoms better Lower the risk of organ damage Improve energy and daily functioning Support safer treatment decisions Improve quality of life If you have repeated symptoms that do not have a clear cause, do not ignore them. Early medical evaluation can make a meaningful difference. Global Impact Of Lupus Lupus affects people across the world. Its impact can be physical, emotional and social. Key facts include: Lupus is an autoimmune disease, not an infection It is not contagious It affects women more commonly than men Symptoms can vary widely from person to person Diagnosis may take time because symptoms can mimic other diseases Lupus may affect work, studies, relationships and mental well-being With proper care, many people with lupus can manage symptoms and live active lives Common Awareness Messages Shared On World Lupus Day On World Lupus Day, awareness campaigns often focus on simple and helpful messages such as: Lupus is real, even when symptoms are not visible Lupus is not contagious Early diagnosis can help prevent complications Fatigue in lupus is more than normal tiredness Sunlight can trigger symptoms in some people Kidney involvement may occur silently Regular monitoring is important Support and understanding can improve daily life for people with lupus How You Can Participate In World Lupus Day You can support World Lupus Day 2026 in simple ways: Wear purple on 10 May Share reliable lupus awareness posts Learn the common symptoms of lupus Encourage someone with persistent symptoms to seek medical advice Support people living with lupus with patience and empathy Avoid spreading myths or unverified health claims Join community awareness activities Talk about preventive health and regular checkups Help make invisible symptoms visible through kind conversations Role Of Preventive Healthcare In Autoimmune Diseases Preventive healthcare cannot always prevent autoimmune diseases, but it can help you stay informed about your health. Regular health checks can identify changes in blood counts, inflammation markers, kidney function, liver function, vitamin levels and other important health markers. For people with symptoms, a timely evaluation helps doctors decide whether autoimmune testing is needed. For people already diagnosed with lupus or another autoimmune condition, regular monitoring helps track disease activity and treatment safety. A full body checkup can also help you understand your overall health better, especially when combined with medical advice and symptom review. Living With Lupus: Practical Self-Care Tips Lupus care is personalised. Your doctor may recommend medicines, lifestyle changes and regular monitoring based on your symptoms and organ involvement. General self-care tips include: Take medicines exactly as prescribed Avoid stopping treatment without medical advice Protect your skin from harsh sunlight Get adequate rest Eat balanced meals Stay physically active as advised by your doctor Track your symptoms and flare triggers Attend regular follow-ups Manage stress with healthy coping methods Report new symptoms early These habits do not replace medical treatment, but they can support better disease management. Key Takeaways World Lupus Day 2026 will be observed on 10 May 2026. The World Lupus Day theme 2026 is Make Lupus Visible. Lupus is a chronic autoimmune disease that can affect many organs. Common symptoms include fatigue, joint pain, butterfly rash, fever, hair loss, mouth ulcers and swelling. The ANA test can support evaluation, but it cannot diagnose lupus alone. Doctors use symptoms, examination and multiple lab tests to diagnose lupus. Early diagnosis and regular monitoring can help reduce complications. Preventive healthcare and routine testing can help you stay aware of your health markers. Conclusion World Lupus Day 2026 is a reminder to listen to your body and take persistent symptoms seriously. Lupus can be complex, but timely diagnosis, regular monitoring and the right medical support can help you manage it better. Metropolis Healthcare supports proactive health management with 4,000 tests, accurate results, expert pathologists, quick turnaround time and convenient home sample collection. You can book tests through the website, app, call or WhatsApp, and access reliable reports to stay informed about your health. Whether you are checking symptoms, monitoring an existing condition or planning preventive health screening, Metropolis can be your trusted diagnostics partner. FAQs About World Lupus Day 2026 What Country Has The Most Lupus? Lupus is reported worldwide, but exact numbers vary because diagnosis, reporting systems and access to healthcare differ by country. Some studies show higher lupus burden in certain populations, including women and people of African, Asian, Hispanic and Indigenous ancestry. No single country can be named with certainty as having the most lupus without consistent global data. When Is Wear Purple Day For Lupus? People commonly wear purple on 10 May for World Lupus Day. Purple is used as a symbol of lupus awareness and support for people living with the condition. When Should I Get Tested? You should speak to a doctor if you have repeated or unexplained symptoms such as extreme fatigue, joint pain, swelling, butterfly rash, sunlight sensitivity, mouth ulcers, fever, hair loss or swelling around the eyes or legs. Your doctor may advise an ANA test and other tests based on your symptoms. Can Lupus Be Cured? There is no known cure for lupus at present. However, treatment can help control symptoms, reduce flares and lower the risk of complications. Many people with lupus manage the condition well with medical care and regular monitoring. Is Lupus Contagious? No. Lupus is not contagious. You cannot catch it from another person through touch, food, air or close contact. Is ANA Positive Always Lupus? No. A positive ANA test does not always mean you have lupus. ANA may be positive in other autoimmune conditions and sometimes in healthy people. Your doctor will interpret the result along with symptoms and other tests.
International Nurses Day 2026: Importance Of Preventive Health Checkups And Routine Blood Tests
International Nurses Day 2026 is a meaningful reminder to honour nurses for their skill, compassion, and constant service. Nurses care for people during some of their most difficult moments. They support treatment, comfort families, assist doctors, guide patients, and help keep healthcare systems running. This year also brings attention to an important message: Nurses need care too. Preventive health checkups, routine blood tests, rest, emotional support, and healthy habits can help nurses protect their own well-being while they continue to care for others. What Is International Nurses Day? International Nurses Day is a global observance held every year to recognise the contribution of nurses to society. It celebrates their role in patient care, health education, disease prevention, and public health. It is more than a nursing awareness day. It is a moment to understand the importance of nurses in healthcare and the need to support them with respect, safe work environments, and better health resources. When Is International Nurses Day 2026 Celebrated? International Nurses Day 2026 will be celebrated on Tuesday, 12 May 2026. The date is observed every year on 12 May, the birth anniversary of Florence Nightingale, who is widely regarded as the founder of modern nursing. International Nurses Day 2026 Theme The International Nurses Day 2026 theme is: Our Nurses. Our Future. Empowered Nurses Save Lives. This theme highlights a simple but powerful idea. When nurses are supported, respected, protected, and empowered, they can deliver better care and help save more lives. Empowerment also includes their own health. Nurses often work long shifts, spend hours on their feet, manage emotional pressure, and care for people with infections or serious illnesses. Preventive health checkups and routine blood tests can help them stay aware of their health markers and act early when needed. History And Origin Of International Nurses Day The International Council of Nurses has celebrated International Nurses Day since 1965. In 1974, 12 May was chosen as the official date to honour Florence Nightingale’s birth anniversary. Florence Nightingale changed the way nursing was viewed. Her work during the Crimean War and her focus on hygiene, patient care, and training helped shape modern nursing. Today, International Nurses Day recognises nurses across specialities, from critical care and emergency care to maternity, community health, paediatrics, elderly care, mental health, and preventive care. Why Nurses Are Important In Healthcare Nurses are often the first point of contact for patients. Their work affects comfort, recovery, safety, and trust. They play an important role by: Monitoring vital signs and symptoms Giving medicines and supporting treatment plans Assisting doctors during procedures Educating patients about medicines, tests, diet, and recovery Supporting families with clear and calm communication Helping patients feel safe during illness or treatment Identifying warning signs early Promoting hygiene, infection control, and preventive care The importance of nurses in healthcare goes beyond medical tasks. They bring skill, empathy, observation, and emotional strength to patient care every day. Why Preventive Health Checkups Matter For Nurses Nurses care for others every day, but they may delay their own health needs due to busy schedules. Preventive health checkups can help them stay informed and take timely action. Regular screening can support nurses by helping with: Early detection of diabetes, high cholesterol, anaemia, thyroid problems, liver concerns, kidney issues, and vitamin deficiencies Better management of stress-related health concerns Monitoring blood pressure, weight, sleep, and energy levels Identifying fatigue linked to anaemia, vitamin B12 deficiency, vitamin D deficiency, or thyroid imbalance Reducing the risk of long-term complications through early care Supporting a healthier and more sustainable nursing workforce Preventive care does not mean expecting illness. It means staying aware, prepared, and proactive. Routine Blood Tests Nurses Should Consider The right tests may vary based on age, symptoms, family history, lifestyle, and doctor’s advice. However, the following routine blood tests are commonly useful for preventive health monitoring. Complete Blood Count A complete blood count, also called CBC, gives information about red blood cells, white blood cells, haemoglobin, and platelets. It can help detect anaemia, infections, inflammation, and other blood-related concerns. For nurses who often deal with fatigue, long shifts, and exposure to infections, CBC can be a useful part of routine screening. Blood Glucose And HbA1c Blood glucose tests and HbA1c help assess sugar levels. HbA1c reflects average blood sugar levels over about three months. These tests can help detect prediabetes or diabetes early. This matters because early lifestyle changes and medical care can make a big difference. Lipid Profile A lipid profile measures cholesterol and triglyceride levels. It helps assess heart health risk. Nurses may experience irregular meals, stress, disrupted sleep, and limited time for exercise. A lipid profile can help them understand their cardiovascular health better. Liver Function Test A liver function test checks markers linked to liver health. It may be useful for routine health monitoring, especially if you have symptoms, take long-term medicines, or have metabolic risk factors. Kidney Function Test A kidney function test usually checks markers such as creatinine and urea. It helps assess how well the kidneys are working. Since blood pressure, diabetes, dehydration, and certain medicines can affect kidney health, this test can be useful in preventive screening. Thyroid Profile A thyroid profile checks thyroid hormone levels. Thyroid imbalance can affect energy, weight, mood, sleep, menstrual health, and heart rate. Since symptoms can be subtle, testing can help identify concerns early. Vitamin D And Vitamin B12 Vitamin D and vitamin B12 deficiencies can contribute to tiredness, weakness, low mood, muscle pain, tingling, and poor bone health. Nurses who work indoors for long hours or follow restricted diets may benefit from checking these levels when appropriate. Role Of Nurses In Preventive Healthcare Nurses do not only care for people when they are unwell. They also help people prevent illness and manage risk factors. Their role includes: Educating patients about healthy habits Encouraging vaccination and regular screening Explaining test preparation and follow-up steps Helping patients understand warning signs Supporting chronic disease management Guiding patients on medicine adherence Promoting hygiene and infection prevention Helping communities understand preventive care In many cases, nurses are the reason patients feel confident enough to complete tests, ask questions, and follow care plans. Health Awareness And Diagnostic Support By Nurses Nurses play a key role in diagnostic support. They help make testing easier, safer, and less stressful for patients. They may support diagnostic care by: Preparing patients before tests Explaining why a test may be needed Helping with sample collection processes Monitoring patients before and after procedures Checking patient history and symptoms Coordinating with doctors and lab teams Guiding patients about reports and next steps This makes nurses important partners in early detection, preventive care, and better treatment outcomes. How To Celebrate International Nurses Day 2026 You can celebrate International Nurses Day in simple and meaningful ways. Thank a nurse who has helped you or your family Share a thoughtful message of appreciation Support nurse well-being initiatives at your workplace Organise health checkups for nursing staff Encourage rest breaks and mental health support Host awareness sessions on preventive healthcare Recognise nurses across departments and specialities Use this nursing awareness day to talk about safer and healthier workplaces The best celebration is not only praise. It is action that supports nurses every day. How Patients Can Support Healthcare Workers As a patient or family member, your behaviour can make a difference. You can support nurses and healthcare workers by: Speaking respectfully, even when you are anxious Following instructions clearly Sharing accurate health history Being patient during busy hours Avoiding misinformation Asking questions calmly Appreciating their effort Following hygiene and safety rules Encouraging loved ones to cooperate during care Kindness helps create a better healing environment for everyone. Preventive Health Tips For Nurses Small, consistent habits can help nurses protect their health. Eat regular, balanced meals when possible Stay hydrated during shifts Use comfortable footwear Take short stretch breaks Prioritise sleep after long shifts Keep vaccinations updated Monitor blood pressure and blood sugar if at risk Seek help for stress, anxiety, or burnout Schedule routine blood tests and health checkups Do not ignore ongoing fatigue, pain, dizziness, or mood changes Caring for yourself is not selfish. It helps you care for others with more strength and clarity. Key Takeaways International Nurses Day 2026 will be celebrated on 12 May 2026. The International Nurses Day 2026 theme is “Our Nurses. Our Future. Empowered Nurses Save Lives.” Nurses are essential to patient care, preventive health, diagnosis, treatment, and recovery. Preventive health checkups help nurses monitor their own health and act early. Routine blood tests such as CBC, HbA1c, lipid profile, liver function, kidney function, thyroid profile, vitamin D, and vitamin B12 can support overall health monitoring. Patients can support nurses through respect, cooperation, and gratitude. A healthier nursing workforce supports a stronger healthcare system. Conclusion International Nurses Day 2026 is a time to honour nurses and also remind them that their health matters. Nurses spend their lives supporting others, but their own preventive care, routine screening, and emotional well-being deserve equal attention. Metropolis Healthcare supports proactive health management with accurate diagnostic services, 4,000+ tests, full body checkup options, speciality testing, and convenient home sample collection. With NABL and CAP-accredited labs, expert pathologists, quick turnaround time, and easy booking through the website, app, call, and WhatsApp, Metropolis makes routine health monitoring simpler and more accessible. This International Nurses Day, let us thank nurses not only with words, but also by supporting their health, dignity, and well-being. FAQs About International Nurses Day 2026 Who Started International Nurses Day? International Nurses Day was started by the International Council of Nurses. The day has been celebrated since 1965, and 12 May was chosen in 1974 to honour Florence Nightingale’s birth anniversary. How Do Nurses Support Diagnostic Testing? Nurses support diagnostic testing by preparing patients, explaining test procedures, assisting with sample collection, monitoring patient comfort, recording symptoms, coordinating with doctors, and helping patients understand follow-up steps. Their guidance makes testing less stressful and more effective. What Is The International Nurses Day 2026 Theme? The International Nurses Day 2026 theme is “Our Nurses. Our Future. Empowered Nurses Save Lives.” It highlights the need to support and empower nurses so they can continue to deliver safe, compassionate, and effective care. Why Are Preventive Health Checkups Important For Nurses? Preventive health checkups help nurses monitor key health markers, detect concerns early, and manage risk factors before they become serious. They are especially helpful because nursing can involve long shifts, stress, physical strain, and exposure to infections. Which Routine Blood Tests Are Useful For Nurses? Commonly useful tests include CBC, blood glucose, HbA1c, lipid profile, liver function test, kidney function test, thyroid profile, vitamin D, and vitamin B12. The exact tests and frequency should depend on age, health history, symptoms, and medical advice.
STD Symptoms in Women: What You Should Know
Sexually transmitted diseases (STDs), also called sexually transmitted infections (STIs), are more common than many people realise. They are caused by bacteria, viruses, or parasites that pass from one person to another through sexual contact. In women, these infections can be easy to overlook because the symptoms are often mild, vague, or absent entirely. Understanding what to watch for can make a real difference. Many STDs are fully treatable, and early diagnosis protects both your health and the health of your partner. This guide covers the key signs, common infections, risk factors, and when to get tested. What Are STDs and Why Do They Affect Women Differently? STDs are infections that spread primarily through vaginal, anal, or oral sex. Some, like herpes or HPV, can also spread through skin-to-skin contact in the genital area. Others, like HIV and syphilis, can pass through blood. Women face a higher risk of acquiring an STD during unprotected sex than men. This is because the vaginal lining is thinner and more delicate than penile skin, making it easier for pathogens to enter. Hormonal changes during pregnancy, menstruation, or menopause can also alter the vaginal environment and increase susceptibility. Because the internal anatomy of women means that symptoms are often less visible, many infections go unnoticed for months or even years. Regular screening is the most reliable way to stay informed about your sexual health. Common STD Symptoms in Women Symptoms can vary widely depending on the type of infection. Some of the most commonly reported signs include: Unusual vaginal discharge: a change in colour, consistency, amount, or smell compared to your normal baseline Burning or pain during urination Itching, irritation, or redness in the genital area Pain during or after sexual intercourse Sores, blisters, ulcers, or warts around the genitals, anus, or mouth Abnormal vaginal bleeding, such as spotting between periods or bleeding after sex Lower abdominal or pelvic pain Swollen lymph nodes in the groin Fever or general feeling of being unwell Not all of these symptoms point to an STD. However, if you notice one or more of them, it is worth speaking with a healthcare provider rather than waiting to see if they resolve on their own. Early Signs of STDs in Women In the early stages, symptoms may be subtle or easy to dismiss. Watch for: Mild itching or unusual discharge that appears different from usual A slight burning sensation while urinating, which may feel like a mild urinary tract infection Small, painless sores in the genital area that heal on their own but may recur A skin rash, including on the palms of the hands or soles of the feet (a possible early sign of syphilis) Flu-like symptoms such as fatigue, mild fever, or swollen glands shortly after a new sexual encounter These early warning signs are easy to attribute to other causes. That is precisely why they are often missed. If you have had unprotected sex or a new sexual partner, it is a good idea to get tested even when symptoms seem minor. STD Symptoms Without Discharge Vaginal discharge is often associated with STDs, but not all infections cause it. Several STDs can be present without any noticeable discharge. Genital herpes, for example, may only cause occasional sores or tingling, especially between outbreaks. Syphilis in its early stage typically presents as a single, painless ulcer that heals without treatment, which can make it easy to overlook. HPV often has no symptoms at all, even when high-risk strains are present. Pelvic inflammatory disease (PID), which is a complication of untreated chlamydia or gonorrhoea, may cause pelvic discomfort, pain during sex, or fever without any visible discharge. It is worth knowing that an absence of discharge does not mean an absence of infection. If you are sexually active and have any concerns, testing is the only way to be sure. Causes and Risk Factors STDs are caused by a range of organisms: Bacteria: Chlamydia, gonorrhoea, and syphilis are bacterial infections that can be cured with antibiotics. Viruses: HIV, herpes, HPV, and hepatitis B are viral infections that cannot be cured but can be effectively managed. Parasites: Trichomoniasis is caused by a parasite and is treatable with antibiotics. Factors that increase the risk of acquiring an STD include: Having multiple sexual partners Inconsistent or incorrect use of condoms A history of STDs Being sexually active at a young age Engaging in anal sex, which carries a higher risk of tissue damage and transmission Using intravenous drugs or sharing needles Pregnancy, which can alter immune response and vaginal pH Common Types of STDs Affecting Women Chlamydia: The most frequently reported bacterial STD. It often has no symptoms, but can cause vaginal discharge, burning during urination, and lower abdominal pain. Without treatment, it can lead to pelvic inflammatory disease and infertility. Gonorrhoea: Caused by bacteria, gonorrhoea is especially common in women aged 15 to 24. Symptoms include vaginal discharge, pain during urination, and irregular bleeding. It can lead to fertility problems if left untreated. Syphilis: This bacterial infection progresses in stages. The first stage causes a painless sore; later stages can affect the heart, brain, and other organs. During pregnancy, it poses serious risks to the baby. Genital Herpes (HSV-2): Caused by the herpes simplex virus, genital herpes causes recurring blisters or sores in the genital area. Many women live with the infection without knowing. There is no cure, but antiviral medication reduces outbreaks and transmission. HPV (Human Papillomavirus): HPV is among the most common STDs worldwide. Certain high-risk strains can cause cervical, vaginal, and vulvar cancers. Most infections clear on their own, but regular cervical screening remains essential. Trichomoniasis: A parasitic infection that is more common in women than men. It causes foul-smelling discharge, itching, and painful sex. It is curable with antibiotics. HIV: The human immunodeficiency virus attacks the immune system. Early symptoms may include fever, fatigue, and swollen lymph nodes. With modern treatment, people living with HIV can maintain a healthy life. How STDs Are Diagnosed in Women A healthcare provider will usually begin with a discussion of your symptoms and sexual history. Tests may include: Urine test: Used to detect chlamydia and gonorrhoea. Swab test: A sample taken from the vagina, cervix, or any sores or discharge for laboratory analysis. Blood test: Used to diagnose HIV, syphilis, herpes, and hepatitis B. Physical examination: To check for visible sores, warts, or abnormal discharge. Pap smear and HPV test: Recommended regularly for women to detect cervical changes linked to HPV. An STD test is simple and straightforward. Many tests can be done during a routine health visit, and some can be completed with a self-collected swab or urine sample. Results are typically available within a few days. Treatment Options for STDs in Women Treatment depends on the type of infection: Bacterial STDs (chlamydia, gonorrhoea, syphilis, trichomoniasis): These are treatable and curable with the appropriate antibiotics. It is important to complete the full course and avoid sexual contact until treatment is finished. Viral STDs (herpes, HPV, HIV, hepatitis B): These cannot be cured, but symptoms and risks can be managed. Antiviral medications for herpes reduce outbreaks. HIV treatment (antiretroviral therapy) keeps the virus suppressed. HPV vaccines prevent infection with the most dangerous strains. After a diagnosis, your doctor may recommend that previous and current partners also get tested and treated. This is an important step in preventing reinfection and protecting others. Complications of Untreated STDs in Women STDs that are not identified and treated promptly can cause lasting harm. Potential complications include: Pelvic inflammatory disease (PID): An infection of the reproductive organs that can cause chronic pelvic pain and increase the risk of ectopic pregnancy. Infertility: Untreated chlamydia and gonorrhoea are leading preventable causes of infertility in women. Increased risk of certain cancers: Persistent HPV infection is linked to cervical, vaginal, and vulvar cancer. Pregnancy complications: STDs during pregnancy can lead to premature birth, low birth weight, and infections in the newborn. Syphilis in particular can be life threatening for the baby. Higher risk of HIV: Active STDs with sores or inflammation make it easier for HIV to enter the body. Chronic liver disease: Untreated hepatitis B can lead to liver cirrhosis or liver cancer over time. Prevention Tips for STDs in Women Use condoms consistently during vaginal, anal, and oral sex. Get vaccinated: The HPV vaccine is recommended for women up to age 26, and sometimes up to 45 after discussing with your doctor. The hepatitis B vaccine is also widely available. Limit the number of sexual partners and discuss testing history before sexual activity. Consider regular STD testing as part of your routine healthcare, not just when symptoms appear. Avoid sharing sex toys or ensure they are cleaned and covered with a condom. Be aware of higher-risk practices, such as anal sex, and take additional precautions. The Importance of Regular STD Screening in Women Many STDs produce no noticeable symptoms for months or years. Chlamydia, in particular, is known as a 'silent infection' because most people who have it do not know. The same is true for HPV and early-stage HIV. This is why waiting for symptoms before getting tested is not an effective approach. Regular screening helps you catch infections early, before they cause complications. It also reduces the risk of passing an infection to others. Health guidelines generally recommend that sexually active women under 25 get tested for chlamydia and gonorrhoea at least once a year. Women over 25 with risk factors should also consider annual testing. Cervical cancer screening (Pap smear and HPV test) is recommended every three to five years, depending on your age and previous results. When to See a Doctor Speak with a healthcare provider if you notice: Unusual vaginal discharge, especially with an odour Pain or burning when you urinate Sores, blisters, or warts in the genital area Pelvic or lower abdominal pain Bleeding between periods or after sex Any skin rash on the body after sexual contact You should also seek testing after unprotected sex with a new partner, if a current partner has been diagnosed with an STD, or if you have had multiple partners without regular screening. Do not wait for symptoms to become severe. The earlier an STD is caught, the simpler and more effective the treatment. Key Takeaways STDs are common, and many cause no obvious symptoms in women. Symptoms to watch for include unusual discharge, genital sores, burning during urination, pelvic pain, and abnormal bleeding. Common STDs include chlamydia, gonorrhoea, syphilis, herpes, HPV, trichomoniasis, and HIV. Untreated STDs can lead to PID, infertility, cancer, and pregnancy complications. Condom use, vaccination, and limiting partners can significantly reduce risk. Regular STD testing is essential for sexually active women, regardless of symptoms. Most bacterial STDs are curable; viral STDs are manageable with treatment. Stay Informed with Metropolis Healthcare Sexual health is an important part of your overall wellbeing, and routine testing plays a key role in staying on top of it. Metropolis Healthcare makes it easy to prioritise your health with a comprehensive range of over 4,000 tests, including speciality testing for sexual health and infectious diseases. Whether you want to get a STD profile test, a full body checkup, or specific screening recommended by your doctor, Metropolis offers accurate, confidential, and timely results. With home sample collection available across 10,000 touchpoints, you do not need to travel to a lab. Book your test through the website, mobile app, WhatsApp, or by phone, at a time that works for you. Reliable results, expert pathologists, and NABL and CAP-accredited labs mean you can trust what you receive. Taking care of your sexual health is not something to put off. With Metropolis, it has never been easier to take that step. FAQs About STD Symptoms in Women How Does a Woman Know If She Has an STD? Many STDs cause no symptoms at all, especially in the early stages. When symptoms do appear, they may include unusual vaginal discharge, genital sores or blisters, pain during urination or sex, abnormal bleeding, or pelvic discomfort. However, the only reliable way to know is through testing. If you are sexually active, especially with multiple partners, regular screening is the most responsible and effective approach. Are STDs Curable in Women? It depends on the type. Bacterial STDs such as chlamydia, gonorrhoea, syphilis, and trichomoniasis are fully curable with the right antibiotics when caught in time. Viral STDs such as herpes, HPV, and HIV cannot be cured but can be managed effectively with medication. Early diagnosis significantly improves outcomes for all STDs. Can STDs Affect Fertility in Women? Yes, they can. Chlamydia and gonorrhoea are among the leading preventable causes of infertility in women. If left untreated, they can cause pelvic inflammatory disease, which leads to scarring of the fallopian tubes and makes it difficult or impossible to conceive. Getting tested and treated promptly greatly reduces this risk. When Should I Get Tested for STDs? It is a good idea to get tested if you have had unprotected sex, started a new relationship, have multiple partners, or notice any unusual symptoms. Sexually active women under 25 are generally advised to test for chlamydia and gonorrhoea annually. Women who are pregnant should be screened for several STDs as part of routine antenatal care. If you are unsure, speak with your doctor about a testing schedule that suits your circumstances. Can STDs Be Asymptomatic? Yes, and this is one of the most important things to understand about STDs. Infections like chlamydia, HPV, and early HIV frequently cause no symptoms at all. A person can carry and transmit an STD without ever knowing they have one. This is why regular screening matters, regardless of whether you feel perfectly well. References Workowski KA, Bolan GA. Sexually transmitted diseases treatment guidelines, 2015. MMWR Recomm Rep. 2015;64(RR-03):1-137. PMID: 26042815. Centers for Disease Control and Prevention. Sexually transmitted infections surveillance, 2022. Atlanta: US Department of Health and Human Services; 2023. World Health Organization. Sexually transmitted infections (STIs). WHO Fact Sheet. 2023. American College of Obstetricians and Gynecologists. Sexually transmitted infections. ACOG Practice Bulletin. 2021. Office on Women's Health, US Department of Health and Human Services. Sexually transmitted infections. Updated 2021.
STD Symptoms in Men: Early Warning Signs
Sexually transmitted diseases (STDs), also called sexually transmitted infections (STIs), affect men of all ages and backgrounds. Yet many men are unaware they have one. This is because STDs often cause no obvious symptoms, especially in the early stages. By the time signs appear, the infection may already have been present for weeks or months. Knowing what to look for, understanding your risk, and getting tested regularly are the most effective ways to protect your health and that of your partner. What Are STDs and How Do They Affect Men? STDs are infections spread primarily through sexual contact, including vaginal, anal, and oral sex. They are caused by bacteria, viruses, or parasites. Some can also spread through blood, such as via shared needles or from mother to child during pregnancy. While anyone who is sexually active can acquire an STD, men who have sex with men face a statistically higher risk of certain infections, including HIV and gonorrhoea. Men with multiple partners or those who do not use condoms consistently also face elevated risk. One key thing to understand is that STDs do not always announce themselves. Many infections are entirely silent for months or even years. This makes regular screening essential, particularly if you are sexually active. Common STD Symptoms in Men When symptoms do occur, they can vary depending on the infection. The most commonly reported signs of STDs in men include: Unusual discharge from the penis, which may be white, yellow, green, or cloudy Burning or pain during urination Pain or discomfort during ejaculation Sores, blisters, ulcers, or warts on the penis, scrotum, anus, or mouth Itching, redness, or irritation in the genital or anal area Swelling or pain in the testicles A rash on the palms of the hands, soles of the feet, or elsewhere on the body Swollen lymph nodes, particularly in the groin Unexplained fever, fatigue, or flu-like symptoms These symptoms are not exclusive to STDs, and some overlap with other conditions. However, if you notice one or more of these signs, especially after sexual contact, it is worth speaking with a doctor promptly. Early Signs of STDs in Men Early STI signs in males are often subtle and easy to dismiss. Watch for: A small, painless sore or ulcer on or around the genitals, anus, or mouth (a common early sign of syphilis) Mild burning or increased frequency of urination, which can resemble a urinary tract infection A slight discharge or unusual dampness from the penis Tiny blisters or clusters of spots in the genital area that appear and then seem to heal on their own Flu-like symptoms including mild fever, fatigue, and swollen glands, which can occur shortly after HIV exposure Genital warts that may appear as flat, flesh-coloured patches or small cauliflower-like clusters STI early signs in males may take anywhere from a few days to several weeks to appear after exposure. For some infections, symptoms may not emerge for months. This window period is part of what makes early STD testing so important. STD Symptoms Without Discharge in Men Discharge is one of the more well-known signs of an STD, but not all infections cause it. Several common STDs can be present without any penile discharge at all. Genital herpes often presents as sores or blisters, itching, or tingling without any discharge. Syphilis in its first stage typically causes a single, painless sore that heals on its own, leaving no obvious trace. HPV frequently causes no symptoms whatsoever, even when high-risk strains are present. HIV may mimic flu symptoms early on, without any genital signs at all. Trichomoniasis is often completely asymptomatic in men. The absence of discharge does not mean the absence of infection. If you have had unprotected sex or a new partner, an STD test remains the only reliable way to confirm your status. Causes and Risk Factors of STDs in Men STDs are caused by three main types of organisms: Bacteria: Chlamydia, gonorrhoea, and syphilis are bacterial STDs that are curable with antibiotics when caught early. Viruses: HIV, herpes, HPV, and hepatitis B are viral infections that cannot be cured but can be effectively managed with treatment. Parasites: Trichomoniasis is caused by a microscopic parasite and is treatable with a short course of antibiotics. Factors that increase the risk of acquiring an STD include: Having multiple sexual partners Inconsistent or incorrect use of condoms Engaging in anal sex, which carries a higher risk of tissue injury and transmission Having sex with men (for men), due to higher prevalence of certain infections in this group A previous history of STDs, which increases susceptibility to reinfection Sharing needles or other drug equipment Sexual contact with a partner who has multiple partners Common Types of STDs Affecting Men Chlamydia: One of the most common bacterial STDs, chlamydia often causes no symptoms in men. When symptoms do appear, typically within one to three weeks of infection, they include painful urination, cloudy discharge, and swollen or tender testicles. Without treatment, it can lead to epididymitis, a painful infection of the tube behind the testicle, and in rare cases, reduced fertility. Gonorrhoea: Also caused by bacteria, gonorrhoea typically produces symptoms within four to eight days, including painful urination and white, yellow, or green penile discharge. It can also affect the throat and rectum. Untreated gonorrhoea can lead to serious complications, including infertility. Syphilis: This bacterial infection progresses in stages. The first stage causes a painless sore (chancre) that often goes unnoticed. The second stage may produce a body rash, fatigue, swollen lymph nodes, and sore throat. If left untreated, tertiary syphilis can damage the heart, brain, and nervous system. Genital Herpes (HSV-2): Caused by the herpes simplex virus, herpes produces clusters of blisters or sores on the genitals, anus, or thighs. After the first outbreak, the virus remains in the body and can cause recurring episodes. Many men carry the virus without knowing. HPV (Human Papillomavirus): HPV is among the most widespread STDs, with dozens of strains identified. Low-risk strains cause genital warts; high-risk strains are associated with cancers of the penis, anus, and throat. Most infections produce no visible symptoms. HPV vaccines are available and recommended for boys and men up to age 26. Trichomoniasis: A parasitic genital infection that is frequently asymptomatic in men. When symptoms occur, they include itching, burning during urination or ejaculation, and mild discharge. It is one of the most easily treatable STDs. Hepatitis B: Spread through blood and bodily fluids, hepatitis B is a liver infection that can cause jaundice, dark urine, fatigue, nausea, and joint pain. It can become chronic if untreated, leading to liver damage over time. A vaccine is available. HIV: HIV attacks the immune system. In the early weeks after infection, some men experience a flu-like illness including fever, fatigue, sore throat, and swollen glands. After this, the virus can remain silent for years while slowly weakening immunity. Modern antiretroviral therapy allows people living with HIV to lead healthy, full lives. How STDs Are Diagnosed in Men If you suspect an STD or want routine screening, a doctor will usually start with a discussion of your symptoms and sexual history. Tests commonly used include: Urine test: Used to detect chlamydia and gonorrhoea Swab from the urethra, rectum, or throat: Depending on sexual practices and symptoms Swab from any sores or lesions: For herpes or syphilis diagnosis Blood test: Used to diagnose HIV, syphilis, herpes, and hepatitis B Physical examination: To check for warts, rashes, discharge, or swelling Testing is straightforward and generally quick. Results are typically available within a few days. Some tests can be done with a urine sample alone, making the process simple and accessible. Treatment Options for STDs in Men Treatment depends on the type of infection: Bacterial STDs (chlamydia, gonorrhoea, syphilis): These are fully curable with antibiotics. It is important to complete the entire course of treatment and avoid sexual contact until the infection has cleared. Both you and your partner should be treated to prevent reinfection. Parasitic STDs (trichomoniasis): Treated effectively with a short antibiotic course, often a single dose of metronidazole or tinidazole. Viral STDs (herpes, HIV, hepatitis B, HPV): These cannot be cured, but they can be managed. Antiviral medication for herpes reduces the frequency and severity of outbreaks. Antiretroviral therapy for HIV keeps viral levels undetectable and prevents transmission. Hepatitis B can be treated with antiviral drugs. Genital warts caused by HPV can be removed by a doctor through freezing or other procedures. After any STD diagnosis, informing recent sexual partners is an important and responsible step so they can also get tested and treated. Complications of Untreated STDs in Men When STDs are not diagnosed and treated in time, they can cause lasting and serious harm: Epididymitis and orchitis: Painful inflammation of the testicles and surrounding structures, caused by untreated chlamydia or gonorrhoea Reduced fertility or infertility: Chronic infections can damage the reproductive tract Increased cancer risk: High-risk HPV strains are linked to penile, anal, and throat cancers; hepatitis B can contribute to liver cancer Systemic organ damage: Advanced syphilis can damage the heart, brain, and nervous system HIV progression to AIDS: Without treatment, HIV eventually leads to severe immune suppression Higher risk of contracting HIV: Active STDs with sores or inflammation make it easier for HIV to enter the bloodstream Early diagnosis and treatment significantly reduce the risk of all these complications. Prevention Tips for STDs in Men Use condoms correctly and consistently during all forms of sexual activity, including anal and oral sex Get vaccinated against HPV and hepatitis B Limit the number of sexual partners and discuss sexual health openly before sexual contact Get tested regularly, even without symptoms, particularly if you have multiple partners or have had unprotected sex Avoid sharing needles, syringes, or any equipment that involves blood contact Be aware of higher-risk sexual practices and take additional precautions accordingly If exposed to HIV, seek post-exposure prophylaxis (PEP) from a doctor as soon as possible, ideally within 72 hours The Importance of Regular STD Screening in Men One of the most persistent misconceptions about STDs is that you will know if you have one. The reality is quite different. Many common STD infections in men, including chlamydia, gonorrhoea, HPV, and early HIV, cause no symptoms at all. A man can carry and transmit an infection for months or years without any indication that something is wrong. Regular STD testing changes this. It gives you accurate, timely information about your health, allows infections to be caught and treated before they cause complications, and protects your partners. Men who are sexually active with multiple partners, who do not use condoms consistently, or who have sex with men are generally advised to test more frequently, often every three to six months. Even men in committed relationships benefit from periodic screening, as some infections can be present from before the relationship began. Testing is not a sign of mistrust or suspicion. It is simply a responsible part of looking after your health. When to See a Doctor See a healthcare provider if you notice: Any unusual discharge from the penis Pain, burning, or increased frequency of urination Sores, blisters, warts, or rashes in the genital, anal, or oral area Swelling or pain in the testicles Itching or redness that does not resolve A skin rash appearing on your palms, soles, or elsewhere on the body after sexual contact Flu-like symptoms, swollen glands, or unexplained fatigue shortly after a new sexual encounter You should also seek an STD test if a current or recent partner has been diagnosed with an STD, if you have had unprotected sex with a new partner, or if you simply have not been tested in a while and are sexually active. Key Takeaways Many STDs cause no symptoms in men, making regular testing the only reliable way to know your status Common signs include penile discharge, painful urination, genital sores, and testicular discomfort STI early signs in males can be subtle and are often mistaken for unrelated conditions Common STDs in men include chlamydia, gonorrhoea, herpes, syphilis, HPV, trichomoniasis, and HIV Bacterial and parasitic STDs are curable; viral STDs are manageable with treatment Untreated STDs can lead to fertility issues, organ damage, and increased cancer risk Condom use, vaccination, and routine screening are the most effective forms of prevention Getting tested is a responsible and straightforward part of sexual health care Take Charge of Your Sexual Health with Metropolis Healthcare Staying on top of your sexual health does not have to be complicated. Metropolis Healthcare offers a comprehensive range of over 4,000 tests, including speciality testing for sexual and reproductive health. Whether you want a targeted STD test or a broader STD profile test, Metropolis provides accurate, confidential results backed by NABL and CAP-accredited laboratories and expert pathologists. With home sample collection available across 10,000 touchpoints across India, you can get tested from the comfort and privacy of your home. Booking is easy through the Metropolis website, mobile app, WhatsApp, or by phone. Reliable results, a quick turnaround time, and a convenient process mean there is no reason to put off testing. Your health is worth prioritising. Taking a simple test today can give you peace of mind and, if needed, open the door to effective treatment early. FAQs About STD Symptoms in Men Can STDs Show Symptoms Immediately in Men? Not usually. Most STDs have an incubation period, meaning symptoms appear some time after initial exposure, not right away. Gonorrhoea may produce signs within a few days; herpes typically takes two to fourteen days; trichomoniasis can take up to four weeks; and syphilis or HIV symptoms may not emerge for weeks or months. Some infections never produce noticeable symptoms at all. This is why testing after potential exposure is important, even if you feel completely well. Are STDs Curable in Men? It depends on the type of infection. Bacterial STDs such as chlamydia, gonorrhoea, syphilis, and trichomoniasis are fully curable with antibiotics when treated promptly. Viral STDs, including herpes, HPV, HIV, and hepatitis B, cannot be cured but can be effectively managed with antiviral or suppressive medication. Early diagnosis gives the best outcomes for all types of STD. Can STDs Affect Fertility in Men? Yes. Untreated chlamydia and gonorrhoea can cause epididymitis, an inflammation of the tube that carries sperm from the testicle. If left untreated, this can lead to scarring and reduced fertility. In some cases, it can contribute to complete infertility. Getting tested and treated early greatly reduces this risk. Can STDs Be Asymptomatic in Men? Yes, and this is particularly common. Chlamydia is asymptomatic in the majority of men who carry it. HPV almost never causes symptoms in men. Early HIV often produces no signs, or symptoms that resemble a mild flu and then resolve. Trichomoniasis is frequently silent. A man with no symptoms can still transmit an infection to a partner, which is why routine STD testing matters regardless of how you feel. References Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. MMWR Recomm Rep. 2021;70(4):1-187. PMID: 34292926. Centers for Disease Control and Prevention. Sexually transmitted infections surveillance, 2022. Atlanta: US Department of Health and Human Services; 2023. World Health Organization. Sexually transmitted infections (STIs). WHO Fact Sheet. 2023. American Urological Association. Sexually transmitted infections in men. AUA Guidelines. 2022. Unemo M, Seifert HS, Hook EW III, Hawkes S, Ndowa F, Dillon JR. Gonorrhoea. Nat Rev Dis Primers. 2019;5(1):79. PMID: 31700051.