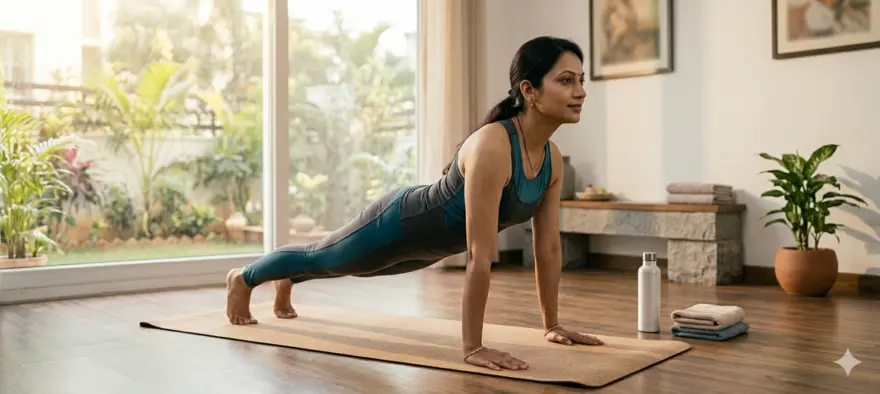Web Stories
Latest Blogs
Yoga For Weight Loss: Effective Asanas To Burn Fat And Improve Fitness
If you want a gentler and more sustainable way to manage your weight, yoga can be a good place to start. It may not feel as intense as a gym workout, but it can still support fat loss, improve fitness, and help you build a healthier routine. Yoga for weight loss works best when you treat it as part of your lifestyle, not as a quick fix. When you stay consistent, move mindfully, and support your body with healthy food and good sleep, yoga can become a practical tool for long-term wellbeing. Introduction To Yoga For Weight Loss Yoga is more than stretching. It combines movement, breathing, balance, and body awareness. This combination can help you become stronger, more active, and more mindful of your daily habits. That matters because weight loss is not only about burning calories in one session. It is also about building routines that you can continue. Yoga can help you do that in a calm and realistic way. Can Yoga Help You Lose Weight? Yes, yoga can help you lose weight. But it helps in a broader way than many people expect. Some forms of yoga can raise your heart rate and challenge your muscles. Others help lower stress, improve sleep, and reduce emotional eating. Together, these effects can support steady weight loss over time. So, if you are wondering whether yoga for weight loss is worth trying, the answer is yes, especially if you want an approach that feels manageable and sustainable. Why Yoga Is Effective For Weight Loss Yoga supports weight loss in several ways. First, it helps you build strength. When your muscles work harder, your body uses more energy and becomes more efficient over time. Second, yoga may support a healthier metabolism by encouraging regular movement, muscle engagement, and better recovery. It is not a magic metabolism booster, but it can form part of an active lifestyle. Third, yoga can help reduce stress. When you feel less stressed, you may be less likely to overeat, snack mindlessly, or rely on comfort foods. Finally, yoga increases body awareness. You become more aware of hunger, fullness, posture, breathing, and fatigue. That can make healthy habits easier to maintain. Benefits Of Yoga For Weight Loss Yoga offers benefits that go beyond the weighing scale: It helps improve flexibility and mobility It builds strength in your core, legs, arms, and back It supports better posture and body control It may reduce stress and improve mood It can help you sleep better It encourages consistency and self-discipline It can support mindful eating habits It may improve stamina and everyday fitness Best Yoga For Weight Loss Dynamic Yoga Styles That May Support Weight Loss If your main goal is calorie burn and fitness, more active yoga styles may suit you better. Vinyasa Yoga uses flowing movement and can feel like a full-body workout. Power Yoga is faster and stronger, with greater muscular effort. Ashtanga Yoga follows a structured sequence and can be physically demanding. These styles are often considered the best yoga for weight loss if you enjoy more movement and want a stronger workout effect. Gentle Yoga Styles That Support Consistency And Recovery Gentler styles can still help, especially if you are a beginner, returning after a break, or dealing with stress and fatigue. Hatha Yoga helps you learn alignment and breathing. Restorative Yoga helps you relax and recover. Yoga Nidra does not burn many calories, but it may support better sleep and stress control. These styles may not feel intense, but they can make it easier for you to stay consistent, and consistency is what drives results. Best Yoga Asanas For Weight Loss If you are looking for yoga asanas for weight loss, these poses are practical and widely used: Surya Namaskar: A flowing sequence that warms up the whole body and helps build stamina Plank Pose: Strengthens your core, shoulders, arms, and legs Warrior Pose: Builds strength in your legs and improves balance and endurance Chair Pose: Activates the thighs, glutes, and core Boat Pose: Works the abdominal muscles and improves balance Bridge Pose: Strengthens the glutes, back, and core Cobra Pose: Opens the chest and strengthens the back Triangle Pose: Improves stability and works the side body Bow Pose: Engages the back, legs, and core Downward Dog: Builds strength and stretches the body at the same time These yoga exercises for weight loss can be done at home with little equipment, as long as you focus on form and move at a pace that feels safe for you. Top 5 Yoga Poses To Burn Belly Fat No yoga pose can remove fat from only one area of your body. But some poses can strengthen your middle, improve fitness, and support overall fat loss. That is why these are often recommended for belly fat goals. Surya Namaskar Surya Namaskar works several muscle groups in one sequence. It helps you move continuously, build stamina, and warm up your whole body. If you want a dynamic start to your session, this is one of the best choices. Plank Pose Plank Pose is excellent for core strength. It also works your shoulders, arms, and legs. When you hold it with proper form, you train stability and muscular endurance at the same time. Boat Pose Boat Pose directly challenges your abdominal muscles and hip flexors. It is useful when you want to improve core control and posture. Chair Pose Chair Pose activates large lower-body muscles, which makes the pose feel demanding quite quickly. It also helps strengthen your core and improve balance. Warrior Pose Warrior Pose builds endurance and strength in your legs and core. It also improves focus and body awareness, which can help you stay engaged in your routine. How Yoga Supports Long-Term Weight Loss The biggest strength of yoga is that many people can continue it for the long term. Extreme plans often fail because they are too hard to maintain. Yoga is different. You can adapt it to your age, body type, fitness level, and schedule. That makes it easier to return to your mat regularly, which matters far more than doing one intense session and then stopping. Yoga also supports habits that protect your progress. It may help you manage stress, sleep better, and feel more in control of your eating pattern. These daily effects can be just as important as the workout itself. How Yoga Promotes Healthy Metabolism Yoga may support healthy metabolism in indirect but meaningful ways. When you move regularly, engage your muscles, and improve your overall activity level, your body becomes more efficient. Stronger muscles also support better physical function and energy use. Yoga may help in another way too. Poor sleep and high stress can make weight management harder. By supporting relaxation and routine, yoga can help create better conditions for healthy metabolism and steady progress. Yoga For Core Strength And Stability A stronger core can improve posture, balance, and exercise performance. These poses are especially useful: Plank Pose for deep core stability Boat Pose for abdominal strength and control Chair Pose for core and lower-body engagement Warrior Pose for balance, endurance, and trunk stability Yoga For Weight Loss: Tips For Beginners If you are just starting, keep things simple. You do not need advanced poses to benefit from yoga. Begin with short sessions. Focus on breathing and alignment. Choose a few basic poses and repeat them consistently. If needed, follow a guided beginner class. You can also add walking to your week for extra support. The goal is not to be perfect. The goal is to keep going. Incorporating Yoga Into A Weight Loss Routine You can make yoga more effective by combining it with simple habits: Practise 3 to 5 times a week if possible Add brisk walking or another form of movement on other days Drink enough water Eat balanced meals with protein and fibre Sleep well and manage stress Increase intensity gradually as your fitness improves How Often Should You Practice Yoga For Weight Loss? A realistic target is 3 to 5 sessions a week. Each session can last around 30 to 60 minutes, depending on your schedule and energy. If that feels too much, start smaller. Even 15 to 20 minutes done regularly is better than aiming too high and stopping. Yoga And The GLP-1 Diet: A Holistic Approach To Weight Loss If you are already following a doctor-guided GLP-1 Diet, yoga can complement it well. Yoga does not replace medical treatment or nutrition advice, but it can support movement, stress control, and routine. That makes it a helpful addition to a wider weight management plan. Yoga For Women And Men: Does The Approach Differ? The core principles are the same for everyone. You do not need separate yoga plans based only on gender. What matters more is your current fitness, flexibility, joint comfort, and personal goal. For example, one person may want better stamina, while another may want better posture or core strength. So instead of looking for male or female-specific routines, focus on the intensity and style that fit your body and your needs. Yoga Poses For Weight Loss: A Simple Step-By-Step Routine Here is a beginner-friendly flow you can follow at home: Start with 2 to 3 minutes of deep breathing Do 4 to 6 rounds of Surya Namaskar Hold Warrior Pose on each side for 20 to 30 seconds Stay in Chair Pose for 20 to 30 seconds Hold Plank Pose for 20 to 40 seconds Move into Boat Pose for 15 to 20 seconds Finish with Bridge Pose for 20 to 30 seconds Cool down with gentle stretching and slow breathing As you improve, you can increase the number of rounds or the holding time. Yoga And Healthy Diet For Weight Loss Yoga works better when your food habits support your goal. You do not need a harsh diet. But you do need a balanced one. Choose meals with enough protein, fibre, vegetables, fruit, whole grains, and healthy fats. Try to reduce ultra-processed foods, sugary drinks, and frequent mindless snacking. A healthy diet gives your body the fuel it needs to recover well and stay active. How To Combine Yoga With Healthy Eating Habits Avoid very heavy meals right before yoga Eat balanced meals rather than skipping food Include protein and fibre in your main meals Stay hydrated through the day Eat slowly and notice hunger and fullness cues Limit late-night snacking when possible Precautions And Contraindications Yoga is generally safe, but it is not one-size-fits-all. Take extra care if you have: Back pain or slipped disc history Knee pain or joint instability Uncontrolled high blood pressure Recent surgery Vertigo or balance problems Pregnancy Severe obesity with limited mobility If you have any of these, speak to your doctor or a qualified yoga instructor before starting. Modify poses when needed. Stop if you feel sharp pain, dizziness, chest discomfort, or unusual breathlessness. Common Mistakes To Avoid Many people do yoga regularly but still feel stuck. These mistakes are often the reason: Expecting instant weight loss Ignoring your food habits Choosing poses that are too advanced too soon Rushing through form and breathing Practising inconsistently Comparing yourself with others Pushing through pain instead of modifying safely When To Consider Health Monitoring During A Weight Loss Journey Weight loss is not only about appearance. It is also about your health markers. If you have concerns about blood sugar, cholesterol, thyroid health, liver function, or overall metabolic health, regular screening can be useful alongside lifestyle changes. This can matter even more if you are already on a structured plan, have a family history of metabolic disease, or are discussing medical weight management with your doctor. In some cases, organised follow-up through a GLP 1 Test Package or GLP-1 Monitor Package may help you keep track of important health markers under medical guidance. Conclusion: Yoga For Sustainable Weight Loss Yoga can be a valuable part of your weight loss journey. It strengthens your body, supports your mind, and helps you build routines that last. While it may not deliver overnight results, it can help you move towards fitter, healthier, and more balanced living. If you want to support your progress with preventive health checks, Metropolis Healthcare can help you stay informed about important health markers through 4,000+ tests, full body checkups, and reliable reports. With easy booking through the website, app, call, or WhatsApp, plus home sample collection across a strong network of touchpoints, Metropolis Healthcare can be your partner in proactive wellness monitoring while you work on healthy habits that last. FAQ Can Yoga Alone Help Me Lose Weight? Yoga alone can help, especially if you are new to exercise or very inactive at the moment. But results are usually better when yoga is paired with healthy eating, good sleep, and regular daily movement. Should I Take GLP-1 Medication While Doing Yoga For Weight Loss? If your doctor has prescribed GLP-1 Agonists, you can usually still do yoga, but the decision should stay personalised. Your doctor can guide you based on your medical history, energy levels, side effects, and overall treatment plan. How Long Does It Take To See Weight Loss Results From Yoga? That depends on your consistency, eating pattern, activity level, and the type of yoga you do. Some people notice better flexibility, sleep, and energy within a few weeks. Visible weight loss often takes longer and tends to happen gradually. What Type Of Yoga Is Best For Burning Calories And Weight Loss? More active styles such as Vinyasa, Power Yoga, and Ashtanga Yoga are usually better for calorie burn. Slower styles still have value because they support consistency, recovery, and stress management. Can Yoga Reduce Belly Fat Specifically? Yoga cannot target fat loss from only one area. But it can strengthen your core, improve overall fitness, and support total body fat loss over time. That may help reduce belly fat as part of broader weight loss. References Harvard Health Publishing. Yoga for Weight Loss: Benefits Beyond Burning Calories. 2021. National Center for Complementary and Integrative Health. Yoga: Effectiveness and Safety. NIH. Accessed 2026. National Center for Complementary and Integrative Health. Yoga for Health: What the Science Says. NIH. Accessed 2026. Centers for Disease Control and Prevention. Physical Activity Guidelines for Adults. Accessed 2026. NHS. Physical Activity Guidelines for Adults Aged 19 to 64. Accessed 2026. Harvard Health Publishing. More Than a Stretch: How Yoga Can Enhance Heart Health. 2025. National Center for Complementary and Integrative Health. Yoga for Health. 2023.
Is Banana Good For Weight Loss? Benefits, Myths, And The Right Way To Eat It
If you are trying to lose weight, you may have wondered whether banana is a good choice or a food to avoid. The short answer is yes. Banana can be part of a healthy weight loss plan when you eat it in the right amount and in the right context. A banana is easy to carry, naturally sweet, filling, and far better than many processed snacks. At the same time, no single food causes weight loss on its own. Your overall eating pattern, activity level, sleep, and portion sizes still matter most. Is Banana Good For Weight Loss? Yes, banana for weight loss can work well for many people. A medium banana is moderate in calories, contains fibre, and can help you feel satisfied between meals. It is also easy to use as a planned snack instead of biscuits, sweets, or deep-fried foods. That is one reason banana often fits well into a calorie-conscious eating pattern. The key is moderation. Eating one banana as part of a balanced diet is very different from eating several high-calorie snacks during the day and then blaming the banana. Banana Nutrition At A Glance Banana gives you more than just natural sweetness. A medium banana usually provides around 105 calories, about 3 grams of fibre, natural carbohydrates, potassium, and vitamin B6. Its nutrition also changes slightly as it ripens. A firmer green banana contains more resistant starch. A ripe yellow banana contains more natural sugars and tastes sweeter. Both can fit into a healthy diet, but the best choice depends on your appetite, digestion, and how you usually eat it. Benefits Of Bananas For Weight Loss The benefits of banana for weight loss are mostly about convenience, fullness, and better snack choices. Banana contains fibre, which may help you feel full for longer. Banana is portion-friendly because one medium fruit is easy to track. Banana can replace cakes, pastries, chips, and other processed snacks. Banana works well before or after exercise when you want quick energy. Banana pairs easily with yoghurt, nuts, seeds, or peanut butter for better satiety. Banana is simple to include in breakfast, smoothies, or an afternoon snack. Banana may support digestive comfort in some people because it is easy to digest. Does Banana Increase Weight? No, banana does not automatically increase weight. Weight gain usually happens when you regularly eat more calories than your body needs. A banana on its own is not the problem. In fact, banana is often a better option than many packaged snacks and desserts. The confusion often comes from the fact that banana is sweeter and a little higher in carbohydrates than some other fruits. That does not make it unhealthy. It simply means portion and meal balance matter. If you eat a banana within your daily needs, it is unlikely to be the reason you gain weight. Green Banana Vs Ripe Banana For Weight Loss Green banana and ripe banana can both fit into a weight loss plan, but they are not exactly the same. A green or less ripe banana contains more resistant starch. This may help with fullness and may lead to a steadier blood sugar response for some people. A ripe banana is softer, sweeter, and easier for many people to digest. If your goal is satiety, a slightly firm banana may work better. If your goal is taste, workout fuel, or easy digestion, a ripe banana may be more practical. You do not need to force yourself to eat green banana if you dislike it. The better choice is the one you can use consistently in a balanced diet. How Many Bananas Can I Eat A Day? There is no one answer that suits everyone, but these points can help: For many people, 1 medium banana a day fits comfortably into a healthy diet. If you are very active, you may include banana more often as part of meals or workout snacks. If you are also eating several other fruits each day, keep your total intake balanced. If you have diabetes or are closely watching carbohydrate intake, portion size and food pairing matter more. If you have kidney disease or have been told to restrict potassium, ask your doctor before eating banana often. So, if you are asking, how many bananas can I eat a day, the answer depends on your total diet, your health conditions, and your activity level. For most people, one banana a day is a reasonable amount. The Right Way To Eat Bananas For Weight Loss The way you eat banana matters more than the banana itself. Eat banana as a planned snack, not as mindless extra eating. Pair banana with protein or healthy fat, such as curd, Greek yoghurt, nuts, seeds, or peanut butter. Add banana to breakfast with oats or yoghurt instead of sugary cereals. Use banana to replace desserts or packaged snacks when cravings strike. Choose a smaller or medium banana if you are watching portions. Avoid turning banana into a high-calorie treat with sugar, cream, chocolate syrup, or ice cream. If you use banana in smoothies, keep the rest of the ingredients simple. Can Bananas Help Burn Belly Fat? No, banana does not burn belly fat directly. No food can target fat loss from one area of the body. If you lose body fat overall through a calorie deficit, regular movement, and healthy habits, your waistline may reduce too. Banana can support that process by helping you choose a more filling, nutritious snack, but it is not a belly-fat remedy. Banana Smoothies For Weight Loss Banana smoothies can help, but only if you make them carefully. Use 1 small or medium banana, not several. Add protein such as plain yoghurt, curd, milk, or protein powder if suitable for you. Add fibre with oats, chia seeds, or flaxseeds. Keep the smoothie unsweetened. Avoid ice cream, extra sugar, chocolate spread, sweet syrups, or too much peanut butter. Treat it as a meal component or planned snack, not an extra drink on top of meals. A good banana smoothie can be balanced. A large café-style smoothie can become very high in calories very quickly. Banana Vs Other Fruits For Weight Loss Banana is healthy, but it is not the only fruit that works for weight loss. Berries, apples, pears, and oranges may offer fewer calories per serving or more fibre relative to their size. That can make them useful if you want a larger volume of fruit for fewer calories. Still, banana remains a strong option because it is convenient, filling, and easy to pair with other foods. So, banana does not have to be better or worse than every other fruit. It simply needs to fit your portion needs and your overall diet. Myths About Banana And Weight Loss Many people still believe things about banana that are not true. Here are some common myths. Myth: Banana always makes you fat False. Banana can fit into a calorie-controlled diet. Myth: Banana is too sugary for weight loss Not necessarily. Banana contains natural sugar, but it also contains fibre and useful nutrients. Myth: You should never eat banana at night False. Timing matters less than your total calorie intake and portion size. Myth: Green banana is always good and ripe banana is always bad False. Green banana and ripe banana both have a place. The better choice depends on your tolerance, appetite, and how you eat it. Myth: Banana alone can help you lose weight False. Banana can support your plan, but it cannot replace a balanced diet and active lifestyle. Bananas And Digestive Health Banana can also support digestive health in a few ways. Banana contains fibre, which supports bowel regularity. Less ripe banana contains more resistant starch, which may support gut health. Banana is often easy to digest and may suit people who want a simple snack. Some people find banana soothing when they want a light food option. Others may notice bloating or heaviness, especially if they eat too much at once. Your response can be personal. If banana suits your digestion and helps you stay full, it can be a helpful part of your routine. Can Bananas Cause Allergy? Symptoms And When To Get Tested Banana allergy is possible, but it is not very common. Some people get mild itching or tingling in the mouth after eating banana. This can happen as part of oral allergy syndrome. Others may develop skin rash, swelling, tummy symptoms, wheezing, or more serious allergic reactions. Seek medical advice if you notice repeated symptoms after eating banana. Get urgent help if you have trouble breathing, throat swelling, dizziness, or signs of anaphylaxis. Do not try to self-diagnose with home tests. A proper medical assessment is the safer option. Who Should Be Careful With Bananas? Banana is healthy for many people, but a few groups may need extra care. You may need to be more mindful if: You have diabetes and need to watch meal composition and portion size. You suspect a banana allergy. You have kidney disease and have been advised to limit potassium. You do better with lower-sugar fruit choices during certain parts of the day. You are following a medically supervised weight-loss plan with specific carbohydrate goals. For most healthy people, moderate banana intake is not a problem. Bananas, Blood Sugar, And Weight Loss Plans Banana contains natural sugars, but that does not mean it must be avoided. The effect on your blood sugar depends on ripeness, portion size, and what you eat with it. A firmer banana may suit some people better than a very ripe one. Pairing banana with yoghurt, nuts, or seeds may also help you feel fuller. If you are following a structured GLP-1 Diet or taking GLP-1 Agonists, banana is not automatically off-limits. In many cases, the better question is whether it suits your appetite, digestion, and overall meal balance. If you are tracking metabolic health more closely, a GLP 1 Test Package or a GLP-1 Monitor Package may help you keep an eye on key health markers as part of a wider weight-management plan. Conclusion So, is banana good for weight loss? Yes, it can be. Banana is not a miracle food, but it is also not a food you need to fear. It can support weight loss when you eat it in moderation, pair it wisely, and include it in a balanced diet. A banana as a planned snack is usually a much better choice than many processed alternatives. If you are trying to manage your weight, it also helps to stay informed about your overall health. Routine blood tests, preventive screening, and full body checkups can give you a clearer picture of blood sugar, cholesterol, thyroid function, and other markers linked to weight and metabolism. Metropolis Healthcare supports proactive wellness with 4,000+ tests, reliable reports, expert-led diagnostics, and convenient home sample collection through a strong network of touchpoints. You can book easily through the website, app, call, or WhatsApp, making regular health monitoring simpler and more accessible. FAQs Is Banana Good For Weight Loss? Yes. Banana can be part of a healthy weight loss plan because it offers fibre, moderate calories, and good satiety when eaten in the right portion. Does Banana Increase Weight? No. Banana does not directly increase weight. Weight gain depends on your total calorie intake and overall eating pattern. How Many Bananas Can I Eat A Day? For many people, 1 banana a day is reasonable. The right amount depends on your calorie needs, activity level, fruit intake, and health conditions. Does Eating Banana At Night Make You Fat? No. Eating banana at night does not automatically make you fat. What matters more is your total intake across the day. Are Bananas High In Sugar For Weight Loss? Banana does contain natural sugar, but it also contains fibre and useful nutrients. Portion size and food pairing matter more than fear of the fruit itself. Can Bananas Help Burn Belly Fat? No. Banana does not burn belly fat directly. It may support overall weight management as part of a balanced plan. Are Bananas Good For Digestion? Yes, for many people. Banana contains fibre, and less ripe banana contains resistant starch, which may support gut health. What Are The Signs Of Banana Allergy? Possible signs include itching in the mouth, rash, swelling, stomach upset, wheezing, or more serious allergic reactions. Seek urgent help for breathing difficulty or throat swelling. Are GLP-1 Medicines Not Suitable With Bananas? Banana is not specifically incompatible with GLP-1 medicines. The main issue is whether banana fits your portion needs, digestion, and overall diet plan while on treatment. References U.S. Department of Agriculture. SNAP-Ed Connection: Bananas, Nutrition Information. Medium banana listed at about 105 calories, 27 g carbohydrate, 3 g dietary fibre, and 14 g sugars. Harvard T.H. Chan School of Public Health. The Nutrition Source: Bananas. Notes that one medium ripe banana provides about 110 calories, 3 g fibre, potassium, vitamin B6, and other micronutrients. Harvard T.H. Chan School of Public Health. The Nutrition Source: Fiber. Notes that resistant starch is found in unripe bananas and acts as a prebiotic fibre source. Phillips KM, et al. Dietary fiber, starch, and sugars in bananas at different stages of ripeness in the retail market. Reported that starch in bananas decreases substantially as fruit ripens, with corresponding changes in sugars and fibre profile. Available via PubMed Central. Mayo Clinic News Network. Go Bananas For... Bananas. Notes that as bananas ripen, the total carbohydrate does not necessarily increase, but blood sugar may rise a little faster with very ripe bananas compared with less ripe bananas. Centers for Disease Control and Prevention. Healthy Habits: Fruits and Vegetables to Manage Weight. States that most fruits and vegetables are naturally low in fat and calories, and that their water and fibre can help you feel full while eating fewer calories. World Health Organization. Healthy Diet. Recommends that carbohydrates in the diet come primarily from whole grains, vegetables, fruits, and pulses, supporting fruit as part of a balanced eating pattern. NHS. Food Allergy. Lists symptoms such as rash, swelling, coughing, wheezing, tummy pain, diarrhoea, and oral allergy syndrome after certain fruits or vegetables. Anaphylaxis UK. Banana Allergy. Notes that banana allergy reactions often involve itching and swelling of the mouth and throat, but can occasionally be serious. NHS. Anaphylaxis. States that anaphylaxis is a life-threatening allergic reaction that happens very quickly and needs urgent medical help. Cleveland Clinic. GLP-1 Diet: What To Eat & Avoid. Advises that a GLP-1 eating pattern generally includes nutrient-dense foods such as fruits and vegetables, rather than banning specific fruits like banana.
10 Fruits For Weight Loss: Best Low-Calorie Fruits To Add To Your Diet
If you are trying to lose weight, fruit can be one of the easiest foods to add to your routine. It is naturally sweet, easy to carry, and far better than many processed snacks when you want something light between meals. Still, it helps to be realistic. Fruits for weight loss can support your progress, but they do not melt fat on their own. The real benefit comes from using them wisely as part of a balanced eating plan, regular activity, and sustainable habits. Introduction To Fruits For Weight Loss Fruit works well in a weight-loss plan because many fruits are rich in fibre, full of water, and naturally lower in calories than biscuits, desserts, or fried snacks. They can help you feel satisfied without making your meals too heavy. That is why fruits good for weight loss are usually the ones that help with fullness, portion control, and better food choices through the day. Whole fruit is usually the smarter choice because it keeps its fibre and takes longer to eat. Why Choose Fruits For Weight Loss? There are several reasons fruits for weight loss are so popular. First, many fruits are naturally lower in calories than packaged snack foods. Second, they contain fibre, which can help you stay full for longer. Third, many are high in water, which adds volume to your snack or meal without adding too many calories. When you choose fruit regularly, you may also find it easier to cut back on sweets, sugary drinks, and heavy snacks. That is why fruits good for weight loss can fit naturally into an everyday routine. How Fruits Support Healthy Weight Management Fruit supports healthy weight management in simple ways. It can help you feel full between meals. It can replace more calorie-dense snacks. It can add nutrients to your day without making your meals overly rich. It can also help you build a more balanced plate. That said, whole fruit and fruit juice are not the same. Juice is easy to drink quickly and usually contains less fibre. If your goal is satiety, whole fruit is the better option. Top 10 Fruits For Weight Loss 1. Apple Apples are one of the easiest fruits for weight loss to include in your day. They are filling, portable, and rich in fibre. You can eat one as a mid-morning snack or slice it into curd or oats for a simple meal. 2. Pear Pears are another excellent choice if you want fruits good for weight loss. They are rich in fibre and can help you feel satisfied for longer. A pear works well as an afternoon snack when you want something sweet but light. 3. Strawberry Strawberries are low in calories and easy to add to breakfast bowls, curd, or salads. They also bring colour and freshness to your meals. If you often crave desserts, strawberries can be a lighter option that still feels satisfying. 4. Blueberry Blueberries are small, but they can fit well into a balanced weight-loss plan. They are easy to portion and work well in smoothies, oats, or plain yoghurt. They are a practical choice when you want something sweet without reaching for a processed snack. 5. Orange Oranges are refreshing, easy to carry, and usually more filling when you eat them whole rather than as juice. Their fibre and water content make them a smart snack option. If you need a simple diet food for weight loss, a whole orange can be a far better choice than packaged juice. 6. Grapefruit Grapefruit is often mentioned in lists of fruits for weight loss because it is light and refreshing. It can fit well into breakfast or a snack plate. But there is one important caution. Grapefruit can interact with some medicines. If you take regular prescription medicines, ask your doctor or pharmacist before adding it often to your routine. 7. Watermelon Watermelon is high in water and can be very refreshing in hot weather. It feels light, which makes it useful when you want a snack that does not feel heavy. Portion still matters, but it can be a good swap for calorie-dense sweets or desserts. 8. Papaya Papaya is easy to digest for many people and works well as part of breakfast or a light evening snack. It is naturally sweet and often easy to include in Indian meal patterns. If you are looking for diet food for weight loss that feels simple and familiar, papaya is a practical option. 9. Kiwi Kiwi is rich in fibre and can add variety to your fruit intake. It works well in fruit bowls, curd, or as a small stand-alone snack. It is especially useful if you want variety and do not want to keep rotating the same fruits every day. 10. Avocado Avocado is different from many other fruits because it is higher in calories and contains more healthy fats. That does not make it a bad choice. In fact, small portions of avocado can help make meals feel more satisfying. You can add a few slices to toast, salads, or grain bowls. The key is portion control. Which Fruits Are Best For Different Weight-Loss Goals? Best Fruits To Keep You Full If fullness is your main goal, choose apples, pears, avocado, and berries. These can help you stay satisfied for longer and may reduce the urge to snack on less helpful foods. Best Water-Rich Fruits For Light Snacking If you want lighter snacks, watermelon, orange, papaya, and other melon varieties can work well. These are especially useful on hot days when you want something fresh. Best Fruits For Fibre Intake If you want to improve fibre intake, apples, pears, kiwi, and berries are strong choices. Fibre is one reason fruits good for weight loss can be so useful in a balanced routine. Are Fruits Enough For Weight Loss On Their Own? No. Fruit can help, but it is not enough on its own. A fruit-only plan may sound appealing, especially if you are searching for a fruit diet for weight loss in 7 days, but it is not a balanced long-term approach. You still need enough protein, healthy fats, whole grains, pulses, and vegetables to support your energy, muscle health, and overall nutrition. Fruit should support your diet, not replace everything else in it. How To Add Fruits To Your Diet Food For Weight Loss The easiest way to use fruit well is to make it replace less helpful foods, not simply add it on top of everything else. You can: Eat fruit as a snack instead of biscuits or sweets Add fruit to breakfast with oats, curd, or eggs on the side Pair fruit with nuts or seeds for better staying power Choose whole fruit over juice Keep cut fruit ready so healthy choices feel easy When you build meals this way, fruit becomes part of practical diet food for weight loss rather than a random extra. A Simple 7-Day Fruit-Inclusive Plan For Weight Loss If you were looking for a fruit diet for weight loss in 7 days, this balanced version is a safer and more useful approach. Day 1: Add apple slices to breakfast and have papaya as an evening snack. Day 2: Eat a pear between meals and add berries to curd. Day 3: Choose orange as a mid-morning snack and watermelon in the afternoon. Day 4: Add kiwi to breakfast and keep a small fruit bowl for the evening. Day 5: Pair strawberries with plain yoghurt or curd. Day 6: Include papaya after breakfast and an apple later in the day. Day 7: Use a mixed fruit bowl with controlled portions and keep the rest of your meals balanced. This kind of plan works better because it keeps fruit inside a realistic eating pattern. Fruits To Be Mindful Of During Weight Loss Fruit is healthy, but some forms need a little more care. Dried fruits are easy to overeat because they are small and concentrated. Fruit juice is less filling than whole fruit. Canned fruit in syrup can carry extra sugar. Fruit desserts with cream, ice cream, or sweet syrups can quickly become high-calorie foods. So yes, fruit can support weight loss, but how you eat it matters. Can Fruit Cause Weight Gain If You Eat Too Much? Any food can contribute to weight gain if portions are too large and your total calorie intake stays high. That does not mean you need to fear fruit. For most people, whole fruit is a far better choice than processed snacks. The answer is not to avoid fruit, but to keep portions sensible and your meals balanced. Allergy And Digestive Considerations Before Increasing Fruit Intake Most people tolerate fruit well, but a few may notice problems. Some fruits may trigger itching in the mouth or throat, especially if you have pollen-related allergies. Others may cause bloating, acidity, or loose motions if you suddenly increase your intake a lot. Acidic fruits may also bother you if you already struggle with reflux. If fruit causes swelling, rash, breathing trouble, repeated stomach upset, or itching after eating, seek medical advice. In some cases, an allergy assessment may be needed. Symptoms such as itching or tingling after certain raw fruits can happen in oral allergy syndrome. Benefits Of A Fruit-Rich Diet For Weight Loss A fruit-rich diet can support your goals in several ways: It can help you feel fuller between meals It can reduce reliance on processed snacks It can improve fibre intake It can support hydration It can make meal planning easier It can add variety and nutrients to your routine It can make healthy eating feel more enjoyable How To Combine Fruits With A Balanced Weight-Loss Routine Fruit works best when it fits into a wider plan. Keep moving regularly. Eat balanced meals. Sleep well. Stay hydrated. Watch portion sizes. Use fruit to support your routine, not to distract from the rest of it. If you are already following a medically guided GLP-1 Diet, fruit can still be part of your meals and snacks, depending on your tolerance and overall plan. You may also have read about the benefits of banana as a quick snack. Banana can absolutely fit into a healthy routine too. The key is to focus on your full day of eating, not to label one fruit as good and another as bad. When To Monitor Your Health During A Weight-Loss Journey If you are trying to lose weight and also have diabetes, thyroid issues, cholesterol concerns, fatty liver, or PCOS, it may help to track your health markers from time to time. This can include blood sugar, lipid profile, liver function, and thyroid testing where appropriate. If you are following a structured medical plan, packages such as a GLP 1 Test Package or GLP-1 Monitor Package may be relevant if your doctor advises ongoing monitoring. Conclusion The best fruits for weight loss are the ones you enjoy, can eat regularly, and can fit into a balanced way of eating. Apples, pears, berries, citrus fruits, watermelon, papaya, kiwi, and even avocado can all play a useful role when portions are sensible and your meals stay balanced. If you want to take a more proactive approach to your health while working on your weight goals, Metropolis Healthcare can support you with 4,000+ tests, full body checkups, home sample collection, and easy booking through the website, app, call, or WhatsApp. That way, you can pair healthy habits with preventive health screening and stay informed about your health markers over time. FAQs Are Fruits Good For Weight Loss? Yes, fruits can be very helpful in a weight-loss plan. Many are lower in calories, rich in fibre, and easier to snack on than processed foods. Can I Lose Weight With A Fruit-Only Diet? You may lose some weight in the short term, but a fruit-only diet is not balanced and is hard to sustain. It can also leave you low in protein and other nutrients. What Is The Best Fruit For Weight Loss In 7 Days? There is no single best fruit. Apples, pears, berries, oranges, papaya, and watermelon are all good options. The better question is whether you can include them consistently in a balanced plan. Are Fruits For Weight Loss Low In Calories? Many are, but not all fruits are equally low in calories. Watermelon and berries tend to be lighter, while avocado and dried fruits are more energy-dense. Both can still fit into a healthy plan if portions are sensible. Which Fruits Keep You Full For Longer? Apples, pears, berries, and avocado often help with fullness because of their fibre, water, or fat content. Is Fruit Juice As Good As Whole Fruit For Weight Loss? Usually not. Whole fruit is more filling and gives you more fibre. Juice is easier to drink quickly and may not keep you satisfied for as long. Should I Avoid Fruits If I Am Following GLP-1 Medication? Not necessarily. Many people can still eat fruit while using GLP-1 Agonists. The right choice depends on your appetite, digestion, blood sugar goals, and your doctor’s advice. Grapefruit is a separate issue because it can interact with some medicines. References World Health Organization. Healthy Diet. 2026. National Institute of Diabetes and Digestive and Kidney Diseases. Eating & Physical Activity To Lose Or Maintain Weight. 2026. NHS. The Eatwell Guide. Updated 2025. Centers for Disease Control and Prevention. Healthy Habits: Fruits And Vegetables To Manage Weight. 2025. U.S. Food and Drug Administration. Grapefruit Juice And Some Drugs Don’t Mix. 2021. Dreher ML. Whole Fruits and Fruit Fiber Emerging Health Effects. Nutrients. 2018;10(12). PMID: 30487459. Bertoia ML, Mukamal KJ, Cahill LE, Hou T, Ludwig DS, Mozaffarian D, Willett WC, Hu FB, Rimm EB. Changes in Intake of Fruits and Vegetables and Weight Change in United States Men and Women Followed for Up to 24 Years: Analysis from Three Prospective Cohort Studies. PLoS Med. 2015;12(9):e1001878. PMID: 26394033. National Institute of Allergy and Infectious Diseases. Characterizing Food Allergy & Addressing Related Disorders. 2024.
Overweight: Symptoms, Causes, BMI Range, Risks, And How To Manage It
If you have been wondering whether your weight is affecting your health, you are not alone. Many people look for clear and trustworthy information before taking the next step. The term overweight refers to having a body weight that is higher than what is generally considered healthy for your height, most often because of excess body fat. That said, your weight is only one part of the picture. Your waist size, body composition, daily habits, and blood test results also matter. The good news is that with the right support and steady lifestyle changes, you can manage overweight safely and improve your overall health. What Is Overweight? Overweight means you weigh more than the recommended range for your height. In most cases, this happens when your body stores extra fat over time. However, weight alone does not define your health. Some people may have a higher body weight because of more muscle, larger body frame, or fluid retention. This is why doctors do not rely on the weighing scale alone. They usually look at your Body Mass Index, waist circumference, lifestyle, and metabolic health before making a full assessment. What Qualifies As Being Overweight? In adults, overweight is usually identified using Body Mass Index, also called BMI. A BMI between 25 and 29.9 is generally classified as overweight. A BMI of 30 or above falls into the obesity range. Even so, BMI is only a screening tool. It does not show where your body fat is stored or how healthy your metabolism is. For example, extra fat around your waist may raise your risk of health problems more than fat stored elsewhere. In children and teenagers, doctors do not use the same adult BMI ranges. They assess weight using BMI-for-age percentiles because age and sex affect growth patterns. Overweight BMI Range And How It Is Measured How BMI Is Calculated BMI is calculated by dividing your weight in kilograms by your height in metres squared. For example, if you weigh 70 kg and your height is 1.7 metres, your BMI is calculated as: 70 ÷ (1.7 × 1.7) = 24.2 Adult BMI Categories Adults are generally grouped like this: Below 18.5: Underweight 18.5 to 24.9: Healthy weight 25 to 29.9: Overweight 30 and above: Obesity Why BMI Alone Does Not Tell The Full Story BMI is useful, but it has limits. It does not measure body fat directly. It also cannot tell whether your weight comes from muscle or fat. That is why your doctor may also check: Waist circumference Blood pressure Blood sugar Cholesterol levels Liver health Thyroid function in some cases Symptoms Of Overweight Overweight does not always cause obvious symptoms in the early stages. Some people feel completely well. Others may notice physical or emotional changes over time. Common overweight symptoms may include: Feeling tired or low on energy Getting breathless during mild activity Sweating more than usual Snoring or disturbed sleep Joint pain, especially in the knees Back pain Reduced stamina or mobility Skin irritation in body folds Low confidence or body image concerns If you also notice rapid weight gain, severe fatigue, irregular periods, or swelling, it is worth speaking to a doctor. These may point to an underlying health condition. Causes Of Overweight There is rarely one single cause of overweight. In most cases, it develops when your calorie intake stays higher than the energy your body uses. But several factors can contribute to this. Lifestyle Causes Daily habits play a major role. Common causes include: Eating more calories than your body needs Frequent intake of sugary drinks and processed foods Large portion sizes Low levels of physical activity Sitting for long hours Poor sleep habits Medical And Biological Causes Your weight can also be affected by factors beyond your control, such as: Family history and genetics Hypothyroidism Polycystic ovary syndrome, or PCOS Metabolic changes with age Certain medicines, including some steroids, antidepressants, and diabetes medicines Stress And Emotional Factors Stress can affect both your appetite and your routine. When you feel stressed, you may reach for comfort foods that are high in sugar or fat. Stress can also affect sleep, which may disturb hunger hormones and make cravings harder to manage. Overweight Vs Obese: What Is The Difference? Overweight and obesity both refer to excess body weight, but they are not the same. If your BMI is between 25 and 29.9, you are generally considered overweight. If your BMI is 30 or higher, you fall into the obesity range. The difference matters because health risks often rise as body fat increases, especially if fat collects around your waist. Still, these terms should be used only as medical categories. They are not labels of personal worth. What matters most is understanding your current health and taking realistic steps to improve it. Health Risks And Problems Linked To Overweight Being overweight can place extra strain on your body. The risk becomes higher if you also have high waist circumference, poor diet, low activity, or a family history of metabolic disease. Metabolic Health Risks Overweight may increase your risk of: Insulin resistance Prediabetes and diabetes High triglycerides Low HDL, or good cholesterol Metabolic syndrome Fatty liver disease Heart And Circulation Risks Excess body fat can affect your heart and blood vessels. This may increase the risk of: High blood pressure High cholesterol Cardiovascular Disease Heart disease Stroke Bone, Joint, And Breathing Problems Extra weight may also affect how you move and breathe. You may be more likely to develop: Knee pain Osteoarthritis Back pain Sleep apnoea Breathlessness during activity Other Long Term Risks Overweight can also be linked to: Gallbladder problems Kidney disease Fertility problems Pregnancy-related complications Sexual health concerns A higher risk of some types of Cancer Not everyone with overweight will develop these conditions. But knowing the risks can help you act early. Overweight And Mental Health Your emotional health matters just as much as your physical health. Living with overweight can affect the way you feel about yourself, especially if you face social judgement or struggle with repeated weight loss efforts. Some people experience: Low self-esteem Frustration Anxiety Depression Shame around eating or body image These feelings can make it harder to stay active, eat well, or seek help. If your weight is affecting your mental wellbeing, support from a doctor, counsellor, or nutrition expert can make a real difference. The Role Of Stress In Overweight Stress can quietly drive weight gain over time. When stress becomes constant, your body produces hormones such as cortisol that may increase hunger and cravings. Stress can also lead to: Emotional eating Poor sleep Lower motivation to exercise Irregular meal timings More cravings for sugary or high-fat foods Managing stress does not mean doing everything perfectly. Small, consistent steps such as regular sleep, mindful eating, walking, breathing exercises, and professional support can help you break the cycle. Tests To Consider If You Are Overweight If you are overweight, a health check can help you understand whether your weight is affecting your metabolism, heart health, or liver health. Your doctor may suggest some or all of the following: BMI calculation Waist circumference measurement Blood pressure check Fasting blood sugar or HbA1c Lipid profile Liver function tests Thyroid profile, if clinically needed Kidney function tests Vitamin D or other tests if symptoms suggest a deficiency These tests are not about judgement. They help identify risks early and guide the right plan for you. Depending on your needs, your doctor may also advise a GLP 1 Test Package or a GLP-1 Monitor Package as part of structured metabolic monitoring. How To Manage Overweight Safely And Sustainably There is no one perfect method that works for everyone. The safest approach is one you can maintain over time. Build A Balanced Diet A Balanced Diet helps you manage hunger, support metabolism, and protect your overall health. Try to include: Vegetables and fruits Whole grains Pulses, beans, eggs, fish, or lean meats Healthy fats in moderate amounts Adequate water intake It also helps to reduce sugary drinks, highly processed snacks, fried foods, and oversized portions. You do not need an extreme plan. A realistic Diet Chart or a personalised Weight Loss Diet is often more effective than short-term restriction. If you are exploring newer treatment approaches, your doctor may also guide you on a GLP-1 Diet alongside lifestyle changes. Move More In Ways You Can Sustain Physical activity supports weight control, heart health, blood sugar balance, and mood. Aim for regular movement that fits your routine, such as: Brisk walking Cycling Swimming Home workouts Strength training Most adults benefit from at least 150 minutes of moderate activity each week. Strength training is useful too because muscle burns more energy than fat and supports long-term weight management. Improve Sleep And Daily Routine Poor sleep can affect appetite and cravings. Try to get enough sleep each night and keep a consistent routine. Simple habits can help: Sleep and wake at similar times Avoid heavy meals late at night Reduce screen time before bed Plan meals in advance Manage Stress And Emotional Eating If stress or emotions affect your food choices, start with small changes. Keep regular meals, notice triggers, and avoid skipping food for long hours. Mindful eating, journalling, counselling, or behavioural therapy can help if emotional eating feels hard to control. Seek Medical Guidance When Needed If you have rapid weight gain, repeated failed attempts to lose weight, symptoms of hormonal imbalance, or obesity-related risks, speak to a doctor. In some cases, your treatment plan may include nutrition therapy, exercise support, counselling, or medicines such as GLP-1 Agonists. How Long Does It Take To Lose Weight? Healthy weight loss takes time. Your body usually responds better to gradual and steady changes than to crash diets. How long it takes depends on: Your starting weight Your eating habits Your activity level Sleep and stress Medical conditions such as PCOS or thyroid disorders The type of plan you follow A slow and sustainable pace is often easier to maintain. Instead of focusing only on the weighing scale, look at the bigger picture. Better energy, improved sleep, smaller waist size, and healthier blood test results are all signs of progress. When Should You Speak To A Doctor? You should consider medical advice if: You have unexplained or sudden weight gain You feel tired all the time You snore heavily or suspect sleep apnoea You have joint pain or breathlessness You have irregular periods or signs of hormonal imbalance You have a family history of diabetes or heart disease You struggle to lose weight despite consistent effort A timely check-up can help rule out underlying causes and reduce future health risks. Preventing Further Weight Gain If you are already overweight, preventing further gain is an important first step. You do not need a perfect routine. Focus on habits you can repeat. Helpful steps include: Eat regular, balanced meals Keep healthy snacks ready Reduce sugary drinks Stay active throughout the day Strength train if possible Sleep well Manage stress early Monitor your health markers regularly These simple actions can lower your risk of overweight problems and support better long-term health. Take Charge Of Your Health With Timely Screening Managing overweight is not only about appearance or numbers. It is about protecting your future health and feeling better in your daily life. The right combination of healthy food, activity, sleep, stress control, and medical guidance can help you move in the right direction. Routine blood tests and full body checkups can also help you track important markers such as blood sugar, cholesterol, liver health, and thyroid function. This is especially useful if you want to take a preventive approach rather than waiting for symptoms to appear. Metropolis Healthcare supports you at every step with accurate results, advanced diagnostic technology, expert-backed testing, and access to 4,000+ tests. Whether you want routine screening, speciality testing, or wellness monitoring, you can book with ease through the website, app, call, or WhatsApp. With reliable reports, quick turnaround time, and a strong home sample collection network across 10,000 touchpoints, Metropolis Healthcare makes proactive health management simpler and more convenient. FAQs Can Overweight Be Reversed? Yes, in many cases, overweight can be managed successfully with consistent lifestyle changes. A healthier diet, regular physical activity, better sleep, and stress management can help you reduce excess weight and improve your metabolic health. The key is to choose habits you can maintain. What Are The First Steps To Take When Managing Overweight? Start by checking your BMI and waist size. Then review your eating habits, activity level, sleep, and stress. A simple health check-up can help identify issues such as high blood sugar, cholesterol imbalance, or fatty liver disease. From there, you can follow a realistic plan. What Tests Should I Do To Check Overweight Health Risks? Common tests include fasting blood sugar or HbA1c, lipid profile, liver function tests, kidney function tests, blood pressure, and sometimes a thyroid profile. Your doctor may personalise tests based on your symptoms, medical history, and family history. How Long Does It Take To Lose Weight If You Are Overweight? There is no fixed timeline. Safe weight loss usually happens gradually. The exact pace depends on your starting point, medical conditions, routine, and how consistently you follow your plan. Slow progress is still meaningful progress. How Many Kg Is Overweight? There is no single number in kilograms that defines overweight for everyone. It depends on your height. Two people can weigh the same in kilograms but fall into different BMI categories because their heights are different. What Qualifies As Being Overweight? In adults, a BMI between 25 and 29.9 usually qualifies as overweight. Doctors may also look at waist circumference, body fat distribution, and blood test results to understand your overall health risk. Is 90 Kg Good For 5'9"? At 5'9", or about 1.75 metres, a weight of 90 kg gives a BMI of around 29.4. That falls in the overweight range. However, BMI is only a screening tool. Your muscle mass, waist size, and metabolic health also matter. Which Weight Is Ideal For Your Height? There is no perfect number that suits everyone. A healthy weight range usually depends on your height, body composition, age, and overall health. BMI can offer a general guide, but your doctor can help you understand what is appropriate for you. Is BMI Always Accurate? No. BMI is useful for screening, but it does not measure body fat directly. It may overestimate or underestimate health risk in some people, especially athletes, older adults, or those with high muscle mass. Can You Be Overweight And Still Have Normal Blood Test Results? Yes, some people with overweight may still have normal blood pressure, blood sugar, and cholesterol for a period of time. However, this does not mean risk is absent. Regular monitoring is still important because metabolic changes can develop gradually. References World Health Organization. Obesity and overweight. WHO. National Institutes of Health. Overweight and obesity. NIH. National Institute of Diabetes and Digestive and Kidney Diseases. Health Risks of Overweight and Obesity. NIDDK, National Institutes of Health. Tong SYC, Davis JS, Eichenberger E, Holland TL, Fowler VG. Staphylococcus aureus infections: epidemiology, pathophysiology, clinical manifestations, and management. Clin Microbiol Rev. 2015;28(3):603-661. PMID: 26016486. Bray GA, Heisel WE, Afshin A, et al. The science of obesity management: an Endocrine Society scientific statement. Endocr Rev. 2018;39(2):79-132. Diabetes Prevention Program Research Group. Long-term effects of lifestyle intervention or metformin on diabetes development and microvascular complications over 15-year follow-up: the Diabetes Prevention Program Outcomes Study. Lancet Diabetes Endocrinol. 2015;3(11):866-875. Chalasani N, Younossi Z, Lavine JE, et al. The diagnosis and management of nonalcoholic fatty liver disease: practice guidance from the American Association for the Study of Liver Diseases. Hepatology. 2018;67(1):328-357. Wadden TA, Tronieri JS, Butryn ML. Lifestyle modification approaches for the treatment of obesity in adults. Am Psychol. 2020;75(2):235-251. Practice Committee of the American Society of Reproductive Medicine. Obesity and reproduction: a committee opinion. Fertil Steril. 2021;116(5):1266-1285. Chu DT, Minh Nguyet NT, Nga VT, et al. An update on obesity: mental consequences and psychological interventions. Diabetes Metab Syndr. 2019;13(1):155-160.
Is Sweet Potato Good For Weight Loss? Nutrition, Benefits, And Best Ways To Eat
If you are trying to lose weight, you may wonder whether sweet potato deserves a place on your plate. The simple answer is yes. Sweet potato can support weight loss when you eat it in the right portion and prepare it in a healthy way. It is filling, naturally rich in fibre, and gives you steady energy. At the same time, no single food causes weight loss on its own. Your overall diet chart, activity level, portion size, and cooking method still matter most. Is Sweet Potato Good For Weight Loss? Yes, sweet potato can be a smart choice in a weight loss plan. It is nutrient-dense, satisfying, and relatively low in calorie density compared with many processed snacks and fried foods. This means you can eat a reasonable serving, feel full, and still stay within your daily calorie goals. That is why sweet potato for weight loss is often recommended in balanced meal plans. However, the benefit depends on how you eat it. A boiled or baked sweet potato is very different from deep-fried sweet potato fries or a sweet potato dessert loaded with butter and sugar. The potato itself is not the problem. It is usually the portion and preparation that decide whether it helps or hinders your progress. What Makes Sweet Potato Good For Weight Loss? Sweet potato works well in a weight loss diet for a few practical reasons. First, it contains fibre. Fibre slows digestion and helps you feel full for longer. This can make it easier to manage hunger and cut down on unnecessary snacking. Second, it has high water content. Foods with more water and fibre can help you feel satisfied without adding too many calories. Third, sweet potato gives you complex carbohydrates. These digest more slowly than highly refined carbohydrates and can give you steadier energy through the day. Finally, sweet potato is nutrient-rich. When you are trying to lose weight, it helps to choose foods that give you vitamins and minerals along with calories. That makes your diet chart easier to maintain and more nourishing. Nutritional Profile Of Sweet Potato A medium sweet potato usually provides: About 110 to 115 calories Around 26 grams of carbohydrates About 3 to 4 grams of fibre About 2 grams of protein Very little fat Vitamin A Vitamin C Potassium Vitamin B6 This is one reason sweet potato benefits go beyond weight management. It can also support overall nutrition when included as part of a balanced meal. How Sweet Potato Helps In Weight Loss And Fat Loss Sweet potato can help with weight loss because it supports fullness. When you feel satisfied after a meal, you are less likely to overeat later in the day. Its fibre content plays a key role here. Fibre can slow stomach emptying and support satiety, which may help you reduce your overall calorie intake. This does not mean sweet potato melts fat. Fat loss still happens when you stay in a calorie deficit over time. What sweet potato does is make that process feel more manageable. It gives you a filling source of carbohydrate that can fit into lunch, dinner, or even a balanced snack. If you are looking at sweet potato fat loss benefits, this is the main point to remember. It supports your plan. It does not replace your plan. The Role Of Fibre In Sweet Potato For Weight Loss Fibre is one of the biggest reasons sweet potato can be helpful when you want to lose weight. It adds bulk to your meals and can help you feel full sooner. It may also help you stay satisfied for longer after eating. This can make it easier to avoid frequent grazing and late cravings. Fibre also supports digestion and gut health. That matters because a comfortable, balanced eating routine is easier to follow consistently. For the best fibre intake, eat sweet potato with the skin on after washing it properly. The skin adds extra texture and fibre to your meal. Sweet Potato Vs Regular Potato For Weight Loss Sweet potato and regular potato can both fit into a healthy weight loss plan. You do not need to fear either one. Sweet potato is often chosen because it is naturally sweet, rich in beta-carotene, and slightly higher in fibre than many common potato varieties. It may also give a steadier blood sugar response depending on the cooking method. Regular potato can also be part of a healthy meal when it is boiled, baked, or roasted without heavy toppings. So this is not about calling one potato good and the other bad. The better question is how you cook it, what you pair it with, and how much you eat. In most cases, a plain boiled or baked potato will serve you better than a fried version of either type. Best Ways To Eat Sweet Potato For Weight Loss If you want to know how to eat sweet potato for weight loss, keep it simple. The best options include: Boiled sweet potato Steamed sweet potato Baked sweet potato Roasted sweet potato with a small amount of oil Sweet potato paired with dal, eggs, paneer, fish, chicken, or salad Sweet potato added to a balanced diet chart with protein and vegetables Try to limit: Deep-fried sweet potato Sweet potato chips Sweet potato with butter, cream, cheese sauce, or sugary syrups Oversized portions Sweet potato eaten alongside other heavy starches in the same meal A good rule is to treat sweet potato as your main carbohydrate for that meal, rather than adding it on top of rice, bread, and dessert. Can You Eat Sweet Potato Every Day For Weight Loss? Yes, you can eat sweet potato regularly if it fits your calorie needs and overall diet chart. There is no rule that says you must avoid it every day. But variety still matters. Your body benefits when you include different vegetables, fruits, proteins, whole grains, and legumes across the week. If you eat sweet potato daily, pay attention to portion size and balance. A simple serving with protein and vegetables is very different from a large restaurant-style portion topped with extra fat or sugar. So yes, daily intake can work, but moderation is still important. Sweet Potato Recipes For Weight Loss Boiled Sweet Potato Chaat Toss boiled sweet potato cubes with onion, tomato, coriander, lemon juice, black pepper, and a little chaat masala. Baked Sweet Potato Wedges Slice into wedges, brush lightly with oil, and season with paprika, pepper, and herbs before baking. Sweet Potato And Veg Bowl Combine roasted sweet potato with sautéed vegetables, sprouts, and a protein source for a balanced meal. Mashed Sweet Potato With Herbs Mash boiled sweet potato with garlic, pepper, and fresh herbs instead of butter and cream. Sweet Potato Salad With Protein Mix sweet potato cubes with cucumber, greens, chickpeas, eggs, or grilled chicken for a filling lunch. Stuffed Baked Sweet Potato Fill a baked sweet potato with paneer bhurji, beans, or mixed vegetables for a simple dinner. When Sweet Potato May Not Support Weight Loss Sweet potato is healthy, but it may not help you lose weight in every form. It can work against your goal when it is: Deep-fried Served with sugary toppings Turned into high-calorie desserts Eaten in very large portions Added to a meal that is already high in calories For example, baked sweet potato can be part of a healthy dinner. But sweet potato casserole, candied sweet potato, or loaded fries can quickly raise the calorie count. So the issue is not whether sweet potato is healthy. The issue is whether the full meal supports your goal. Who Should Be Careful About Eating Sweet Potato? Most people can enjoy sweet potato as part of a balanced diet. Still, some situations need a little care. If you have diabetes or have been told to monitor your carbohydrate intake, portion size matters. Sweet potato is still a carbohydrate-rich food, so it should be planned within your overall meal pattern. If you notice bloating or digestive discomfort after eating it, try a smaller portion or a simpler preparation method. If you have a medical condition that affects digestion, kidney health, or blood sugar, it is best to follow your doctor or dietitian’s advice on how often and how much you should eat. Simple Tips To Add Sweet Potato To A Weight Loss Diet Keep these tips in mind if you want to include sweet potato in your meals: Choose boiled, steamed, baked, or roasted preparations Keep portions sensible Pair it with protein for better balance Add vegetables to increase volume and nutrition Avoid turning it into a high-sugar or high-fat dish Include it within a realistic diet chart that you can follow consistently The best weight loss foods are the ones that help you stay full, stay nourished, and stay consistent. Sweet potato can do all three when used wisely. Conclusion Sweet potato can be a healthy and satisfying part of your weight loss journey. It is rich in fibre, naturally filling, and easy to include in balanced meals. The key is to focus on healthy cooking methods, sensible portions, and your overall eating pattern. If you want to manage your weight in a more informed way, it helps to combine healthy food choices with regular preventive health checks. Metropolis Healthcare supports your wellness journey with 4,000+ tests, full body checkups, speciality testing, accurate reports, and convenient home sample collection through a strong service network. You can book easily through the website, app, call, or WhatsApp, making it simpler to stay on top of your health while building better habits. FAQs Can Sweet Potato Help With Weight Loss? Yes, sweet potato can help with weight loss because it is filling and rich in fibre. It can support portion control and reduce hunger between meals. But it works best as part of a calorie-conscious and balanced diet. How Many Calories Does Sweet Potato Have? The calorie count depends on the size and how it is cooked. A medium plain sweet potato generally has: About 110 to 115 calories Very little fat Around 26 grams of carbohydrates About 3 to 4 grams of fibre Once you fry it or add butter, sugar, or creamy toppings, the calorie count rises quickly. What Is The Best Way To Cook Sweet Potato For Weight Loss? The best ways are boiling, steaming, baking, or roasting with very little oil. These methods keep the dish simple and help you avoid extra calories from deep frying or rich toppings. Can You Eat Sweet Potato At Night For Weight Loss? Yes, you can. There is nothing wrong with eating sweet potato at night if it fits your total calorie intake and portion plan. The better focus is the full meal, not the time on the clock. Is Sweet Potato Better Than Regular Potato For Weight Loss? Sweet potato is often preferred because it is rich in fibre and vitamin A, but regular potato can also fit into a healthy diet. The cooking method, toppings, and portion size matter more than choosing one potato over the other. Are GLP-1 Medications Suitable With Sweet Potato? In general, sweet potato can still fit into meals for many people who are following a GLP-1 Diet or using GLP-1 Agonists. There is no common rule that says sweet potato and these medicines should not be taken together. However, these medicines can reduce appetite and slow digestion in some people, so smaller portions and simple cooking methods may feel more comfortable. If you are managing blood sugar, appetite, or side effects, follow your doctor’s advice. Depending on your needs, you may also come across broader monitoring options such as a GLP 1 Test Package or GLP-1 Monitor Package as part of your overall health review. References U.S. Department of Agriculture. FoodData Central. Sweet potato nutrient data. Agricultural Research Service, U.S. Department of Agriculture. National Library of Medicine. Dietary Fiber. MedlinePlus. Updated April 25, 2023. Howarth NC, Saltzman E, Roberts SB. Dietary fiber and weight regulation. Nutr Rev. 2001;59(5):129-139. PMID: 11396693. Clark MJ, Slavin JL. The effect of fiber on satiety and food intake: a systematic review. J Am Coll Nutr. 2013;32(3):200-211. PMID: 23885994. Bahado-Singh PS, Riley CK, Wheatley AO, Lowe HIC. Relationship between processing method and the glycemic indices of ten sweet potato (Ipomoea batatas) cultivars commonly consumed in Jamaica. J Nutr Metab. 2011;2011:584832. PMID: 22132322. National Library of Medicine. Semaglutide Injection. MedlinePlus Drug Information. Last revised February 15, 2026.
National Walking Day 2026: Benefits Of Walking For Heart Health, Weight Loss, And Fitness
National Walking Day is a simple reminder that better health does not always begin with a big change. Sometimes, it starts with one walk. Observed on the first Wednesday of April, National Walking Day 2026 falls on 1 April. The day encourages you to take at least 30 minutes to walk and make movement a regular part of your life. That may sound small, but regular walking can support your heart, help with weight management, improve fitness, and reduce stress. If you have been meaning to become more active, this day offers a realistic place to begin. What Is National Walking Day? National Walking Day is an annual health awareness day that encourages people to walk for at least 30 minutes and take simple steps towards a more active lifestyle. It was started to highlight how regular walking can improve overall health, especially heart health. In a time when many people spend long hours sitting at desks, in cars, or in front of screens, walking remains one of the easiest ways to add movement to your day. You do not need a gym membership or expensive equipment to start. A comfortable pair of shoes and a little time are often enough. The History Of National Walking Day National Walking Day was established in 2007 by the American Heart Association. The idea was clear and practical: encourage people to move more and sit less. Over time, the day has become more than a one-day event. It now serves as a reminder that walking is a simple habit with long-term health benefits. It supports not only your heart but also your energy levels, fitness, sleep, mood, and daily routine. That is what makes the day so relevant even now. It focuses on a type of exercise that is accessible, low-impact, and easy to build into everyday life. Why Walking Is One Of The Best Forms Of Exercise Walking is often underestimated because it feels simple. But simple does not mean ineffective. Walking is one of the most practical forms of exercise because it is: Easy to start, even if you have been inactive Gentle on your joints compared with high-impact workouts Suitable for different age groups and fitness levels Flexible enough to fit into your day Possible indoors or outdoors Easy to continue over time This matters because the best form of exercise is often the one you can do consistently. Benefits Of Walking For Heart Health Walking is especially valuable for your heart. Regular walking can support cardiovascular health in several ways: It helps improve blood circulation It can help lower blood pressure over time It supports healthy cholesterol levels when combined with a balanced lifestyle It helps reduce the risks linked to long periods of sitting It strengthens your heart by making it work more efficiently It supports better stamina for daily activity A brisk walk can be particularly helpful because it raises your heart rate without putting too much strain on your body. If you are looking for a manageable way to care for your heart, walking is a strong place to begin. Can Walking Help With Weight Loss? Walking can support weight loss, especially when you do it regularly and combine it with healthy eating habits. Here is how walking helps: It burns calories It supports your metabolism It can reduce sedentary time, which is linked to weight gain It is easier for many people to sustain than intense exercise routines It can help you stay consistent, which matters most for long-term results Walking alone may not lead to rapid weight loss, but it is often an effective and realistic part of a weight management plan. Even short walks done daily can add up over time. The Fitness Benefits Of Walking Walking does more for your fitness than many people realise. With consistency, it can improve how your body feels and functions. Some of the key fitness benefits include: Better endurance Improved stamina Greater lower-body strength Better balance and coordination Improved joint mobility More energy for everyday activities You can also make walking more challenging as your fitness improves. You can walk faster, choose a longer route, add gentle inclines, or include intervals of brisk walking. How Walking Supports Mental Well-Being Walking is not only good for your body. It can also support your mental well-being. A short walk can help you step away from stress, reset your mind, and feel more refreshed. Regular walking may help: Reduce stress Improve mood Support better sleep Ease mental fatigue Create a sense of routine and control Even a walk during a work break can help you feel calmer and more focused. If you feel overwhelmed by complicated fitness plans, walking offers a gentler and more reassuring approach. How Much Walking Do You Really Need? You do not need to walk for hours to see benefits. Even 30 minutes a day can make a meaningful difference. You can do this in one stretch or break it into smaller sessions during the day. For example, three 10-minute walks can still help you move more and reduce long periods of sitting. If you are just starting, begin with a comfortable pace and a shorter duration. As your stamina improves, you can gradually increase your speed or distance. What matters most is consistency. A habit you can maintain is far more useful than a routine you cannot stick with. National Walk To Work Day And How It Connects National Walk To Work Day is a separate observance, but it connects closely with the message of National Walking Day. Both encourage you to bring more movement into your daily routine. Walking to work may not be possible for everyone, but the idea behind it is practical. You can still: Walk part of your commute Get off public transport one stop earlier Park a little farther away Take a short walk before starting work Use part of your lunch break to walk These small choices can make walking feel less like a task and more like a normal part of your day. How To Celebrate National Walking Day 2026 You do not need an elaborate plan to take part. You just need to get moving. Take A 30-Minute Walk Use the day as your starting point. Walk around your neighbourhood, office campus, or a nearby park. Walk With Someone A friend, family member, or colleague can make the walk more enjoyable and easier to stick with. Take Walking Breaks At Work Get up from your desk and add short walks into your day. Choose Walking Over Short Rides For nearby errands, consider walking instead of driving. Make It Social Encourage your team or loved ones to join in and build a healthier routine together. Use It To Start A Habit Let National Walking Day be the day you begin walking regularly, not just once. Tips To Start Walking Safely And Consistently If you are new to walking or coming back after a long break, start gently. Wear comfortable and supportive shoes Begin at a pace that feels manageable Stay hydrated, especially in warm weather Keep your posture upright and relaxed Warm up if needed, especially before brisk walking Increase time and intensity gradually Listen to your body and rest when needed If you have an existing heart condition, joint pain, or another medical concern, it is sensible to speak to your doctor before starting a new exercise routine. Making Walking Part Of Your Everyday Routine Walking becomes more effective when it becomes part of your normal day. You can try: A short walk in the morning A walk after meals Walking during phone calls A quick stroll during work breaks Evening walks with family Weekend walks in a park or open space Many people also notice the Benefits of Morning Walk, such as a fresh start to the day, better focus, and a greater chance of staying consistent with exercise. You do not need the perfect routine. You just need one that works for you. Conclusion National Walking Day is a reminder that health does not always require dramatic changes. A regular walk can support your heart, help with weight management, improve fitness, and reduce daily stress. The important thing is to begin. One walk can become a routine. One routine can become a healthier lifestyle. If you are working on your preventive health goals, Metropolis Healthcare can support you with a wide range of diagnostic services, including full body checkups and doctor-advised health tests, along with convenient home sample collection and easy booking options. Frequently Asked Questions What Are The Benefits Of Walking Every Day? Walking every day can support heart health, improve stamina, help manage weight, reduce stress, and improve overall fitness. It also helps reduce the effects of sitting for long hours. Can Walking Help In Weight Loss? Yes, walking can help with weight loss when done regularly and combined with a balanced diet. It helps burn calories and supports a more active lifestyle. How Does Walking Improve Heart Health? Walking improves circulation, supports healthy blood pressure, helps strengthen the heart, and reduces the risks linked to inactivity. Brisk walking may offer added cardiovascular benefits. What Is The Best Time Of Day To Walk For Fitness? The best time is the time you can maintain regularly. Some people prefer mornings, while others find afternoon or evening walks easier. Consistency matters more than timing. Can Walking Reduce Stress? Yes, walking can help reduce stress and mental fatigue. It may also improve mood and support better sleep, especially when done regularly. Is 30 Minutes Of Walking A Day Enough? For many people, yes. Thirty minutes of walking a day is a practical and effective way to support heart health, fitness, and overall well-being. Is National Walking Day The Same As National Walk To Work Day? No. They are different observances, but both encourage you to add more walking to your daily life. References American Heart Association. National Walking Day. American Heart Association. American Heart Association. Move More Toolkit. American Heart Association. World Health Organization. Physical Activity. World Health Organization. Centers for Disease Control and Prevention. Benefits Of Physical Activity. CDC. NHS. Walking For Health. National Health Service.
Prevention of Blindness Week: Causes of Vision Loss and Tips to Protect Your Eye Health
Your eyesight supports almost every part of daily life. It helps you learn, work, travel, and care for the people around you. That is why Prevention of Blindness Week, observed from 1 to 7 April, is an important reminder to pay attention to your eye health. This awareness week encourages you to act early, not late. Many causes of vision loss can be prevented, treated, or managed better when they are picked up in time. Regular check-ups, healthy habits, and timely treatment can go a long way in protecting your sight. What Is Prevention of Blindness Week? Prevention of Blindness Week is observed in India every year to spread awareness about avoidable vision loss and the importance of timely eye care. It brings attention to common eye problems, encourages regular eye examinations, and promotes better understanding of how lifestyle, nutrition, and medical conditions can affect your vision. The week also supports community action. Free eye camps, awareness drives, educational activities, and conversations around early diagnosis all help people recognise that eye health should not be ignored. Prevention of Blindness Week Theme 2026 In 2026, the message strongly highlighted during this period is “Uniting for a Glaucoma-Free World.” This focus is important because glaucoma often develops slowly and may not cause clear symptoms in the early stages. It is often called the silent thief of sight because it can damage the optic nerve before you notice a problem. Once vision loss from glaucoma happens, it cannot usually be reversed. That is why awareness, screening, and timely treatment matter so much. Why Prevention of Blindness Week Matters Many people delay eye check-ups because they think they will notice if something is wrong. In reality, several serious eye conditions can progress quietly. Prevention of Blindness Week matters because it reminds you to take small but important steps before damage becomes severe. It encourages you to: Understand common causes of vision loss Recognise symptoms early Get regular eye check-ups Manage long-term conditions such as diabetes and high blood pressure Support eye health awareness in your family and community Common Causes of Vision Loss You Should Know Cataracts Cataracts happen when the natural lens of the eye becomes cloudy. This can make your vision blurry, dull, or hazy. Cataracts are common with ageing, but timely treatment can restore vision in many cases. Glaucoma Glaucoma is a group of eye diseases that damage the optic nerve. It often develops without warning signs in the early stages. If you are over 40, have diabetes, or have a family history of glaucoma, regular eye examinations become even more important. Refractive Errors Uncorrected refractive errors, such as short-sightedness, long-sightedness, and astigmatism, can interfere with daily life and learning. They are often easy to manage with proper correction, but many people continue without diagnosis or treatment. Diabetic Retinopathy High blood sugar can damage the small blood vessels in the retina. Over time, this may affect your vision. If you live with diabetes, regular monitoring is essential even when your sight seems normal. Vitamin A Deficiency Vitamin A Deficiency can harm the surface of the eye and affect night vision. In severe cases, it can lead to serious eye damage and blindness, especially in children. A balanced diet plays an important role in prevention. Age Related Eye Conditions As you grow older, your risk of cataracts, glaucoma, and other retinal conditions rises. This is why age appropriate screening is important even if you do not have obvious symptoms. Eye Injuries And Infections Trauma, unsafe work practices, sports injuries, poor contact lens hygiene, and untreated infections can all affect vision. Quick care can prevent complications. Optic Neuritis Optic Neuritis is inflammation of the optic nerve. It may cause sudden blurred vision, reduced colour vision, or pain when moving the eye. Unlike common eye strain, Optic Neuritis needs prompt medical attention. Who May Be At Higher Risk Of Vision Loss? You may need closer attention to eye health if you: Are over 40 Have diabetes or high blood pressure Smoke Have a family history of glaucoma or other eye disease Spend long hours on screens without breaks Work in environments with dust, chemicals, or flying particles Have poor nutrition or risk factors for vitamin A deficiency Notice sudden pain, blur, or colour vision changes that could suggest Optic Neuritis Early Signs of Eye Problems You Should Not Ignore Please do not ignore symptoms such as: Blurred or dim vision Trouble seeing at night Frequent headaches linked to vision Eye pain or pressure Halos around lights Sudden redness or watering Sudden loss of vision Pain on eye movement Reduced colour vision Some of these signs may point to glaucoma, retinal disease, infection, or Optic Neuritis. Early medical advice can help protect your sight. Statistics On Vision Loss And Preventable Blindness The World Health Organization states that at least 2.2 billion people worldwide live with near or distance vision impairment. At least 1 billion of these cases could have been prevented or have not yet been addressed. WHO identifies unoperated cataract and uncorrected refractive error as the two main global causes of vision impairment. In India, a nationally representative survey in adults aged 50 years and above found cataract to be the leading cause of blindness, while untreated cataract and uncorrected refractive errors were major contributors to visual impairment. Tips To Protect Your Eye Health Get Regular Eye Examinations Do not wait for symptoms. Routine check-ups can detect glaucoma, cataracts, and retinal problems early. Control Diabetes And Blood Pressure Good control of chronic conditions can lower your risk of retinal damage and other complications. Eat A Balanced Diet Include leafy greens, colourful vegetables, fruits, nuts, and other nutrient-rich foods. This helps reduce the risk of nutritional problems such as vitamin A deficiency. Protect Your Eyes From UV Exposure Choose sunglasses that block 99 to 100 per cent of UVA and UVB rays. Follow Healthy Screen Habits Use the 20 20 20 rule. Every 20 minutes, look at something about 20 feet away for 20 seconds. Avoid Smoking Smoking increases the risk of several eye diseases and can worsen overall health. Use Protective Eyewear Wear safety glasses or goggles during sports, home repairs, and high risk work. Seek Help Early If your vision changes suddenly, do not delay evaluation. Eye Care Tips For Children And Adults For Children Children may not always say that they cannot see clearly. Instead, you may notice squinting, sitting too close to screens, poor concentration, or frequent eye rubbing. Regular vision checks can support learning and development. A healthy diet also matters. Preventing vitamin A deficiency in childhood is an important part of protecting long term eye health. For Adults And Older Adults As an adult, especially after 40, you should not skip routine eye examinations. Conditions such as glaucoma and diabetic retinopathy may begin without obvious symptoms. If you have diabetes, high blood pressure, or a family history of eye disease, you may need more regular follow-up. How Early Detection And Screening Help Prevent Blindness Early detection can make a real difference because: Some eye diseases begin silently Treatment is usually more effective when started early Screening can identify risk before vision is seriously affected Follow-up care helps prevent avoidable progression Community eye camps and awareness drives can improve access to timely checks Screening is not just for older adults. Children, people with chronic illness, and anyone with symptoms can benefit from timely assessment. How Lifestyle Choices Affect Your Eye Health Your daily choices can either support or strain your eyes. Smoking can raise the risk of serious eye disease. Poor nutrition can increase the risk of vitamin A deficiency and other health issues that affect the eyes. Long hours of screen use without breaks may worsen eye strain and dryness. Uncontrolled diabetes and high blood pressure can damage the retina over time. Lack of sun protection may also increase harm to your eyes. Small habits matter. Better food choices, regular movement, good sleep, screen breaks, and routine health monitoring all support healthier vision. Common Eye Health Myths You Should Stop Believing Myth: If you can see well, you do not need an eye test. Fact: Some serious conditions, including glaucoma, may not cause early symptoms. Myth: Only older adults get eye disease. Fact: Children and younger adults can also develop vision problems, injuries, infections, and inflammatory conditions. Myth: Screens cause blindness. Fact: Screens mainly contribute to strain and dryness, but unhealthy screen habits should still be corrected. Myth: Eye problems always come with pain. Fact: Many important eye conditions can be painless in the beginning. Myth: Wearing glasses makes your eyes weaker. Fact: Glasses correct your vision. They do not weaken your eyes. Awareness Campaigns And Community Support Local Awareness Efforts Local campaigns during Prevention of Blindness Week often include free eye screening camps, school awareness sessions, educational talks, and community outreach. These efforts can help people who may otherwise delay care. Corneal donation awareness and public education also play an important role in improving understanding and support. Global Eye Health Efforts Across the world, public health campaigns continue to focus on avoidable blindness, regular screening, early diagnosis, and access to treatment. Global awareness efforts around glaucoma have also strengthened the message that protecting sight requires action at both individual and community level. When Should You Book An Eye Check-Up? You should plan an eye check-up if: You are over 40 You have diabetes or high blood pressure You have a family history of glaucoma You notice blurred vision, eye pain, or sudden changes Your child shows signs of poor vision You have symptoms such as pain with eye movement or reduced colour vision You have been told you may be at risk of Optic Neuritis or another optic nerve problem Conclusion Prevention of Blindness Week is a timely reminder that caring for your eyes should be part of your overall health routine. Not every cause of blindness can be prevented, but many causes of vision loss can be reduced, detected early, or treated better with awareness and timely medical care. If you are living with diabetes, high blood pressure, or other long-term health concerns, routine testing and preventive health checks can support earlier risk detection. Metropolis Healthcare helps you take that preventive step with 4,000+ tests, full body checkups, speciality testing, accurate results, quick turnaround time, and convenient home sample collection backed by a strong network of 10,000+ touchpoints. You can book easily through the website, app, call, or WhatsApp. Frequently Asked Questions How Can You Protect Your Eyes From Vision Loss? Protecting your eyes starts with regular eye examinations, good diabetes and blood pressure control, a balanced diet, UV protection, healthy screen habits, and early treatment when symptoms appear. Is Blindness Preventable? Not every type of blindness is preventable. However, many causes of vision loss can be prevented, treated, or managed more effectively when detected early. What Is The Theme For Prevention Of Blindness Week 2026? The theme widely highlighted in 2026 is “Uniting for a Glaucoma-Free World.” It places strong focus on glaucoma awareness, early diagnosis, and timely screening. Why Is Glaucoma Called The Silent Thief Of Sight? Glaucoma is called the silent thief of sight because it can damage the optic nerve slowly and quietly, often before you notice symptoms. Who Should Get Regular Eye Check-Ups? Children, adults over 40, people with diabetes or high blood pressure, smokers, and anyone with a family history of eye disease should prioritise regular eye check-ups. References World Health Organization. Blindness and vision impairment. Fact sheet. Updated 10 February 2026. Vashist P, Senjam SS, Gupta V, Gupta N, Shamanna BR, Wadhwani M, Shukla P, Manna S, Yadav S, Bharadwaj A. Blindness and visual impairment and their causes in India: Results of a nationally representative survey. PLoS One. 2022;17(7):e0271736. PMID: 35862402. National Eye Institute. Glaucoma. Updated 26 November 2025. World Glaucoma Week. Uniting for a Glaucoma-Free World. 2026 campaign theme. World Health Organization. Vitamin A deficiency. Nutrition Landscape Information System. Hoorbakht H, Bagherkashi F. Optic neuritis, its differential diagnosis and management. Open Ophthalmol J. 2012;6:65-72. PMID: 22888383. National Eye Institute. Keep Your Eyes Healthy. Updated 11 September 2025. American Academy of Ophthalmology. How to Choose the Best Sunglasses to Avoid Sun Damage. Updated 29 May 2024.