Preventive Healthcare
Periampullary Carcinoma: Symptoms, Diagnosis And Treatment
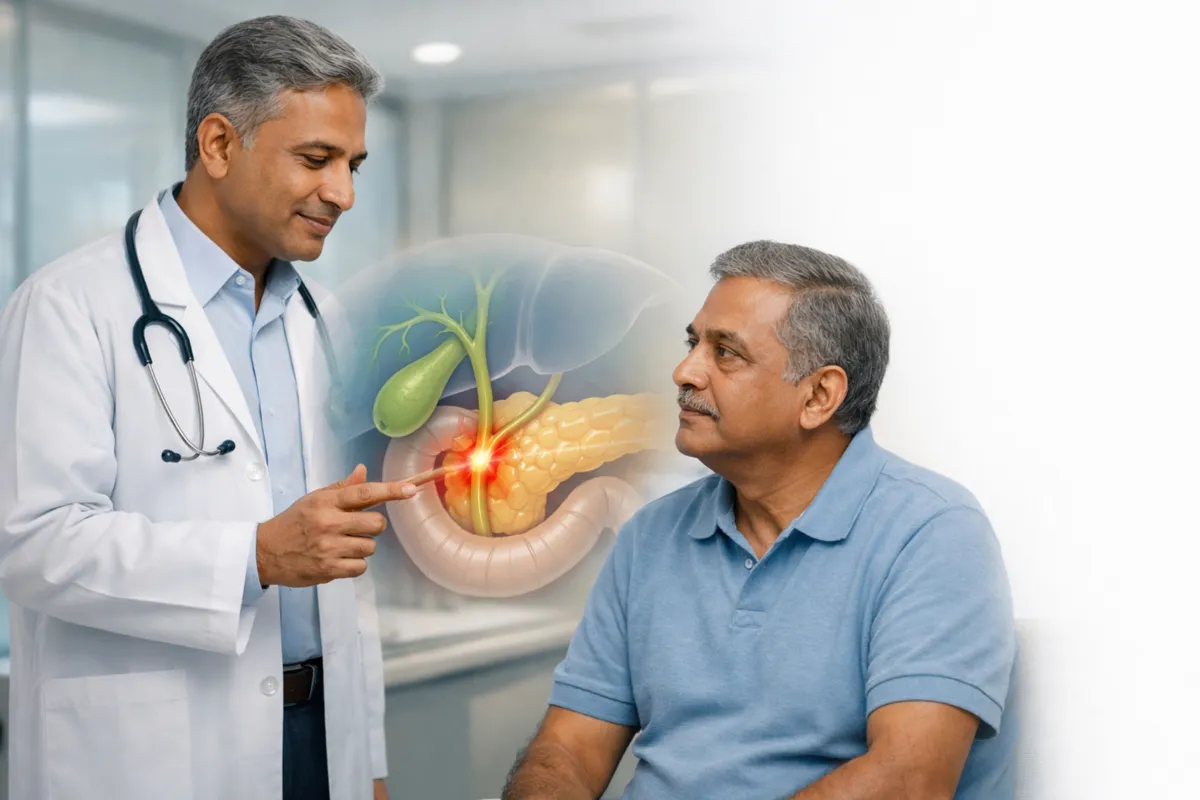
Table of Contents
- What Is Periampullary Carcinoma?
- Where Does Periampullary Carcinoma Occur?
- Types Of Periampullary Carcinoma
- Causes And Risk Factors
- Genetic And Familial Risk Factors
- Lifestyle And Medical Risk Factors
- Symptoms Of Periampullary Carcinoma
- Why Jaundice Is A Key Warning Sign
- How Periampullary Carcinoma Is Diagnosed
- Blood Tests And Tumour Markers
- Imaging Tests (CT, MRI, MRCP)
- Endoscopy And Biopsy
- Staging Of Periampullary Carcinoma
- Treatment Options For Periampullary Carcinoma
- Surgery For Periampullary Carcinoma
- Whipple Procedure (Pancreaticoduodenectomy)
- Chemotherapy And Radiotherapy
- Treatment Based On Cancer Stage
- Prognosis And Survival Rates
- Factors Affecting Prognosis
- Complications Of Periampullary Carcinoma
- Living With Periampullary Carcinoma
- Follow-Up And Monitoring After Treatment
- When To See A Doctor
- Conclusion
- FAQ’s
- References
What Is Periampullary Carcinoma?
Periampullary carcinoma is a term used for cancers that arise in a small, crowded area where the bile duct and pancreatic duct meet and drain into the first part of the small intestine. Because several organs connect at this junction, tumours can start in slightly different places but cause similar symptoms, especially jaundice.
Periampullary carcinoma is not one single disease. It is a group of cancers that behave differently depending on their exact origin and their “type” under the microscope. Your care plan is usually personalised once the origin and stage are clear.
Where Does Periampullary Carcinoma Occur?
The periampullary region surrounds the ampulla of Vater, which is the opening where bile (from the liver) and digestive enzymes (from the pancreas) enter the duodenum (the first part of the small intestine).
This location matters because:
- A small tumour can block bile flow early, leading to jaundice.
- The region sits close to major blood vessels and the pancreas, which affects surgery planning.
- Symptoms from different tumours in this area can look similar, so careful testing is needed to identify the source.
Types Of Periampullary Carcinoma
Doctors often group periampullary cancers based on where they start:
- Ampullary cancer: Begins in the ampulla itself.
- Pancreatic head cancer: Starts in the head of the pancreas but can present like a periampullary tumour.
- Distal bile duct cancer: Begins in the lower end of the bile duct.
- Duodenal cancer: Starts in the duodenum close to the ampulla.
There is also another important layer: some tumours have an “intestinal” type pattern under the microscope, while others look “pancreatobiliary” (more like pancreatic or bile duct tissue). This distinction can influence prognosis and, in some cases, treatment choices.
Causes And Risk Factors
In many people, no single clear cause is found. Most cancers develop due to a combination of age-related changes, genetics, and environmental exposures.
Genetic And Familial Risk Factors
Some inherited conditions can increase the risk of growths (polyps) and cancers around the ampulla and duodenum. These may include syndromes such as familial adenomatous polyposis (FAP) and certain hereditary bowel cancer syndromes.
If you have a strong family history of bowel polyps, bowel cancer, or rare gastrointestinal cancers, tell your doctor. You may need earlier evaluation or surveillance.
Lifestyle And Medical Risk Factors
Depending on the tumour origin, risk factors can overlap with pancreatic and bile duct conditions. Your doctor may discuss factors such as:
- Smoking
- Long-term inflammation of the pancreas (chronic pancreatitis)
- Long-standing diabetes in some cases
- Certain bile duct and liver conditions
Having a risk factor does not mean you will develop cancer. It simply helps your doctor decide how closely to evaluate symptoms and test results.
Symptoms Of Periampullary Carcinoma
Symptoms often happen when the tumour blocks bile flow or irritates nearby structures. Many of these symptoms can also occur with non-cancerous conditions, which is why proper diagnosis matters.
Common symptoms include:
- Yellowing of the skin or eyes (jaundice)
- Itching (often linked to bile buildup)
- Dark urine and pale stools
- Upper abdominal discomfort or back pain
- Loss of appetite, nausea, or vomiting
- Unexplained weight loss
- Fever in some cases (especially if infection develops in blocked bile ducts)
It is also worth noting that some early signs can overlap with pancreatic cancer symptoms, which is why doctors treat persistent jaundice and unexplained weight loss seriously.
Why Jaundice Is A Key Warning Sign
Jaundice is one of the most important early clues because periampullary tumours can block the bile duct before they become large. This often leads to:
- Raised bilirubin (a blood marker linked to jaundice)
- Raised liver enzymes linked to bile obstruction (such as ALP and GGT)
- Symptoms like itch, dark urine, and pale stools
If jaundice appears suddenly or is worsening, you should seek medical advice promptly.
How Periampullary Carcinoma Is Diagnosed
Diagnosis usually happens step-by-step. Your doctor combines symptoms, blood tests, imaging, and endoscopic tests to confirm what is happening and whether the tumour can be removed safely.
Blood Tests And Tumour Markers
Blood tests help assess bile blockage, inflammation, nutrition, and suitability for procedures. Common tests include:
- Liver function tests (including bilirubin, ALP, and GGT)
- Complete blood count (to check anaemia or signs of infection)
- Kidney function and electrolytes (important before scans and treatments)
- Clotting profile (bile obstruction can affect vitamin K absorption)
- Tumour markers such as CA19-9 and sometimes CEA
Tumour markers can support the overall picture, but they cannot confirm cancer on their own. CA19-9, for example, may rise with bile duct blockage from non-cancer causes as well, so results must be interpreted carefully.
Imaging Tests (CT, MRI, MRCP)
Imaging helps locate the tumour, look for spread, and assess whether surgery is possible.
Common scans include:
- Contrast CT scan (pancreas protocol): Often the first detailed scan for staging and surgical planning.
- MRI: Helpful for soft tissue detail.
- MRCP: A special MRI technique that maps the bile and pancreatic ducts and helps clarify the level of blockage.
Your doctor may also use imaging to check for liver involvement, lymph nodes, or blood vessel contact.
Endoscopy And Biopsy
Endoscopic tests allow doctors to look directly at the region and take tissue samples.
You may be advised:
- Endoscopic ultrasound (EUS): Uses an ultrasound probe on an endoscope to assess tumour depth and nearby lymph nodes, and to guide fine-needle sampling when appropriate.
- ERCP: Can visualise the bile duct opening, take samples, and sometimes place a stent to relieve jaundice.
A biopsy can confirm the diagnosis, but sometimes sampling can miss deeper cancer cells. If suspicion remains high, your care team may recommend additional sampling or proceed based on combined findings.
Staging Of Periampullary Carcinoma
Staging describes how far the cancer has grown and spread. It usually considers:
- Tumour size and invasion into nearby structures
- Lymph node involvement
- Spread to distant organs (such as the liver or lining of the abdomen)
Staging is essential because it determines whether surgery is an option and what additional treatments may help.
Treatment Options For Periampullary Carcinoma
Treatment depends on the tumour origin, stage, and your overall fitness. Care is usually coordinated across specialists (surgery, oncology, gastroenterology, and nutrition support).
Surgery For Periampullary Carcinoma
If the tumour is considered resectable (removable) and you are fit for surgery, surgery offers the best chance of long-term control.
Surgery is a major decision. Your team will assess:
- Whether the tumour involves major blood vessels
- Whether there are signs of distant spread
- Your nutrition, strength, and other health conditions
Whipple Procedure (Pancreaticoduodenectomy)
The most common operation for cancers in this region is the Whipple procedure (pancreaticoduodenectomy). It usually involves removing:
- The head of the pancreas
- The duodenum
- The gallbladder and part of the bile duct
- Sometimes part of the stomach (depending on the approach)
The digestive tract is then reconstructed to allow food, bile, and pancreatic enzymes to flow again.
Recovery can take time. Many people need nutritional support, careful monitoring of blood sugar, and sometimes pancreatic enzyme supplements.
Chemotherapy And Radiotherapy
Chemotherapy may be recommended:
- After surgery (adjuvant therapy) to reduce recurrence risk
- Before surgery in selected cases
- When surgery is not possible, to control disease and symptoms
Radiotherapy is used in some situations, but its role varies depending on tumour type and clinical context.
Your doctor may also consider tumour subtype (intestinal versus pancreatobiliary) when discussing systemic treatment options.
Treatment Based On Cancer Stage
In practical terms, treatment often follows these paths:
- Early and resectable disease: Surgery, often followed by chemotherapy depending on risk factors.
- Locally advanced disease: Systemic therapy first, then reassessment for surgery if the tumour shrinks or stabilises.
- Advanced or metastatic disease: Chemotherapy and supportive care focused on symptom control, nutrition, and quality of life.
Prognosis And Survival Rates
Prognosis varies widely because periampullary carcinoma includes several different cancers. In general, outcomes tend to be more favourable for true ampullary and some duodenal cancers than for pancreatic ductal adenocarcinoma, but the stage at diagnosis is critical for every type.
Factors Affecting Prognosis
Key factors your doctor may discuss include:
- Tumour origin and histological subtype
- Lymph node involvement
- Whether the tumour was fully removed with clear margins
- Response to systemic treatment when used
- Your overall fitness and nutritional status
Complications Of Periampullary Carcinoma
Possible complications can arise from bile blockage, poor digestion, or treatment side effects. These may include:
- Cholangitis (infection in the bile ducts)
- Pancreatitis
- Malabsorption and weight loss
- Vitamin deficiencies due to reduced bile flow
- Post-surgical issues such as delayed stomach emptying or pancreatic leaks
If you develop fever, worsening jaundice, confusion, severe weakness, or uncontrolled vomiting, contact your doctor urgently.
Living With Periampullary Carcinoma
Living with this condition often involves balancing treatment with day-to-day wellbeing. Helpful supports may include:
- Dietitian-led nutrition planning to maintain weight and strength
- Symptom control for itch, nausea, and pain
- Gradual return to activity after treatment
- Emotional support for you and your family
If you are trying to make sense of abdominal pain causes, it is best to avoid self-diagnosis and share a clear symptom timeline with your doctor. Even small details can help guide the right tests.
Follow-Up And Monitoring After Treatment
Follow-up plans vary, but commonly include:
- Regular clinical review of symptoms and weight
- Blood tests to monitor liver function and overall health
- Tumour marker monitoring in selected cases
- Imaging scans at intervals advised by your specialist team
Follow-up is also a time to address fatigue, digestion changes, appetite issues, and emotional health.
When To See A Doctor
Seek medical advice if you notice:
- New jaundice or worsening yellowing of the eyes or skin
- Persistent itching with dark urine or pale stools
- Unexplained weight loss
- Ongoing upper abdominal pain or pain that radiates to the back
- Fever with chills, especially if you are jaundiced
- Symptoms that persist or worsen despite basic care
Prompt assessment does not mean the cause is cancer. It means you are giving yourself the best chance of an early and accurate diagnosis.
Conclusion
Periampullary carcinoma is a group of cancers near the junction of the bile duct and pancreatic duct. Because this area can block bile flow early, symptoms such as jaundice often appear sooner than many people expect. Diagnosis usually involves blood tests, imaging, and endoscopic evaluation, followed by a treatment plan tailored to tumour type and stage.
If your doctor has advised testing, you can simplify the process with Metropolis Healthcare. With 4,000 plus tests, expert pathology oversight, and convenient booking through the website, app, call, or WhatsApp, you can access reliable testing with options such as home sample collection across 10,000 touchpoints. This can be especially helpful when you need timely blood work such as liver function tests and tumour marker evaluation as part of your care journey.
FAQ’s
Is Periampullary Carcinoma Curable?
It can be curable in some people, particularly when diagnosed early and treated with complete surgical removal. Your personal outlook depends on tumour type, stage, and surgical findings.
How Is Periampullary Cancer Different From Pancreatic Cancer?
Periampullary cancer refers to cancers arising around the ampulla of Vater, including tumours from the bile duct, duodenum, ampulla, and pancreatic head. Some periampullary tumours have a better prognosis than pancreatic ductal adenocarcinoma, but accurate classification is essential.
What Is The Survival Rate Of Periampullary Carcinoma?
Survival varies widely. It depends on the exact tumour origin, stage, lymph node involvement, and whether complete removal is possible. Your specialist team is best placed to discuss realistic expectations for your specific diagnosis.
Is Surgery Always Required?
Surgery is the main curative option for resectable disease. If the tumour is not resectable or has spread, treatment usually focuses on chemotherapy, symptom control, and supportive care. Some people may receive systemic therapy first and be reassessed for surgery later.
What Tests Confirm Periampullary Carcinoma?
Confirmation typically requires a combination of imaging (CT, MRI, MRCP), endoscopic tests (EUS and or ERCP), and tissue diagnosis through biopsy or fine-needle sampling. Blood tests support diagnosis and guide safe treatment but do not confirm cancer alone.
References
- Walter D, Schnitzbauer AA, Schulze F, Trojan J. The diagnosis and treatment of ampullary carcinoma. Dtsch Arztebl Int. 2023;120(43):729-735. PMID: 37656482.
- Regalla DKR, Jacob R, Manne A, Paluri RK. Therapeutic options for ampullary carcinomas. A review. Oncol Rev. 2019;13(2):440. PMID: 31565197.
- Williams JL, Chan CK, Toste PA, Elliott IA, Vasquez CR, Sunjaya DB, et al. Association of histopathologic phenotype of periampullary adenocarcinomas with survival. JAMA Surg. 2017;152(1):82-88. PMID: 27732711.
- Chandrasegaram MD, Gill AJ, Samra J, Price T, Chen J, Fawcett J, et al. Ampullary cancer of intestinal origin and duodenal cancer - a logical clinical and therapeutic subgroup in periampullary cancer. World J Gastrointest Oncol. 2017;9(10):407-415. PMID: 29085567.
- Singh S, Tang SJ, Sreenarasimhaiah J, Lara LF, Siddiqui A. The clinical utility and limitations of serum carbohydrate antigen (CA19-9) as a diagnostic tool for pancreatic cancer and cholangiocarcinoma. Dig Dis Sci. 2011;56(8):2491-2496. PMID: 21516323.
- Verma A, Shukla S, Verma N. Diagnosis, preoperative evaluation, and assessment of resectability of pancreatic and periampullary cancer. Indian J Surg. 2015;77(5):362-370. PMID: 26722198.
- Andersson M, Kostic S, Johansson M, Lundell L, Asztély M, Hellström M. MRI combined with MR cholangiopancreatography versus helical CT in the evaluation of patients with suspected periampullary tumors: a prospective comparative study. Acta Radiol. 2005;46(1):16-27. PMID: 15841735.
- Rösch T, Braig C, Gain T, Feuerbach S, Siewert JR, Schusdziarra V, et al. Staging of pancreatic and ampullary carcinoma by endoscopic ultrasonography. Comparison with conventional sonography, computed tomography, and angiography. Gastroenterology. 1992;102(1):188-199. PMID: 1727753.
- van der Gaag NA, Rauws EAJ, van Eijck CHJ, Bruno MJ, van der Harst E, Kubben FJGM, et al. Preoperative biliary drainage for cancer of the head of the pancreas. N Engl J Med. 2010;362(2):129-137. PMID: 20071702.
- Johnson JC, DiSario JA, Grady WM. Surveillance and treatment of periampullary and duodenal adenomas in familial adenomatous polyposis. Curr Treat Options Gastroenterol. 2004;7(2):79-89. PMID: 15010021.