Preventive Healthcare
Lymphatic System: How It Works And Key Disorders
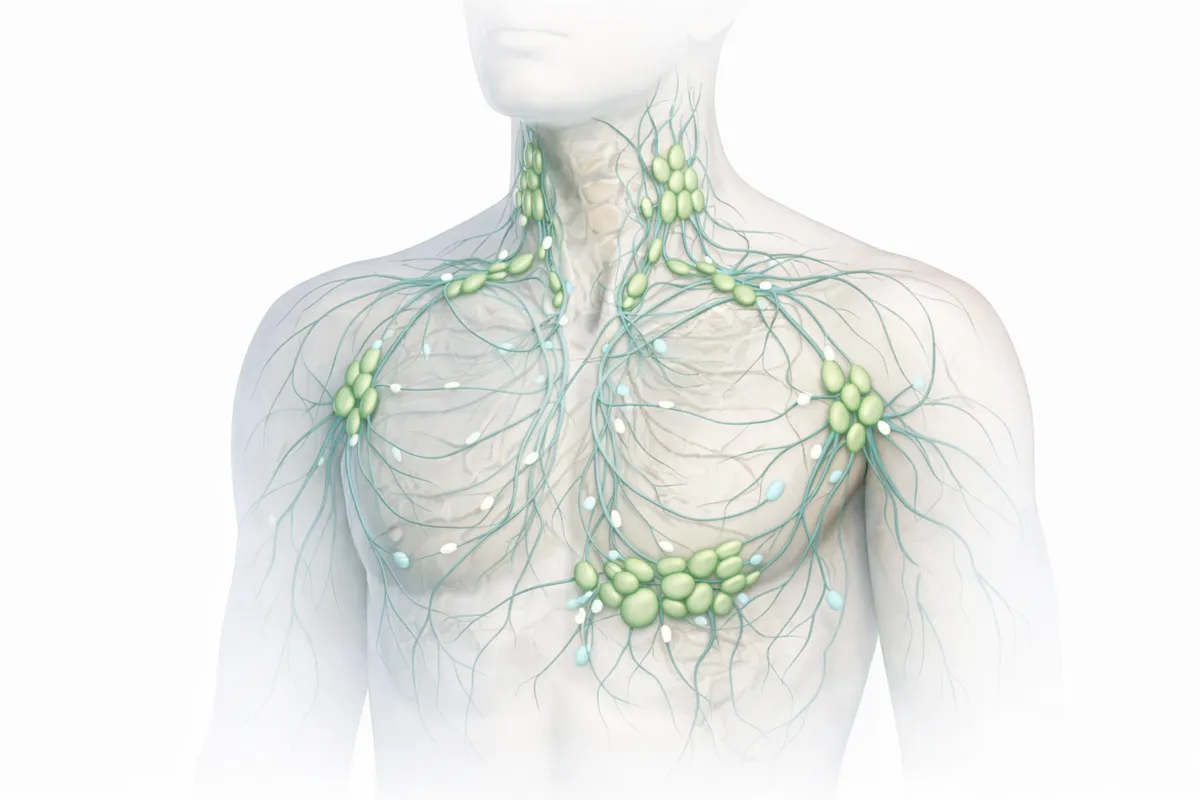
Table of Contents
- What Is The Lymphatic System?
- What Does The Lymphatic System Do?
- Parts Of The Lymphatic System
- How The Lymphatic System Works
- Lymphatic System And Immunity
- Lymphatic System And Fluid Balance
- Common Symptoms Of Lymphatic System Problems
- Key Disorders Of The Lymphatic System
- Causes And Risk Factors
- How Lymphatic Disorders Are Diagnosed
- Blood Tests And Imaging
- Biopsy And Specialised Tests
- Treatment Options For Lymphatic Disorders
- Medical Treatment
- Compression And Physical Therapy
- Surgical Treatment
- How To Keep The Lymphatic System Healthy
- When To See A Doctor
- Conclusion
- FAQ’s
- References
Your lymphatic system quietly supports you every day. It helps keep fluid levels balanced, carries infection-fighting cells, and removes waste from tissues. You usually notice it only when something changes, such as swollen glands in your neck during a cold. Understanding how this system works can help you recognise what is normal, what is not, and when you should seek medical advice.
What Is The Lymphatic System?
The lymphatic system is a network of tiny vessels, larger ducts, lymph nodes, and specialised organs. It collects extra fluid from your tissues, filters it, and returns it to your bloodstream. Along the way, it supports your immune system by moving and organising white blood cells that protect you from infections.
What Does The Lymphatic System Do?
Your lymphatic system has three core roles:
- Maintaining fluid balance: It drains excess fluid and proteins that leak out of blood vessels into your tissues, helping prevent persistent swelling.
- Supporting immunity: It transports immune cells and helps your body identify and respond to germs.
- Helping fat absorption: In your small intestine, specialised lymph vessels absorb dietary fats and fat-soluble vitamins and transport them into circulation.
Parts Of The Lymphatic System
The lymphatic system includes:
- Lymph: A clear fluid formed from the extra fluid in your tissues. It can contain proteins, fats, immune cells, and cellular waste.
- Lymphatic vessels: Thin tubes that carry lymph in one direction, using valves and muscle movement to keep it flowing.
- Lymph nodes: Small, bean-shaped filters located in areas like your neck, armpits, chest, abdomen, and groin. They help trap germs and support immune responses.
- Key lymphatic organs:
How The Lymphatic System Works
Think of your blood vessels as a delivery network that brings oxygen and nutrients to tissues. Some fluid naturally leaks into the space around cells as part of this process. Your lymphatic system collects that extra fluid, now called lymph, and moves it back toward large veins near your collarbones.
This movement is supported by:
- One-way valves inside lymph vessels
- The squeezing action of nearby muscles during normal movement
- Pressure changes in your chest when you breathe
Because lymph flow relies on movement and valve function, prolonged inactivity or damage to lymph vessels can contribute to swelling.
Lymphatic System And Immunity
Your lymph nodes act as meeting points for immune cells. When germs, damaged cells, or unusual proteins are carried in lymph, lymph nodes help your immune system “decide” what to do next. This is why lymph nodes may swell during common infections. It is often a sign that your immune system is doing its job.
Lymphatic System And Fluid Balance
If lymph drainage slows or becomes blocked, fluid can build up in tissues. This can cause swelling that may feel heavy, tight, or uncomfortable. When this swelling is persistent, it may be called lymphedema. Early assessment matters because long-standing swelling can affect skin health and raise the risk of repeated infections.
Common Symptoms Of Lymphatic System Problems
Symptoms depend on the underlying cause, but common signs include:
- Swollen lymph nodes that persist, enlarge, or feel unusual
- Unexplained swelling in an arm, leg, or part of the face or trunk
- A feeling of heaviness or tightness in a limb
- Skin changes over a swollen area, such as thickening, dryness, or recurrent irritation
- Repeated skin infections in the same area
- Unexplained fever, night sweats, or weight loss, especially when combined with lymph node swelling
Many of these symptoms can also occur in non-lymphatic conditions. That is why you should treat them as a reason to check in with a clinician, rather than a reason to panic.
Key Disorders Of The Lymphatic System
Lymphedema
Lymphedema is long-term swelling caused by reduced lymph drainage. It can occur after surgery or radiotherapy that affects lymph nodes, after injury, or sometimes due to inherited lymph vessel differences. It often affects arms or legs, but it can happen elsewhere too.
Lymphadenopathy
This means enlarged lymph nodes. It is commonly linked to infections, inflammation, or immune responses. In many cases, nodes settle as you recover. Persistent, enlarging, or hard nodes need evaluation.
Lymphangitis
This is inflammation of lymph vessels, sometimes seen as tender, red streaks on the skin. It can occur with bacterial skin infections and needs prompt medical care.
Lymphoma
Lymphoma is a cancer of lymphocytes, a type of white blood cell. There are multiple subtypes. A single phrase you may come across is Lymphoma Cancer, and it generally refers to cancers that start in the lymphatic system. If lymphoma is suspected, diagnosis depends on clinical assessment and specialised tests.
Lymphatic Filariasis
This parasitic infection can damage lymph drainage and cause significant swelling in some cases. It is more common in certain tropical regions and is managed with targeted public health measures and medical treatment.
Causes And Risk Factors
You may be at higher risk of lymphatic disorders if you have:
- Recent or repeated infections
- Skin injuries, especially when not healing well
- Surgery or radiotherapy involving lymph nodes
- Chronic inflammatory conditions
- Reduced immunity due to illness or certain medicines
- Obesity, which can strain lymph flow
- Prolonged immobility
- A family history of primary lymphedema
Risk factors do not mean you will develop a problem. They simply help a clinician decide what to check and how urgently.
How Lymphatic Disorders Are Diagnosed
Diagnosis usually starts with your symptoms, medical history, and a physical examination. Your clinician may then recommend tests to identify infection, inflammation, immune conditions, or abnormal cells.
Blood Tests And Imaging
Blood tests can support diagnosis by showing signs of infection, inflammation, or blood-related disorders. For example, your doctor may recommend a cbc test to evaluate white blood cell patterns, anaemia, or other clues that guide next steps.
Other tests may include inflammatory markers, liver and kidney tests, and specific infection-related tests depending on your symptoms.
Imaging can help assess lymph nodes or swelling, and may include ultrasound, CT, MRI, or other scans depending on the clinical question.
Biopsy And Specialised Tests
If lymph nodes remain enlarged without a clear explanation, a biopsy may be recommended. This may be done using a needle sample or by removing a lymph node for detailed analysis. Specialised testing can help identify lymphoma subtypes or other less common conditions.
For suspected lymphedema, clinicians may also use specialised imaging to assess lymph flow, depending on availability and clinical need.
Treatment Options For Lymphatic Disorders
Treatment depends on the cause and severity. Many lymphatic issues are manageable, especially with early evaluation.
Medical Treatment
Medical treatment may include:
- Antibiotics for bacterial infections
- Anti-inflammatory or immune-modulating medicines for inflammatory or autoimmune causes
- Targeted therapy, chemotherapy, or radiotherapy when cancer is diagnosed
- Supportive care to reduce symptoms while investigations continue
Always take prescribed medicines exactly as directed, even if you start feeling better.
Compression And Physical Therapy
For lymphedema, the goal is to reduce swelling and protect your skin. Your care plan may include:
- Compression garments or bandaging
- Manual lymphatic drainage performed by trained professionals
- Exercise plans that support lymph flow
- Skin care routines to reduce infection risk
These measures often improve comfort, mobility, and long-term outcomes.
Surgical Treatment
Surgery is not needed for most people, but it may be considered in selected cases, such as:
- Lymphatic reconstruction procedures in specialist centres
- Removal of excess tissue in advanced lymphedema
- Surgery for underlying causes that are blocking lymph drainage
Your clinician will guide you on whether surgery is appropriate for your situation.
How To Keep The Lymphatic System Healthy
There is no single “lymph detox” shortcut. The most reliable support comes from simple habits:
- Stay active: Walking, stretching, and gentle strength training can help lymph flow.
- Stay hydrated: Fluids support healthy circulation and lymph movement.
- Protect your skin: Clean minor cuts and keep skin moisturised to reduce cracking and infection risk.
- Maintain a healthy weight: This can reduce strain on lymph drainage.
- Avoid smoking and limit alcohol: These support overall immune and vascular health.
- Manage long-term conditions well: Diabetes and vascular conditions can affect healing and infection risk.
If you already have swelling, avoid self-treatment that could irritate the skin. It is safer to get personalised advice.
When To See A Doctor
Seek medical advice if you notice:
- Swollen lymph nodes that last more than two to three weeks
- Lymph nodes that are rapidly enlarging, very hard, or fixed in place
- Unexplained swelling in a limb, especially if it is worsening
- Fever, night sweats, unexplained weight loss, or ongoing fatigue
- Red, painful streaks on the skin, or signs of skin infection
- Swelling with shortness of breath, chest pain, or severe unwellness
If you feel worried, it is reasonable to get checked. Most causes are treatable, and early assessment often brings reassurance.
Conclusion
Your lymphatic system supports fluid balance, immunity, and fat absorption, often without you noticing. When symptoms appear, they can range from minor and temporary to signs that need prompt evaluation. The most helpful step is to focus on evidence-based care: monitor changes, protect your skin, and seek medical advice when symptoms persist.
If your clinician recommends diagnostic testing, Metropolis Healthcare can support you with a wide range of pathology services, including 4,000+ tests and preventive health checkups. With NABL and CAP-accredited labs, expert pathologists, and convenient home sample collection across 10,000+ touchpoints, you can access accurate reports with a quick turnaround. Booking is simple through the website, app, call, or WhatsApp. You can also explore more Metropolis articles to stay informed and confident about your health.
FAQ’s
What Is The Main Function Of The Lymphatic System?
Its main function is to maintain healthy fluid balance by draining excess tissue fluid back into your bloodstream. It also supports immunity and helps absorb dietary fats.
What Are The Five Diseases Of The Lymphatic System?
Common examples include lymphedema, lymphadenopathy, lymphangitis, lymphoma, and lymphatic filariasis. The exact condition that matters to you depends on your symptoms and clinical assessment.
Is Lymphatic System Disease Serious?
Some lymphatic problems are mild and temporary, such as lymph node swelling during a viral infection. Others can be more serious, especially persistent swelling, recurrent infections, or suspected cancer. A clinician can help you understand the cause and level of concern.
How Do I Tell If My Lymphatic System Is Clogged?
There is no single symptom that confirms it. Persistent swelling, heaviness, tightness, or recurrent skin infections in the same area can suggest reduced lymph drainage. Proper diagnosis requires clinical evaluation.
Can Lymphatic Disorders Be Cured?
Some causes, such as infections, can resolve fully with treatment. Others, such as lymphedema, are usually managed rather than cured, with measures that reduce swelling and protect your skin and mobility.
References
- Ozdowski L., Gupta V. (2025). Physiology, Lymphatic System. StatPearls [Internet]. PMID: 32491765
- Liao S., von der Weid P. Y. (2015). Lymphatic System: An Active Pathway For Immune Protection. Seminars In Cell And Developmental Biology, 38, 83-89. PMID: 25534659
- Liao S., Padera T. P. (2013). Lymphatic Function And Immune Regulation In Health And Disease. Lymphatic Research And Biology, 11(3), 136-143. PMID: 24024577
- Willard-Mack C. L. (2006). Normal Structure, Function, And Histology Of Lymph Nodes. Toxicologic Pathology, 34(5), 409-424. PMID: 17067937
- Dixon J. B. (2010). Mechanisms Of Chylomicron Uptake Into Lacteals. Annals Of The New York Academy Of Sciences, 1207(Suppl 1), E52-E57. PMID: 20961306
- Rockson S. G. (2001). Lymphedema. The American Journal Of Medicine, 110(4), 288-295. PMID: 11239847
- Warren A. G., Brorson H., Borud L. J., Slavin S. A. (2007). Lymphedema: A Comprehensive Review. Annals Of Plastic Surgery, 59(4), 464-472. PMID: 17901744
- Gaddey H. L., Riegel A. M. (2016). Unexplained Lymphadenopathy: Evaluation And Differential Diagnosis. American Family Physician, 94(11), 896-903. PMID: 27929264
- Ansell S. M. (2015). Hodgkin Lymphoma: Diagnosis And Treatment. Mayo Clinic Proceedings, 90(11), 1574-1583. PMID: 26541251
- Medeiros Z. M., Vieira A. V. B., Xavier A. T., Bezerra G. S. N., Lopes M. F. C., Bonfim C. V., Aguiar-Santos A. M. (2021). Lymphatic Filariasis: A Systematic Review On Morbidity And Its Repercussions In Countries In The Americas. International Journal Of Environmental Research And Public Health, 19(1), 316. PMID: 35010576