Preventive Healthcare
Oropharynx: Anatomy, Symptoms & Common Diseases
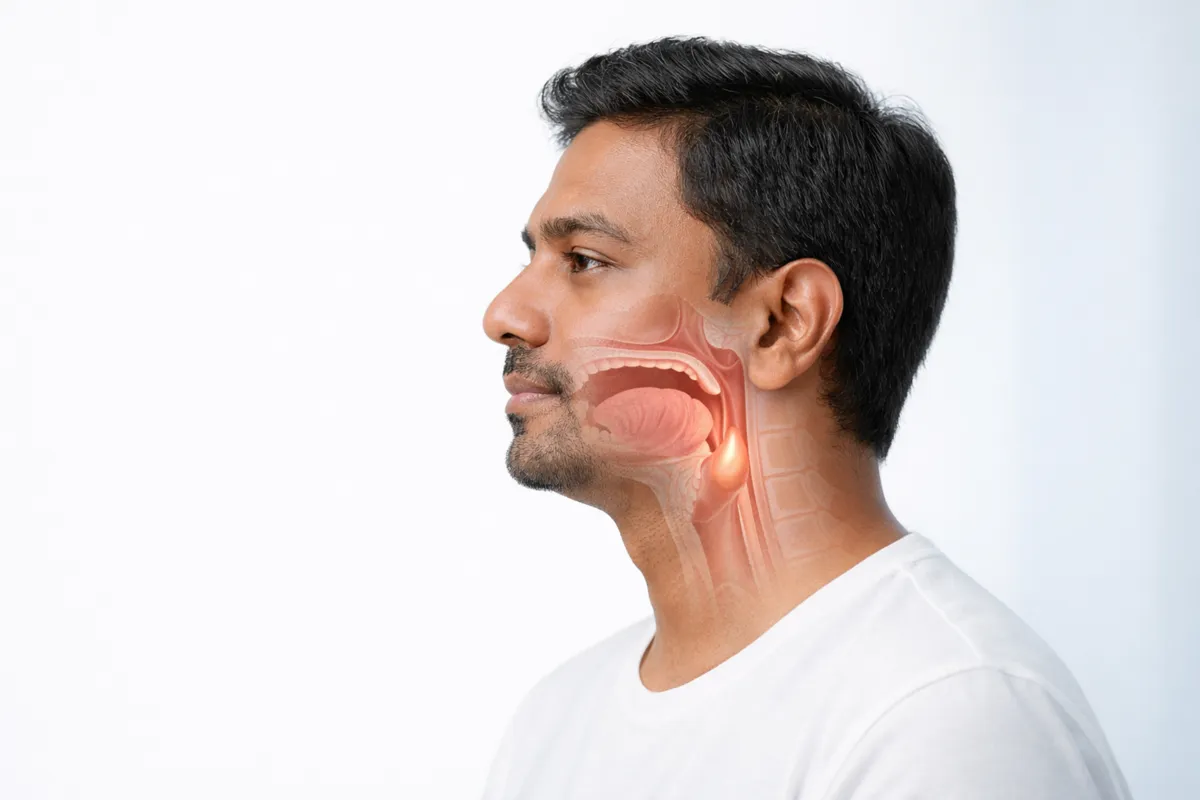
Table of Contents
- What Is the Oropharynx?
- Where Is the Oropharynx Located?
- Anatomy of the Oropharynx
- Parts of the Oropharynx
- Functions of the Oropharynx
- Role of the Oropharynx in Swallowing
- Role of Tonsils in Immune Defence
- Common Symptoms Related to the Oropharynx
- Common Diseases of the Oropharynx
- Risk Factors for Oropharyngeal Diseases
- Symptoms That May Indicate Cancer
- How Oropharyngeal Conditions Are Diagnosed
- Physical Examination & Throat Exam
- Imaging & Endoscopy
- Biopsy and Lab Tests
- Treatment Options for Oropharyngeal Diseases
- Medical Treatment (Antibiotics, Antivirals)
- Surgical & Advanced Treatments
- Prevention & Oral-Throat Health Tips
- When to See a Doctor
- Conclusion
- FAQ's
- References
If you have ever wondered why a sore throat can affect swallowing, speaking, and even your ears, the answer often lies in a small but important area called the oropharynx. Understanding your oropharynx can help you recognise common problems early and know when you should get checked.
What Is the Oropharynx?
The oropharynx is the middle part of your throat, located behind your mouth. It forms a shared passageway for air (when you breathe) and food and liquids (when you swallow).
Where Is the Oropharynx Located?
Your oropharynx sits between two other throat regions:
- Above: The nasopharynx (behind your nose)
- Below: The hypopharynx (lower throat, leading towards the oesophagus and voice box)
It extends roughly from the soft palate at the back of the roof of your mouth down to the level of the hyoid bone and upper epiglottis region.
Anatomy of the Oropharynx
The oropharynx is lined by a moist surface (mucosa) and supported by muscles that help you swallow and speak. It also contains lymphoid tissue that supports immune defence.
Parts of the Oropharynx
Key structures include:
- Soft palate and uvula (the hanging tissue at the back of the mouth)
- Palatine tonsils (one on each side)
- Base of the tongue (the back one-third of your tongue)
- Side and back walls of the throat
Functions of the Oropharynx
Your oropharynx plays several essential roles:
- Breathing: It allows air to pass from your nose and mouth into your lower airway.
- Swallowing: It helps move food and liquids safely backwards towards your oesophagus.
- Speech: It contributes to resonance and clear articulation.
- Immune support: Tonsils and related tissue can help trap and respond to germs.
Role of the Oropharynx in Swallowing
When you swallow, muscles in the tongue and throat push food backwards. At the same time, the soft palate lifts to reduce the chance of food or liquid going up into your nasal passages. This is one reason throat inflammation can make swallowing painful.
Role of Tonsils in Immune Defence
Your tonsils sit at a strategic point where germs may enter through the mouth or nose. They can help your immune system recognise threats, especially earlier in life. Because they actively respond to infection, they can also become swollen and sore.
Common Symptoms Related to the Oropharynx
Many oropharyngeal symptoms overlap with common viral illnesses, which is reassuring. Still, it helps to track what you feel and how long it lasts. Common symptoms include:
- Sore throat
- Pain when swallowing
- A dry, scratchy, or burning feeling
- A “lump in the throat” sensation
- Hoarseness or voice changes
- Bad breath
- Fever and body aches (more common with infections)
- Ear pain (sometimes referred pain from the throat)
- Swollen glands in the neck
If you are trying to make sense of sore throat symptoms, focus on the pattern: sudden onset with fever may suggest infection, while a longer, recurring pattern may point to reflux, irritation, or another underlying issue.
Common Diseases of the Oropharynx
Common causes of oropharyngeal discomfort include:
- Viral pharyngitis: The most frequent cause of sore throat, often improving with rest, fluids, and symptom relief.
- Bacterial throat infections (including streptococcal infection): More likely when you have fever, swollen neck glands, and no cough.
- Inflammation from postnasal drip or allergies: Mucus irritation can cause repeated throat clearing and soreness.
- Fungal infection (oral thrush): More likely if you are immunocompromised or have used inhaled steroids without rinsing your mouth.
- Laryngopharyngeal reflux: Stomach contents reaching the throat can cause hoarseness, throat clearing, and a globus sensation.
- Peritonsillar abscess (quinsy): A more severe complication that can cause one-sided throat pain, difficulty opening your mouth, and a muffled voice.
- Oropharyngeal cancer: Less common, but important to recognise early. Some cases are linked to HPV.
The term tonsillitis refers specifically to inflammation of the tonsils, which can occur due to viral or bacterial infection.
Risk Factors for Oropharyngeal Diseases
Your risk can increase with:
- Close contact with people who have viral infections
- Smoking or chewing tobacco
- Regular alcohol intake
- Poor oral hygiene
- Reflux symptoms
- Reduced immunity (due to illness or certain medications)
- HPV infection (linked to a portion of oropharyngeal cancers)
Symptoms That May Indicate Cancer
Most sore throats are not cancer. Still, you should not ignore symptoms that persist or progress. Consider medical review if you have:
- A sore throat lasting more than three weeks
- A lump in your neck
- Persistent difficulty swallowing or a feeling that food is sticking
- Ongoing ear pain on one side without an ear infection
- Unexplained weight loss
- A persistent ulcer or growth in the throat or at the back of the tongue
- Coughing up blood (even small amounts)
HPV-associated oropharyngeal cancers often involve the tonsil or base of tongue region and may present subtly at first. If you have concerning symptoms, getting assessed early is a sensible step, not a reason to panic.
How Oropharyngeal Conditions Are Diagnosed
Diagnosis usually starts with a careful history and throat examination. Your clinician may then recommend targeted tests depending on suspected cause.
Physical Examination & Throat Exam
A clinician typically checks:
- The mouth, tongue, tonsils, and back of throat
- Neck glands for swelling or lumps
- Signs of dehydration or breathing difficulty
Imaging & Endoscopy
If symptoms persist, recur frequently, or a mass is suspected, you may be advised to have:
- Flexible endoscopy (a thin camera to examine deeper throat areas)
- CT or MRI scans to assess soft tissues and lymph nodes
Biopsy and Lab Tests
Depending on findings, you may need:
- A throat swab to confirm bacterial infection such as group A strep
- Basic blood work if infection severity or complications are suspected
- A biopsy of any suspicious lesion, sometimes with HPV-related testing where appropriate
Treatment Options for Oropharyngeal Diseases
Your treatment depends on the cause and severity.
Medical Treatment (Antibiotics, Antivirals)
Common approaches include:
- Self-care for viral illness: Hydration, warm salt-water gargles, soothing fluids, and appropriate pain relief.
- Antibiotics: Used when bacterial infection is confirmed or strongly suspected, to treat infection and reduce complications.
- Antifungals: For oral thrush.
- Reflux management: Dietary changes, timing of meals, and medications if advised.
Avoid self-medicating with antibiotics without medical advice, as unnecessary use can cause side effects and antibiotic resistance.
Surgical & Advanced Treatments
You may need procedures when complications or persistent problems occur, such as:
- Drainage and treatment for a peritonsillar abscess
- Consideration of tonsil surgery for selected cases of recurrent severe throat infections
- For cancers, treatment may include surgery, radiotherapy, chemotherapy, targeted therapy, or immunotherapy based on staging and overall health
Prevention & Oral-Throat Health Tips
Small habits can make a real difference:
- Wash your hands regularly and avoid sharing utensils during infections
- Stay well hydrated
- Limit smoking and alcohol, or stop if you can
- Maintain good oral hygiene and regular dental care
- Manage reflux triggers (late meals, very spicy or fatty foods, excess caffeine)
- Discuss HPV vaccination with your clinician if relevant to your age and eligibility
- Seek timely care for persistent or recurring symptoms
When to See a Doctor
Arrange medical review if:
- Your throat pain is severe or worsening
- You have high fever, dehydration, or cannot swallow fluids
- You have breathing difficulty, drooling, or noisy breathing
- You develop one-sided swelling, trouble opening your mouth, or a muffled voice
- You notice a neck lump or symptoms lasting longer than expected
If you feel unsure, it is always reasonable to get checked. Reassurance after an examination can be just as valuable as treatment.
Conclusion
Your oropharynx is a busy crossroads for breathing, swallowing, and immune defence, so it is not surprising that it can become irritated or infected. Most oropharyngeal conditions are treatable, especially when you act early and follow medical advice.
If your clinician recommends tests such as a throat swab, blood investigations, or specialised screening, Metropolis Healthcare can support you with 4,000+ tests, NABL and CAP-accredited laboratories, and accurate reporting. You can also benefit from home sample collection supported by strong coverage across 10,000 touchpoints, plus convenient booking via the website, call, app, or WhatsApp. Metropolis also offers a range of preventive packages, including full body checkups, to help you stay on top of your health.
FAQ's
What Is The Main Function Of The Oropharynx?
Its main function is to act as a shared passageway for air, food, and liquids, supporting both breathing and swallowing.
What Causes Pain In The Oropharynx?
Common causes include viral infections, bacterial throat infections, inflammation from postnasal drip, reflux-related irritation, and less commonly, abscesses or cancers.
Is Oropharyngeal Cancer Serious?
Yes, it is a serious condition, but outcomes can be better with early detection and appropriate treatment. Persistent symptoms should be assessed promptly.
How Is Oropharyngitis Treated?
Treatment depends on the cause. Viral cases usually need symptom relief and rest, while bacterial cases may require antibiotics. Your clinician will guide the right approach.
Can HPV Cause Oropharyngeal Cancer?
HPV is linked to a proportion of oropharyngeal cancers, particularly in the tonsil and base of tongue region. Risk varies between individuals, and vaccination and safer practices can reduce risk.
References
- Vogel DWT, Zbaeren P, Thoeny HC. Cancer of the oral cavity and oropharynx. Cancer Imaging. 2010;10(1):62-72. PMID: 20233682.
- Pytynia KB, Dahlstrom KR, Sturgis EM. Epidemiology of HPV-associated oropharyngeal cancer. Oral Oncol. 2014;50(5):380-386. PMID: 24461628.
- Lechner M, Liu J, Masterson L, Fenton TR. HPV-associated oropharyngeal cancer: epidemiology, molecular biology and clinical management. Nat Rev Clin Oncol. 2022;19(5):306-327. PMID: 35105976.
- Panwar A, Batra R, Lydiatt WM, Ganti AK. Human papilloma virus positive oropharyngeal squamous cell carcinoma: a growing epidemic. Cancer Treat Rev. 2014;40(2):215-219. PMID: 24080155.
- Sykes EA, Wu V, Beyea MM, Simpson MTW, Beyea JA. Pharyngitis: approach to diagnosis and treatment. Can Fam Physician. 2020;66(4):251-257. PMID: 32273409.
- Bisno AL. Acute pharyngitis. N Engl J Med. 2001;344(3):205-211. PMID: 11172144.
- Franco RA Jr. Laryngopharyngeal reflux. Allergy Asthma Proc. 2006;27(1):21-25. PMID: 16598989.
- Galioto NJ. Peritonsillar abscess. Am Fam Physician. 2017;95(8):501-506. PMID: 28409615.
- Nimmana BK, Paterek E. Tonsillitis. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan [updated 2025 Jul 7]. PMID: 31335062.