Preventive Healthcare
Peristalsis: How Food Moves Through Your Digestive System
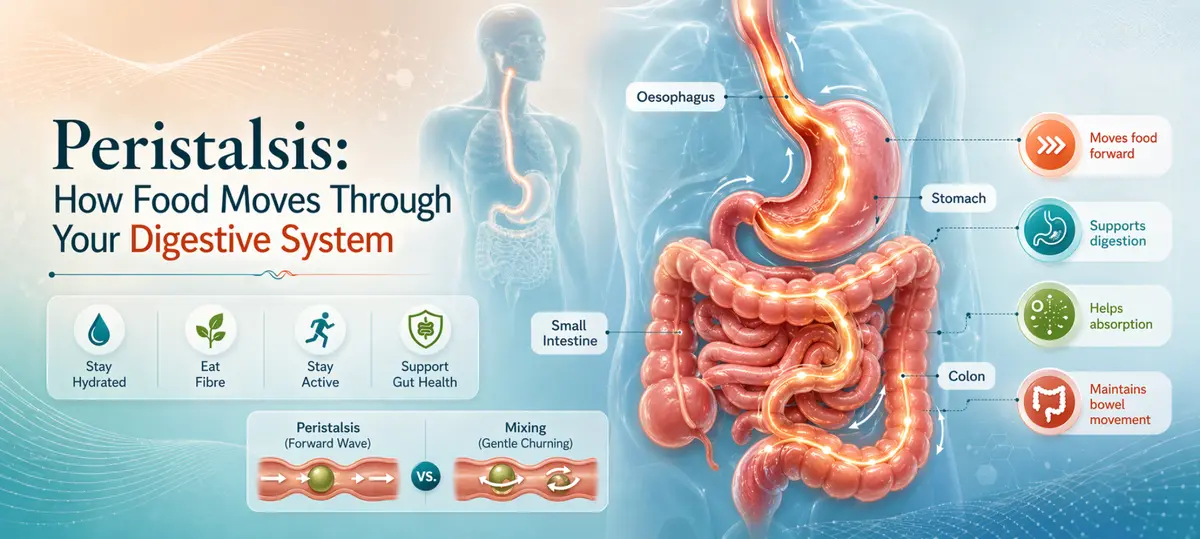
Table of Contents
- What Is Peristalsis?
- Where Does Peristalsis Occur In The Body?
- How Peristalsis Works
- Peristalsis Vs Segmentation
- Role Of Peristalsis In Digestion
- Muscles And Nerves Involved In Peristalsis
- What Happens When Peristalsis Is Disrupted?
- Conditions Related To Abnormal Peristalsis
- Symptoms Of Peristalsis Problems
- How Peristalsis Disorders Are Diagnosed
- Treatment Options For Peristalsis Disorders
- Tips To Support Healthy Digestion And Peristalsis
- Key Takeaways
- FAQs About Peristalsis
- Take A Proactive Approach To Digestive Health
- References
When you eat, your food does not move through your body by gravity alone. Your digestive system uses a coordinated series of muscle contractions to push food, fluids, and waste forward. This process is called peristalsis.
Understanding peristalsis can help you make sense of how digestion works and why symptoms such as bloating, constipation, diarrhoea, acid reflux, or difficulty swallowing can happen when this movement is disrupted.
What Is Peristalsis?
Peristalsis is the involuntary, wave like squeezing movement of muscles in your digestive tract. In simple terms, the peristalsis meaning is the automatic muscle action that moves what you swallow from one part of the gut to the next.
You do not control peristalsis consciously. It happens on its own through signals from nerves and muscles in your digestive system.
This peristalsis movement begins after you swallow and continues as food is broken down, nutrients are absorbed, and waste is moved out of your body.
Where Does Peristalsis Occur In The Body?
Peristalsis occurs in different parts of your digestive system, including:
- Oesophagus: Pushes swallowed food from your throat into your stomach
- Stomach: Mixes food with acid and digestive juices to form chyme
- Small Intestine: Moves and mixes chyme so your body can absorb nutrients
- Large Intestine: Pushes waste forward while water is absorbed
- Rectum: Helps move stool towards elimination
Although this article focuses on digestion, similar muscle contractions also help move bile and urine through other tube like structures in the body.
How Peristalsis Works
Peristalsis follows a simple pattern:
- You swallow food or liquid.
- Muscles behind the food contract.
- Muscles in front of the food relax.
- This creates a forward moving wave.
- The wave pushes food to the next part of the digestive tract.
- The process repeats until digestion and waste removal are complete.
In the oesophagus, this movement is especially important because it helps food reach your stomach even when you are sitting up, lying down, or eating quickly.
In the stomach and intestines, peristalsis also helps mix food with digestive juices. This keeps digestion moving at the right pace.
Peristalsis Vs Segmentation
Peristalsis and segmentation are not the same.
Peristalsis pushes food forward.
Segmentation mainly mixes food back and forth, especially in the intestines, so digestive juices can break it down more effectively.
You need both. Peristalsis supports forward digestive tract movement, while segmentation improves mixing and absorption.
Role Of Peristalsis In Digestion
Peristalsis is essential for normal digestion. Without it, food would not move smoothly from your mouth to your stomach and then through your intestines.
It helps your body:
- Move food in the right direction
- Mix food with stomach acid, bile, and enzymes
- Support nutrient absorption in the small intestine
- Move stool through the colon
- Clear waste and excess bacteria from the gut
This steady movement is a key part of gastrointestinal motility, which means the way your digestive system moves its contents.
Muscles And Nerves Involved In Peristalsis
Peristalsis depends on a close partnership between muscles and nerves.
The main muscles involved are:
- Circular muscles, which tighten around the digestive tube
- Longitudinal muscles, which shorten and help move contents forward
These muscles are guided by the enteric nervous system, which is often called your gut's own nervous system. Hormones and signals from your brain also influence digestion.
In the oesophagus, stomach, and intestines, this system works continuously to coordinate normal movement. When this coordination is disturbed, problems with esophageal motility or intestinal movement can develop.
What Happens When Peristalsis Is Disrupted?
When peristalsis becomes too slow, too fast, weak, uncoordinated, or blocked, digestion can become uncomfortable and less efficient.
Slow movement may lead to:
- Constipation
- Bloating
- A heavy feeling after meals
- Bacterial overgrowth
- Nausea
Fast movement may lead to:
- Diarrhoea
- Cramping
- Poor nutrient absorption
- Urgency
Abnormal movement in the oesophagus can cause food to feel stuck, chest discomfort, or regurgitation. Problems lower down in the gut can lead to abdominal pain, irregular bowel habits, or severe fullness after eating.
Conditions Related To Abnormal Peristalsis
Several conditions can affect peristalsis or broader gastrointestinal motility, including:
- Achalasia: A disorder in which the lower oesophagus does not relax properly and normal esophageal motility is impaired
- Gastroparesis: Delayed stomach emptying
- Irritable bowel syndrome or IBS: A functional gut disorder linked to altered bowel habits and abdominal pain
- Gastroesophageal reflux disease or GERD: Reflux can worsen when the lower oesophageal sphincter is weak
- Intestinal pseudo obstruction: A rare condition in which the bowel acts blocked even when there is no physical blockage
- Paralytic ileus: Temporary slowing or stopping of intestinal movement, often after surgery or illness
- Diabetes related nerve damage: Can affect digestive nerves and slow movement
- Thyroid disorders, connective tissue disorders, or neurological conditions: These may also affect gut muscle and nerve function
Symptoms Of Peristalsis Problems
Symptoms can vary depending on where the problem occurs and how severe it is.
Common symptoms include:
- Difficulty swallowing
- A feeling that food is stuck in your throat or chest
- Acid reflux or regurgitation
- Nausea or vomiting
- Early fullness while eating
- Bloating
- Burping
- Abdominal pain or cramping
- Constipation
- Diarrhoea
- Excess gas
- Abdominal swelling
- Poor appetite
- Weight loss in more serious cases
If you are exploring constipation causes, slow bowel movement is one possible factor, but low fibre intake, dehydration, medicines, thyroid problems, and low activity can also contribute.
How Peristalsis Disorders Are Diagnosed
Diagnosis depends on your symptoms and the part of the digestive system involved.
Your doctor may begin with your medical history, a physical examination, and questions about your bowel habits, swallowing, diet, medicines, and symptom pattern.
Tests may include:
- Upper GI endoscopy: To look at the oesophagus, stomach, and upper small intestine
- Barium swallow or other imaging: To assess swallowing and movement
- High resolution oesophageal manometry: To measure pressure and muscle coordination in the oesophagus
- Gastric emptying study: Often used when gastroparesis is suspected
- Blood tests: To look for dehydration, diabetes, thyroid problems, inflammation, or nutritional issues
- Stool or imaging tests: In selected cases, depending on symptoms
Your doctor may also need to rule out a physical blockage before diagnosing a true motility problem.
Treatment Options For Peristalsis Disorders
Peristalsis treatment depends on the cause. There is no single treatment that works for every motility disorder.
Lifestyle And Diet Changes
For milder symptoms, your doctor may advise:
- More fibre, if appropriate
- Better hydration
- Regular physical activity
- Smaller, more frequent meals
- Eating slowly
- Limiting very fatty or highly processed foods
- Avoiding meals close to bedtime if reflux is a problem
Medicines
Medicines may be used to:
- Stimulate gut movement
- Relieve nausea or vomiting
- Reduce diarrhoea
- Support constipation relief
- Manage reflux
- Treat the underlying condition contributing to poor motility
Treating The Underlying Cause
This may include managing:
- Diabetes
- Thyroid disease
- Electrolyte imbalance
- Medication side effects
- Inflammation or infection
- Neurological or connective tissue disorders
Specialised Treatment
Some people may need more specific care, such as:
- Swallowing therapy
- Endoscopic procedures
- Treatment for achalasia
- Nutrition support
- Hospital care if symptoms are severe
The right plan depends on whether the problem affects your oesophagus, stomach, small intestine, or colon.
Tips To Support Healthy Digestion And Peristalsis
You can support healthy gut movement with a few everyday habits:
- Drink enough water through the day
- Eat enough fibre from fruits, vegetables, pulses, and whole grains
- Stay physically active
- Do not ignore the urge to pass stool
- Try to eat meals at regular times
- Chew food well
- Cut down on excess ultra processed foods
- Review medicines with your doctor if you notice new bowel changes
- Manage stress with rest, walking, breathing exercises, or other calming routines
- Seek medical advice for symptoms that persist, worsen, or interfere with eating
Key Takeaways
- Peristalsis is the automatic muscle movement that pushes food and waste through your digestive system.
- It starts when you swallow and continues through the stomach and intestines.
- This process supports digestion, absorption, and bowel movements.
- Problems with peristalsis can lead to reflux, swallowing difficulty, bloating, constipation, diarrhoea, and nausea.
- Motility disorders can affect the oesophagus, stomach, or intestines.
- Treatment depends on the cause and may include diet changes, medicines, and specialised testing.
FAQs About Peristalsis
What Is Peristalsis In Digestion?
Peristalsis is the automatic squeezing and relaxing action of muscles that moves food through your digestive system. It helps carry food from your oesophagus to your stomach and then through your intestines.
What Happens If Peristalsis Stops?
If peristalsis stops completely, food, fluid, and waste cannot move normally through the gut. This can lead to severe bloating, vomiting, constipation, or blockage like symptoms and needs prompt medical attention.
What Is The Difference Between Peristalsis And Peristaltic?
Peristalsis is the process itself. Peristaltic is the describing word used for anything related to that movement, such as peristaltic waves.
How Do You Stimulate Peristalsis?
You can often support normal peristalsis by drinking enough water, staying active, eating enough fibre, and keeping regular meal and toilet habits. If symptoms are persistent, you should speak with your doctor rather than trying to self treat for too long.
Where Does Peristalsis Occur In The Body?
It occurs throughout the digestive tract, especially in the oesophagus, stomach, small intestine, and large intestine. Similar muscle contractions also occur in other tubular structures such as the ureters.
How Does Peristalsis Move Food Through The Digestive Tract?
Muscles behind the food contract while muscles in front relax. This creates a wave that pushes food forward in a coordinated direction.
What Muscles Are Responsible For Peristalsis?
The main muscles are circular and longitudinal smooth muscles in the wall of the digestive tract. They work together under nerve control to move food along.
What Happens If Peristalsis Stops Working?
You may develop swallowing difficulty, nausea, vomiting, constipation, reflux, abdominal swelling, or pain depending on the area affected. The severity can range from mild to urgent.
What Diseases Affect Peristalsis?
Conditions such as achalasia, gastroparesis, IBS, GERD, intestinal pseudo obstruction, diabetes related nerve damage, thyroid disease, and some neurological disorders can affect gut movement.
How Can I Improve Peristalsis Naturally?
The most helpful natural measures are hydration, fibre, regular movement, stress management, and consistent meal timing. These steps support healthy digestion, but they do not replace medical care when symptoms are significant.
Does Fibre Help Peristalsis?
Yes, fibre can help bowel movement in many people by adding bulk and supporting easier stool passage. However, the right amount depends on your symptoms, and in some motility disorders too much fibre may worsen bloating.
Can Stress Affect Digestive Movement?
Yes, stress can affect the brain gut connection and may worsen bowel symptoms, especially in people with IBS or sensitive digestion. It may not be the only cause, but it can make symptoms more noticeable.
Take A Proactive Approach To Digestive Health
Peristalsis works quietly in the background every day, but when digestive movement changes, you may notice it quickly. Paying attention to symptoms such as ongoing bloating, reflux, swallowing difficulty, constipation, or diarrhoea can help you seek the right advice early and avoid unnecessary discomfort.
Looking after your digestive health is not only about reacting to symptoms. It is also about staying informed about your overall health. Routine blood tests and full body checkups can help monitor related factors such as blood sugar, thyroid function, inflammation, and nutritional status, which may influence digestive wellbeing.
Metropolis Healthcare supports proactive health monitoring with over 4,000 tests, full body checkups, and speciality testing backed by accurate results from NABL and CAP accredited labs. With home sample collection across a strong network of 10,000 touchpoints, quick turnaround time, and easy booking through the website, app, call, or WhatsApp, you can stay on top of your health with greater ease and confidence.
References
- Huizinga JD, Lammers WJEP. Gut peristalsis is governed by a multitude of cooperating mechanisms. Am J Physiol Gastrointest Liver Physiol. 2009;296(1):G1-G8. PMID: 18988693.
- Yadlapati R, Kahrilas PJ, Fox MR, Bredenoord AJ, Gyawali CP, Roman S, et al. Esophageal Motility Disorders: Current Approach to Diagnostics and Therapeutics. Gastroenterology. 2022;162(6):1617-1634. PMID: 35227779.
- Schol J, Wauters L, Dickman R, Drug V, Mulak A, Serra J, et al. United European Gastroenterology and European Society for Neurogastroenterology and Motility consensus on gastroparesis. United European Gastroenterol J. 2021;9(3):287-306. PMID: 33939892.
- van der Schoot A, Drysdale C, Whelan K, Dimidi E. The Effect of Fiber Supplementation on Chronic Constipation in Adults: An Updated Systematic Review and Meta-Analysis of Randomized Controlled Trials. Am J Clin Nutr. 2022;116(4):953-969. PMID: 35816465.
- Camilleri M. Diagnosis and Treatment of Irritable Bowel Syndrome: A Review. JAMA. 2021;325(9):865-877. PMID: 33651094.
- Qin HY, Cheng CW, Tang XD, Bian ZX. Impact of psychological stress on irritable bowel syndrome. World J Gastroenterol. 2014;20(39):14126-14131. PMID: 25339801.




























