Preventive Healthcare
Duodenum: Meaning, Anatomy, Functions, and Common Conditions
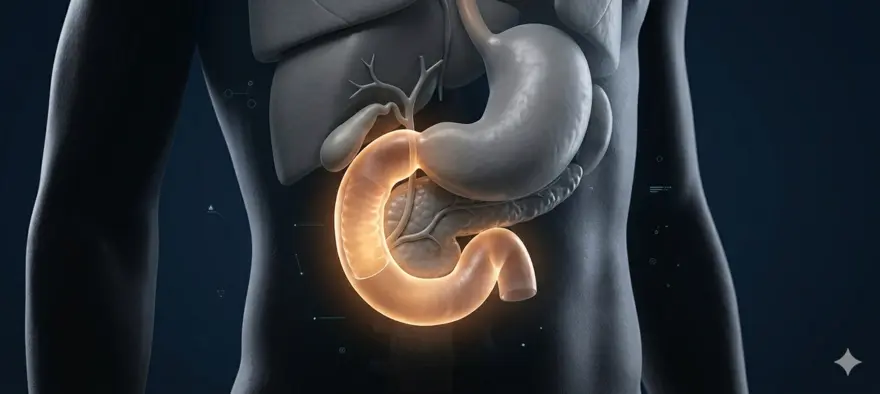
Table of Contents
- What Is the Duodenum?
- Where Is the Duodenum Located?
- Duodenum Anatomy: Structure and Overview
- Parts of the Duodenum
- Duodenum Function in Digestion
- Duodenum Histology: Microscopic Structure Explained
- How the Duodenum Works with Other Digestive Organs
- Common Diseases of the Duodenum
- Symptoms of Duodenum Problems
- How Doctors Diagnose Duodenal Conditions
- Treatment Options for Duodenal Disorders
- When Should You See a Doctor?
- Can You Live Without a Duodenum?
- Frequently Asked Questions
- Support Your Digestive Health with Awareness and Action
- References
Your digestive system is a remarkable network of organs working together to turn food into fuel. At the heart of this process sits a small but mighty structure called the duodenum. Though it measures just about 25 centimetres, it does some of the most important work in your entire digestive tract.
Here is everything you need to know about the duodenum, from its anatomy and functions to the conditions that can affect it and how to keep it healthy.
What Is the Duodenum?
The duodenum is the first and shortest section of the small intestine. It sits just below the stomach and acts as a critical transition zone between stomach digestion and nutrient absorption.
When partially digested food leaves your stomach, it enters the duodenum as a thick, acidic mixture called chyme. The duodenum then takes over, neutralising the acid, mixing in digestive enzymes from the pancreas and bile from the liver, and beginning the process of absorbing nutrients into your bloodstream.
Despite its small size, the duodenum is where much of the real chemical digestion happens. Without it, your body would struggle to break down and absorb fats, proteins, and carbohydrates properly.
Where Is the Duodenum Located?
The duodenum is located in the upper abdomen, sitting just below the stomach. It curves to the right and downward, then crosses horizontally and rises slightly before connecting to the next section of the small intestine, the jejunum.
Key points about its location:
- It begins at the pylorus, the valve at the bottom of the stomach that controls food flow into the small intestine
- It forms a "C" or horseshoe shape that wraps around the head of the pancreas
- It lies mostly behind the peritoneum, the lining of the abdominal cavity, making it largely retroperitoneal
- It sits in front of the right kidney in its descending portion
- It connects to the jejunum at a point called the duodenojejunal flexure
Duodenum Anatomy: Structure and Overview
The duodenum is a tubular, C-shaped structure that connects the stomach to the rest of the small intestine. It is the widest part of the small intestine and has a thick wall designed to handle the highly acidic chyme it receives.
Length of the Duodenum and Why It Matters
The duodenum is approximately 25 centimetres long, roughly the width of 12 fingers placed side by side. This is in fact what its name means: "duodenum" comes from the Latin for "twelve fingers." While this may seem short compared to the full length of the small intestine, which can extend to about 6 to 7 metres, the duodenum performs a disproportionately significant role. The majority of critical chemical digestion and much of the early nutrient absorption take place within these 25 centimetres.
Parts of the Duodenum
The duodenum is divided into four sections, each named according to its position and direction.
First Part: Superior Duodenum (Duodenal Bulb)
The superior segment is the first and shortest part of the duodenum, measuring about 5 centimetres. It connects directly to the stomach via the pylorus. The section that meets the pylorus is called the duodenal bulb. This area is particularly vulnerable to damage because it is the first point of contact for the highly acidic stomach contents. Most duodenal ulcers form here for this reason.
Second Part: Descending Duodenum
The descending segment runs downward alongside the right side of the vertebral column. It is approximately 8 to 10 centimetres long and is the most important section in terms of digestion. This is where the common bile duct and the pancreatic duct open into the duodenum through a small opening called the major duodenal papilla. Bile from the liver and gallbladder, along with digestive enzymes from the pancreas, enter the duodenum here and begin breaking down fats, proteins, and carbohydrates.
Third Part: Horizontal Duodenum
The horizontal segment, also called the inferior duodenum, runs from right to left across the body. It is about 10 centimetres long and passes in front of important blood vessels including the aorta and the inferior vena cava. This section continues to mix chyme with digestive juices as it moves food along the digestive tract.
Fourth Part: Ascending Duodenum
The ascending segment is the shortest part of the duodenum, measuring just 2 to 3 centimetres. It travels upward and to the left before connecting with the jejunum at the duodenojejunal flexure. This junction is supported by a band of muscle called the ligament of Treitz, which anchors the duodenum in position.
Duodenum Function in Digestion
The duodenum plays a central role in digestion. Its functions go beyond simple food transport. It actively processes chyme, signals other organs to release digestive substances, and begins absorbing nutrients.
How the Duodenum Neutralises Stomach Acid
Chyme arriving from the stomach is highly acidic. If it were to pass into the rest of the small intestine without being treated, it would damage the intestinal lining.
The duodenum addresses this by:
- Stimulating the release of the hormone secretin, which signals the pancreas to produce bicarbonate
- Mixing the bicarbonate into the chyme to raise its pH and make it less acidic
- Receiving alkaline mucus from Brunner's glands in the duodenal wall, which provides additional protection against acid
Role of Bile and Pancreatic Enzymes
Once the acid in the chyme is neutralised, the duodenum brings in digestive substances from neighbouring organs:
- The liver and gallbladder release bile through the common bile duct into the descending duodenum. Bile emulsifies fats, breaking them into smaller droplets that are easier to digest
- The pancreas releases pancreatic juice containing lipase to break down fats, amylase to break down carbohydrates, and proteases such as trypsin and chymotrypsin to break down proteins
- These substances mix with the chyme inside the duodenum, completing the chemical breakdown of food before it moves further into the intestine
Hormones Released by the Duodenum
The duodenum is also an endocrine organ. It produces hormones that regulate digestion throughout the gastrointestinal tract:
- Secretin is released in response to acid from the stomach. It stimulates the pancreas to release bicarbonate and slows gastric emptying
- Cholecystokinin (CCK) is released in response to fats and proteins in the chyme. It triggers the gallbladder to contract and release bile, and stimulates the pancreas to release digestive enzymes
- Gastric inhibitory peptide (GIP) slows the rate at which the stomach empties, preventing the duodenum from being overwhelmed with too much chyme at once
Duodenum Histology: Microscopic Structure Explained
Under a microscope, the duodenum has a specialised structure that sets it apart from other parts of the digestive tract.
Layers of the Duodenal Wall
Like other parts of the gastrointestinal tract, the duodenum has four distinct layers:
- Mucosa: The innermost layer, lined with tiny finger-like projections called villi. Each villus is further covered with even smaller microvilli, forming what is called the brush border. These structures dramatically increase the surface area available for nutrient absorption. The mucosa also contains goblet cells that secrete mucus for protection
- Submucosa: This layer sits beneath the mucosa and contains blood vessels, lymphatic vessels, and connective tissue. It also houses Brunner's glands, which are unique to the duodenum
- Muscularis: A layer of smooth muscle arranged in circular and longitudinal bands. This muscle contracts rhythmically to mix chyme with digestive juices and push food towards the jejunum through a wave-like motion called peristalsis
- Serosa: The outermost layer, made up of a thin sheet of protective cells. It covers the parts of the duodenum that are not retroperitoneal
Brunner's Glands and Their Protective Role
Brunner's glands are found exclusively in the submucosa of the duodenum. They produce an alkaline, mucus-rich secretion that helps neutralise the acid in chyme and forms a protective layer over the duodenal lining. Without Brunner's glands, the duodenal wall would be far more vulnerable to acid-related damage and ulcer formation. Their presence is one of the key features that distinguishes duodenal histology from that of the rest of the small intestine.
How the Duodenum Works with Other Digestive Organs
The duodenum does not work in isolation. It functions as a hub that coordinates the activity of several key digestive organs.
The stomach regulates how quickly it releases chyme through the pyloric valve, based on signals it receives from the duodenum. When the duodenum senses that it has received enough acid or fat, it sends hormonal signals back to slow gastric emptying.
The pancreas, which sits nestled within the curve of the duodenum, delivers digestive enzymes and bicarbonate directly into the descending segment.
The liver produces bile continuously, which is stored in the gallbladder and released into the duodenum when cholecystokinin signals a fatty meal is present.
This coordinated action ensures that digestion is efficient, appropriately timed, and well-regulated.
Common Diseases of the Duodenum
Several conditions can affect the duodenum. Many are related to excess stomach acid, infection, or inflammation:
- Duodenal ulcer: A painful sore that forms in the lining of the duodenum, most commonly in the duodenal bulb. The most frequent cause is infection with the bacterium Helicobacter pylori (H. pylori). Long-term use of non-steroidal anti-inflammatory drugs (NSAIDs) such as aspirin and ibuprofen is another common cause. If untreated, ulcers can deepen and cause serious complications including bleeding
- Duodenitis: Inflammation of the duodenal lining, often caused by H. pylori infection, excessive alcohol use, or NSAID overuse
- Celiac disease: An autoimmune condition in which the immune system attacks the duodenal lining in response to gluten. This damages the villi and impairs nutrient absorption
- Crohn's disease: A chronic inflammatory bowel disease that can affect any part of the digestive tract, including the duodenum. It causes deep inflammation, ulcers, and scarring
- Duodenal cancer: A rare but serious condition in which malignant cells develop in the duodenum
- Small bowel obstruction: A blockage in the small intestine, including the duodenum, that prevents food from passing through. This is a medical emergency
- Duodenal atresia or stenosis: Congenital conditions in which a baby is born with a completely or partially closed duodenum, requiring surgical correction shortly after birth
- Duodenal diverticulum: Small pouches that push outward through the duodenal wall. These are usually harmless but can become problematic if they get infected
Symptoms of Duodenum Problems
The symptoms of duodenal conditions often overlap with general digestive complaints. Common signs to be aware of include:
- Abdominal pain, particularly in the upper abdomen, which may be worse on an empty stomach
- A burning or gnawing sensation that can ease temporarily after eating
- Bloating and excessive gas
- Nausea and vomiting
- Indigestion or discomfort after meals
- Diarrhoea or constipation
- Unexplained weight loss
- Dark or tarry stools, which can indicate bleeding
- Vomiting blood, which is a sign of a bleeding ulcer and requires immediate medical attention
How Doctors Diagnose Duodenal Conditions
If your doctor suspects a problem with your duodenum, they may use one or more of the following approaches:
- Medical history and physical examination: Your doctor will ask about your symptoms, diet, medication use, and family history
- Blood tests: To check for signs of infection, anaemia, or nutritional deficiencies that may indicate malabsorption
- H. pylori testing: This can be done through a breath test, blood test, stool test, or biopsy, depending on the clinical situation
- Upper endoscopy (gastroscopy): A thin, flexible tube with a camera is passed through the mouth and into the duodenum. This allows direct visualisation of the duodenal lining and the ability to take biopsies
- Imaging: Ultrasound, CT scans, and MRI scans can help identify structural abnormalities, growths, or inflammation
- Barium swallow or upper GI series: An X-ray procedure in which the patient swallows a contrast substance to highlight the oesophagus, stomach, and duodenum on imaging
Treatment Options for Duodenal Disorders
Treatment depends on the specific condition diagnosed, but common approaches include:
- Antibiotics: Used to eradicate H. pylori infection, typically as a combination therapy
- Proton pump inhibitors (PPIs): Medications that reduce the amount of acid the stomach produces, giving ulcers time to heal
- H2 blockers and antacids: These also reduce or neutralise stomach acid and may be used alongside PPIs or independently
- Corticosteroids or immunosuppressants: Used to reduce inflammation in conditions like Crohn's disease
- Dietary changes: A strict gluten-free diet is the primary treatment for celiac disease and is essential for allowing the duodenal lining to recover
- Surgery: Required for structural problems, cancer, severe complications of ulcers such as perforation or bleeding, or conditions like duodenal atresia. The Whipple procedure is a complex surgical option used for duodenal and pancreatic cancer
- Lifestyle modifications: Stopping smoking, limiting alcohol intake, and avoiding NSAIDs where possible can significantly reduce the risk of recurring duodenal problems
When Should You See a Doctor?
Some digestive discomfort is common and passes on its own. However, you should seek medical advice promptly if you experience:
- Persistent or worsening upper abdominal pain
- Pain that wakes you at night or is relieved only temporarily by eating
- Unintended weight loss
- Vomiting blood or passing black, tarry stools
- Severe bloating or nausea that does not resolve
- Symptoms of malnutrition such as fatigue, hair loss, or anaemia, which may point to malabsorption
Early diagnosis leads to better outcomes for most duodenal conditions. Do not wait for symptoms to become severe before seeking help.
Can You Live Without a Duodenum?
It is possible to survive without a duodenum, but it significantly affects digestion and nutrient absorption. In some cases, such as duodenal cancer or severe trauma, a surgical procedure called the Whipple operation (pancreaticoduodenectomy) removes part or all of the duodenum along with surrounding tissue.
After such surgery, the digestive system requires significant adjustment. Patients often need to follow special diets, take enzyme supplements, and receive ongoing nutritional support. The body can adapt over time, but the absence of the duodenum has lasting implications for how the digestive system functions.
Frequently Asked Questions
Why Is the Duodenum the Most Common Site for Peptic Ulcers?
The duodenum, particularly the duodenal bulb, is the first section of the small intestine to receive acidic chyme from the stomach. This area bears the brunt of the acid load before sufficient neutralisation can occur. When this acid exposure is prolonged or excessive, especially in the presence of H. pylori infection or NSAIDs, the protective mucosal lining erodes and an ulcer forms. The duodenum accounts for the majority of peptic ulcer cases.
What Enters the Duodenum from the Pancreas and Liver?
The pancreas delivers pancreatic juice into the descending duodenum through the pancreatic duct. Pancreatic juice contains bicarbonate to neutralise acid, along with enzymes including lipase, amylase, and proteases. The liver produces bile, which is stored in the gallbladder and released through the common bile duct into the same region. Bile salts emulsify fats to make them easier to digest and absorb.
What Are Brunner's Glands and Why Are They Unique to the Duodenum?
Brunner's glands are mucus-secreting glands found exclusively in the submucosa of the duodenum. They produce a thick, alkaline secretion that neutralises acidic chyme and coats the duodenal lining with a protective layer. Their presence in the duodenum reflects the unique challenge this organ faces: it must handle highly acidic stomach contents while still performing delicate absorption work. No other section of the intestine has these glands.
How Does the Duodenum Regulate Stomach Emptying?
The duodenum monitors the composition of the chyme it receives and sends hormonal signals back to the stomach to control the pace of emptying. When the duodenum detects high acidity, fat content, or high osmolarity in the chyme, it releases hormones such as secretin and gastric inhibitory peptide. These hormones slow the movement of food from the stomach into the duodenum, preventing the digestive system from being overwhelmed and allowing adequate time for neutralisation and enzyme activity.
Is the Duodenum Retroperitoneal?
For the most part, yes. The second, third, and fourth parts of the duodenum are considered retroperitoneal, meaning they sit behind the peritoneum and are fixed in position. Only the first part, the superior duodenum or duodenal bulb, is intraperitoneal and has some mobility. The retroperitoneal position of most of the duodenum gives it stability but also makes it more difficult to access surgically.
Support Your Digestive Health with Awareness and Action
The duodenum may be a short segment of the digestive tract, but its role in digestion, nutrient absorption, and hormonal regulation makes it indispensable to your overall health. Taking care of your gut means watching what you eat, avoiding excess alcohol and unnecessary medications, and paying attention to persistent digestive symptoms.
Good digestive health is also connected to your broader wellbeing. If you have been experiencing recurring digestive discomfort, unexplained fatigue, or nutritional deficiencies, it may be worth checking in on your internal health with a proper diagnostic screen.
Metropolis Healthcare offers a comprehensive range of blood tests, full body checkups, and speciality diagnostics to help you stay ahead of potential health concerns. With home sample collection available across an extensive network, quick turnaround times, and accurate results, you can take a proactive step towards understanding your health from the comfort of your home. Book easily through the website, app, call, or WhatsApp.
Because the best time to understand your health is before a problem becomes serious.
References
- Johnson LR, ed. Physiology of the Gastrointestinal Tract. 5th ed. Academic Press; 2012.
- Rehfeld JF. The new biology of gastrointestinal hormones. Physiol Rev. 1998;78(4):1087-1108. PMID: 9790570.
- Malfertheiner P, Megraud F, O'Morain CA, et al. Management of Helicobacter pylori infection: the Maastricht V/Florence Consensus Report. Gut. 2017;66(1):6-30. PMID: 27707777.
- Bayliss WM, Starling EH. The mechanism of pancreatic secretion. J Physiol. 1902;28(5):325-353. PMID: 16992627.
- Rubio-Tapia A, Hill ID, Kelly CP, Calderwood AH, Murray JA. ACG clinical guidelines: diagnosis and management of celiac disease. Am J Gastroenterol. 2013;108(5):656-676. PMID: 23609613.
- Baumgart DC, Sandborn WJ. Crohn's disease. Lancet. 2012;380(9853):1590-1605. PMID: 22914295.
- Townsend CM, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 20th ed. Elsevier; 2017.























