Preventive Healthcare
Digestive System: Functions, Organs, and Disorders
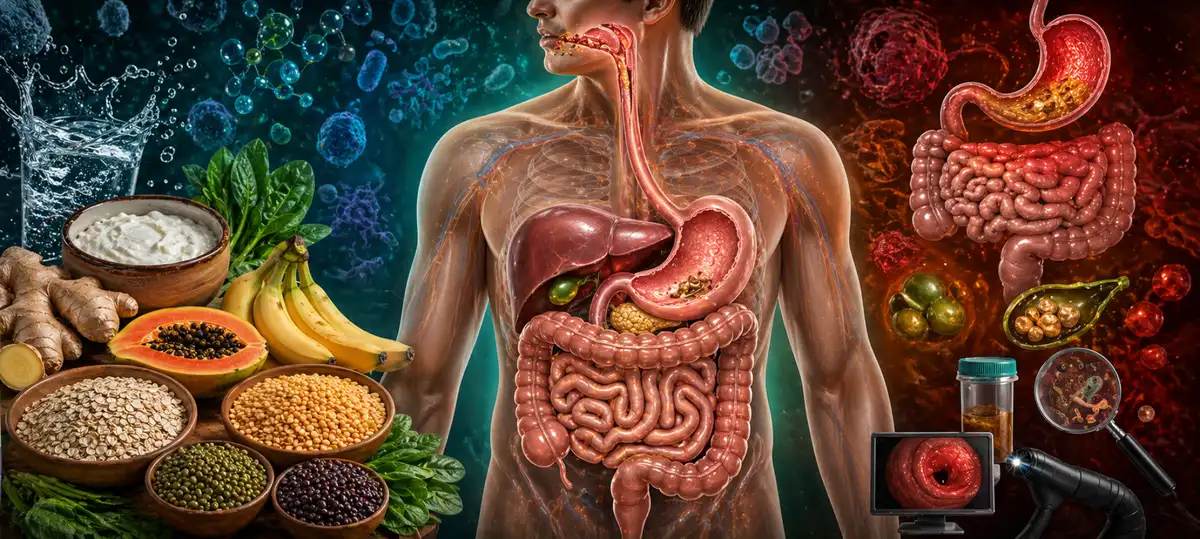
Table of Contents
- What Is the Digestive System?
- Main Functions of the Digestive System
- Organs of the Digestive System
- How Digestion Works: Step-by-Step Process
- Role of Enzymes and Digestive Juices
- Common Digestive System Disorders
- Symptoms of Digestive Problems
- Causes and Risk Factors of Digestive Disorders
- How Digestive Disorders Are Diagnosed
- Tests to Check the Digestive System
- Treatment Options for Digestive Disorders
- Tips to Keep Your Digestive System Healthy
- Foods That Support Good Digestion
- When to See a Doctor
- Key Takeaways
- FAQs About the Digestive System
- Your Gut Health Deserves Attention
- References
Your body does something remarkable every single time you eat. What begins as a plate of food is gradually broken down, sorted, absorbed, and moved along a carefully coordinated route that spans nearly the entire length of your torso. This is your digestive system at work, and it never really stops.
Most people only think about their digestion when something goes wrong. But understanding how this system functions, what can disrupt it, and how to support it can help you make better choices for your long-term health and wellbeing.
What Is the Digestive System?
The digestive system is a group of organs that work together to break down food and liquids, absorb the nutrients your body needs, and eliminate what it does not. It is one of the most complex systems in the human body, involving not just the organs you eat through, but also accessory organs that produce and deliver the chemicals needed to process food at a molecular level.
Medically, the digestive system is divided into two main parts. The gastrointestinal (GI) tract is the long, continuous tube that runs from the mouth to the anus. The biliary tract consists of the liver, gallbladder, pancreas, and bile ducts, which support digestion by producing and releasing enzymes and fluids. Together, these form the gastrointestinal system that sustains nearly every function in your body.
Main Functions of the Digestive System
The digestive system performs several distinct but interconnected functions:
- Ingestion: Taking food and liquids into the body through the mouth
- Mechanical digestion: Physically breaking food into smaller pieces through chewing and muscular churning in the stomach
- Chemical digestion: Using acids, enzymes, and bile to break nutrients down into molecules small enough to be absorbed
- Propulsion: Moving food through the digestive tract via a wave-like muscular action called peristalsis
- Absorption: Transferring nutrients, water, and electrolytes from the intestines into the bloodstream
- Elimination: Forming and expelling waste from the body as stool
Each of these functions depends on organs working in precise coordination. A disruption anywhere along the system can affect digestion as a whole.
Organs of the Digestive System
The digestive system involves more organs than most people realise. Each one plays a specific role in the overall process.
Gastrointestinal Tract
The GI tract is a continuous tube running approximately 9 metres in length when fully stretched. It comprises the following organs:
Mouth: Digestion begins here. The teeth break food into smaller pieces mechanically, while saliva moistens the food and introduces digestive enzymes that start breaking down carbohydrates before the food even leaves the mouth.
Oesophagus: A muscular tube located behind the windpipe that carries chewed food from the mouth to the stomach. It does this through peristalsis, a rhythmic series of muscular contractions.
Stomach: A muscular, J-shaped organ that churns food and mixes it with gastric acid and enzymes. The stomach's primary job is to break down proteins and continue the process of reducing food to a semi-liquid form called chyme.
Small intestine: The longest section of the GI tract, measuring roughly 6 to 7 metres. This is where most digestion and nutrient absorption takes place. The inner walls of the small intestine are lined with tiny finger-like projections called villi, which dramatically increase the surface area available for absorption.
Large intestine (colon): Receiving the remnants of digestion from the small intestine, the large intestine absorbs water and electrolytes, and houses billions of beneficial bacteria that further process undigested material. The remaining waste is compacted into stool.
Rectum and anus: The rectum stores stool until the body is ready to eliminate it, and the anus is the final opening through which waste leaves the body.
Biliary Tract and Accessory Organs
Liver: One of the body's most versatile organs, the liver produces bile, a fluid that helps digest fats. It also filters toxins from the blood, metabolises drugs, and processes nutrients absorbed from the small intestine before they enter general circulation.
Gallbladder: A small, pear-shaped organ tucked beneath the liver that stores and concentrates bile between meals. When fatty food enters the small intestine, the gallbladder contracts and releases bile to aid digestion.
Pancreas: Positioned behind the stomach, the pancreas performs two critical roles. As a digestive organ, it produces enzymes that break down proteins, fats, and carbohydrates. As an endocrine organ, it releases insulin and glucagon to regulate blood sugar.
Bile ducts: A network of channels that carry bile from the liver and gallbladder into the small intestine.
How Digestion Works: Step-by-Step Process
Digestion is a continuous journey, and it begins before you even take your first bite.
Step 1: Anticipation and the mouth
The sight and smell of food stimulate the salivary glands to begin producing saliva. When you eat, your teeth chew food into smaller pieces while saliva softens it and begins breaking down starches. The tongue shapes the softened food into a ball called a bolus, which is then swallowed.
Step 2: Through the oesophagus
The bolus travels down the oesophagus to the stomach. Peristalsis ensures food moves in one direction. A muscular valve called the lower oesophageal sphincter opens to allow food into the stomach and then closes to prevent it from flowing back up.
Step 3: In the stomach
The stomach churns the food vigorously and mixes it with hydrochloric acid and digestive enzymes. This acidic environment also helps kill potentially harmful bacteria. After one to four hours, food leaves the stomach as chyme, a thick, soupy liquid.
Step 4: Small intestine and absorption
Chyme enters the small intestine, where the majority of digestion is completed. The pancreas delivers enzymes, the liver and gallbladder supply bile, and the intestinal walls themselves produce additional enzymes. Nutrients including amino acids, sugars, fatty acids, vitamins, and minerals are absorbed through the intestinal lining into the bloodstream.
Step 5: Large intestine and waste processing
The remaining material passes into the large intestine, which absorbs water and electrolytes. Gut bacteria break down any remaining organic matter. The waste becomes progressively more solid as it moves through the colon.
Step 6: Elimination
Stool is stored in the rectum until a bowel movement occurs, after which it is expelled through the anus.
The entire journey from eating to elimination typically takes between 24 and 72 hours, though this varies from person to person.
Role of Enzymes and Digestive Juices
Digestion depends heavily on the chemicals produced at different points along the system.
Saliva contains amylase, an enzyme that begins breaking down carbohydrates in the mouth. The stomach produces hydrochloric acid, which creates the acidic environment needed for protein digestion, along with pepsin, the enzyme responsible for breaking proteins apart. The pancreas contributes a range of enzymes including lipase for fats, proteases for proteins, and amylase for carbohydrates. These are delivered to the small intestine via the pancreatic duct. Bile, produced by the liver and stored in the gallbladder, emulsifies fats, breaking them into smaller droplets so that lipase can work on them more efficiently.
Without these enzymes and digestive juices, nutrients could not be released from food or absorbed into the body, regardless of how well you eat.
Common Digestive System Disorders
The digestive system can be affected by a wide range of conditions. Some are short-lived, while others are chronic and require ongoing management. Gut health problems are among the most commonly reported medical concerns worldwide.
- Gastro-oesophageal reflux disease (GORD/GERD): Stomach acid flows back into the oesophagus, causing heartburn and irritation. Recognising acid reflux symptoms early can help prevent long-term damage to the oesophageal lining.
- Irritable bowel syndrome (IBS): A functional disorder affecting the large intestine that causes cramping, bloating, and changes in bowel habits. IBS symptoms may include alternating constipation and diarrhoea, along with abdominal discomfort.
- Inflammatory bowel disease (IBD): This includes Crohn's disease and ulcerative colitis, both of which cause chronic inflammation of the digestive tract and can lead to significant complications if untreated.
- Celiac disease: An autoimmune condition in which consuming gluten triggers an immune response that damages the lining of the small intestine, impairing nutrient absorption.
- Gastroenteritis: A viral or bacterial infection causing inflammation of the stomach and intestines, typically presenting with nausea, vomiting, diarrhoea, and cramping.
- Stomach ulcers (peptic ulcers): Open sores that develop on the lining of the stomach or the upper part of the small intestine, often caused by Helicobacter pylori bacteria or long-term use of anti-inflammatory medications.
- Gallstones: Hard deposits that form in the gallbladder, which can obstruct the bile duct and cause significant pain.
- Diverticular disease: Small pouches (diverticula) form in the walls of the colon. When they become inflamed or infected, the condition is called diverticulitis.
- Haemorrhoids: Swollen veins in the rectum or around the anus that can cause itching, pain, and bleeding.
- Colorectal cancer and other GI cancers: Cancers can develop in any part of the GI tract and are among the most serious digestive system disorders.
Symptoms of Digestive Problems
Many digestive conditions share overlapping symptoms. Common signs that the digestive system may need attention include:
- Persistent abdominal pain or cramping
- Bloating or a feeling of fullness after small meals
- Nausea or vomiting
- Heartburn or acid rising into the throat
- Diarrhoea lasting more than a few days
- Constipation or difficulty passing stool
- Changes in stool colour, consistency, or frequency
- Blood in the stool or very dark stools
- Unexplained weight loss
- Fatigue that may accompany poor nutrient absorption
- Excessive gas or belching
Occasional digestive discomfort is normal. However, symptoms that are persistent, worsening, or recurring warrant a medical review.
Causes and Risk Factors of Digestive Disorders
Digestive disorders arise from a wide range of causes. Understanding the contributing factors can help in both prevention and early identification.
- Diet: Low-fibre diets, high fat intake, excessive sugar, processed food, and insufficient hydration can all impair digestive function
- Infections: Bacterial, viral, and parasitic infections can cause acute or chronic digestive illness
- Chronic stress: Stress disrupts gut motility and is closely linked to conditions like IBS and GORD
- Medications: Long-term use of pain relievers, antibiotics, and certain other drugs can damage the stomach lining or alter the gut microbiome
- Smoking and alcohol: Both irritate the digestive tract and increase the risk of ulcers, reflux, and digestive cancers
- Obesity: Excess weight increases pressure on the stomach and raises the risk of reflux, gallstones, and fatty liver disease
- Autoimmune conditions: Conditions such as celiac disease and IBD involve the immune system attacking the digestive tract
- Genetic predisposition: A family history of colorectal cancer, IBD, or celiac disease increases individual risk
- Sedentary lifestyle: Physical activity plays a role in healthy gut motility; inactivity is linked to constipation and related issues
- Age: The digestive system changes with age, and older adults are more prone to certain conditions including diverticular disease and colorectal cancer
How Digestive Disorders Are Diagnosed
Diagnosing digestive conditions typically begins with a detailed review of your symptoms, medical history, and lifestyle. Your doctor will ask about the nature, location, and duration of symptoms, as well as any dietary patterns, medications, or relevant family history.
Based on this, they may recommend one or more investigations to get a clearer picture of what is happening inside the digestive tract.
Tests to Check the Digestive System
Several diagnostic tools are used to assess the health of the digestive system:
- Blood tests: A complete blood count (CBC), liver function tests, inflammatory markers, and tests for coeliac antibodies or H. pylori can all provide important information
- Stool tests: Used to detect infections, blood in the stool, inflammatory markers, or signs of malabsorption
- Endoscopy: A flexible camera is inserted through the mouth or rectum to directly visualise the inside of the GI tract. Upper endoscopy examines the oesophagus, stomach, and upper small intestine, while colonoscopy examines the large intestine
- Ultrasound: Commonly used to evaluate the liver, gallbladder, and pancreas for stones, cysts, or structural changes
- CT or MRI scans: Provide detailed cross-sectional images of the abdominal organs and GI tract
- X-ray and barium studies: Barium swallow or barium enema studies help visualise the movement of food or the structure of the GI tract
- Biopsy: Tissue samples taken during endoscopy to test for conditions such as celiac disease, cancer, or H. pylori infection
- Breath tests: Non-invasive tests used to detect H. pylori, lactose intolerance, or small intestinal bacterial overgrowth (SIBO)
- pH monitoring: Used to measure acid levels in the oesophagus, particularly useful for confirming GORD
Treatment Options for Digestive Disorders
Treatment varies considerably depending on the specific condition and its severity.
Lifestyle and dietary changes are the first line of management for many digestive issues. This includes eating a balanced, high-fibre diet, staying well hydrated, managing stress, reducing alcohol, and quitting smoking. These changes can significantly improve conditions like constipation, IBS, and mild GORD.
Medications are prescribed based on the diagnosis. Proton pump inhibitors reduce stomach acid in GORD and ulcers. Anti-inflammatory drugs and immunosuppressants are used for IBD. Antibiotics treat H. pylori. Laxatives or motility agents may help with constipation or other bowel disorders.
Probiotics and gut microbiome support are increasingly used alongside standard treatment for conditions like IBS and after antibiotic courses, to restore a healthy balance of gut bacteria.
Surgical intervention is required for conditions such as severe gallstones, bowel obstruction, Crohn's disease complications, diverticulitis, colorectal cancer, and certain cases of GORD. Surgery may involve removing damaged tissue, repairing structural problems, or removing tumours.
Specialist care is often needed for complex or chronic digestive conditions, involving gastroenterologists, dietitians, and in some cases oncologists or surgeons.
Tips to Keep Your Digestive System Healthy
Supporting your digestive health does not require drastic measures. Consistent daily habits make the most significant difference:
- Drink plenty of water throughout the day, as hydration is essential for smooth movement of food through the digestive tract
- Eat a diet rich in dietary fibre from fruits, vegetables, whole grains, and legumes to support bowel regularity and gut bacteria
- Include fermented foods such as yoghurt, buttermilk, and fermented vegetables, which provide beneficial probiotics
- Eat slowly and chew food thoroughly, as proper chewing reduces the workload on the rest of the digestive system
- Avoid skipping meals and aim for regular eating patterns that support consistent digestive rhythm
- Limit highly processed, high-fat, and high-sugar foods that promote inflammation and disrupt gut bacteria
- Reduce or eliminate smoking and excessive alcohol consumption, both of which significantly harm the digestive tract
- Exercise regularly, as physical activity helps maintain healthy gut motility
- Manage stress through adequate sleep, relaxation techniques, and physical activity, since the gut-brain connection is well established
- Do not ignore persistent symptoms; early attention prevents minor issues from becoming chronic conditions
Foods That Support Good Digestion
What you eat directly influences how well your digestive system functions. Foods that are particularly supportive include:
- High-fibre foods: Oats, lentils, beans, whole grains, apples, and broccoli help maintain bowel regularity and feed beneficial gut bacteria
- Probiotic-rich foods: Curd (yoghurt), lassi, and fermented foods introduce healthy bacteria into the gut
- Ginger: Well known for its anti-nausea properties, ginger supports gastric motility and soothes the digestive tract
- Papaya: Contains papain, an enzyme that aids protein digestion
- Bananas: Gentle on the digestive system and helpful during episodes of diarrhoea or stomach upset
- Leafy greens: Spinach, fenugreek, and other greens provide fibre, magnesium, and nutrients that support gut health
- Water and herbal teas: Staying hydrated is one of the simplest ways to support digestive movement and reduce constipation
- Lean proteins: Easier to digest than fatty meats and provide the amino acids needed for gut repair and function
Limiting red meat, fried foods, refined sugars, carbonated drinks, and excessive caffeine is equally important for maintaining a well-functioning gut.
When to See a Doctor
Occasional digestive discomfort is normal and usually resolves on its own. However, you should seek medical attention if you experience:
- Abdominal pain that is severe, persistent, or progressively worsening
- Blood in the stool or very dark, tarry stools
- Unexplained weight loss over a short period
- Persistent vomiting, especially if it contains blood
- Difficulty swallowing or a sensation of food getting stuck
- Symptoms that last more than two weeks or keep returning
- A family history of colorectal cancer or IBD, which may warrant earlier screening
- Any new and unexplained change in your usual bowel habits
Early investigation of digestive symptoms can catch conditions at a more manageable stage. Do not wait for symptoms to become severe before seeking advice.
Key Takeaways
- The digestive system includes the GI tract and biliary tract, working together to break down food, absorb nutrients, and eliminate waste
- Key organs include the mouth, oesophagus, stomach, small intestine, large intestine, liver, gallbladder, and pancreas
- Digestion involves mechanical and chemical processes, with enzymes and digestive juices playing essential roles
- Common digestive disorders include GORD, IBS, IBD, celiac disease, gallstones, and stomach ulcers
- Symptoms such as persistent abdominal pain, changes in bowel habits, blood in the stool, or unexplained weight loss require medical evaluation
- A high-fibre diet, adequate hydration, regular exercise, and stress management support a healthy digestive system
- Several diagnostic tests including blood tests, endoscopy, ultrasound, and stool tests are available to assess digestive health
- Early diagnosis and management of digestive disorders leads to significantly better outcomes
FAQs About the Digestive System
What Are the Main Functions of the Digestive System?
The digestive system has five core functions: ingesting food, mechanically and chemically breaking it down, absorbing nutrients and water into the bloodstream, and eliminating indigestible waste from the body. Each function depends on multiple organs working in synchrony. Without any one of these steps functioning properly, the body cannot efficiently obtain the energy and nutrients it needs to sustain health.
Which Organs Are Part of the Digestive System?
The digestive system includes the mouth, oesophagus, stomach, small intestine, and large intestine as the primary GI tract organs. The accessory organs, which support digestion without food passing through them directly, include the liver, gallbladder, pancreas, and bile ducts. Together, these form a highly coordinated system that processes everything you consume.
How Does the Digestive System Work?
Digestion begins in the mouth with chewing and saliva, continues through the oesophagus into the stomach where acids and enzymes break food down further, then moves to the small intestine where most nutrient absorption occurs. The liver, gallbladder, and pancreas contribute bile and enzymes to aid this process. Finally, the large intestine absorbs water and forms waste, which is eliminated through the rectum and anus.
What Are Common Digestive System Disorders?
Common digestive disorders include GORD (acid reflux), IBS, IBD (Crohn's disease and ulcerative colitis), celiac disease, gastroenteritis, stomach ulcers, gallstones, diverticular disease, and haemorrhoids. More serious conditions include colorectal cancer and other GI malignancies. Many digestive conditions are manageable with lifestyle changes, medication, or a combination of both.
What Are the Symptoms of Digestive Problems?
Symptoms of digestive disorders often include abdominal pain or cramping, bloating, nausea, heartburn, diarrhoea, constipation, and changes in stool. More serious warning signs include blood in the stool, difficulty swallowing, unexplained weight loss, and persistent vomiting. Symptoms that last more than two weeks or are worsening should prompt a visit to a healthcare provider.
How Can I Improve My Digestion Naturally?
Natural approaches to improving digestion include eating more fibre, staying well hydrated, chewing food slowly and thoroughly, exercising regularly, reducing stress, limiting processed and fatty foods, and including probiotic-rich foods such as curd and fermented foods in your diet. Avoiding smoking and excessive alcohol also makes a measurable difference to gut health over time.
What Foods Help Digestion?
Foods that support digestion include those rich in fibre such as oats, lentils, fruits, and vegetables, as well as probiotic foods like yoghurt. Ginger, papaya, bananas, and leafy greens are also known to support digestive function. Staying well hydrated and including lean proteins supports the gut lining and overall motility.
How Long Does Digestion Take?
The entire digestive process from eating to elimination typically takes between 24 and 72 hours. The stomach empties into the small intestine within one to four hours of eating. Absorption in the small intestine takes several more hours. The large intestine then takes between 10 and 59 hours to process and eliminate waste. These timings vary based on age, metabolism, diet, activity level, and individual gut health.
What Causes Indigestion?
Indigestion can be triggered by eating too quickly, overeating, consuming fatty or spicy foods, drinking too much alcohol or caffeine, smoking, stress, or taking certain medications such as aspirin and ibuprofen. It can also be a symptom of an underlying condition such as GORD, gastritis, or a peptic ulcer. Occasional indigestion is common, but frequent episodes should be discussed with a doctor.
When Should I See a Doctor for Digestive Issues?
See a doctor if your digestive symptoms are persistent, worsening, or accompanied by warning signs such as blood in the stool, unexplained weight loss, severe pain, vomiting, or difficulty swallowing. You should also seek advice if you have a family history of digestive cancers or IBD, or if over-the-counter remedies are no longer providing relief. Early diagnosis leads to better outcomes for nearly all digestive conditions.
Your Gut Health Deserves Attention
Your digestive system is working every moment of every day, and the signs it sends should not be ignored. From persistent bloating to unexplained weight loss, many digestive symptoms point to conditions that respond well to early diagnosis and management.
Taking a proactive approach to your health, rather than waiting for symptoms to worsen, is one of the most valuable things you can do for yourself and your family. Regular health screening can reveal important markers of digestive and overall health, including liver function, blood sugar, inflammatory indicators, and more.
Metropolis Healthcare offers a comprehensive range of diagnostic tests to support your gut health and overall wellbeing, including liver function tests, complete blood counts, stool analysis, full body checkups, and speciality panels. With over 4,000 tests, NABL and CAP-accredited laboratories, and a home sample collection network spanning 10,000 touchpoints across India, getting tested is simple, convenient, and reliable. Book through the Metropolis website, app, WhatsApp, or phone, and take the first step towards knowing your health better.
References
- Tortora GJ, Derrickson BH. Principles of Anatomy and Physiology. 15th ed. Hoboken, NJ: Wiley; 2017.
- Mayer EA. Gut feelings: the emerging biology of gut-brain communication. Nat Rev Neurosci. 2011;12(8):453-466.
- Quigley EMM. Gut bacteria in health and disease. Gastroenterol Hepatol (N Y). 2013;9(9):560-569.
- Lacy BE, Mearin F, Chang L, et al. Bowel disorders. Gastroenterology. 2016;150(6):1393-1407.
- Soll AH. Peptic ulcer and its complications. In: Feldman M, Friedman LS, Sleisenger MH, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 7th ed. Philadelphia: Saunders; 2002.
- Rubio-Tapia A, Hill ID, Kelly CP, Calderwood AH, Murray JA. ACG clinical guidelines: diagnosis and management of celiac disease. Am J Gastroenterol. 2013;108(5):656-676.
- World Gastroenterology Organisation. WGO Global Guidelines: Diet and the Gut. World Gastroenterology Organisation; 2018.
- Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68(6):394-424.