Preventive Healthcare
Umbilical Cord: Its Role During Pregnancy
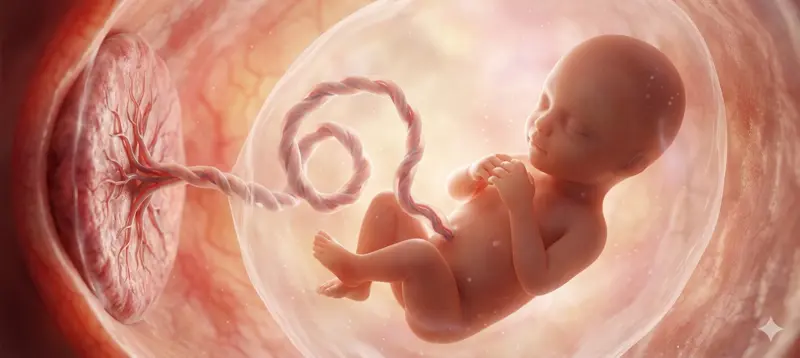
Table of Contents
- What Is the Umbilical Cord?
- What Does the Umbilical Cord Do?
- Structure of the Umbilical Cord
- Where Is the Umbilical Cord Located?
- How the Umbilical Cord Supports Fetal Development
- When Does the Umbilical Cord Form?
- What Happens to the Umbilical Cord After Birth?
- Delayed Cord Clamping: Benefits and Considerations
- Umbilical Cord Care After Birth
- Signs of Infection in the Umbilical Stump
- Common Umbilical Cord Problems During Pregnancy
- How Umbilical Cord Problems Are Diagnosed
- Umbilical Cord Blood Banking
- Pregnancy Care Tips
- When to Consult a Doctor
- Conclusion
- Frequently Asked Questions
- References
Pregnancy is a remarkable journey, and at the heart of it is a structure that quietly does one of the most important jobs imaginable. The umbilical cord is your baby's lifeline from the very early weeks of pregnancy right up until the moment of birth. Understanding what it does, how it works, and how to care for it after delivery can help you feel more confident and informed throughout this incredible time.
What Is the Umbilical Cord?
The umbilical cord is a flexible, coiled, rope-like structure that connects your developing baby to the placenta during pregnancy. It is the channel through which everything your baby needs to grow and thrive travels, including oxygen, nutrients, and hormones. At the same time, it carries waste products away from the baby back to the placenta, where your body processes them.
After birth, the cord is clamped and cut, leaving a small stump on your baby's tummy. This stump dries up and falls off naturally within a few weeks, and the spot where it was attached becomes your baby's belly button.
What Does the Umbilical Cord Do?
The umbilical cord performs several essential functions throughout pregnancy:
- It delivers oxygen-rich blood from the placenta to the fetus, supporting every organ and system as they develop.
- It provides fetal nutrition, carrying glucose, amino acids, fatty acids, vitamins, and minerals needed for healthy growth.
- It removes waste products, including carbon dioxide and urea, transporting them from the fetus back to the placenta for your body to eliminate.
- It transfers antibodies from mother to baby, offering some degree of immune protection.
- It acts as a flexible, protected channel that accommodates your baby's movements throughout the pregnancy.
In essence, the cord acts as the fetus's external circulatory, respiratory, and digestive system all in one, until your baby's own organs are ready to take over at birth.
Structure of the Umbilical Cord
The umbilical cord is made up of several distinct components:
- One umbilical vein: This vessel carries oxygenated, nutrient-rich blood from the placenta to the fetus.
- Two umbilical arteries: These cord blood vessels transport deoxygenated blood and waste products away from the fetus and back to the placenta.
- Wharton's jelly: A soft, gelatinous connective tissue that surrounds and cushions the three blood vessels, protecting them from compression or twisting caused by fetal movement.
- Amnion sheath: The outermost covering of the cord, a thin but tough membrane that encases everything within.
The cord is naturally coiled along its length, much like a telephone cable. These coils make it stronger and more resistant to kinking or squishing as the baby grows and moves. A typical cord measures between 50 and 60 centimetres in length and around 1 to 2 centimetres in diameter by the end of the second trimester.
Where Is the Umbilical Cord Located?
The umbilical cord sits within the fluid-filled amniotic sac inside your uterus. One end attaches to the centre of the placenta, the temporary organ anchored to the wall of the uterus. The other end connects to the fetus at what will eventually become the belly button (navel).
The placenta itself plays a crucial role in filtering everything that passes through the cord, ensuring that nutrients and oxygen reach the baby while waste products are removed. The cord and placenta work as one integrated system throughout pregnancy.
How the Umbilical Cord Supports Fetal Development
The cord is far more than a passive tube. It actively supports every stage of fetal development. In the earliest weeks, when the baby's organs are just beginning to form, the cord ensures a steady supply of the nutrients required to build those systems. As the baby grows larger and more complex, the cord keeps pace, expanding to meet increasing demands.
Fetal nutrition supplied through the cord fuels not just physical growth but also brain development, bone formation, and the maturation of vital organs such as the heart, lungs, and kidneys. The oxygen delivered through the cord is essential for cell metabolism throughout the body.
Because the cord lacks nerves, your baby feels no sensation through it. This means the clamping and cutting of the cord at birth causes no pain whatsoever to your newborn.
When Does the Umbilical Cord Form?
The umbilical cord begins developing around four weeks into pregnancy, very early in the first trimester. It forms from the same cells that create the placenta and amniotic sac, and it quickly becomes functional as the embryo's needs for nutrients and oxygen grow rapidly in those first weeks.
By the end of the first trimester, the cord is well established and continues to grow in length and thickness as the pregnancy progresses.
What Happens to the Umbilical Cord After Birth?
Immediately after your baby is born, the cord is clamped in two places and then cut between the clamps. This is a routine, painless procedure. It separates your baby from the placenta and marks the moment your newborn begins to breathe, feed, and function independently.
A short stump, usually a few centimetres long, is left attached to your baby's navel. Over the following one to three weeks, this stump gradually dries out, shrinks, and changes colour from yellowish-green to brown to black before falling off on its own, revealing the belly button beneath.
Delayed Cord Clamping: Benefits and Considerations
In recent years, delayed cord clamping has become a topic of growing interest in maternity care. Rather than clamping the cord immediately after birth, some practitioners wait one to three minutes before doing so. During this brief window, blood continues to flow from the placenta into the newborn.
Potential benefits of delayed clamping include:
- Increased iron stores in the newborn, which may reduce the risk of iron deficiency anaemia in the months after birth.
- Higher levels of stem cells transferred to the baby.
- Potentially improved outcomes for preterm babies, including better cardiovascular stability.
There are situations where immediate clamping remains necessary, such as when the baby or mother requires urgent medical attention. Your obstetric team will advise the approach best suited to your individual circumstances.
Umbilical Cord Care After Birth
Once you are home with your newborn, caring for the cord stump properly helps prevent infection and supports natural healing.
- Give your baby sponge baths only until the stump falls off. Avoid submerging the stump in water.
- Keep the stump clean and dry. Allow it to air dry after cleaning.
- Fold the front of the nappy down and away from the stump to prevent contact with urine or stool.
- If the stump gets soiled, wipe it gently with a damp cloth and allow it to dry completely.
- Let the stump fall off naturally. Do not attempt to pull it off, even if it appears to be hanging by a thread.
- Avoid applying alcohol to the stump. Current guidance advises against this, as it may interfere with the natural separation process.
- Dress your baby in loose clothing that does not rub against the stump.
Signs of Infection in the Umbilical Stump
The stump will change in appearance as it heals, but certain signs suggest infection and require prompt medical attention. Contact your paediatrician if you notice:
- Increasing redness or discolouration of the skin around the stump.
- Swelling at or near the base of the stump.
- Pus, cloudy fluid, or a foul smell coming from the stump.
- Bleeding that does not stop when gently wiped.
- Your baby has a fever or appears unusually unwell.
- Your baby cries when the stump or surrounding skin is touched.
- The stump has not fallen off after three weeks.
Common Umbilical Cord Problems During Pregnancy
Most pregnancies involve a cord that functions without any difficulty. However, certain conditions can arise that may affect blood flow or delivery:
- Nuchal cord: The cord loops around the fetus's neck. A loose loop is usually harmless, but a tight one can occasionally cause complications during labour.
- True knot: A genuine knot forms in the cord. Tight knots can restrict blood flow to the baby.
- Cord prolapse: The cord slips into the birth canal ahead of the baby, which can compress it during contractions. This is a medical emergency requiring immediate delivery, usually by caesarean section.
- Single umbilical artery: The cord contains only one artery instead of two. This can be associated with certain genetic conditions or structural changes in the baby's organs and warrants close monitoring.
- Abnormal cord coiling: Too many or too few coils in the cord, which may be linked to changes in fetal movement or blood flow.
- Umbilical cord cysts: Fluid-filled sacs within the cord. These are often harmless but may occasionally press on the vessels.
- Velamentous cord insertion: The cord attaches to the membranes outside the placenta rather than to the placenta itself, which can affect fetal growth.
- Vasa praevia: Unprotected cord vessels cross the cervical opening. This is a serious condition that requires early diagnosis and planned caesarean delivery.
Many of these complications are rare. Your prenatal team monitors your pregnancy closely and uses ultrasound to identify any concerns early.
How Umbilical Cord Problems Are Diagnosed
Ultrasound Examination
Routine ultrasound scans during pregnancy allow your doctor to examine the umbilical cord's attachment to the placenta, the number of vessels present, and the general appearance of the cord. Many cord abnormalities are identified during these standard scans, sometimes before any symptoms arise.
Doppler Studies
Doppler ultrasound measures blood flow through the umbilical vessels. It is particularly useful when fetal growth restriction is a concern, as reduced or abnormal blood flow through the cord can be an early indicator that the baby is not receiving adequate nourishment. Doppler studies are a non-invasive and safe way to assess how well the cord is functioning.
Monitoring During Labour
During labour, your baby's heart rate is continuously monitored using a cardiotocograph (CTG). Changes in the heart rate pattern can suggest cord compression or reduced blood flow and allow the team to respond quickly if intervention is needed.
Umbilical Cord Blood Banking
Cord blood is the blood remaining in the umbilical cord and placenta after birth. It is rich in stem cells, which have the potential to develop into various types of blood cells and may be used in the treatment of certain medical conditions.
Parents have the option of donating cord blood to a public bank, where it may be used by patients in need, or storing it privately for potential future use by their family.
Benefits of Cord Blood Storage
- Cord blood stem cells can be used in the treatment of certain blood disorders, immune conditions, and some cancers.
- It is a non-invasive collection process that poses no risk to the mother or baby.
- Privately stored cord blood offers a potentially compatible stem cell match for the child or certain family members.
- It is collected at the time of birth and cannot be retrieved later, making the decision a time-sensitive one.
It is worth discussing cord blood banking with your obstetrician during pregnancy so you can make an informed decision in advance of your due date.
Pregnancy Care Tips
While many cord-related conditions are not preventable, certain habits during pregnancy support overall fetal wellbeing and reduce avoidable risks:
- Attend all scheduled prenatal appointments and ultrasound scans.
- Report any significant reduction in your baby's movements to your midwife or doctor promptly.
- Maintain a nutritious, balanced diet to support healthy placental function and fetal growth.
- Avoid smoking, alcohol, and recreational substances, all of which can impair blood flow and fetal development.
- Manage any pre-existing conditions such as diabetes or hypertension with the guidance of your healthcare team, as these can affect placental and cord health.
- Sleep on your side during the later stages of pregnancy, as this supports optimal blood flow to the baby.
- Seek immediate care if you experience unusual pain, bleeding, or a sudden change in fetal movement.
When to Consult a Doctor
During pregnancy, contact your doctor or midwife if you notice:
- A significant or sudden decrease in your baby's movements.
- Unusual abdominal pain or cramping.
- Vaginal bleeding at any stage.
- Leaking fluid before your due date.
After birth, contact your paediatrician if the cord stump shows signs of infection, bleeds persistently, or has not fallen off within three weeks of birth.
Any concerns, however small, are always worth raising with your healthcare provider. Trust your instincts as a parent.
Conclusion
The umbilical cord is one of nature's most elegant solutions, a small but extraordinary structure that sustains your baby's life from the earliest weeks of pregnancy until the very moment of birth. Understanding its role, recognising potential concerns, and knowing how to care for the cord stump after delivery are all part of being well-prepared for your journey into parenthood.
Staying healthy throughout pregnancy also means staying informed about the markers that shape your overall wellbeing. At Metropolis Healthcare, you can access a wide range of speciality tests and health screenings, including those relevant to pregnancy and maternal health, all from the comfort of your home through a trusted home sample collection network. With over 4,000 tests, fast and accurate reports, and easy booking available through the website, app, call, or WhatsApp, Metropolis makes proactive health monitoring simple at every stage of life.
A healthy pregnancy begins with consistent care, for both you and your baby.
Frequently Asked Questions
What Is the Main Function of the Umbilical Cord?
The umbilical cord's primary function is to connect the developing fetus to the placenta, enabling the transfer of oxygen and nutrients from the mother to the baby, and carrying waste products such as carbon dioxide away from the fetus. It is the essential channel through which all fetal nourishment travels throughout pregnancy.
Does Cutting the Cord Hurt the Baby?
No. The umbilical cord does not contain any nerves, which means your baby has no sensation in the cord at all. Clamping and cutting the cord at birth is completely painless for your newborn. Similarly, as the stump dries and falls off in the weeks after birth, your baby will not feel any discomfort from the process.
Can Umbilical Cord Issues Affect Baby Health?
Yes, in some cases. Conditions such as cord prolapse, true knots, or vasa praevia can restrict blood flow to the baby or create complications during delivery. A single umbilical artery may be associated with certain chromosomal or structural conditions. However, many cord variations are harmless, and regular prenatal monitoring means most problems are identified and managed early.
How Long Does the Stump Take to Fall Off?
The umbilical cord stump typically dries up and falls off within one to three weeks of birth. During this time, it will change colour from yellowish-green to brown to black as it shrinks. If the stump has not separated by three weeks, or if you notice signs of infection, it is important to consult your paediatrician.
Can Babies Survive Cord Complications?
Many cord complications, when identified and managed early, do not lead to lasting harm. Conditions like a loose nuchal cord or minor cord cysts are usually monitored without intervention. More serious complications such as cord prolapse or vasa praevia require immediate medical attention but are manageable with prompt action. Early diagnosis through regular prenatal care is the most important factor in ensuring good outcomes.
Is Cord Blood Banking Necessary?
Cord blood banking is not a medical requirement, but it is a personal decision some families make. Cord blood contains stem cells that may be valuable in treating certain conditions in the future. Public donation means the blood can help any patient in need, while private banking preserves it specifically for your family. Discussing the options with your doctor before your due date will help you decide what is right for your circumstances.
References
Benirschke K, Burton GJ, Baergen RN. Pathology of the Human Placenta. 6th ed. Springer; 2012.
Umbilical cord abnormalities. StatPearls. National Library of Medicine; 2023.
Delayed umbilical cord clamping after birth. Committee Opinion No. 814. Obstet Gynecol. 2020;136(6):e100-e106.
Pappa KI, Anagnou NP. Novel sources of fetal stem cells: where do they fit on the developmental continuum? Regen Med. 2009;4(3):423-433.
World Health Organization. WHO recommendations for care of the preterm or low-birth-weight infant. Geneva: WHO; 2022.
Hasegawa J, Matsuoka R, Ichizuka K, et al. Umbilical cord complications during labor. J Obstet Gynaecol Res. 2009;35(5):826-829.
McDonald SJ, Middleton P, Dowswell T, Morris PS. Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes. Cochrane Database Syst Rev. 2013;7:CD004074.




























