Bone marrow test
TORCH Screen: Purpose, Procedure and Results
What Is the TORCH Test? A TORCH test is a comprehensive panel of tests that help detect infections during pregnancy. These infections can usually be passed on to your foetus during the pregnancy, so early detection and treatment can help prevent any complications for your newborn. TORCH, also known as TORCHS, is the shortened form of the different types of infections that are covered within this screening, namely: Toxoplasmosis Other include parvovirus, varicella, HIV, hepatitis virus Rubella Cytomegalovirus Herpes simplex Syphilis What Is the TORCH Test Used for? The TORCH test helps doctors screen for antibodies to infectious diseases during pregnancy. Antibodies are those proteins that recognize and destroy harmful substances in the body, such as viruses or bacteria. There are two specific antibodies that this tests for namely: Immunoglobulin G (IgG) which is an antibody that an individual has had in the past but is not considered to be acutely ill Immunoglobulin M (IgM) which is an antibody that is present when you are acutely ill with an infection Your doctor will use this test to detect your history of infection and assess if your foetus has been exposed to these infections. Test Results of the TORCH Test A TORCH test in pregnancy is usually needed to understand if you have a current infection or if you have had one. If your TORCH profile test detects the presence of IgG or IgM antibodies, it gives you a TORCH test-positive result. Treatment for the detected infection can then be started to avoid spreading these infections to your foetus. If no antibodies are detected, there is no trace of current or past infections, so you do not have to worry about passing on a condition to your baby. Why Do I Need a TORCH Test? Contracting a disease during your pregnancy could affect the baby in the womb. Most babies are more sensitive to harm during the initial 3 to 4 months of pregnancy. The TORCH test in pregnancy can help screen foetuses for infections that can cause Congenital disabilities Problems with the brain or nervous system Growth delays What Happens During the TORCH Test? Your healthcare provider will first clean and disinfect a small area, usually on your finger. They then use a sharp needle or a lancet to make a small prick in the area. The resultant blood is then collected in a small glass tube, on a test strip, on a slide or in a small container. If the bleeding continues, you will be given a small piece of cotton or a round bandage to apply on the puncture site. What Does a Positive TORCH Mean? The TORCH test result is termed positive or negative. A positive TORCH test result indicates IgG or IgM antibodies were found in the blood. This shows that you had one of the screened infections in the past; you currently have an infection or have been vaccinated against one of these diseases. Here are some key points to consider: The TORCH panel tests for several infections, including toxoplasmosis, rubella, cytomegalovirus (CMV), herpes simplex virus (HSV) and HIV. A positive result for any of these infections indicates that the mother has been exposed to the infection at some point in her life. It is important to determine the timing of the infection and whether it occurred before or during pregnancy to assess the risk of transmission to the foetus. Further diagnostic tests, such as ultrasound or amniocentesis, may be recommended to evaluate the health of the foetus. Early detection and appropriate management of these infections can help reduce the risk of complications for both mother and baby. What Diseases Are Tested for Using the TORCH Panel? The following diseases are tested for and detected using the TORCH test: Toxoplasmosis: Toxoplasmosis is a disease caused by the parasite (Toxoplasma gondii) that can enter the body through the mouth. While infants who contract this disease in the womb do not show symptoms for many years after which they may experience vision loss, deafness, seizures and mental retardation. Rubella: This is also known as German measles and can cause a rash in women. The side effects for the child are minor, but if infected in the womb, this can cause severe congenital disabilities like problems with vision, heart defects, and delayed development. Cytomegalovirus: This is a part of the herpes group of viruses that can cause hearing loss, intellectual disabilities and epilepsy in a developing foetus. Herpes simplex: This virus is usually transmitted from the mother to the foetus during the birth canal delivery. It can cause severe brain damage, seizures and breathing problems. What Is the TORCH Test After Miscarriage? A TORCH test after a miscarriage can help diagnose if the miscarriage was caused by exposure to TORCH infections during pregnancy. Here are some key points about the TORCH test after miscarriage: The purpose of the TORCH test is to identify any current or past infections that could have contributed to the miscarriage. Screening for these infections is important because they can potentially harm the foetus and lead to miscarriage or other complications. If any of the infections are detected, further testing or treatment may be necessary to prevent future complications. Is the TORCH Test Necessary? A TORCH test can help in the early detection and treatment of infectious diseases so that you do not pass them on to your foetus. This can avoid severe congenital disabilities and issues, making it necessary for your baby's health. When Is the TORCH Test Done in a Pregnancy? When the TORCH test is done in pregnancy, it is essential as the earlier it is, the less likely you are to pass on the infection to your foetus. If you are planning a baby, some doctors may also advise you to take a TORCH test before pregnancy to ensure the presence or absence of infection. Here is when the TORCH test is typically done in a pregnancy: During the first prenatal visit: The TORCH test is often included as part of routine prenatal screening. It is usually done in the early stages of pregnancy, ideally during the first trimester. If there are symptoms or risk factors: In some cases, the TORCH test may be ordered if the mother has symptoms that could suggest an infection, such as fever, rash or flu-like symptoms. Additionally, if there are known risk factors for certain infections, such as exposure to someone with a confirmed infection, the TORCH test may be recommended. Repeated testing: Depending on the results of the initial TORCH test and other factors, additional testing may be required throughout the pregnancy. This can help monitor any changes in infection status and guide appropriate management. What Does the TORCH Test Indicate? A TORCH test indicates the presence or absence of antibodies IgG and IgM when contracting an infectious disease. It is important to note that a positive result on the TORCH test does not necessarily mean that a baby will be affected by the infection. Further diagnostic testing and consultation with a healthcare provider are needed for proper evaluation and management. Conclusion The TORCH test is essential during pregnancy to maintain the health of your foetus. As TORCH infections can cause a miscarriage, doing these early in your pregnancy journey is important. If you are pregnant or planning to become pregnant, speak with your healthcare provider about whether the TORCH test may be recommended for you. Top diagnostic centres like Metropolis Labs have dedicated test packages that include every test you need during your pregnancy to gauge your health and the health of your foetus. Check out the entire list of services and tests available now.
What is Bone Marrow Biopsy: Procedure and Results
What Is a Bone Marrow Biopsy? A bone marrow test, also known as bone marrow biopsy, is a procedure used to diagnose any condition affecting your bone marrow or blood. Your bone marrow is where the blood cells of your body are made, which is why it is one of the best samples to use while looking for signs of blood-related diseases. During the bone marrow biopsy, the healthcare professional will take a small sample of marrow from your bone; afterwards, a pathologist will examine the sample under a microscope for any signs of the suspected disease. Many doctors use a bone marrow test to confirm some cancers and different blood diseases. What Is Bone Marrow? Bone marrow is located in the hollow part of more giant bones. It consists of a liquid and sponge-like tissue that is soft to the touch. The soft tissue in the bone marrow helps produce three significant components of our blood namely: Red Blood Cells (RBCs): That helps carry oxygen to other parts of our body. White Blood Cells (WBCs): The protector cells that help fight diseases. Platelets: The cells that help in blood clotting and stop bleeding whenever there is any damage to your blood vessels. The liquid in the bone marrow usually contains stem cells or maturing blood cells, making the required vitamins like Vitamin D needed for cell production. The bone marrow biopsy test is only used to test the tissue part of the bone marrow, whereas the liquid part is tested using a different procedure known as the bone marrow aspiration test. When Would a Doctor Order a Bone Marrow Biopsy? Your doctor is most likely to order a bone marrow test when he wants to: Evaluate or diagnose your condition: A bone marrow biopsy helps to understand any abnormalities in your blood cells. This can help your healthcare provider diagnose blood disorders such as cancers, other infections and unexplained fevers. Stage Cancer: Cancer staging helps doctors understand how your cancer has progressed. A bone marrow test tells them whether cancer has been spread to the bone marrow or if the tumour present in your bone marrow is growing. Monitor your treatment progress: Bone marrow blood tests can also help your doctor understand if the planned treatment is working or if you need to change the plan. It also allows doctors to understand if your bone marrow is producing enough blood cells after you have received the correct treatment. A bone marrow density test is also used to determine how compatible the donor cells are in the case of an allogeneic stem cell transplant. If an individual has too few healthy blood cells, they may need a donor to provide healthy stem cells, but the cells from the donor and recipient must match. What Conditions and Diseases Are Diagnosed with a Bone Marrow Biopsy? Any condition that involves too many or too few blood cells can be diagnosed with the help of a bone marrow test, which includes the following: Bone marrow test for anaemia: Anaemia is when your body does not have enough red blood cells to carry oxygen. Aplastic anaemia, a condition where your bone marrow does not produce enough RBCs, WBCs and platelets, can also be tested with the help of this test. Leukopenia and leukocytosis: Conditions in which the body contains too few white blood cells Thrombocytopenia and thrombocytosis: Bone marrow tests for low platelets or too many platelets help diagnose these conditions. Polycythemia vera: This kind of rare blood cancer can cause your bone marrow to produce excess red blood cells. Leukaemia: This type of blood cancer leads to abnormal blood cells, especially WBCs. Lymphoma: Lymphatic cancer that leads to an abnormal number of WBCs and RBCs. Multiple myeloma: This is another kind of rare blood cancer that can harm plasma cells Secondary cancers: A bone marrow density test can be used to test for secondary cancers like breast or lung cancer that may have spread to your bone marrow. Myelofibrosis: This condition involves the replacement of bone marrow with fibrous scar tissue. Myelodysplastic syndrome: This is a bone marrow disorder that does not allow the stem cells in the body to mature correctly. A bone marrow test can also help detect chromosome abnormalities and nutritional or vitamin deficiencies that cause the production of misshapen or large RBCs. Who Performs a Bone Marrow Biopsy? A haematologist (blood disorder specialist) or oncologist (cancer specialist) performs bone marrow biopsies. A nurse specially trained for the purpose could also help perform this test. How Can I Prepare for a Bone Marrow Biopsy? Before the bone marrow test is carried out, your healthcare provider will instruct you about the necessary preparations that may be needed for the test. Some steps may include taking a sedative to help reduce the pain on the day of the procedure if you need to fast the night before. Suppose you need someone to drive you home after the process is completed. During this time, you must also give your healthcare provider detailed information about any medical history or current medications you may be taking. Here is some vital information your doctor needs to know before carrying out the procedure: If you have a history of haemophilia or bleeding disorders If you are taking medication that thin your blood If you are taking vitamins or supplements If you are taking any allergy medicines If you are pregnant What Should I Expect During a Bone Marrow Biopsy? The bone marrow density test can be done in a hospital or your healthcare provider's office. This procedure takes about 30 minutes, and you will be awake the entire time. Your doctor will numb the test site with local anaesthesia to ensure you are comfortable before conducting the test. Steps for Bone Marrow Biopsy Depending on the biopsy site, your doctor will ask you to lie on your belly or side. A sample is commonly taken from the back of the hip bone, known as the posterior iliac crest. The doctor will then clean the skin with the help of an antiseptic and inject a kind of numbing medication onto the surface of the bone. A small incision is made at the side, and a special biopsy needle is inserted into the bone. With the help of a small syringe attached to the needle, the liquid in your bone marrow is removed. This process is called bone marrow aspiration. Next, a needle with a hollowed-out centre is inserted, which collects a small piece of your marrow. This process is called core biopsy because the hand removes a cylindrical-shaped core tissue sample. The needle is removed, and pressure is applied to the site to stop bleeding before the wound is bandaged. The collected sample is then sent to the lab for further processing. How Painful Is a Bone Marrow Biopsy? As bone cannot be numbed, you may feel slight pressure while pushing in and pulling out of the needles and samples, which can cause discomfort. Other than that, you may also feel a sharp sting during the bone marrow aspiration and a dull, brief pain during the removal of the core biopsy. You can talk to your healthcare provider about the expected pain during this procedure and solutions that help numb the site to be more comfortable during the entire process. What Should I Expect After a Bone Marrow Biopsy? Most often, you are allowed to go home on the same day as the procedure. If you choose to be sedated during the process, you may need to ask someone else to drive you home. Ensure you follow all the instructions your healthcare provider provides so you give yourself the correct care and have a speedy bone marrow biopsy recovery. Care tips for better recovery include the following: Avoid strenuous physical exercise for 24 hours after the procedure. Keep the wound dry for a minimum of 24 hours. Take a pain reliever to help with the residual discomfort and pain. Are There Risks to a Bone Marrow Biopsy? A bone marrow biopsy is a relatively risk-free procedure; however, there have been complications like heavy bleeding and infections at the side of the biopsy. The excess bleeding usually stops by applying pressure to the wound, while your doctor could prescribe an antibiotic cream for any infection. What Type of Results Do You Get, and What Do the Results Mean? After the specialist has analysed your bone marrow sample under the microscope, they will send the results to you or, in some cases, directly to your healthcare provider. The doctor will review the findings and use the bone marrow biopsy to create a treatment plan for you. They may order additional tests to confirm your diagnosis or to recommend or adjust the treatments depending on your results. Conclusion A bone marrow test helps identify diseases related to the blood and the creation of blood components. Few specialist labs provide such advanced tests. Talk to your healthcare provider about your options to conduct the test and what the results mean for you. Metropolis offers diagnostic labs across India that provide accurate blood testing and health check-up services. The reports are shared online via email and the Metropolis TruHealth app. Contact Metropolis Labs today for more information about this or other advanced testing services.
Metropolis Expert Speaks About Curing Cancer with Bone Marrow Transplant
A bone marrow transplant (BMT) is a medical procedure that involves replacing damaged or diseased bone marrow with healthy bone marrow stem cells. It is a treatment option for a variety of conditions, including certain types of cancer, autoimmune diseases, and inherited disorders. While a bone marrow transplant is a complex procedure, it offers hope to many people with life-threatening conditions. This blog provides an overview of bone marrow transplants, including their types, procedures, and recovery processes. It shares expert insights from Dr Sanjay Gohil, Head of Haematology and Transplant Immunology, Metropolis Healthcare Limited, Mumbai, on how to cure bone marrow transplants. What is a Bone Marrow Transplant? In India, there are more than 2,000 bone marrow transplants performed annually, and the number is rapidly rising. Increased BMT centres, access to standardised care, and modern technologies all greatly contribute to the procedure's safety. A stem cell transplant, also known as a bone marrow transplant, is a life-saving procedure in which the body is transfused with healthy blood-forming stem cells to replace defective or cancer-affected bone marrow. The supple, spongy tissue found inside bones is called bone marrow. The majority of the body's blood cells are generated, stored, and then discharged into the peripheral circulation. White blood cells, red blood cells, and platelets can all be formed from stem cells, which are the parent cells typically found in the marrow. BMT employs these stem cells. Autologous and Allogenic Bone Marrow Transplant The transplantation of stem cells may be autologous or allogenic. The patient is the donor in an autologous transplant. After undergoing intense therapy, the patient's frozen stem cells are returned after being removed from the patient via bone marrow harvest or apheresis (a technique for collecting peripheral blood stem cells). In allogeneic bone marrow transplants, stem cells are obtained from a genetically compatible donor—typically a sibling or sister—rather than from parents or other unrelated genetically compatible donors, who can be found through national bone marrow registries. Cord blood transplants are an additional allogeneic transplant type that uses stem cells from umbilical cord blood. Bone Marrow Transplant Procedure In specialised transplant immunology (HLA) labs, blood samples from donors and recipients are examined for the presence of human leukocyte antigen (HLA). After the initial transplant examination, the receiver has a procedure called "conditioning," where they receive chemotherapy and radiation to kill cancer cells that might spread to other regions of the body, suppress the immune system, and prepare the bone marrow for the new stem cells. Similar to a blood transfusion, stem cells are injected into the bloodstream after this myeloablative therapy. A process called engraftment helps transfused stem cells enter the bone marrow and start replicating and creating new, healthy blood cells. Engraftment typically occurs between days 15 and 30 after the transplant, depending on the type of disease being treated and the transplant. Bone Marrow Transplant Side Effects Blood counts are regularly examined to assess whether engraftment has been successful. Delays in engraftment may be caused by concurrent infections, a low number of donor stem cells, graft failure, and medications. Some individuals may experience difficulties following a bone marrow transplant, including infections, respiratory problems, bleeding due to low platelets, graft failure, and graft vs. host disease. A bone marrow transplant can result in a significant and potentially fatal complication called graft-versus-host disease (GVHD). When the immune system of the donor responds to the tissue of the recipient, GVHD results. The long-term prognosis of BMT varies from patient to patient. It also depends on factors such as the patient's age and general health, transplant type, HLA matching, type and severity of the disease being treated, disease response to treatment, adherence to medication and severity of complications. Bone Marrow Transplant Success Rate The success of bone marrow transplants has been considerably enhanced by emerging technology as more and more transplants are performed to treat various disorders. Following a bone marrow transplant, the patient needs ongoing follow-up care. The best chance for a successful bone marrow transplant is provided by a team of transplant specialists that consists of a medical oncologist or haematologist with specialisation in transplant, a lab transplant immunologist, a nurse coordinator, a social worker, a dietician, and a physiotherapist, as well as GI and respiratory specialists. Still, there is a huge gap between supply and demand that needs to be closed, and BMT production should be done at reasonable costs. Metropolis Expert on Bone Marrow Transplant Dr Sanjay Gohil has shared his expert insights on how to cure bone marrow transplants. He believes that a bone marrow transplant is a powerful treatment option that can offer hope to many patients. However, he emphasises the importance of selecting the right donor for an allogeneic transplant, as the success of the transplant depends on a good match between the donor and the patient. He also stresses the importance of close monitoring during the recovery phase to prevent and manage potential complications. Conclusion In conclusion, bone marrow transplantation is a complex but promising treatment option for many life-threatening conditions. Patients and their families should be well informed about the procedure and its potential risks and benefits. With the right donor and close monitoring during the recovery phase, bone marrow transplants can be a successful way to cure certain diseases.
Bone Marrow: Know Functions of Bone Marrow, Histology & Types
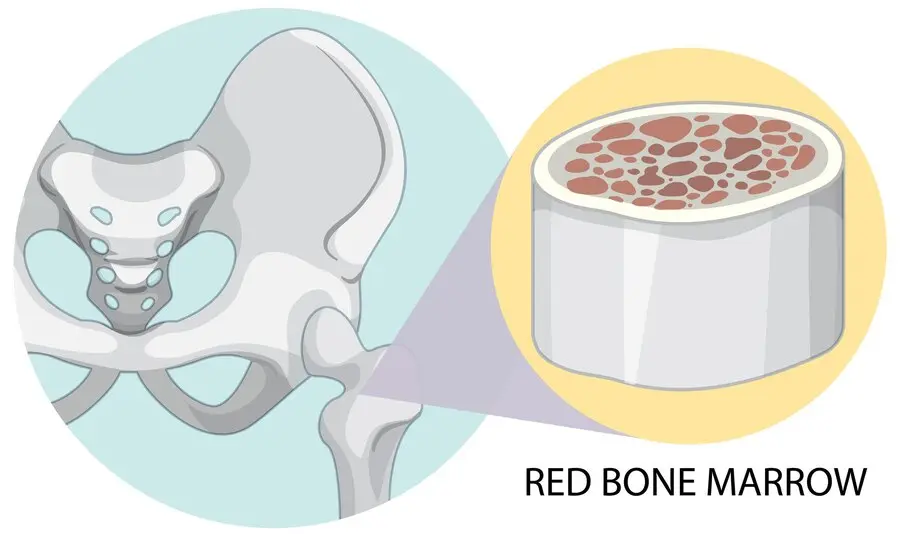
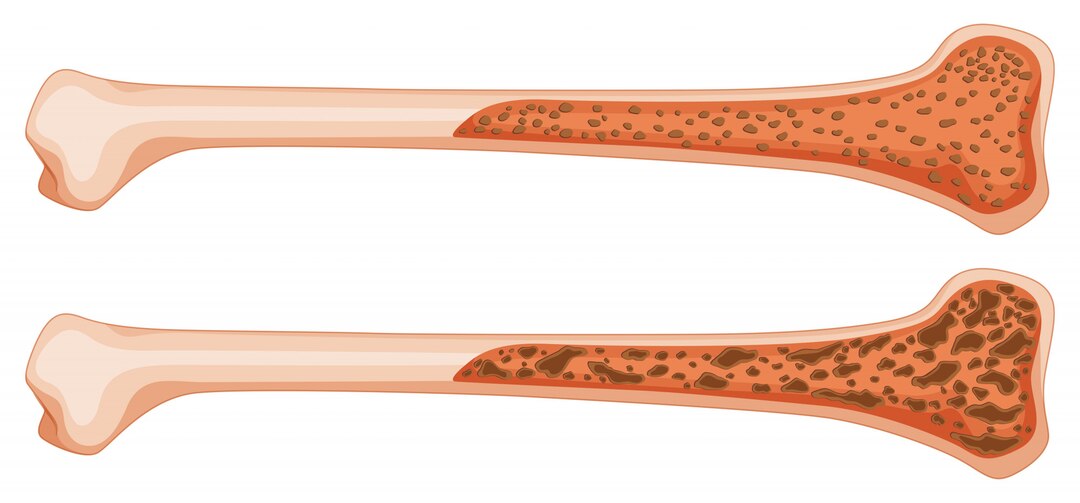
Bone marrow is the largest organ in the human body, accounting for almost 5% of the human body weight. It is responsible for the formation of the blood's cellular components. It appears like soft and spongy tissue. The safety and toxicity assessment of the blood-related disorders can be done by studying the bone marrow. Hence a chemical or a toxin causing harm to the bone marrow can be detected by the histology changes in the bone marrow. You can get to know every aspect of bone marrow histology, different types of bone marrow, and the important features of the bone marrow in this article. Where is the Bone Marrow Located? The bones in your body are anatomically made up of 3 parts: compact, spongy, and marrow. The compact bone represents the outer layer of bone and is comparatively stronger. The spongy part forms the end parts of the bone. The bone marrow forms the centre portion of the compact bones and is present at the end parts of spongy bones. The bone marrow is most commonly located in the cavities of long and axial bones; thus, it fills up the cavity of bone and blood vessels. Bone marrow is not rigid like bone. It is jelly-like and fills the cavities left by the trabecular network. What are the Functions of Bone Marrow? The two main functions of the bone marrow are as follows: To produce the blood cells like red blood cells (RBCs or erythrocytes), platelets, and white blood cells (WBCs, namely lymphocytes, granulocytes, and monocytes). This is highly vascular and constitutes Red Bone Marrow. To store the fat. It has adipocytes (fat cells) and constitutes Yellow Bone Marrow. It is comparatively less vascular than red bone marrow. What are the Histological Characteristics of the Bone Marrow? In order to diagnose an abnormal finding, it is necessary to understand the normal make-up of the tissues and cells (histology) that constitute the bone marrow. You, therefore, need to know the normal bone marrow histology. It shows the following characteristics: The exterior of the bone shows the presence of cartilage tissue and tendons. The interior hematopoietic tissue islands and adipose cells are surrounded by vascular sinuses and held within a meshwork of trabecular bone. The outer surface of this meshwork has cells known as osteoblasts. Occasional multinucleated osteoclasts are also present at the trabecular margins. Arterioles and venules occupy the interspaces between the meshwork. Bone marrow stroma consists of a heterogeneous mixture of adipocytes, fibroblasts, macrophage-like cells, and a complex extracellular matrix. Normal histology biopsy specimens show 40-60% non-bony tissue composed of hematopoietic cells. Cellularity will change depending on age. Granulocytes and monocytes are distributed in the specimens, while mature megakaryocytes are easily seen due to their large volumes. A normal bone marrow histology also shows the presence of lymphocytes, mast cells, and plasma cells. What are the Different Types of Bone Marrow? There are two types of bone marrow - red and yellow. Red bone marrow consists of hematopoietic stem cells that produce the components of your whole blood: RBCs, WBCs, and platelets. Yellow bone marrow is responsible for storing fat. It hosts adipocytes and mesenchymal stem cells. These cells preserve fat used in energy production and help develop bones, cartilage, muscles, and fat cells. Fact: Your red bone marrow makes up the entire bone marrow almost until age 7. As you grow gradually, it is replaced by the yellow bone marrow. What are the Key Features of the Bone Marrow that Make it an Important Organ? Here are some key features of the bone marrow: The bone marrow is an important part of your body as it daily produces the whole blood components without which your survival is not possible. The RBCs produced by the bone marrow provide oxygen to the whole body. The WBCs prevent and fight infections while the platelets control bleeding. It also stores fat that helps in the production of energy. Any dysfunction or abnormality in your bone marrow can be dangerous and even fatal. The common symptoms you may experience if your bone marrow is not properly functioning include - Anaemia Frequent bruising Bleeding Frequent infections Tiredness Muscle weakness What are the Diseases of Bone Marrow? Leukaemia is a blood cancer. The bone marrow makes abnormal WBCs. Lymphoma is a cancer of the lymphatic system, and bone marrow may get involved. Aplastic anemia is a condition in which RBCs are not formed in the bone marrow. How is the Abnormality in Bone Marrow Detected? The cells present in the bone marrow, its architecture, and the other features of the bone marrow can be detected by performing some tests. These include - Biopsy: Removal of a small portion of the bone marrow using a needle Aspiration: Removal of the bone marrow concentrate using aspiration Histology and cell assessment: Further detection of an abnormality A bone marrow test is hematopathology testing, which involves identifying cancerous changes in blood and bone marrow. It requires blood smears, bone marrow smears, and histopathology of tissue sections. Based on the clinical features and the condition the clinician may prescribe bone marrow tests from the list of various bone marrow profiles. Can Bone Marrow be Replaced? Bone marrow is the foundation of your blood cells, bones, and muscles. Maintain a healthy bone marrow with adequate proteins and vitamins in your diet. In certain cancers (leukaemia, lymphoma) that originate due to bone marrow abnormality, bone marrow stem cells from a healthy donor are transplanted into the bloodstream of the patient so that they can produce whole blood components.