Health Test
Liver Cirrhosis: Symptoms, Tests and Treatment
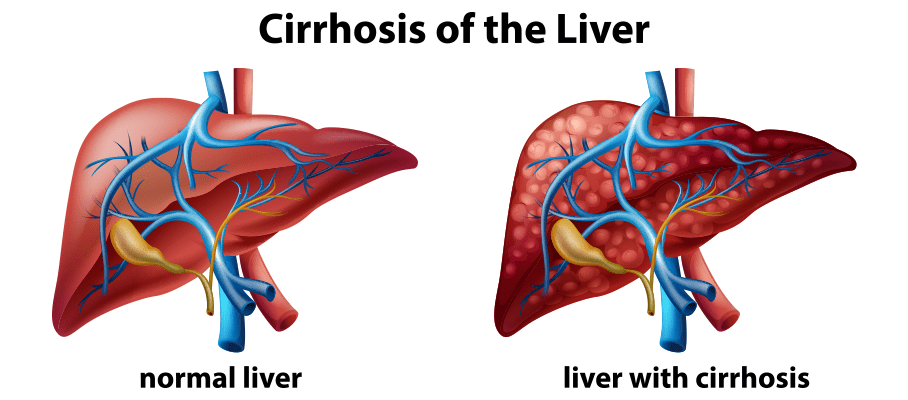
Table of Contents
Liver is one of the major abdominal organs in humans performing the important function of metabolism of carbohydrates, proteins and fats along with detoxification of harmful substances and toxins from the body by production of bile. It also functions as a major site for production of proteins and clotting factors. It also serves to store glycogen reserves for the body as well as storage of important vitamins and minerals.
Keep an eye on your liver health with a liver function test.
Here, we have discussed late-stage liver disease called liver cirrhosis, a condition in which the normal architecture of the liver is replaced by fibrotic tissue. Usually after cirrhosis sets in, it is irreversible. As the normal functions of liver are hampered due to fibrosis in liver over time, multiple complications arise, and the most important and troublesome of it is portal hypertension, where blood coming from portal vein (draining blood from entire GIT) toward liver faces excessive resistance due to fibrosis in the liver. Clinically patients with portal hypertension are identified by presence of low blood platelet count and enlarged spleen.
Symptoms of Liver Cirrhosis
The clinical signs and symptoms in cirrhosis mimic the level of fibrosis in the liver. The early signs usually include feeling tired or weak, loss of appetite, unintentionally losing weight, nausea, vomiting, mild pain or discomfort in the abdomen. Other features associated with loss of normal liver functions are development of jaundice coagulation disorder, encephalopathy, etc.
While any liver insult can ultimately lead on to cirrhosis unless intervened in time, the most common causes are chronic alcohol use, chronic viral infections affecting liver like hepatitis B and C viruses, biliary cirrhosis, autoimmune liver inflammation and rarely some inherited liver disorders. Overall chronic alcohol consumption remains to be a major cause for cirrhosis in India and worldwide. The accurate diagnosis of alcohol causing liver cirrhosis requires accurate history regarding the amount and duration of intake along with corroborative symptoms like vague upper abdominal pain, nausea, vomiting, diarrhoea and even malaise. Meanwhile a few patients may present straight away with complications of cirrhosis like abdominal distension, edema and even gastrointestinal variceal haemorrhage.
Test for Liver Cirrhosis
Laboratory investigations may reveal signs of acute blood loss as in anemia along with nutritional deficiency with low platelet counts commonly.
- Liver function tests may show signs of mild increase in serum bilirubin as fibrosis in liver hampers its elimination along with elevation in levels of liver enzymes in blood, both ALT and AST are elevated but AST levels higher than ALT approximately in a ratio of 2:1 are typical of alcoholic liver disease and cirrhosis.
- Coagulation profile may show increased PT time.
- Pathological confirmation of cirrhosis can be obtained with the help of liver biopsy.
- For patients with suspected viral cause for cirrhosis blood tests may be done for detecting HCV RNA, HBsAg, HBeAg and Anti HBe levels along with quantitative HBV DNA levels.
- For autoimmune causes of cirrhosis, blood levels of antinuclear antibody (ANA) or anti-smooth-muscle antibody (ASMA) may be done.
- Anti-Mitochondrial auto-antibodies (AMA) are present in patients developing cirrhosis due to biliary cause along with other signs of cholestasis.
- Fibroscan may help detect the level of fibrosis in the liver and the need for liver transplant in future.
- For patients who have risk factors associated with development of cirrhosis it is prudent to rule out development of portal hypertension at the earliest. One should be vigilant for development of ascites and features of hypersplenism like low platelet counts (thrombocytopenia) and low WBC counts (leukopenia).
- It is important to rule out variceal bleeding in suspected patients at onset of cirrhosis with the help of endoscopy.
- Ascitic fluid study may be done to rule out other causes for it.
- Apart from these radiological investigations like CT scan or MRI abdomen should be done to evaluate the level of cirrhosis and portal hypertension.
Treatment for Liver Cirrhosis
Management of people with cirrhosis primarily revolves around 2 main components- first managing the etiology causing it and other managing the complications arising due to cirrhosis. All the complications arising due to cirrhosis require specific management.
In general, the main treatments include reducing salt from your diet and taking a type of medicine called a diuretic.
- For people developing liver cirrhosis due to excessive consumption of alcohol abstinence is the cornerstone of therapy. Patients who are unable to abstain from alcohol are shown to have significantly low 5 year survival.
- Occasionally patients with alcoholic cirrhosis have been shown to benefit from the use of glucocorticoids or oral pentoxifylline (drug causing decrease in pro inflammatory cytokines).
- For patients developing cirrhosis due to viral etiologies antiviral drugs have shown to benefit. For Hepatitis B virus Entecavir or tenofovir are useful, and for patients with cirrhosis due to Hepatitis C Virus direct antivirals have replaced the use of pegylated interferon and ribavirin.
- For patients developing cirrhosis due to autoimmune inflammation of the liver, immunosuppressive therapies are useful.
- UDCA is shown to help cirrhotic patients with etiology of biliary stasis.
Managing complications arising due to cirrhosis revolves around managing complications of portal hypertension. The measures revolve around managing portal hypertension and ascites. In people with advanced cases of liver cirrhosis, a liver transplant may be the only treatment option as the liver may not be functional.
Make sure to follow your doctor's advice and get all tests done as advised.




























