Metropolis healthcare blog
Understanding Conjunctivitis Symptoms and Signs : A Comprehensive Guide
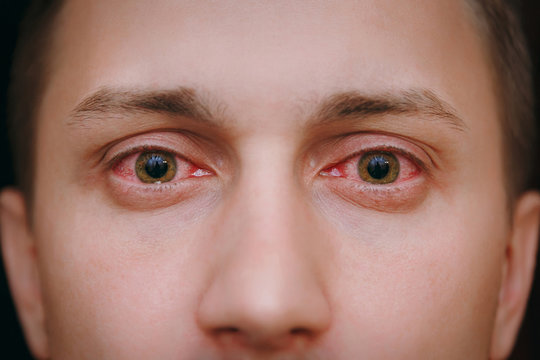
Conjunctivitis, also referred to as pink eye or eye flu, is an eye condition that can make people feel uncomfortable, irritated, and have red eyes. The thin membrane that covers the white area of the eye and the inner surface of the eyelids, the conjunctiva, becomes inflamed, which is how it is identified. To assist you in recognising and comprehending this widespread eye condition, we will break down the conjunctivitis symptoms and indicators in this post. Redness of the Eye The redness of the eyes is one of the main and most obvious signs of conjunctivitis. Because of the pink or red colour of the eye caused by the inflamed blood vessels in the conjunctiva, the condition is frequently referred to as "pink eye." Depending on the underlying cause of conjunctivitis, the degree of redness can range from mild to severe. Itching and Irritation Conjunctivitis frequently causes itching and irritation in the affected eye or eyes. People may feel the urge to touch their eyes to ease the itching, which can range from mild to severe. However, in the event of infectious conjunctivitis, scratching the eyes can exacerbate the illness and possibly transmit the infection. Watery or Discharge from the Eye Conjunctivitis can cause the eyes to tear excessively or discharge. While bacterial conjunctivitis may provide a thicker, yellow or greenish discharge, viral conjunctivitis typically results in a clear and watery discharge. Due to the body's immunological reaction to allergens, allergic conjunctivitis can also result in watery discharge. Swollen Eyelids Conjunctivitis occasionally results in swollen eyelids, making it difficult to fully open or close the eyes. The inflammation that affects the tissues of the eyelids usually causes swelling. Sensitivity to Light (Photophobia) Conjunctivitis can cause photophobia, a condition in which the eyes become sensitive to light. People who have conjunctivitis may experience discomfort and suffering when exposed to bright lights or sunshine. Crust Formation on the Eyelids Particularly after waking up in the morning, bacterial conjunctivitis can cause the development of crusts or "eye boogers" on the eyelids. These crusts develop as a result of dry discharge gathering on the eyelids while you sleep. Foreign Body Sensation Some people with conjunctivitis could feel as though they have grit or a foreign body in their eyes. This sensation may be uncomfortable and increase the desire to massage one's eyes. For early detection and suitable care, it is essential to recognise the symptoms and signs of conjunctivitis. A qualified eye care practitioner must be consulted if you suffer redness, irritation, excessive tearing, or discharge from your eyes in order to make an accurate diagnosis and receive the appropriate treatments. While the majority of conjunctivitis instances are not dangerous and can be treated with self-care or medical procedures, prompt treatment can help reduce discomfort and stop the conjunctivitis from spreading to other people. Keep in mind that having healthy eyes is crucial for sustaining vision and general wellbeing.
From Infancy to Adulthood: Understanding Hypocalcemia as a Persistent Deficiency
Low calcium can have a devastating effect on your overall wellness. Hypocalcemia is a leading condition. It is increasingly plaguing the population beyond the post-reproductive age groups. Besides, its side effects include poor blood clotting, meaning severe blood loss from minor bruises. Check this article to learn more about the hypocalcemia symptoms and how to have them treated at the earliest. Hypocalcemia: Overview Calcium is among the most vital macronutrients your body requires daily. It's synonymous with robust bones and healthy teeth. Besides, it's crucial in natural muscle coordination and circulatory functions. Individuals with poor calcium supply in their diet can experience hypocalcemia symptoms. Hypocalcemia causes acute bone issues, unexplained weight loss, and poor immunity, among severe side effects. These can turn chronic when early signs don't receive prompt clinical attention. Besides, common among individuals have contributing factors like age and underlying complications. Hypocalcemia symptoms: How to recognise the early signs? Whether a brief discomfort while climbing stairs or a sudden back ache when performing domestic chores, hypocalcemia symptoms appear with enhanced deficiency. Never ignore the mentioned symptoms below since low calcium does irreparable damage. Check out the potential signs of calcium deficiency in your body: Unexplained tetany or continuous muscle spasms. Brittle nails with marked stunted growth. Poor wound healing properties. Mental confusion with hallucinatory tendencies. Tendency to get injured from brief abrasion. Sudden numbness of hands and feet. Loss of memory with increasing seizures in epilepsy patients. While immediate consumption of calcium supplements immediately is a preventive step, please consult your physician to get treated for potential hypocalcemia symptoms. Hypocalcemia causes: What are the underlying factors? Hypocalcemia doesn't appear overnight. As your body fails to replenish the macronutrient requirements, the signs turn acute over time. Potential factors include dietary deficiencies as the primary reason, besides age, and poor immunity also spikes the calcium crisis in your body. Check out the contributing factors that could worsen your hypocalcemia: Malnutrition and poverty. Excessive physical work without adequate replenishment. Vitamin D deficiency. Improper parathyroid and thyroid functioning. Aged folks with poor calcium metabolism. Women at menopause. Surgical operations, including treatment of mechanical injuries or removal of thyroid and parathyroid glands. Chronic renal failure. Drug side effects. Acute pancreas ailments. Potential autosomal disorders like DiGeorge Syndrome and muscular dystrophy. Individuals having rheumatoid arthritis. Rapid blood transfusion to compensate for clinical ailments. Hypocalcemia diagnosis: How to catch it early? Hypocalcemia gets promptly detected through manual examination by a registered medical practitioner. Besides, pathological tests and imagery analysis help your specialist pinpoint the affected regions and the prognosis. Here's more about detecting hypocalcemia symptoms: Manual detection through tapping on potential bone joints and muscles to look for unexplained contraction and trauma. Blood test for checking calcium levels (hypocalcemia if the concentration is below 8.8 mg/dl). Tests for detecting anomalies in thyroid and parathyroid glands (these produce hormones responsible for calcium metabolism). Imagery techniques to detect osteomalacia, gouts, osteoporosis and rickets. Hypocalcemia treatment: How to control further advancement of symptoms? The primary hypocalcemia treatment includes prompt replenishment of underlying deficiencies. However, potential recovery is incomplete without addressing the root cause of low calcium in your body. Your physician shall proceed as per the diagnostic report and follow treatment or change existing medications to enhance your blood calcium levels. Here's more about hypocalcemia treatment techniques: Oral medication containing calcium supplements helps replenish the underlying shortage. Your doctor might prescribe vitamin D supplements to ensure better calcium absorption in your body. Treatment of thyroid and parathyroid ailments to naturalise secretion of calcitonin and thyrocalcitonin. Immediate supply of calcium over IV if you are experiencing potential tetany signs. Reorganise your existing medications to ensure natural blood calcium levels. How to prevent hypocalcemia during early signs? Hypocalcemia symptoms are preventable if careful about the infrequent body discomfort as the early signs. Remember, poor tolerance to pain, frequent weight loss, and abrasion from limited impact are alarming signs of calcium deficiency. Besides regular health checkups, here's more about taking a preventive approach to counter low blood calcium: Take care of your dietary intake (milk, beans, cheese, yoghurt, and sea fish). No alcohol since it pulls down your vital mineral concentration. Get treated for existing thyroid/parathyroid issues. Don't ignore frequent body discomfort persisting after laborious work (lower back pain, abnormal spasms, and muscle contractions). Get a complete health check to detect underlying autosomal or autoimmune conditions that degrade calcium levels. Reduce overweight and practice yoga or strength exercises to boost healthy muscle development (boosts calcium metabolism). Who's prone to develop hypocalcemia? Hypocalcemia symptoms are no longer limited to folks above 60. Whether neonatal, teenagers, young adults, or women in menopause, anyone with poor calcium replenishment can experience these symptoms. Check the potential features of individuals prone to develop calcium deficiencies: Newborn babies can experience low calcium levels if the mother has diabetes and contributing complications. Young kids to teenagers could develop hypocalcemia from poor dietary habits. Adults can show poor calcium levels from lifestyle issues (smoking, alcoholism, sedentary lifestyle). Men and women over 50 are prone to hypocalcemia since hormonal changes from menopause disrupt natural calcium metabolism. Individuals with genetic and autoimmune disorders are vulnerable to experiencing calcium deficiency without clinical support. Conclusion Hypocalcemia is a curable condition. Most individuals experience it at least once during their lifetime. Clinical experts suggest a balanced lifestyle and preventive care to ensure your body doesn't experience low calcium levels. Besides, never ignore potential symptoms or rely on OTC drugs for temporary relief without a clinical consultation. CTA: Hypocalcemia treatment requires blood diagnostic tests to ascertain the underlying ailments. Do you need a doorstep collection of your blood samples? Trust Metropolis Labs, thanks to their versatile technicians providing seamless collection and delivery to state-of-the-art testing facilities. For more information about the calcium total serum test, visit Metropolis Labs today.
NextGen HLA Typing in Organ Transplantation - Metropolis New Test Launch
Organ transplantation is often the last step in many chronic diseases. The human leukocyte antigen is among the primary protein whose compatibility decides the transplant's success. Besides, the accuracy of HLA testing plays a crucial role in promptly recognising potential donors' organ tissue. This article comprises the advantages of the next-generation sequencing technology (NGS) from Metropolis Healthcare. Read more to learn how the NextGen HLA typing test will transform accuracy compatibility for transplantation. NextGen HLA typing procedure: Overview The NextGen HLA testing provides the maximum HLA typing matching between recipient and donor. Among other factors, three antigen types, A, B, and DR, play a crucial role in recipient and donor compatibility. This NextGen HLA testing is a higher-resolution molecular test for solid organ and haematopoietic stem cell transplantation. Know more about this compatibility test, which helps seamless tissue matching and organ transplantation in recipients with maximum accuracy. How does the NextGen HLA testing work? Every individual inherits two pairs of A, B, and DR proteins from their parents. The NextGen HLA typing test analyses suitable donors through the matching for tissues, bone marrow, and organ transplantation. The highest chances of compatibility lies between twins and siblings. The HLA proteins are a part of the major histocompatibility complex (MHC). It functions in tandem with the T-receptor cells. This means the detection of foreign antigens in your body. Besides, it helps distinguish between self-cells and those of foreign origins to prevent auto-immune reactions. If your body contains incompatible tissues or preexisting cross-matching antibodies, HLA testing reduces rejection chances. What makes NextGen HLA testing state-of-the-art? Often in the HLA typing procedure, there's an ambiguity in choosing antibody incompatibility as the compatibility sign for transplantation. But it can also lead to rejection if other factors like lymphocyte matching are left ignored. The NextGen HLA typing test considers the following conditions: Ethnicity Antibody testing Lymphocyte cross-matching Blood typing These factors make NextGen HLA testing accurate to detect maximum HLA compatibility. Besides, it considers allelic variants in your genes to ensure the most accurate allelic profiling for donor selection. It reduces the chances of the destruction of inserted tissues in the future and enhances the success rate of organ transplantation. What are the advantages of NextGen HLA testing? The NextGen HLA typing test comprises genetic and immunological factors. These ensure maximum compatibility between donor and recipient. It offers confirmation of successful transplantation based on available stem cell transplants or solid organs from a foreign donor. Check out the various advantages of the NextGen technique over other HLA typing results: It helps predict the underlying presence of pathogenic and auto-immune disorders. NextGen technique ensures maximum allelic compatibility for haematopoietic tissues and organ transplantation. It helps choose the most suitable donor based on the preexisting allelic profiling of the recipient. Considers all existing compatibility factors to remove HLA typing ambiguity, providing near-perfect transplantation outcomes. It saves time and resources. This means higher compatibility ensures successful organ transplantation without immunity rejection issues. What else should you know about the NextGen HLA testing? Unlike most HLA typing procedures, the NextGen technique earns its impeccable reputation as the best HLA testing. Thanks to its state-of-the-art allelic characterisation, it comprises all factors that may come into play during foreign tissue and organ transplantation. Considered the gold standard approach, it's among the best available HLA typing in organ transplantation. Besides, this technique also compensates for the potential complications of graft rejection. It provides qualitative compatibility to ensure patients undergoing haematopoietic stem cell transplantation (HSCT) and organ transplantation don't experience graft vs host issues. The NextGen HLA typing procedure compensates for the recipient's survivability, especially when vital organ transplantation (kidney, liver, pancreas) happens. It also considers potential factors like underlying auto-immune disorders or conditions that can thwart a healthy organ or tissue transplantation. NextGen HLA typing - Final word The role of organ transplantation is peerless to save patients who have an impaired organ system or lost one from underlying conditions. The NextGen HLA typing procedure ensures maximum compatibility between the recipient system and potential donors. This state-of-the-art diagnostic procedure has helped reduce unexplained graft rejections in patients with suitable HLA antigen compatibility. The best part is that the NextGen HLA testing for kidney transplants is available in India. It reduces the expensive treatment cost while enhancing the accuracy towards near-perfect organ transplantation. Besides, this technique helped reduce unnecessary donor organ and tissue waste, making it a path-breaking solution in transplantation procedures.
Benefits of NextGen HLA Testing: Explains Metropolis' Experts
The NextGen HLA typing procedure helps detect a higher donor and recipient compatibility percentage. This procedure provides unmistakable human leukocyte antigen (HLA) indexing outcomes. It ensures reduced chances of graft rejection among patients receiving foreign haematopoietic tissues and organ transplantation. This high-resolution molecular diagnostic technique helps choose the perfect donor based on the characteristics of the recipient's allele. Check out more about the NextGen HLA typing procedure from Metropolis Healthcare and its state-of-the-art compatibility testing. What to Know About the NextGen HLA Testing? According to Dr Kirti Chadha, Chief Scientific Officer at Metropolis Healthcare, the NextGen testing conveniently scans through the human leukocyte antigen (HLA). This protein has the most diverse loci in the human genome, leading to unique allelic distribution in every individual. It plays a crucial role as the chief determinant of the compatibility of bone marrow and organ transplantation. Without checking for genotypic HLA allelic compatibility, the transplantation can go wrong. The validation of the NextGen HLA typing procedure helps define better genes and detect polymorphisms, resolving potential clinical impacts. How Does the NextGen HLA Typing Function? The NextGen HLA testing detects the percentage of human leukocyte antigen matching between prospective donors and the recipient's genetic setup. It helps match the HLA allelic patterns to measure the approximate similarity of the organs and tissues, reducing graft rejection. The HLA proteins help differentiate self-cells from foreign bodies, preventing auto-immune reactions. Besides, the NextGen HLA typing procedure detects the Major Histocompatibility Complex (MHCs) proteins. It helps evaluate all potential antigen complexes that may cause graft rejection post-transplantation. The NextGen technique reduces all HLA typing ambiguities concerned with tissue and organ transplantation. What Makes the NextGen HLA Typing Procedure Effective? Unlike general HLA tests, the NextGen HLA testing procedure considers parameters more than just the three pairs of human leukocyte antigens. Besides providing an accurate match between the A, B and DR between host and donor, it scans for allelic compatibility of their respective genomes. These factors often get overlooked in general HLA typing and may trigger transplant destruction even in patients with superior HLA compatibility. Next, it also considers primary factors like antibody matching, blood typing, ethnicity and lymphocyte compatibility. These evaluate the chances of HLA activation and graft rejection. The NextGen HLA typing ensures that a recipient receives the most compatible donor for their transplant, lowering any scope for graft rejection. Why Does the NextGen HLA Procedure Provide a Better Compatibility Match? The NextGen HLA typing procedure is more accurate than available HLA typing tests. Its principal design helps find the most compatible donor for their haematopoietic tissues and organ transplantation procedures. Unlike general HLA tests, it considers various factors, as mentioned above. Patients requiring HLA tissue typing for kidney transplants are vulnerable to potential organ rejection. It can wreak havoc on the overall wellness of such ailing patients. Thanks to the NextGen HLA typing procedure, which prevents post-transplantation complications, which often cause the recipient to relapse and even lead to death. While considering underlying genetic and pathological factors, doctors ensure the natural assimilation of transplanted organs for healthy living. It saves valuable life, reduces treatment costs and prevents the wastage of donor organ tissues. What Conditions Get Detected Using the NextGen HLA Typing Test? The role of the NextGen HLA typing procedure extends far beyond transplant compatibility. It is peerless in detecting underlying allelic patterns that can have antagonistic effects like drug incompatibility, auto-immune disorders and prone to develop autosomal sicknesses. The NextGen HLA typing results can detect potential conditions like silent genetic anomalies or inherited autosomal combinations. It includes testing for the below conditions: Celiac disease Narcolepsy Spondyloarthritis Ankylosing spondylitis Crohn's disease Psoriatic and reactive arthritis Sacroiliitis Uveitis Pathogenic infections Cancer Emphysema Besides, early detection of these conditions helps prompt treatment to slow down the rapid degeneration of the illness. The NextGen HLA typing procedure helps doctors detect underlying conditions with little surface symptoms. Also, if your blood comprises significant anti-HLA antibodies, it helps detect other health anomalies that may or may not include immunological factors. Final Take Besides the effectiveness of the NextGen HLA testing technique, here is what Dr Sushil Shah, Chairman of Metropolis Healthcare, shared the unique selling point about the organisation. In recent years, Metropolis Healthcare has established a centre of excellence supporting all transplant-related diagnostic techniques. It includes a state-of-the-art array of diagnostic tools, accurate report interpretation, expert laboratory technicians and dedicated subject matter specialists. According to the chairman, it makes Metropolis Healthcare a one-stop destination for all transplant-related diagnostic solutions. He also highlighted how the NextGen HLA typing helps doctors find the ideal donor for recipients and ensure better transplantation records.
What is a Heat Wave? Everything You Need to Know
Heat waves have become very common these days. With the increasing temperature, life in summer is wrapped in sweat and uncontrollable heat. Moreover, almost 90% of the Indian subcontinent has faced severe changes due to climate change. Undoubtedly, summer is expected to be cursed with scorching heat and loo. Heat waves should not be treated casually. In typical cases, a person hit by sunstroke or heat stroke recovers with glucose and water after some time. But diabetic patients are more prone to sickness in summer. Heat waves and increased temperature directly affects blood sugar lever. High heat results in excessive sweating, and if it is followed by low water intake, a persona will suffer from dehydration, which increases blood sugar levels. If such heat continues, the body will release hormones like vasopressin and cortisol, enhancing the body's glucose level and causing a spike in sugar levels. Many Metropolis doctors have stated about heat waves and diabetes, so let's look at their statements before moving ahead. As per Dr Shibani Ramchandran, Medical Affairs, Metropolis Healthcare, high temperature may impact the body's insulin which causes changes in blood sugar levels if not monitored properly. In many parts of India, humidity is also a problem with heat which further puts diabetes management on the toss. What is a Heat Wave? A heat wave is defined as abnormally hot weather or high heat accompanied by high humidity. Heat waves generally last for two to three days. However, with gradual climate change, heat waves have become more frequent during summer. Last year, parts of Europe and America have reported heat waves. In Asian countries like India, heat waves are reaching new limits causing more and more heat strokes in diabetic people along with others. How Do Heat Waves Affect a Person Having Diabetes? Heat waves are directly connected to imbalanced blood sugar levels. High heat causes more sweating. As a result, you lose excess water from your body. If you don't drink enough water in summer, you may fall sick of dehydration. Lack of sufficient water in the body causes dehydration. As a result, your blood becomes thick and the sugar or glucose present in your blood is deposited. Now this excess sugar creates an imbalance in your average blood sugar level. Furthermore, if you have a low blood sugar level, a sudden increase due to a heat wave may invite further medical complications. Rush to the hospital if you see anyone falling sick during a heat wave. Certain diabetic conditions can damage your blood vessels. Hence, your body fails to release excess heat, causing heat stroke. Heat strokes are severe and can be fatal. Effects of Heat Wave on a Diabetic Person High heat with high humidity in the Indian subcontinent in the coastal areas creates more of a menace in summer. If you have diabetes, you may develop any of the following medical conditions: Fatigue Dehydration Heat exhaustion Hypoglycaemia Symptoms Of a Heat Stroke Common symptoms from which you can understand that heat is affecting you are: Fatigue Low blood pressure Palpitations Dizziness Dry mouth Darker urine However, you should be careful of the following specific symptoms: Heat Exhaustion Though heat exhaustion is not similar to heat strokes, it can lead to heat strokes. Do not neglect the following symptoms: Low blood pressure Headache Dizziness Nausea Vomiting Muscle cramps Cool skin Hypoglycaemia You should immediately consult a doctor if your blood sugar level falls below 70 mg/dl. Keep an eye out for the following symptoms: Palpitations Excessive sweating Tremors Hyperglycaemia You may have hyperglycemia if your blood sugar level exceeds 130 mg/dl before eating and 180 mg/dl after your meal. Heat waves affect people differently. Take care of yourself and your near ones if you are experiencing: Frequent urinating Dizziness Fatigue Feeling thirsty frequently. When Should You Visit a Doctor? You can consume 15 grams of carbs if your blood sugar level drops suddenly. However, you can take a dose of insulin if your glucose level strikes high. Visit your nearest health care centre to initiate treatment immediately. Treatment Your doctor will treat you based on your blood sugar level. Preventive Measures To prevent yourself from getting affected during heat waves, you should follow specific instructions: Simple diet Avoid rich and oily food during heat waves. Instead, bring a change in your daily food habits. Try eating simple and easy-to-digest foods like porridge, dal and rice. Getting a personalised diet chart from a dietician would be best. Have plenty of water-rich fruits and vegetables such as watermelons, cucumbers, tomatoes, tender coconut etc. More liquid intake Add more liquid food to your daily diet. Drink at least 3 litres of water in summer. Avoid going outside without a bottle of water. Refrain from consuming alcohol or even soda. You can have buttermilk, curd and sugar-free fruit juices. Medicines Always keep your medicines with you. Talk to your doctors about whether you have to change certain medications during a heat wave. Take your pills or insulin regularly and on time. Reduced exercise Limit your regular high-intensity exercise during heat waves. High-intensity exercises cause more sweating. Excess water loss is not suitable for your health now. Instead, shift to moderate or light exercise like warm-ups or do it at a cooler time of day. Wear loose clothes Avoid wearing any dark-coloured or tight-fitted clothes during summer. Tight garments will obstruct the heat from releasing from your body. You may feel exhausted. Moreover, light colours deflect heat whereas dark colours absorb heat. Stay in the shade Try to stay indoors as much as possible. Reduce frequent outdoor work as much as you can. You can do regular chores like grocery shopping in the evening if necessary. Regular checking of blood sugar level Since diabetes is directly connected with heat waves, check your glucose level regularly during heat waves. Conclusion Heat waves are getting more and more harmful and can affect anyone. If you have diabetes, you should be careful during heat waves. Take preventive measures such as drinking plenty of water, monitoring your blood sugar level regularly, getting involved in regular exercise and eating a healthy diet. Drinking at least 1.5-2 litres of water is always advised to escape the scorching heat.
Whole Genome Sequencing and Next Generation Sequencing (NGS) Technologies
Drug resistance in Mycobacteria Tuberculosis (MTB) is attributed to the point mutation in a specific target gene. Using targeted NGS seems to hold much promise regarding early diagnosis of drug-resistant tuberculosis. The World Health Organisation's End of TB strategy is based on providing universal access to methods of early diagnosis and comprehensive drug susceptibility tests for all individuals with TB. This is one of the critical components of patient-centric care. This article expresses the views of Dr. Niranjan Patil, HOD and Scientific Business Head, Clinical Microbiology and Molecular Biology at the Global Reference Laboratory, Metropolis Healthcare Limited, Mumbai. He is a leading expert in Metropolis Healthcare. He aims to help you understand just a little bit more about targeted sequencing that can be attained through Sanger sequencing, Pyrosequencing, and Next-generation sequencing (NGS). Basis of DNA testing Each strand of DNA consists of 4 chemical units known as nucleotides. They make up your genetic alphabet. These include Adenine (A), Guanine (G), Cytosine (C), and Thymine (T). Sequencing of these nucleotides is what determines the meaning of all the information or genetic code in that part of your DNA. If these sequences get disturbed, it can lead to different forms of mutation known as Deletion Substitution Addition Deletion mutation Point mutations, etc. DNA sequencing refers to the technology or methods used to determine the order or sequence of the 4 base nucleotides (A, G, C, and T). This can be used to understand any kind of mutation that may have occurred in the genes. In the case of MTB, drug resistance is detected using Targeted sequencing. This helps generate information about a small area known as the genetic locus of interest. Whole genome sequencing (WGS) on the other hand provides a breakup of the entire genome of MTB in your sample. Targeted gene testing vs Whole genome sequencing As mentioned earlier, drug resistance in MTB occurs due to a target mutation in a specific gene. This is why it is beneficial to use targeted gene testing like Sanger sequencing, Pyrosequencing, and Next-generation sequencing (NGS). New developments in NGS technology have enabled the routine use of this technique for targeted NGS and WGS of Mycobacterium tuberculosis complex samples (MTCS), especially in high-resource settings. Whole genome sequencing using NGS has a lot of potentials to give a quick diagnosis of drug-resistant tuberculosis. Several challenges associated with conventional phenotype testing are now easily overcome with the help of WGS using NGS methodologies. At the same time, the WGS approach by NGS also overcomes other shortcomings of less comprehensive molecular tests like real-time PCR, CBNAAT tests, or line probe assays because of its quick, exhaustive, and detailed nucleic acid sequence information for whole genomes as well as multiple genetic regions of Mycobacterium tuberculosis. Uses of NGS Currently, NGS is used for Predicting TB drug resistance phenotypes by detecting variants in mycobacterial genomic sequence. Identifying and recognising different strain lineages of mycobacterial species to survey TB. Recognising and identifying genetically related strains to determine which is the transmission chain and using this information to break the chain of transmission. Resolving different results that have been obtained using different technologies. Diagnosing mixed infections. Predicting heteroresistance. Identifying novel drug resistance mutations that may not be covered under less comprehensive rapid molecular assays. Identifying point mutations. For screening and predicting resistance to retreatment. Who can benefit from Whole genome sequencing tests? Patients suspected of multidrug resistance. Patients with bacteriological confirmed MTB complex. Patients with rifampicin-resistant MTB complex detected using a phenotypic or molecular assay. Patients whose first or second-line therapy fails. Patients who have experienced a relapse of MTB complex infection. Patients whose first-line antimycobacterial therapy was discontinued but now want to re-initiate it. Patients with an underlying predisposition make treatment difficult. Patients that are in close contact with known MDR/XDR cases. While factors like higher initial cost, integration into the existing laboratory workflow, and the need for technical expertise to perform, analyse, and interpret these results have been a hamper to the growth of such techniques, there has been an increase in the number of patients utilising and adopting these techniques. Conclusion At Metropolis Health, we currently offer whole genome sequencing tests in which 18 different anti-TB drugs are tested simultaneously. Reflex strategies for TB diagnostics include genotypic molecular tests and phenotypic DST. To provide convenience to our customers, we provide different packages at affordable rates for patients and clinicians in challenging clinical scenarios. Find out more about our services today.
Common Food Allergies in Babies: What You Need to Know
Food allergies are infrequent in the Indian subcontinent. A recent report says that though the sensitisation rate of certain food items is relatively high in India (almost 26.5%), the probability of developing food allergies is very low(1.2%). However, there is still no positive explanation for these strange results. Therefore, food allergies are considered dangerous in India. Contrary to that, a global report says that although the prevalence of food allergies among adults is very low(1-2%), nearly 6-8% of children are diagnosed with food allergies. Five everyday food items aid food allergies among children. Breast milk is the best source of nutrition for babies up to 6 months. Introducing solids can be a great milestone for many parents but they must check their baby's body's reaction to new foods. As per Dr Ashish Sahdev, Head Marketing - Medico and PMT, Metropolis Healthcare Ltd, many children develop food allergies, which are abnormal reactions to certain foods. What is Allergy? Allergy is a common medical condition when foreign particles or allergens attack your immune system and the body exhibits specific reactions to them. When foreign particles enter your body, your immune system produces antibodies to fight those foreign particles. These antibodies may identify the allergens as harmful even if they don't have any potential to harm your body. In such cases, your body cannot hold it in and starts showing severe reactions. Allergies can occur due to several factors like pollen grains, dust, certain food items, air pollutants, etc. Thankfully, allergy is not life-threatening but severe cases can prove fatal. What is Food Allergy? Food allergy is a type of allergy that develops in your body after you eat certain food items. When your baby eats a different food for the first time, they will not show any symptoms as they get sensitised by the food. But during the second time, the IgE antibodies in your baby's body will react to the allergens and produce histamines. As a result, your baby may suffer from hives, itching in the mouth, diarrhoea and vomiting. Difference Between Food Allergy and Food Intolerance It is equally crucial for you to know that food allergy and food intolerance are not similar conditions. Your baby's immune system gets triggered by food allergies which can be life-threatening in severe cases. But food intolerance is a more superficial condition where your baby cannot digest certain foods. Food intolerance is not life-threatening and does not attack your baby's immune system. Common Food Allergies in Babies Doctors have spotted some of the most common food items that cause allergies in babies and children. They are as follows: Milk Your baby can develop allergies to cow milk as soon as you introduce formula. 85% of babies are prone to a milk allergy at the initial stage. However, they may resolve in later years. Eggs Eggs are one of the most common foods that cause allergies in babies. Please do not feed an entire egg to your baby. Separate the egg yolk and then try. If your baby cannot withstand it, you should stop giving them eggs. They could be allergic to the protein in eggs. Fish and shellfish Babies often fall sick of fish, especially shellfish. Be careful while feeding fish to your baby. Peanuts Nuts, including cashew, almond and pistachio, can cause allergies. Moreover, allergies to peanuts can be futile. Allergies from nuts do not usually go away. Take your baby to the nearest hospital as soon as possible if they show any symptoms or unusual behaviour. Wheat Babies may be allergic to glutens present in wheat. Don't add wheat to your baby's food once it is sure that wheat is the reason for the allergy. This gluten allergy may go away in the coming years. Soy Babies below 5 years sometimes exhibit allergies to soy. Be careful of what you are feeding your infant. Symptoms of Food Allergies Rush to the nearest healthcare centre if your baby shows any of the following symptoms after eating any allergic food: Vomiting Diarrhoea Cramps Hives Difficulty in breathing Eczema Swelling Itchiness around the mouth, lips, tongue Tightness in the throat Wheezing Treatment of Food Allergies If your baby is diagnosed with food allergies, their treatment should be initiated immediately. Visit a paediatrician and tell them about your baby's food chart. They may advise you to get an allergy test done. If it is not severe, your doctor will omit those food items the child is allergic to from the chart. They may suggest substitutes for those food items if necessary. In severe cases, infants are injected with epinephrine to reverse anaphylaxis by constricting blood vessels to increase blood pressure and opening airways to help to breathe. Preventive Measures If your baby is prone to food allergies, please follow the following instructions: Get a food allergy test done It is highly recommended to get an allergy test done to find out what foods your baby is allergic to. Eliminate Foods That Trigger Your Baby's Allergy Omit the foods that cause your baby to fall sick. These allergies may go away later but don't take any risk now. It is essential to check the ingredients present in packaged foods before feeding them to your baby. Carry Safe Foods Always carry simple, easy-to-digest food with you. You can seek the guidance of a nutritionist to make a balanced food chart. Check on Your Baby 24/7 Though it is not easy, it is advised to observe your child when introducing them to new foods. Conclusion Food allergies are not usually considered dangerous but a severe allergy could be fatal. Get your child tested to diagnose any allergies. Take care to keep those food items that they are allergic to, beyond their reach. Watch out for any reactions after introducing any new food to them. Pay additional attention to the food mentioned above as such foods are known to cause allergies in young ones. Always consult your doctor if you notice any severe changes in your body after a new food introduction.
 Home Visit
Home Visit Upload
Upload















 WhatsApp
WhatsApp